Abstract
The aim of this study is to explore the relationship between the MTNR1B gene variants rs1387153 and rs10830963 and the risk of gestational diabetes mellitus (GDM). Additionally, the study sought to investigate gene-environment interactions, assess the cumulative genetic risk through the application of Genetic Risk Scores (GRSs), and establish a predictive model for GDM. A case-control study was conducted with 500 GDM patients and 502 controls. MTNR1B gene variants were genotyped using SNPscan™. Associations between clinical data, genetic models, haplotype and GDM risk or blood glucose levels were analyzed using statistical tests. Gene-environment interactions were preliminarily analyzed with GMDR and logistic regression. SNP-age interactions were further explored through stratified analysis and GRS. A predictive model was developed using logistic regression, validated with bootstrap resampling, and its clinical utility was evaluated with decision curve analysis. The study has identified a significant association between the MTNR1B gene variants rs1387153 and rs10830963 and an increased risk of GDM, particularly in women under 30 years of age (all OR > 1, P < 0.05; rs1387153 TT vs. CC: OR = 2.969, P < 0.001, rs10830963 GG vs. CC: OR = 3.066, P < 0.001). The gene-age interaction was found to be statistically significant (P < 0.05). The analysis of the TC haplotype (OR > 1, P < 0.001) and the GRS, specifically in the top quartile of GRS (OR > 3, P < 0.001), further corroborates the cumulative impact of these variants on the risk of GDM among pregnant women under 30 years. The variants also significantly increase postprandial blood glucose levels in pregnant women under 30 years of age (P < 0.05). A predictive model that includes MTNR1B polymorphisms, maternal age, and pre-pregnancy BMI has shown good predictive accuracy for GDM risk (C-Statistics = 0.682, P < 0.001). The study highlights the key role of MTNR1B gene variants rs1387153 and rs10830963 in GDM risk among young pregnant women under the age of 30, with no correlation observed in pregnant women aged 30 and above. The gene-age interaction and GRS provide additional insights into GDM risk. These findings serve as a significant inspiration for future research on populations with MTNR1B gene variations, hopefully prompting more researchers to pay attention to adopting appropriate research, screening, prevention, and intervention strategies for pregnant women with diabetes at different age stages.
Similar content being viewed by others
Introduction
Gestational diabetes mellitus (GDM) is a prevalent condition emerging during pregnancy, presenting substantial health hazards to both the mother and the child. Characterized by the interplay of insulin resistance and β-cell dysfunction1, GDM, if not promptly addressed, can result in serious complications such as fetal macrosomia, birth trauma, and an escalated risk of type 2 diabetes (T2DM) later in life2,3. The genesis of GDM is intricate, stemming from a tapestry of genetic susceptibilities, environmental influences, and the physiological shifts intrinsic to pregnancy4,5. Pinpointing the genetic factors that heighten the risk of GDM is essential for crafting tailored approaches to screening and prevention.
Melatonin, a hormone synthesized in the pineal gland, plays a crucial role in regulating circadian rhythms and glucose metabolism. The MTNR1B gene encodes the melatonin receptor, which is expressed in pancreatic beta cells and is involved in insulin secretion. Genetic variations in MTNR1B, such as rs10830963, have been shown to increase the expression of MTNR1B mRNA in pancreatic islets, leading to enhanced melatonin signaling. This, in turn, can impair insulin secretion and contribute to elevated blood glucose levels, a key feature of GDM6,7,8.
The MTNR1B gene has garnered attention for its pivotal role in the regulation of circadian rhythms and the maintenance of glucose equilibrium, and its association with the pathophysiology of T2DM positions it as a key suspect in GDM research6,9. The MTNR1B gene encodes the melatonin receptor, which plays a crucial role in the human body. Melatonin is a hormone synthesized in the pineal gland, and it is key in regulating the sleep-wake cycle, biological rhythms, and influencing reproduction. The expression of the MTNR1B gene is mainly concentrated in the retina, brain, and pancreatic beta cells, where melatonin signaling is essential for maintaining normal physiological functions10,11.
In diabetes research, especially in the occurrence of GDM, variations in the MTNR1B gene have been found to be associated with the regulation of blood glucose levels12. For instance, the rs10830963 risk variant on the MTNR1B gene is an expression quantitative trait loci (eQTL), which has been found to increase the expression of MTNR1B mRNA in human islets. This means that individuals carrying the G allele of this variant may have a stronger melatonin signal in the pancreas, which could affect the transcription and secretion of insulin, thereby influencing blood glucose levels7. Specific genetic variations within this gene, notably the rs1387153 and rs10830963 polymorphisms, have garnered considerable research focus due to their hypothesized association with GDM risk. Concurrently, environmental determinants such as maternal age and pre-pregnancy BMI (pre-BMI) are well-established as significant contributors to GDM risk. Environmental influences may alter the manifestation of genetic risk factors, resulting in a spectrum of disease expression13. While the interactions between genetic and environmental factors is acknowledged as a critical component in progression of GDM, the nuanced interplay between these elements and genetic predisposition remains to be fully elucidated.
Riskscore is one of the important methods to evaluate the risk prediction ability in epidemiological studies. The method of incorporating genetic susceptibility factors into the riskscore to evaluate the effect of genetic susceptibility factors in the risk prediction model is called geneticriskscore (GRS). In recent years, GRS have covered some SNPs of candidate genes related to GDM, and their use in combination with known risk factors helps to predict the disease14. However, they have been less applied in MTNR1B rs1387153 and rs10830963.
This study endeavors to broaden our comprehension by undertaking a thorough examination of the nexus between MTNR1B genetic variations and GDM risk, taking into account the complex interactions between genetic and environmental factors, and evaluating the aggregate genetic risk through GRSs. The integration of genetic and environmental parameters into predictive models is anticipated to refine the precision of GDM risk estimation and to inform strategic preventative measures. Age-specific analysis may further delineate the influence of rs1387153 and rs10830963 on GDM risk across various age brackets, thereby contributing to the formulation of individualized preventative and interventional strategies.
Materials and methods
Study subjects
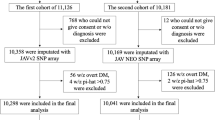
All pregnant women in the study were recruited from the Shunde Women and Children’s Hospital of Guangdong Medical University. Glucose tolerance tests were conducted according to the diagnostic criteria of the International Association of Diabetes and Pregnancy Study Groups (IADPSG), between 24 and 28 weeks of gestation. Blood glucose levels were measured after a 75 g oral glucose tolerance test (OGTT), including fasting plasma glucose (FPG), 1-hour plasma glucose (1 h-PG), and 2-hour plasma glucose (2 h-PG). GDM was diagnosed if the following criteria were met: FPG ≥ 5.1 mmol/L, or 1 h-PG ≥ 10.0 mmol/L, or 2 h-PG ≥ 8.5 mmol/L. Eligibility for inclusion was determined based on these criteria. The study included 500 women diagnosed with GDM and 502 healthy controls. Controls were matched to cases based on age (± 3 years), ethnicity (Han Chinese), and gestational age at the time of glucose tolerance testing (24–28 weeks). Inclusion criteria were: voluntary informed consent, no prior diagnosis of diabetes (All participants underwent FPG testing in early pregnancy. If the fasting glucose level was ≥ 5.1 mmol/L, a 75 g OGTT was immediately performed to rule out pre-pregnancy diabetes. Participants meeting any of the following criteria were excluded: Fasting glucose ≥ 7.0 mmol/L or 2-hour glucose ≥ 11.1 mmol/L. Participants with normal OGTT results were retained in the study and underwent repeat OGTT at 24–28 weeks of gestation to screen for GDM), Han ethnicity, age 18 or above, no pregnancy complications, and no use of hypoglycemic medications. Exclusion criteria included non-Han ethnicity, pre-existing diabetes, or any other significant medical conditions that could affect glucose metabolism.
This study was approved by the Ethics Committee of the Shunde Women and Children’s Hospital of Guangdong Medical University, and each participant provided voluntary informed consent. All methods were performed in accordance with the relevant guidelines and regulations.
Data collection
Demographic and clinical data, including age, ethnicity, height, gravidity and parity were collected, participants’ prepregnancy weight was also noted. The pre-BMI (expressed in Kg/m^2) was derived by dividing the weight in kilograms by the square of the height in meters. Utilizing pre-BMI values, the classification of obesity among the Chinese population was categorized as follows: obese (BMI ≥ 28 Kg/m^2), overweight (24 Kg/m^2 ≤ BMI < 28 Kg/m^2), normal weight (18.5 Kg/m^2 ≤ BMI < 24 Kg/m^2), and underweight (BMI < 18.5 Kg/m^2).
SNP genotyping
The genomic DNA was extracted utilizing the QIAamp DNA blood kit, a product of Qiagen from Germany. The detection of individual SNPs’ genotypes was executed through the SNPscan technique. The ABI3730XL sequencer from Applied Biosystems in the USA, along with GeneMapper 4.1 software, was employed for the collection and analysis of the raw data, respectively. Genesky Technologies Inc., based in Shanghai, China, was involved in this process. Further quality control measures were implemented to confirm the precision of the genotyping outcomes.
Statistical analyses
Continuous variables (mean ± standard deviation) were compared using the independent samples t-test; discrete variables, including the assessment of Hardy-Weinberg equilibrium (HWE) within the control group, were evaluated using the chi-square test. The correlation between Age or pre-BMI and the risk of GDM was explored through the receiver operating characteristic (ROC) curve analysis. Binary logistic regression analysis was utilized to evaluate the correlation between various genetic models and the risk of GDM, quantifying this relationship with odds ratios (OR) and 95% confidence intervals (CI). The statistical analyses were executed using SPSS 20.0 software (SPSS, Chicago, Illinois, USA). Initial assessments of gene-environment interactions were performed using the GMDR tool alongside logistic regression. Haplotype analysis was conducted via the online platform “SHEsisPlus.”
The sample size was calculated based on an assumed OR of 1.5 for the risk alleles, a minor allele frequency (MAF) of 0.430 for rs1387153 and 0.413 for rs10830963 (Based on the 1000 Genomes CHBS database), a significance level of 0.05, and a power of 90%. Using the Quanto software (version 1.2.4), we determined that a sample size of 500 cases and 502 controls would be sufficient to detect the expected associations. The study achieved a power of > 90% for both SNPs. This indicates that our study had sufficient power to detect the reported associations.
The interactions between SNPs and established risk factors, such as age, were identified through the application of simple count genetic risk scores (SC-GRS), direct logistic regression genetic risk scores (DL-GRS), and stratified analysis methodologies. The SC-GRS was ascertained by aggregating the risk alleles of the identified SNPs, with participants categorized into quartiles based on the distribution of GRS scores at the 25th, 50th, and 75th percentiles (Quartile 1: ≤ 25th percentile, Quartile 2: between 25th and 50th percentiles, Quartile 3: between 50th and 75th percentiles, Quartile 4: > 75th percentile). The β-coefficients associated with each SNP were derived from an additive genetic model logistic regression, which was then used to calculate the weighted DL-GRS. Given the constraints on sample size, the study’s dataset served as a training set for model development, followed by internal validation through Bootstrap resampling. A Logistic regression model was established, a Nomogram was charted, and the model’s predictive accuracy was appraised using C-Statistics, with further validation and Calibration plotting via the Bootstrap resampling technique. The decision curve analysis (DCA) was applied to assess the clinical utility of the predictive model. These analyses were conducted using R software (version 4.4.1). The influence of SNPs on blood glucose levels was examined and graphically represented using GraphPad Prism 9.5 for one-way ANOVA. Statistical significance was determined at the threshold of P < 0.05 for all bilateral tests.
Results
General clinical characteristics of the subjects
In this case-control study, we enrolled 500 women diagnosed with GDM and a matched group of 502 healthy controls. Genotyping for the MTNR1B gene’s rs1387153 and rs10830963 single nucleotide polymorphisms (SNPs) was successfully conducted for all participants. Table 1 presents the clinical baseline characteristics of the study population. Comparative analysis revealed that the GDM group exhibited significantly higher mean values for age, pre-BMI, and blood glucose levels compared to the control group (P < 0.05). Additionally, the GDM group showed a statistically significant difference in gravidity and parity when compared to the control group across the entire study sample (P < 0.05). However, these differences were not observed when the subjects were stratified by age, indicating no association between age-stratified groups and gravidity or parity in this study.
Association between age or pre-BMI and GDM risk
Advanced maternal age and elevated pre-BMI have been established as risk factors for GDM in previous studies. Our findings corroborate this association, demonstrating a significant correlation between maternal age and GDM risk, which increases progressively with age (OR = 1.132, 95% CI: 1.098–1.167, P < 0.001). The ROC curve analysis yielded an Area Under the Curve (AUC) of 0.646 (95% CI: 0.612–0.680, P < 0.001), with the maximum Youden index of 0.222 at an age threshold of 30 years, yielding a sensitivity of 0.616 and a specificity of 0.606 (Fig. 1A; Table 2).
The diagnostic efficacy of (A) Age or (B) pre-BMI in GDM.
Inaddition, a significant association was observed between pre-BMI and GDM risk, with an increased risk of GDM as pre-BMI rose (OR = 1.138, 95% CI: 1.084–1.195, P < 0.001). The corresponding ROC curve analysis indicated an AUC of 0.598 (95% CI: 0.563–0.633, P < 0.001), with the maximum Youden index of 0.167 at a pre-BMI threshold of 21.6755 kg/m^2, resulting in a sensitivity of 0.426 and a specificity of 0.741 (Fig. 1B; Table 2).
Overall analysis the association between MTNR1B rs1387153, rs10830963 and GDM risk
Table 3 presents the findings from the HWE analysis and the MAF for the two SNPs within the control group. The genotype distributions were in accordance with HWE, with P-values exceeding the 0.05 threshold, indicating a representative sample from the genetic pool.
We assessed the correlation between the genotypes of the MTNR1B gene rs1387153 and rs10830963 SNPs and the risk of GDM using five genetic models: codominant homozygous, codominant heterozygous, dominant, recessive, and allele models. Both crude and adjusted ORs with their respective 95% CIs were calculated for each model. After adjusting for potential confounders, including age, pre-BMI, gravidity, and parity, all genetic models demonstrated a significant association with an elevated GDM risk for both SNPs.
For the rs1387153 SNP, the adjusted ORs were as follows: TT vs. CC (OR = 1.857, 95% CI: 1.271–2.712, P = 0.001), CT vs. CC (OR = 1.490, 95% CI: 1.083–2.050, P = 0.014), TT + CT vs. CC (OR = 1.595, 95% CI: 1.178–2.160, P = 0.003), TT vs. CT + CC (OR = 1.421, 95% CI: 1.041–1.939, P = 0.027), and T vs. C (OR = 1.347, 95% CI: 1.121–1.619, P = 0.002).
Similarly, for the rs10830963 SNP, the adjusted ORs were: GG vs. CC (OR = 2.087, 95% CI: 1.428–3.051, P < 0.001), CG vs. CC (OR = 1.501, 95% CI: 1.104–2.042, P = 0.010), GG + CG vs. CC (OR = 1.653, 95% CI: 1.235–2.212, P = 0.001), GG vs. CG + CC (OR = 1.607, 95% CI: 1.164–2.220, P = 0.004), and G vs. C (OR = 1.435, 95% CI: 1.193–1.726, P < 0.001), as detailed in Table 4.
The impact of gene-age and gene-preBMI interactions on GDM risk
Based on the aforementioned analysis, both MTNR1B rs1387153 and rs10830963, along with advanced maternal age and elevated pre-BMI, are established risk factors for GDM. To further investigate potential interactions between these genetic variants and age or pre-BMI, we employed the Gene-Environment Multifactor Dimensionality Reduction (GMDR) approach for interaction analysis.
In the gene-age interaction analysis, rs10830963 in combination with age emerged as the optimal two-factor model, demonstrating a significant interaction (cross-validation consistency of 9 out of 10, sample testing accuracy of 59.09%, and a significant P-value of 0.001); a significant interaction was also observed between rs10830963, rs1387153, and age (cross-validation consistency of 10 out of 10, sample testing accuracy of 54.30%, with a significant P-value of 0.011) (Table 5). However, no significant interaction was detected in the gene-pre-BMI interaction analysis.
Subsequently, a logistic regression model was developed to explore the interactive effects of rs1387153-age and rs10830963-age on the outcome of GDM (Fig. 2A and B). The results indicated that in women under the age of 30, the probability of developing GDM increased with age for those with the MTNR1B rs1387153 homozygous variant TT and heterozygous variant CT genotypes compared to the wild-type CC genotype. Similarly, the probability of GDM was higher for women with the MTNR1B rs10830963 homozygous variant GG and heterozygous variant CG genotypes compared to the wild-type CC genotype, with the homozygous mutation showing the most pronounced effect (Fig. 2C and D). However, the impact of MTNR1B rs1387153 and rs10830963 variations on the likelihood of GDM was attenuated in individuals aged 30 and above (Fig. 2E and F). This suggests that the influence of MTNR1B rs1387153 and rs10830963 genotypes on GDM risk is more pronounced at a younger age, with the effect diminishing as the population ages.
Interaction between the MTNR1B rs1387153, rs10830963 polymorphism and age (in years) in determining GDM. (A) The interaction of rs1387153 with age in the overall subjects. (B) The interaction of rs10830963 with age in the overall subjects. (C) The interaction of rs1387153 with age in the age < 30 years subjects. (D) The interaction of rs10830963 with age in the age < 30 years subjects. (E) The interaction of rs1387153 with age in the age ≥ 30 years subjects. (F) The interaction of rs10830963 with age in the age ≥ 30 years subjects.
Age-stratified analysis of the association of rs1387153 and rs10830963 with GDM risk
Building upon our previous findings, we conducted a more refined analysis to determine the association of the rs1387153 and rs10830963 with the susceptibility to GDM using age-stratified analysis. Notably, in the group of women under 30 years of age, after adjusting for age and pre-BMI, all genetic models for the MTNR1B rs1387153 and rs10830963 SNPs showed a significant association with an increased risk of GDM. The ORs for the rs1387153 SNP were as follows: TT vs. CC (OR = 2.969, 95% CI: 1.658–5.315, P < 0.001), CT vs. CC (OR = 1.964, 95% CI: 1.218–3.168, P = 0.006), TT + CT vs. CC (OR = 2.186, 95% CI: 1.379–3.466, P = 0.001), TT vs. CT + CC (OR = 1.835, 95% CI: 1.155–2.873, P = 0.010), and T vs. C (OR = 1.587, 95% CI: 1.219–2.066, P = 0.001). For the rs10830963 SNP, the adjusted ORs were: GG vs. CC (OR = 3.066, 95% CI: 1.745–5.388, P < 0.001), CG vs. CC (OR = 1.763, 95% CI: 1.128–2.756, P = 0.013), GG + CG vs. CC (OR = 2.038, 95% CI: 1.331–3.122, P = 0.001), GG vs. CG + CC (OR = 2.118, 95% CI: 1.316–3.410, P = 0.002), and G vs. C (OR = 1.697, 95% CI: 1.302–2.211, P < 0.001), as detailed in Table 6. However, in the age group 30 years and above, no significant correlation with GDM risk was observed (Supplementary Table 1). This refined analysis, underscores the MTNR1B rs1387153 and rs10830963 significant genetic predisposition to GDM among younger women.
Association between haplotype and GDM risk
The linkage disequilibrium between the MTNR1B rs1387153 and rs10830963 was notably strong (D’ = 0.80). Haplotype analysis indicated that there was a significant difference in the frequencies of the haplotypes CC and TG, formed by rs1387153 and rs10830963, between the GDM and control groups (CC: χ2 = 14.536, P < 0.001; TG: χ2 = 15.764, P < 0.001). Notably, these differences remained pronounced in the group of women under the age of 30 (P < 0.001). However, no significant differences were observed in the group aged 30 and above (P > 0.05) (Table 7). This analysis underscores the potential MTNR1B rs1387153 and rs10830963 genetic markers that may predispose younger women to GDM.
Associations between GRSs based on MTNR1B rs1387153 and rs10830963 and GDM risk
We compared the GRSs of two types between the GDM group and the control group. It was observed that the GRSs of GDM-affected pregnant women were significantly higher than those of the control group (P < 0.001, results not shown). Furthermore, both the SC-GRS and DL-GRS were divided into four parts based on quartile intervals. As depicted in Fig. 3, the overall analysis indicates that as the SC-GRS score increases, so does the risk of GDM (all OR > 1, P < 0.05). Regardless of covariate adjustment, the risk of GDM for the SC-GRS > 3 group (the highest quartile) was at least twice that of the SC-GRS ≤ 1 group (the lowest quartile) (OR = 2.218, 95% CI: 1.515–3.265, P < 0.001; adjusted OR = 2.077, 95% CI: 1.393–3.113, P < 0.001). For the DL-GRS, except for the group with scores between 0.716 and 1.033 (the third quartile), which showed no significant difference, the effects on GDM risk were similar to those of the SC-GRS. The DL-GRS > 1.033 group (the highest quartile) had at least twice the GDM risk of the DL-GRS ≤ 0.317 group (the lowest quartile) (OR = 2.341, 95% CI: 1.625–3.391, P < 0.001; adjusted OR = 2.223, 95% CI: 1.516–3.274, P < 0.001) (Fig. 4). Particularly in the subgroup of individuals under 30 years of age, similar results were obtained. It is noteworthy that in the subgroup of individuals under 30 years of age, the risk of GDM for the SC-GRS > 3 group was at least three times that of the SC-GRS ≤ 1 group (OR = 3.218, 95% CI: 1.781–5.878, P < 0.001; adjusted OR = 3.383, 95% CI: 1.840–6.295, P < 0.001). Similarly, the DL-GRS > 1.033 group had at least three times the GDM risk of the DL-GRS ≤ 0.317 group (OR = 3.231, 95% CI: 1.859–5.683, P < 0.001; adjusted OR = 3.319, 95% CI: 1.882–5.928, P < 0.001) (Fig. 4). However, in the subgroup of individuals aged 30 and above, no significant differences were observed (Supplementary Table 2). This suggests that the genetic variants MTNR1B rs1387153 and rs10830963 may have a greater impact on GDM risk in individuals under 30 years of age, with the influence of these genetic variations diminishing as age increases.
The association of GRS with GDM risk in the overall subjects. *Adjusted by age, pre-BMI, gravidity and parity.
The association of GRS with GDM risk in the age < 30 years subjects. *Adjusted by age and pre-BMI.
Clinical value of multifactorial prediction of GDM by SNPs, age, and pre-BMI
Based on our study and previous research, the MTNR1B SNPs rs1387153 and rs10830963, along with age and pre-BMI, have been identified as major risk factors for GDM. Integrating these factors into clinical practice, we constructed a predictive model for GDM using MTNR1B rs1387153, rs10830963, age, and pre-BMI. The model’s parameter, C-Statistics, was 0.682, and a nomogram was developed for practical application. To assess and validate the model’s performance, the Hosmer-Lemeshow goodness-of-fit test was visualized by constructing a calibration curve. The results indicated that the predicted and observed rates were closely aligned, nearly coinciding with the Y = X line, with an absolute error of 0.013 between the simulated and actual curves, demonstrating a strong consistency and indicating good model calibration. Further evaluation of the predictive model’s clinical utility was conducted using DCA. The DCA demonstrated that the “nomogram” curve was above the blue line, suggesting that the nomogram model could provide clinical benefit to patients. Based on the DCA results, a clinical impact curve (CIC) was constructed to assess the nomogram’s clinical efficacy. The CIC indicated that the nomogram had a superior net benefit and a practical threshold probability range, particularly within the high-risk threshold of 0.4 to 1, where the “Number high risk” curve closely matched the “Number high risk with event” curve, indicating the predictive model’s good predictive value (Fig. 5). we constructed a predictive model for GDM using MTNR1B rs1387153, rs10830963, age, and pre-BMI. The model’s parameter, C-Statistics, was 0.682. We further constructed separate predictive models for GDM for different age groups. The results showed that the parameter, C-statistic, for the model in the group under 30 years old was 0.678 (Supplementary Fig. 1); for the group aged 30 and above, the C-statistic was 0.618 (Supplementary Fig. 2). For the two genetic variations of MTNR1B rs1387153 and rs10830963, they play a more important role in predicting GDM in younger pregnant women.
Construction and validation of a nomogram model for GDM diagnosis in the overall subjects. (A) The diagnostic efficacy of combining age, pre-BMI, MTNR1B rs1387153, and rs10830963 in GDM. (B)Nomogram to predict the occurrence of GDM. (C) Calibration curve to assess the predictive power of the nomogram model. (D) DCA curve to evaluate the clinical value of the nomogram model. (E) Clinical impact curve based on the DCA curve to assess the nomogram model.
Association between genotype and blood glucose levels
In the final analysis, we examined the impact of MTNR1B rs1387153 and rs10830963 genotypes on blood glucose levels during the oral glucose tolerance test (OGTT). The results indicated that individuals with the rs1387153 TT and CT genotypes exhibited a significantly higher 1-hour glucose level compared to those with the CC genotype (P < 0.05). Additionally, the TT genotype showed a significantly higher 2-hour glucose level compared to the CC genotype (P < 0.05). For the rs10830963 variant, the GG genotype was associated with significantly higher FPG, as well as 1-hour and 2-hour glucose levels compared to the CC genotype (P < 0.05). The CG genotype also demonstrated a significantly higher 1-hour glucose level compared to the CC genotype, and the GG genotype had significantly higher 1-hour and 2-hour glucose levels compared to the CG genotype (Fig. 6). Notably, in the age group under 30 years, the differences in glucose level at 1-hour and 2-hour remained significant among the groups (Fig. 7). However, in the age group 30 years and above, only the rs10830963 GG genotype showed a significantly higher 1-hour glucose level compared to the CC genotype (P < 0.05), with no other groups showing significant differences (P > 0.05) (Supplementary Fig. 3). This analysis elucidates the genotype-specific effects on glucose response during OGTT and highlights the age-related nature of these genetic influences on glucose metabolism.
Association between SNPs polymorphisms genotype and plasma glucose levels in the overall subjects. (A) rs10830963. (B) rs1387153. FPG fasting plasma glucose, 1 h-PG 1 h plasma glucose, 2 h-PG 2 h plasma glucose. *P < 0.05, **P < 0.01, ***P < 0.0005, ***P < 0.0001.
Association between SNPs polymorphisms genotype and plasma glucose levels in the age < 30 years subjects. (A) rs10830963. (B) rs1387153. FPG fasting plasma glucose, 1 h-PG 1 h plasma glucose, 2 h-PG 2 h plasma glucose. *P < 0.05, **P < 0.01, ***P < 0.0005.
Discussion
Melatonin and its receptor MTNR1B play a significant role in glucose homeostasis. During pregnancy, the role of MTNR1B gene variants in blood glucose metabolism not only affects fasting blood glucose and early insulin release during pregnancy, also profoundly influences postprandial blood glucose and the conversion of proinsulin15. The G risk allele of rs10830963 is associated with increased expression of MTNR1B in pancreatic beta cells, which may enhance the melatonin effect that impairs insulin secretion6.
In this study, we demonstrated that the MTNR1B rs10830963 C > G polymorphism, in linkage disequilibrium with the MTNR1B rs1387153 C > T, is significantly associated with the risk of GDM and high blood glucose levels, with evidence of age heterogeneity. Following the initial discovery by Kim et al. in 2011 that two variants within the MTNR1B locus, rs10830963 and rs1387153, were significantly associated with GDM risk16, multiple studies, including ours, have shown a significant correlation between genetic variations in MTNR1B and the occurrence of GDM1,17,18,19.
In this study, the p-values for the five genetic models at the rs10830963 locus were all less than 0.05, and the OR were all greater than 1, indicating a high correlation between the mutant G allele and the risk of GDM, consistent with previous research17,18,20,21. Additionally, a large-scale analysis of Chinese pregnant women found that MTNR1B is the most important signal for all blood sugar traits, including the previously unreported OGTT1H and OGTT2H18. This study also confirmed that the levels of FPG, OGTT1H, and OGTT2H were significantly higher in individuals with the GG genotype at rs10830963 than those with the CC genotype, especially in pregnant women under the age of 30 years, the impact of the G allele at rs10830963 on the increase in blood sugar concentrations during OGTT1H and OGTT2H.
Previous research has found that the rs1387153 variant promotes the development of GDM16,17,22, and this study also shows that the risk allele T at rs1387153 significantly increases the risk of GDM. Furthermore, while previous studies have found an association between the rs1387153 locus and elevated FPG23, but this study found that individuals with the TT genotype at rs1387153 had significantly higher levels of OGTT1H and OGTT2H compared to those with the CC genotype in pregnant Chinese women. It may be the variation at rs10830963, which is in linkage disequilibrium with rs1387153, has a greater impact on postprandial blood sugar in pregnant women.
Although there is a considerable amount of research on the association between MTNR1B gene variants and GDM, most of it is based on analyses conducted in the general population and at the genetic level alone, potentially lacking more comprehensive evidence. Therefore, our study adds to the literature by examining gene-age interactions and providing a more refined and comprehensive analysis.
Our study further tested the age-rs1387153-rs10830963 interaction and found a significant interaction, but the size of the genetic effect gradually decreased with increasing age. The impact of these genetic variations is more pronounced in pregnant women aged ≤ 30 years. Stratified analysis by age, haplotype analysis, and GRSs analysis further support this view, especially for the homozygous variants of rs1387153 and rs10830963, where the risk of GDM is approximately three times that of the wild type. The highest scoring group of SC-GRS and DL-GRS has more than three times the risk of GDM compared to the lowest scoring reference group. Additionally, in our analysis, the positive correlation between SC-GRS and DL-GRS and the risk of GDM is evident; the higher the GRS quartile, the higher the likelihood of GDM. This dose-response relationship between GRS and GDM risk suggests a potential cumulative effect of genetic variations on GDM susceptibility. However, no statistical differences in the above indicators were found in pregnant women aged ≥ 30 years. At the same time, MTNR1B variants significantly increased the postprandial blood glucose levels of young pregnant women during OGTT.
Similar to the mechanisms involved in the development of T2DM, the pathogenesis of glucose intolerance or GDM during pregnancy mainly includes two pathological mechanisms: β-cell dysfunction and abnormal insulin resistance. It is worth noting that in senile diabetes T2DM, the main cause of β-cell dysfunction is likely due to the long-term burden of insulin secretion, which is obviously related to aging24; whereas in GDM, pregnant women are relatively young, and β-cell dysfunction is more likely to be caused by genetic defects related to insulin secretion function. In vitro and in vivo studies have shown that melatonin and its receptors have a direct effect on the function of pancreatic β-cells, among which the common rs10830963 G variant of the MTNR1B receptor is most likely to be associated with impaired pancreatic β-cell secretory function8; Similarly, studies have shown that the impact of the MTNR1B-rs10830963 polymorphism on fasting blood glucose levels is greater in young people, and diminishes in the elderly, to the point where no statistically significant effect is found in the elderly population25. Additionally, Holzapfel et al. analyzed the correlation of this polymorphism in children and adolescents, finding that each G allele was associated with an increase in fasting blood glucose by 0.205 mmol/L (3.69 mg/dL) (P < 0.0001). Therefore, they concluded: “The effect size in children and adolescents appears to be stronger than in adults.” This conclusion supports our results regarding age interaction, as well as our observation that the impact is greater in younger populations than in older adults26. In summary, all of these results tend to suggest that the MTNR1B rs10830963 G variant has a stronger inhibitory effect on insulin secretion in younger populations, especially in GDM. Our study further confirms that the MTNR1B rs10830963 G variant significantly increases the level of postprandial blood glucose and the risk of GDM in populations under 30 years old, which is likely related to its variant’s inhibition of insulin secretion in pregnant women. It is particularly interesting to note that there is no significant correlation between MTNR1B variation and the risk of GDM in women aged 30 and above. This may mean that other factors become more influential in regulating the risk of GDM in the age group of 30 and above. These may include reduced insulin sensitivity, changes in glucose metabolism, increased prevalence of obesity, other genetic variations, and age-related metabolic changes that may mask the effects of MTNR1B genetic variation24. Collectively, the age-specific association of MTNR1B variants with GDM risk may be related to the differential impact of genetic and environmental factors on glucose metabolism across age groups. In younger women, genetic factors such as MTNR1B variants may play a more prominent role in impairing insulin secretion, leading to a higher risk of GDM. In contrast, in older women, other factors such as reduced insulin sensitivity, age-related metabolic changes, and increased prevalence of obesity may overshadow the effects of MTNR1B variants. This is consistent with previous studies showing that the impact of MTNR1B variants on fasting glucose levels is more pronounced in younger individuals and diminishes with age25,26.
Therefore, in previous studies, this gene-age interaction was obscured in large cohorts. According to our study results, although a strong gene-age interaction was observed in the overall analysis, if we do not target the age-gene interaction analysis between MTNR1B-rs10830963 polymorphism and age as our further analysis goal, the correlation between MTNR1B-rs10830963, rs1387153 and GDM and OGTT blood glucose in the entire population has significant statistical significance. However, despite the association between MTNR1B-rs10830963, rs1387153 and GDM has been widely described in other studies, and the novelty of our re-research is precisely that the MTNR1B-rs10830963, rs1387153 risk variants are not associated with GDM and OGTT blood glucose in older pregnant subjects (≥ 30 years old), but are significantly associated with GDM in pregnant women under 30 years old. Therefore, our study results may help to re-analyze the correlation of published MTNR1B-rs10830963, rs1387153 polymorphisms in other cohorts, and better characterize their heterogeneity in age and population. This may help to obtain more accurate information for future precision medicine or precision nutrition27. Our study results emphasize the necessity of age-specific risk assessment for GDM, especially in young women who may have a higher genetic risk.
However, this study also has limitations. First, due to the fact that only a small portion of the subjects agreed to have fasting insulin levels tested, we have a severe shortage of data on fasting insulin, and thus lack valid analysis data for the relationship between MTNR1B-rs10830963, rs1387153 genotypes and insulin resistance index (HOMA-IR) and pancreatic β-cell function index (HOMA-β). In subsequent studies, this part of the data should be supplemented to provide direct evidence of the impact of MTNR1B variations on insulin secretion. Additionally, since the study only focused on the interaction between genes and Age and pre-BMI, it neglected the potential impact of other factors on the occurrence of the disease, resulting in a slightly lower test and prediction efficiency of the comprehensive prediction model, and no external validation was conducted. Additionally, hypertension, a known risk factor for GDM, was not measured in this study. In future studies, more other potential risk factors should be collected and included, and a better prediction model should be established using a larger dataset from different centers. By conducting more comprehensive and in-depth research, the research results can be extended to clinical practice.
Conclusion
The MTNR1B rs1387153 and rs10830963 polymorphisms interact with age to influence the occurrence of GDM, and their risk variants increase the risk of GDM in Chinese women, potentially having a cumulative effect on GDM susceptibility, especially in pregnant women under 30 years old, but show no correlation in those aged 30 and above.
Data availability
All data generated or analysed during this study are included in this published article and its supplementary information files.
References
Liu, J. et al. Melatonin receptor 1B genetic variants on susceptibility to gestational diabetes mellitus: A hospital-based case-control study in Wuhan, central China. Diabetes Metab. Syndr. Obes. 15, 1207–1216 (2022).
Johns, E. C. et al. Gestational diabetes mellitus: Mechanisms, treatment, and complications. Trends Endocrinol. Metab. 29 (11), 743–754 (2018).
Moon, J. H., Kwak, S. H. & Jang, H. C. Prevention of type 2 diabetes mellitus in women with previous gestational diabetes mellitus. Korean J. Intern. Med. 32 (1), 26–41 (2017).
Kampmann, U. et al. Gestational diabetes: A clinical update. World J. Diabetes. 6 (8), 1065–1072 (2015).
Franzago, M. et al. Nutrigenetics, epigenetics and gestational diabetes: Consequences in mother and child. Epigenetics 14 (3), 215–235 (2019).
Lyssenko, V. et al. Common variant in MTNR1B associated with increased risk of type 2 diabetes and impaired early insulin secretion. Nat. Genet. 41 (1), 82–88 (2009).
Tuomi, T. et al. Increased melatonin signaling is a risk factor for type 2 diabetes. Cell. Metab. 23 (6), 1067–1077 (2016).
Takeuchi, F. et al. Common variants at the GCK, GCKR, G6PC2-ABCB11 and MTNR1B loci are associated with fasting glucose in two Asian populations. Diabetologia 53 (2), 299–308 (2010).
Jia, G. et al. Effects of MTNR1B genetic variants on individual susceptibility to gestational diabetes mellitus: A meta-analysis. Am. J. Perinatol. 37 (6), 607–612 (2020).
Pandi-Perumal, S. R. et al. Melatonin: Nature’s most versatile biological signal? FEBS J. 273 (13), 2813–2838 (2006).
Mulder, H. et al. Melatonin receptors in pancreatic Islets: Good morning to a novel type 2 diabetes gene. Diabetologia 52 (7), 1240–1249 (2009).
Mussig, K. et al. Genetic variants in MTNR1B affecting insulin secretion. Ann. Med. 42 (6), 387–393 (2010).
Perisic, M. M. et al. Polygenic risk score and risk factors for gestational diabetes. J. Pers. Med., 12(9). (2022).
Kawai, V. K. et al. A genetic risk score that includes common type 2 diabetes risk variants is associated with gestational diabetes. Clin. Endocrinol. (Oxf). 87 (2), 149–155 (2017).
Liao, S. et al. The impact of genetic variants for different physiological characterization of type 2 diabetes loci on gestational insulin signaling in nondiabetic pregnant Chinese women. Reprod. Sci. 22 (11), 1421–1428 (2015).
Kim, J. Y. et al. Melatonin receptor 1 B polymorphisms associated with the risk of gestational diabetes mellitus. BMC Med. Genet. 12, 82 (2011).
Zhang, Y. et al. MTNR1B gene variations and high pre-pregnancy BMI increase gestational diabetes mellitus risk in Chinese women. Gene 894, 148023 (2024).
Zhen, J. et al. Genome-wide association and Mendelian randomisation analysis among 30,699 Chinese pregnant women identifies novel genetic and molecular risk factors for gestational diabetes and glycaemic traits. Diabetologia 67 (4), 703–713 (2024).
Jia, Y. et al. MTNR1B gene on susceptibility to gestational diabetes mellitus: A two-stage hospital-based study in Southern China. Mol. Genet. Genomics. 295 (6), 1369–1378 (2020).
Li, C. et al. Association between a melatonin receptor 1B genetic polymorphism and its protein expression in gestational diabetes mellitus. Reprod. Sci. 26 (10), 1382–1388 (2019).
Tarnowski, M. et al. MTNR1A and MTNR1B gene polymorphisms in women with gestational diabetes. Gynecol. Endocrinol. 33 (5), 395–398 (2017).
Liao, S. et al. Association of genetic variants of melatonin receptor 1B with gestational plasma glucose level and risk of glucose intolerance in pregnant Chinese women. PLoS ONE. 7 (7), e40113 (2012).
Bouatia-Naji, N. et al. A variant near MTNR1B is associated with increased fasting plasma glucose levels and type 2 diabetes risk. Nat. Genet. 41 (1), 89–94 (2009).
Weir, G. C. et al. Beta-cell adaptation and decompensation during the progression of diabetes. Diabetes 50 (Suppl 1), S154–S159 (2001).
Sorli, J. V. et al. Chronological age interacts with the circadian melatonin receptor 1B gene variation, determining fasting glucose concentrations in mediterranean populations. Additional analyses on Type-2 diabetes risk. Nutrients, 12(11). (2020).
Holzapfel, C. et al. Association of a MTNR1B gene variant with fasting glucose and HOMA-B in children and adolescents with high BMI-SDS. Eur. J. Endocrinol. 164 (2), 205–212 (2011).
Ordovas, J. M. et al. Personalised nutrition and health. BMJ 361, bmjk2173 (2018).
Acknowledgements
Not applicable.
Funding
National Natural Science Foundation of China (81873649); Doctoral scientific research Initiate funding project of Shunde Women and Children’s Hospital of Guangdong Medical University (Maternity and Child Healthcare Hospital of Shunde Foshan) (2020BSQD007); Self-financing science and technology project of Foshan (2420001004539; 2320001006049).
Author information
Authors and Affiliations
Contributions
All authors conceptualized and designed the study. Qiaoli Zeng, Dehua Zou, Guofang Zeng and Runmin Guo are responsible for the statistical analyses and writing, original draft. All authors contributed to the data interpretation and writing, review and editing and approved the final version of manuscript as submitted.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.

Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zeng, Q., Liu, X., Liu, J. et al. MTNR1B variants increase gestational diabetes mellitus risk in young Chinese pregnant women. Sci Rep 15, 19643 (2025). https://doi.org/10.1038/s41598-025-02248-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-02248-9