Abstract
To explore opportunities for improving care based on the experiences and perspectives of different types of COPD patients based on the Information-Motivation-Behavioral skills (IMB) model with poor self-management behaviors. We used ethnographic methods (over 1000 h of observations for 30 participants), and conducted 34 semi-structured interviews with different patient profiles. Data were transcribed verbatim and analysed using thematic analysis. According to the IMB model, we divided participants into three categories, namely low-information and low motivation group, high information but low motivation group and low-information but strong motivation group. The first group had limited opportunities to acquire knowledge and decreased memory capacity. Also, patients did not feel the seriousness of COPD, or thought that self-management was not important, which led to the lack of self-management knowledge and motivation for this group of patients. In the second group, patients were pessimistic about the cure of the disease because of too much information or too much attention to the details of knowledge, which was also the reason why patients were unwilling to implement self-management although they had mastered enough knowledge. The third patient profile, with strong motivation, would seek health information resources through various channels. Because of this, they could easily acquire incorrect or unscientific information, which would make the situation worse. This qualitative study suggested COPD patients exhibited distinct self-management experiences, barriers, and recommendations due to variations in information processing and motivational characteristics. Future research should tailor precise self-management strategies based on individual patient profiles.
Similar content being viewed by others
Introduction
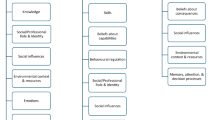
Chronic obstructive pulmonary disease (COPD) is a chronic respiratory disease with no cure that can cause a range of symptoms including dyspnea, cough, expectoration and systemic inflammation, especially in the elderly1. Self-management has been advocated for mitigating disease progression, curbing medical costs, and enhancing health-related quality of life among COPD patients2. Despite the prevalent reports on the benefits of self-management, COPD patients continue to exhibit a suboptimal level of self-management skills. For example: In a study, researchers used the Chinese version of Chronic Disease Self-Management Study Program (CDSSP) to evaluate the self-management behaviors of COPD patients, which includes the frequency of exercise, cognitive symptom management, and communication with physician. Findings from this study showed that participants had a low level of self-management behaviors3. The factors contributing to this status are many and likely include the knowledge of self-management and the motivation to implement it, as advocated by the Information-Motivation-Behavioral skills (IMB) model: as individuals acquire knowledge regarding health management strategies and their motivation intensifies, they progressively master and refine the behavioral skills required for positive transformation. In essence, the IMB model highlights the pivotal role of these three components in fostering a proactive stance towards health management (Fig. 1)4. Among COPD patients exhibiting suboptimal self-management behaviors, a subset may possess limited self-management knowledge, some may be devoid of motivation for sustained self-care, while others may experience both these deficiencie5. Nevertheless, the self-management experiences and barriers faced by COPD patients lacking either information, motivation, or both, may vary significantly. Qualitative research may help improve the quality of care that people receive through providing a detailed and nuanced picture of their experiences. However, previous qualitative studies have primarily focused on exploring the experiences and barriers of self-management among COPD patients. The results showed that the main barriers to the low self-management ability of COPD patients was the limited understanding of self-management knowledge or related to patients’ negative emotions, and emphasized the importance of health literacy and psychological counseling from their family6,7. However, these previous studies did not notice the differences between COPD patients. For example, a study showed that even if patients had a wealth of self-management knowledge, their self-management ability was still low5. This showed that there were other factors affecting self-management ability in COPD patients. An in-depth analysis of patients with varying factors of self-management barriers and the differences in their self-management experiences and barriers has not been conducted.
IMB model.
In this study, we aimed to identify and explore opportunities for improving care based on the experiences and perspectives of different types of COPD patients with suboptimal self-management behaviors.
Methods
Study design, participants, and settings
We conducted ethnographic observations and semi-structured interviews with patients aged 40 years and older who were diagnosed with COPD and evaluated as poor self-management by the COPD Self-Management Scale8. These patients were mild enough to cooperate with the interview and were hospitalized in a general hospital in southwest China, a region reporting the highest prevalence of COPD (20.2% compared to 15.6% in Northeast China and 13.6% in Northwest China)9. We identified participants via a data query that provided the contact information for individuals had been hospitalized for COPD, and called them to make an appointment. Purposive sampling captured a diverse sample in terms of gender and place of residence. The Medical Ethical Committee of the Medical Center Hospital of Qionglai city approved the study (NO 202356).We informed the participants of the purpose and significance of the study, and obtained the participants’ consent and signed the informed consent form. We confirmed that all methods were performed in accordance with the relevant guidelines and regulations, including the principles outlined in the COREQ (Consolidated Criteria for Reporting Qualitative Research) framework10, as well as the ethical standards set forth by the medical ethical committee of the Medical Center Hospital of Qionglai City, and all qualitative research procedures conducted in this study adhered rigorously to the ethical principles outlined in the Declaration of Helsinki, as revised in 2013 by the World Medical Association (WMA). This document serves as a fundamental ethical guideline for biomedical research involving human subjects. These guidelines ensured the protection of participants’ rights, privacy, and confidentiality throughout the research process11.
Data collection
We conducted semi-structured interviews for 34 participants in the hospital and over 1000 h of ethnographic observations for additional 30 participants (these participants were not drawn from the 34 participants who were interviewed) in their home from April 2022 to February 2024. We collected the basic information of participants through self-report, including their age, education level (time of education according to China’s education system: primary school ≤ 6 years; 6 years < middle school ≤ 9 years; 9 years < high school or technical secondary school ≤ 12 years; college degree or above > 12 years), marital status and years of diagnosis of COPD. Initially, we assessed participants’ knowledge of COPD self-management by the Chinese version of Bristol COPD Knowledge Questionnaire, which encompassed clinical symptoms, rehabilitation training, home oxygen therapy, smoking, application of antibiotics, steroid hormone therapy, inhalation bronchodilator, etc. The total score of the questionnaire is 30 points, and a total score of less than 18 points is considered as a low level of knowledge12. Researchers asked questions one by one according to the item of the questionnaire, and patients answered according to their actual situation. Following this, we administered the Patient Activation Measure 13 (PAM-13) to evaluate their level of patient activation, thereby assessing their motivation13. Based on their knowledge and motivation, we categorized the participants with poor self-management into three distinct groups by systematic clustering and k-means clustering methods14 (classification procedures and number of participants in each group: Fig. 2). Then, we conducted 34 semi-structured interviews with participants, and were conducted in Chinese by three female nurses (XCM; NYW; JL; RZ), who have received training in qualitative research methods and have extensive experience in interviews, through face-to-face communication in the quiet and undisturbed meeting room of the hospital.
Patient selection and classification procedures.
The interview guide (Table 1) was developed based on some reviews of COPD self-management and a study about IMB model7,15,16,17. In the above references on self-management, we mainly explored the experience of COPD patients in self-management and what they were eager to get help with. At the same time, through the systematic review of self-management intervention, we aimed to explore effective self-management interventions, and then we added these measures to the interview and asked the participants about their previous implementation and feelings. On the other hand, we were guided by the IMB model in order to put forward a comprehensive outline. The entire interview process adhered strictly to principles of voluntary participation and confidentiality, taking place in a serene and undisturbed environment conducive to candid sharing. The interviews ranged from 15–60 min, were fully recorded by voice recorder, and promptly transcribed within 24 h, and transcribed documents were returned to the participants for confirmation. Follow-up interviews were conducted to address any gaps among those who provided incomplete or ambiguous responses during the initial interviews, and participants were recruited until no new relevant knowledge was being obtained from new participants (namely data saturation)10. Researchers actively prompted participants to articulate their authentic experiences and sentiments. Subsequently, ethnographic observations were conducted in the homes of 30 participants after the semi-structured interviews, and the ethnographic observations were carried out by the same researchers who conducted the semi-structured interviews (XMC and RZ). They have undergone rigorous training in both theoretical and practical aspects of ethnography. Observations focused on daily self-management behaviors and motivations, and consisted of respiratory function exercise, inhalant use, home oxygen therapy, physical activity, and diet. The general focus of work occurred in these homes for about 12 days per site. This enabled us to gain a deeper insight into the participants’ self-management implementation, encompassing the specifics and accuracy of execution. Furthermore, it facilitated the distinct differentiation between active and passive execution, along with an analysis of the correctness and intensity of these two distinct modes of execution. Fieldwork consisted of over 1000 h of observations and informal conversations with 30 patients and their family members. Field notes and audios were written up into word documents.
Data analysis
In this qualitative study, we used the software NVivo 11.0 for data analysis and Excel for data management, which were collected through two different methods: ethnographic observations of 30 participants and semi-structured interviews with 34 participants. Thematic analysis served as the primary analytical tool for both datasets due to its flexibility and capacity to uncover underlying patterns and themes within qualitative data. For the ethnographic observation data, the analysis began with an in-depth familiarization process where the two researchers (XMC and RZ) meticulously reviewed extensive field notes taken in participants’ homes, reading and re-reading each note multiple times to gain a holistic understanding of observed behaviors, interactions, and environmental factors, making detailed annotations to highlight key events. For the semi-structured interview data, the analysis process started with in-depth familiarization with interview transcripts, where researchers read and re-read each transcript multiple times, taking notes on content, structure, tone, and participants’ language use. All material from observations and interviews was coded and then themed. This process commenced with the first author reading and re-reading all the data and coding the data to highlight anything that was relevant to the research aim. Next, the relationships between codes were explored, resulting in the development of a series of emerging themes and subthemes. These were developed further in discussion with the second author. The findings of our topic were fed back to the participants. Following the feedback of the study findings to the participants, we engaged in a follow-up discussion to elicit their perspectives on the presented results and to ascertain whether they had any recommendations for modifications or enhancements18.
Results
Participants’ characteristics
64 individuals participated in the study. 25(39.1%) participants were classified as individuals with low information and low motivation, and only 2(8%) participants reported high school education and above. In groups of participants with high information but low motivation, consisting of 19 (29.7%) participants, and 7 (36.9%) participants reported high school education or above. However, among participants with low information but strong motivation [consisting of 20 (31.2%) participants], 15 (75%) participants reported middle school education and below (Table 2).
Themes
We developed 6 main themes that reflect experiences with barriers to self-management (Table 3). Each theme includes examples with additional detail about participants’ qualitative experiences. However, significant differences in self-management experiences exist in the three groups.
Perspectives of low-information and low motivation group
Theme 1: Challenges in knowledge acquisition and retention
The limited self-management capabilities of these patients stem primarily from a deficiency in self-management knowledge. This stems from their relatively weak educational backgrounds or rural residences, which collectively hinder their access, acquisition, and comprehension of health-related information. Notably, some patients reported never having received formal self-management education, particularly those who have not been hospitalized for COPD or undergone standardized COPD treatment.
Further examination reveals that these patients predominantly adopt a passive learning approach, lacking the motivation to actively seek health knowledge from diverse sources, thereby constraining the expansion of their knowledge base. Compounding this issue, some patients indicate that healthcare providers often deliver relevant management information only during times of disease exacerbation or active treatment, resulting in reduced immediacy of knowledge absorption and long-term retention (Female, 79 years:‘If the doctor doesn’t tell you some health knowledge in hospital, how would we know? We don’t understand anything, and we don’t know who to ask or where to find that information’).
Moreover, even when patients initially demonstrate proficiency in skills and knowledge, age and disease-related memory decline impedes their ability to sustainably retain this information over time, ultimately affecting the consistency and effectiveness of their self-management capabilities (Male, 72 years: ‘Now that I am old, my memory is not as sharp as before, and a lot of health knowledge can’t be retained’).
Theme 2: Struggles with personal perception and coping in the disease
The self-management motivation of such COPD patients is notably inadequate, which can be attributed to the combined effects of multiple cognitive and emotional factors. Specifically, some patients fail to fully recognize the potential harm of COPD and the pivotal role of self-management in disease control due to their low frequency of acute exacerbation and mild symptoms (Male, 73 years: ‘I didn’t even realize I was sick, so I didn’t pay much attention to it usually, and I didn’t need any management knowledge as well’). Others tend to overly rely on pharmacotherapy while neglecting the positive effects of self-management. Another group of patients, plagued by recurrent and severe symptoms, experienced intense feelings of frustration and hopelessness, leading to weakened will to survive and subsequent passive attitudes, refusing or struggling to adhere to medical protocols and daily self-management tasks (Female, 77 years:‘I trained for a few days, but it didn’t work. I still had difficulty breathing after training, so I stopped. It’s useless, why bother training?). Furthermore, some patients have adapted to COPD symptoms, establishing a lifestyle that coexists with the disease, lacking the motivation to alter their status quo to meet stricter disease management requirements.
This population is often constrained by lower levels of education and their rural residency, resulting in generally limited self-management abilities and a pronounced reliance on external support, particularly the long-term dependence on healthcare providers. In the realm of health management, they exhibited a heavy reliance on the guidance and intervention of professional medical personnel. Moreover, due to a lack of recognition of their active role in disease management, these patients tend to underestimate their self-efficacy, leading to passive self-management behaviors that hinder their proactive engagement in health maintenance and disease management processes (Male, 78 years: ‘The doctors can’t cure this illness of mine. It recurs many times a year and gets worse. Since the doctors can’t do anything about it, what can I do? My role in this must be minimal, right?’).
Perspectives of high information but low motivation group
Theme 1: Burdened by excessive details and information
This group is primarily concentrated among those with higher cultural literacy, whose educational level is relatively high and ability to accept and understand knowledge is relatively strong. They have extensively and deeply delved into the knowledge and information in the field of health management through diversified channels, such as from health care staffs, from community and family support, from the internet and social media, etc. However, due to the abundance of information sources and the vast amount of information, this segment of the population may encounter the problem of information overload when confronted with intricate and complex health information, subsequently leading to feelings of confusion and disorientation. (Male, 74 years: ‘There are too many sources of information, from the Internet and other people’s opinions in daily life. I know too much, so it’s hard to judge’) Furthermore, given their tendency towards rigorous and meticulous behavior, some patients may exhibit a heightened focus and pursuit of details in health management practices, potentially even slipping into an excessive obsession with the minutiae of health management, thereby neglecting the effectiveness and sustainability of overall health management.
Theme 2: Resistance and negativity in treatment engagement and habit modification
This group possesses relatively abundant knowledge about the specific medical condition, yet they lack the motivation to engage in self-management. Unlike patients with inadequate information and low motivation, this group fully acknowledges the incurability of COPD, hence firmly believing that self-management is futile. (Male, 72 years: ‘This illness is incurable, and there’s no miracle drug. We have been to top hospital, but the treatment effect is not good. So we think that other methods will definitely be less effective’) On the other hand, some patients are unable to meet the demands of self-management due to their difficulty in altering existing lifestyle habits.
Perspectives of low- information but strong motivation group
Theme 1: Deficiency and misinformation in information availability
This patient population was predominantly concentrated in rural areas and generally possessed a moderate level of education. Despite the fact that some patients did not fully acquire the relevant knowledge system for self-management, they exhibited a profound aspiration for good health, manifested in a strong willingness and motivation to engage in self-management practices. Consequently, they tend to actively seek knowledge and skills related to self-management through diverse channels, such as listening to other people’s comments, asking their elders for help, and actively looking for indigenous methods. However, due to a relative lack of rational evaluation capabilities, the information acquired in this process may be inaccurate or unscientific, potentially posing a threat to the effectiveness and safety of their self-management efforts. (Female, 74 years: ‘I’ve tried all those herbs they talked about, which are easily found all over the mountains. Basically, whenever I heard about any plant that could soothe coughs and dispel phlegm, I would try it’)
Theme 2: Proactive pursuit and application of information resources
This group demonstrated a pronounced level of concern and proactive approach towards their own health status, evidenced by their robust execution of health behaviors. They actively seek and integrated diverse resources to acquire knowledge and skills for self-management and health promotion. Once equipped with these skills, they tend to maintain consistent implementation over time (Female, 77 years: ‘I’ll walk around, listen to others’ opinions and observe their practices. No matter what I have learned, I will try). Nevertheless, it was noteworthy that this group exhibited a relatively weak capacity in evaluating the authenticity of health information, rendering them susceptible to non-expert or misleading external opinions during the information acquisition and execution process. Consequently, they may adopt and followed inaccurate or unscientific health guidelines, posing additional challenges for healthcare professionals in assessing the effectiveness of their self-management efforts.
Comparisons of experience among three groups
Each displaying unique differences in health information and self-management motivation. Specifically, for patients who lack both information and motivation, the core issue is limited understanding of COPD or inability to effectively comprehend and retain health-related knowledge, which may also significantly contribute to their low motivation. Conversely, patients who have limited access to information but exhibit strong motivation face the primary challenge of easily adopting and implementing inaccurate or unscientific health information, which may potentially exacerbate their symptoms. Their high level of self-management motivation actually increases the likelihood of persisting in erroneous behavioral patterns. As for patients who are well-informed but lack motivation, despite possessing sufficient knowledge of treatment and health management, it is precisely this knowledge base that may lead them to overly focus on minor physical changes and psychologically magnify these changes, potentially resulting in anxiety. This classification highlights the importance of tailored suggestions and interventions to address the specific challenges faced by each patient profile in order to improve COPD care and management (Table 4).
Discussion
This study used ethnographic method and semi-structured interviews to explore opportunities for improving care based on the experiences and perspectives of different types of COPD patients. This study yielded several barriers that influence self-management of different patient profile based on the information-motivation-behavioral skills model. We found that different patient profile have different experiences of difficulties in managing COPD, and we identified strategies to optimize competencies of different types of COPD patients.
We discern those with inadequate information and low motivation exhibited distinct challenges in navigating barriers to self-care practices, as compared to individuals with abundant information but sufficient motivation. As posited by Hibbard and colleagues, low-activation patients exhibited marked deficits in health literacy, management skills, and valuing self-care, hence termed “passive patients”19. This underscores the need for tailored interventions that not only enhance informational access but also motivate and empower such individuals to actively engage in their health. Hence, patients with low activation exhibit suboptimal health knowledge, skills, and beliefs, with disparities rooted in distinct experiences. Notably, those with inadequate information and low motivation predominantly reside in lower-educated or rural settings, lacking systematic education, which resulted in limited comprehension of disease management, mirroring prior findings6. In addition, another study confirmed that COPD patients were prone to cognitive impairment, and the incidence of cognitive impairment in patients with COPD can be up to 56.5%20. COPD patients often experience impairments in attention, memory, and executive functions, pivotal for self-management. This manifests in poor communication with healthcare providers, hindering information reception. Memory deficits further compromise long-term retention of health knowledge, undermining patients’ ability to apply acquired information21. Therefore, patients with COPD often lack effective knowledge about health management. According to the IMB model, it can be deduced that information can influence motivation22. We can understand it as: when patients lack sufficient health knowledge, their beliefs, confidence, and actions in carrying out healthy behaviors will be significantly lacking. Consequently, patients will demonstrate specific behaviors related to a weak motivation for self-management, manifesting as fatalistic views or reluctance to adjust lifestyles. Strengthening self-management knowledge is paramount, achieved via science popularization, medical consultations, and for memory-impaired patients, memory strategies or cognitive training23.
Our findings indicated that patients with sufficient knowledge but lacking motivation were predominantly those with some cultural awareness or are relatively youthful. Despite familiarity with COPD self-management, their motivation remains low, possibly due to a perceived incurability and belief that self-management efforts are futile. These entrenched beliefs hinder agreement with medical advice. However, research has shown that peer support has been effective in enhancing compliance with self-management, as they tend to resonate with shared experiences from those in similar circumstances24. Therefore, engaging COPD patients who excel in self-management to share their positive experiences could bolster the motivation of informed yet unmotivated patients. Additionally, fostering family involvement in overseeing and supporting the patient’s self-management practices is pivotal to enhancing overall outcomes25.
Consistent with our study, notable disparities emerged in the self-management experiences of COPD patients based on their informational and motivational profiles. Specifically, those with inadequate information and low motivation, as well as those with limited information but strong motivation, confronted comparable challenges in health literacy, notably the scarcity of health information. Prior research echoes this, highlighting unclear inhaler instructions and inadequate communication between healthcare providers and patients as primary barriers to compliance, further underlining the need for targeted interventions to address these gaps26. Patients with limited information but strong motivation exhibited elevated levels of activation, resulting in superior overall execution capabilities. Notably, they proactively utilized tools to compensate for memory deficits, sought diverse information sources to address their health knowledge gaps, and seamlessly integrated disease management into their daily routines, fostering habit formation. Another study also demonstrated that higher patient activation levels positively correlate with engagement in health-promoting behaviors19. In addition, patients with high motivation were more likely to obtain the information they need from healthcare providers27. Despite their heightened motivation, and proficiency in maintaining healthy habits, these patients faced a significant disadvantage: an inability to critically assess the veracity of information, leading them to readily accept others’ opinions and potentially perpetuate incorrect health behaviors over time. This predicament posed a formidable challenge for healthcare professionals, who were tasked with delivering scientific, and tailored health education while also monitoring patients’ adherence to evidence-based practices. Consequently, it is imperative to empower these patients with the means to discern knowledge accuracy and to encourage familial support in monitoring their behaviors, thereby mitigating the risk of unscientific practices.
Limitations
There are limitations to this study. First, participants in this study are only COPD patients who have received treatment in a tertiary hospital in Chengdu, China, and the sample may be not representative enough. People in different parts of China have different habits and values, so our findings should not be generalized to all patients with COPD. Second, the interviews with a few inactive interviewees were short. They felt that our research could not help them, so they did not want to share so much about the topic. Finally, we employed a convenience sampling method, and the interviewees were hospitalized COPD patients, which may have led to selection bias in the study subjects.
Conclusions
Drawing upon the IMB model, the suboptimal self-management behaviors observed among COPD patients can be categorized into three distinct types, each with unique experiences of encountering barriers to self-care. We propose the adoption of tailored improvement measures specific to each patient profile. By offering targeted health education or enhancement strategies that are grounded in patients’ individual types and their respective self-management challenges, we can foster an environment conducive to the enhancement of patients’ self-management capabilities.
Data availability
No datasets were generated or analysed during the current study.
References
Agustí, A. et al. Global initiative for chronic obstructive lung disease 2023 report: GOLD executive summary. Eur. Respir. J. 61, 2300239 (2023).
Effing, T. W. et al. Definition of a COPD self-management intervention: International Expert Group consensus. Eur. Respir. J. 48, 46–54 (2016).
Lan, X., Lu, X., Yi, B., Chen, X. & Jin, S. Factors associated with self-management behaviors of patients with chronic obstructive pulmonary disease. Jpn. J. Nurs. Sci. 19, e12450 (2022).
Amico, K. R., Toro-Alfonso, J. & Fisher, J. D. An empirical test of the information, motivation and behavioral skills model of antiretroviral therapy adherence. AIDS Care 17, 661–673 (2005).
Chen, X. et al. The impact of cognitive impairment on patient activation and their value in self-management among COPD patients. Patient Educ. Couns. 129, 108397 (2024).
Russell, S. et al. Qualitative systematic review of barriers and facilitators to self-management of chronic obstructive pulmonary disease: views of patients and healthcare professionals. NPJ Prim. Care Respir. Med. 28, 2 (2018).
Zhao, D. & Lu, Y. W. A systematic review of qualitative research on self-management experiences of patients with chronic obstructive pulmonary disease. J. Nurses Train. 36, 1021–1029 (2021).
Wang, L., Nygårdh, A., Zhao, Y. & Mårtensson, J. Self-management among patients with chronic obstructive pulmonary disease in China and its association with sociodemographic and clinical variables. Appl. Nurs. Res. 32, 61–66 (2016).
Fang, L. et al. Chronic obstructive pulmonary disease in China: a nationwide prevalence study. Lancet Respir. Med. 6, 421–430 (2018).
Tong, A., Sainsbury, P. & Craig, J. Consolidated criteria for reporting qualitative research (COREQ):a 32-item checklist for interviews and focus groups. Int. J. Qual. Health Care 19, 349–357 (2007).
World Medical Association World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA 310, 2191–2194 (2013).
Niu, M. E. et al. Cognitive status of patients with chronic obstructive pulmonary disease towards their disease. Nurs. J. Chin. People’s Liberation Army 27, 1699–1700 (2010).
Chen, S. Q. et al. Reliability and validity analysis for the Chinese version of the patientactivation measure for patients with chronic heart failure. J. Nurses Train. 35, 198–203 (2020).
Wang, Y. X., Lin, R., Yan, Y. J. & Li, H. ldentification of subtypes of diabetes patients with mild cognitive impairment: a cluster analysis. J. Nurs. Sci. 4, 45–48 (2024).
Cravo, A. et al. The importance of self-management in the context of personalized care in COPD. Int. J. Chron. Obstruct. Pulmon. Dis. 17, 231–243 (2022).
Schrijver, J. et al. Self-management interventions for people with chronic obstructive pulmonary disease. Cochrane Database Syst. Rev. 1, CD002990 (2022).
Lim, K. E., Kim, S. R., Kim, H. Y., Kim, S. R. & Lee, Y. C. Self-management model based on Information-Motivation-Behavioral skills model in patients with chronic obstructive pulmonary disease. J. Adv. Nurs. 78, 4092–4103 (2022).
Hari, R., Geraghty, S. & Kumar, K. Clinical supervisors’ perspectives of factors influencing clinical learning experience of nursing students from culturally and linguistically diverse backgrounds during placement: a qualitative study. Nurse Educ. Today 102, 104934 (2021).
Hibbard, J. H., Stockard, J., Mahoney, E. R. & Tusler, M. Development of the Patient Activation Measure (PAM): conceptualizing and measuring activation in patients and consumers. Health Serv. Res. 39, 1005–1026 (2004).
Chen, X. et al. Rural-urban differences in mild cognitive impairment among patients with chronic obstructive pulmonary disease in ChengDu, China. Int. J. Chron. Obstruct. Pulmon. Dis. 18, 2497–2508 (2023).
Baird, C., Lovell, J., Johnson, M., Shiell, K. & Ibrahim, J. E. The impact of cognitive impairment on self-management in chronic obstructive pulmonary disease: a systematic review. Respir. Med. 129, 130–139 (2017).
Wang, H. et al. Effect of health intervention via web-based education on improving Information-Motivation-Behavioral skills related to HPV vaccination among Chinese female college students. Int. J. Public. Health 68, 1605596 (2023).
Park, M. O., Oh, H. S. & Seo, W. S. Effects of a cognitive rehabilitation programme on cognitive function, self-management and quality of life in patients with chronic obstructive pulmonary disease. Int. J. Nurs. Pract. 27, e12932 (2021).
Aboumatar, H. et al. Comparing self-management programs with and without peer support among patients with chronic obstructive pulmonary disease: a clinical trial. Ann. Am. Thorac. Soc. 19, 1687–1696 (2022).
Liu, Y. R., Wang, Y., Liu, J. & Xie, H. Path analysis of illness perception, medication beliefs, family support on inhaler adherence in elderly COPD patients: based on triadic reciprocal determinism. Patient Educ. Couns. 130, 108465 (2025).
O’Toole, J., Krishnan, M., Riekert, K. & Eakin, M. N. Understanding barriers to and strategies for medication adherence in COPD: a qualitative study. BMC Pulm. Med. 22, 98 (2022).
Greene, J. & Hibbard, J. H. Why does patient activation matter? an examination of the relationships between patient activation and health-related outcomes. J. Gen. Intern. Med. 27, 520–526 (2012).
Acknowledgements
This study was supported by National Social Science Funding Project (20BRK039).
Author information
Authors and Affiliations
Contributions
X.M.C., N.Y.W., J.L. conducted the data collection and analysis and produced the initial draft of the manuscript. Y.X.H. and L.W. implemented the intervention and commented on drafts. R.Z. reviewed and commented on drafts. Y.N.Y. is the qualitative lead and overall guarantor, conducted analysis and reviewed and edited the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
This study involves human participants and was approved by the Medical Ethical Committee of the Medical Center Hospital of Qionglai city approved the study (NO 202356). Participants gave informed consent to participate in the study before taking part. We confirmed that all methods were performed in accordance with the relevant guidelines and regulations, and all procedures were performed in accordance with the Declaration of Helsinki.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Chen, X., Wen, N., Liu, J. et al. Self-management and COPD: a qualitative study to explore the perceived barriers and recommendations to improve COPD management using the Information-Motivation-Behavioral skills model. npj Prim. Care Respir. Med. 35, 34 (2025). https://doi.org/10.1038/s41533-025-00443-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41533-025-00443-9