Abstract
Clinical studies have reported that anemic patients with lower back pain exhibit significantly more severe lumbar intervertebral disc (IVD) degeneration compared to non-anemic individuals. Given that iron deficiency (ID) is the leading cause of anemia, we hypothesized that ID may disrupt IVD metabolism—particularly extracellular matrix synthesis—thereby contributing to aberrant disc development and degeneration. To investigate this, we established an iron-deficiency anemia (IDA) rat model via an iron-deficient diet and induced IVD degeneration through needle puncture. Degenerative changes were assessed using MRI, while morphological alterations were evaluated via O-fast green and hematoxylin-eosin (H&E) staining. The gene expression was measured by quantitative reverse transcription PCR (RT-qPCR). Immunofluorescence staining was employed to observe the protein expression. Additionally, TUNEL (TdT-mediated dUTP nick end labeling) was performed to assess apoptosis in nucleus pulposus cells. Our findings revealed that iron deficiency significantly impaired the development of rat caudal intervertebral discs characterized by reduced MRI signal intensity, diminished notochordal cell populations in the nucleus pulposus, thinning of the cartilage endplate, and Impaired type II collagen synthesis. However, despite these developmental abnormalities, iron deficiency did not exacerbate puncture-induced disc degeneration. MRI and histological analyses showed no significant differences in degenerative severity between IDA and control groups following needle injury. Additionally, TUNEL assays indicated no marked increase in apoptotic activity in IDA rats.
Similar content being viewed by others
Introduction
Iron is an essential trace element for the human body, widely involved in various life activities such as oxygen transport, DNA synthesis, mitochondrial respiration, and neurotransmitter synthesis1,2,3,4. As the most prevalent nutritional deficiency globally, iron deficiency (ID) primarily stems from insufficient dietary intake, chronic inflammation, and persistent blood loss1,5. According to the World Health Organization (WHO), approximately 42% of anemic children and 50% of anemic women globally require iron supplementation therapy1. In the United States, about 11% of children (aged 6 months to 5 years), 15% of premenopausal women, and 18% of pregnant women suffer from iron deficiency6,7. ID and iron deficiency anemia (IDA) are more prevalent in low- and middle-income countries8. Clinical symptoms of ID, whether or not accompanied by IDA, may include fatigue, drowsiness, decreased attention, dizziness, tinnitus, pallor, and headaches1. Additionally, ID and IDA can exacerbate the clinical symptoms of certain diseases and affect their prognosis, including heart failure and ischemic heart disease9,10. Severe IDA may lead to hemodynamic instability. Furthermore, preoperative anemia increases the risk of perioperative blood transfusion and is associated with postoperative mortality11.
Emerging evidence indicates that iron deficiency (ID) and iron deficiency anemia (IDA) may significantly disrupt bone metabolism. Medeiros et al.12,13 created an iron-deficient rat model by feeding them a low-iron diet to investigate the effects of iron deficiency on bones. The study revealed that rats fed a low-iron diet had significantly lower bone density, femoral cortical bone area, and vertebral trabecular number compared to the normal control group. Subsequent investigations by the same group demonstrated that iron chelation therapy impaired osteoblast mineralization capacity14. in vitro studies by Edwards et al.15 revealed that iron depletion (5 μM DFO) under osteogenic conditions significantly downregulated key osteogenic markers including osteocalcin, type I collagen (Col1), and dentin matrix protein 1 (DMP1), while simultaneously reducing alkaline phosphatase activity and mineralization potential. Zhao et al.16 further elucidated a dose-dependent biphasic effect of iron on osteoblast function, where mild deficiency stimulated activity but severe deficiency proved inhibitory. Furthermore, clinical studies have shown that, after adjusting for covariates such as protein and energy intake, higher iron intake has a beneficial effect on vertebral bone density in postmenopausal women17. Adequate iron intake can prevent anemia and directly increase oxygen supply to bones, thereby preventing osteoporosis17. Another epidemiological study indicated a significant negative correlation between anemia/low hemoglobin levels and bone mineral density18. A meta-analysis confirmed significantly lower serum iron levels in osteoporosis patients compared to healthy controls, establishing ID as an independent risk factor of osteoporosis19.
Although studies have shown that iron deficiency may lead to abnormal bone metabolism, its effects on the structure and function of the intervertebral disc (IVD) and the underlying mechanisms remain incompletely understood. Iron plays a pivotal role not only in cellular replication and DNA synthesis but also serves as an essential cofactor for prolyl hydroxylase, a key enzyme in collagen biosynthesis20,21. Previous studies have demonstrated that iron chelators and deferoxamine can suppress collagen synthesis in tendon cells and fibroblasts22,23. Given that the IVD—comprising the nucleus pulposus, annulus fibrosus, and cartilaginous endplates—contains abundant collagen as its primary extracellular matrix component, it is plausible that ID may impair collagen synthesis within the IVD, leading to structural and functional deterioration. In vivo studies have shown that pretreatment of mesenchymal stem cell implants with ascorbic acid and iron can significantly increase type II collagen expression and promote cartilage repair in the knee joints of miniature pigs24, highlighting iron’s critical role in cartilage regeneration. Zhang et al.25 demonstrated that iron deficiency, using deferoxamine and knockdown of DMT-1 and TfR1, can lead to decreased PolE expression and increased expression of apoptosis-related genes in nucleus pulposus cells. This study suggests that iron deficiency may contribute to intervertebral disc degeneration by inhibiting DNA polymerase expression in nucleus pulposus cells and promoting cell apoptosis.
Clinically, our recent studies have revealed that anemic patients with lower back pain exhibit more severe lumbar disc degeneration and a greater number of degenerated disc segments compared to non-anemic patients26,27. To elucidate the mechanistic relationship between iron levels and IVD degeneration, this study employs an iron-deficient rat model to assess the impact of iron deficiency on caudal IVD development. Additionally, we induce IVD degeneration via needle puncture to further evaluate the effects of ID on disc degeneration.
Materials and methods
Animals and diets
A total of 20, 3-week-old male Sprague Dawley rats were purchased from Liaoning Changsheng Biotechnology Co., Ltd. All experiments were approved by the Institutional Review Board of Hebei Normal University (protocol code 2023LLSC027) and complied with the National Institutes of Health Guidelines for the Care and Use of Laboratory Animals. Our experimental procedures on rats are consistent with the ARRIVE guidelines. The basic diet plan provided 20% of energy from protein, 5% from corn oil, 50% from sucrose, and 15% from cornstarch28. The remainder of the diet consisted of a mixture of vitamins and minerals. The normal diet contained about 113 mg Fe/kg, while the iron-deficient diet was formulated to contain 1–2.5 mg Fe/kg. The iron concentration of the iron-deficient diet was analyzed by atomic absorption spectroscopy to meet the required standard (< 2.5 mg/kg, Xi’an Guolian Quality Testing Technology Co., Ltd.).
The rats were randomly allocated into four groups (n = 5 per group): rats fed an iron-deficiency diet only (LN), rats fed an iron-deficiency diet and further underwent needle puncture (LP), rats fed a normal diet only (CN), and rats fed a normal diet and further underwent needle puncture (CP). All animals were housed individually in a controlled environment maintained at 22 ± 1 °C with 55 ± 10% relative humidity and a 12-h light–dark cycle. After 8-wk feeding, two groups of rats (LP and CP) underwent needle puncture surgery on caudal discs. Postoperative magnetic resonance (MR) imaging of coccygeal vertebrae was performed at 2 and 4 weeks following the surgical intervention. The rats were killed by an intraperitoneal overdosage injection of 10% pentobarbital, and the tails and blood samples were collected on 4 weeks after surgery.
Surgical procedure
The LP and CP groups underwent standardized intervertebral disc puncture surgery. Briefly, rats were anesthetized via intraperitoneal injection of 1% sodium pentobarbital (40 mg/kg). Following successful anesthesia, the tail was sterilized with povidone-iodine, and the rats were positioned in a prone posture. Under X-ray fluoroscopic guidance, the Co6/7, Co7/8, and Co8/9 intervertebral discs (IVDs) were identified. A 21G needle was inserted perpendicularly through the IVD to the contralateral skin. The needle tip was then retracted to the center of the tail, guided by another needle for comparison. The needle was rotated 360° and maintained in position for 30 s to induce consistent disc degeneration before removal. For the LN and CN groups, rats received anesthesia and tail disinfection but no needle puncture. Postoperatively, all animals were closely monitored for recovery and allowed unrestricted cage activity.
MRI examinations
Four weeks post-surgery, rats underwent the magnetic resonance imaging (MRI) examination. Mid-sagittal T2-weighted images were acquired. The parameters were as follows: repetition time (TR): 3000 ms, echo time (TE): 80 ms, field of view (FOV): 100 mm × 25 mm, and slice thickness: 1.2 mm. The severity of disc degeneration was assessed according to the Pfirrmann grading system29. The T2 signal intensity of the nucleus pulposus in the Co6/7 disc and the five adjacent caudal IVDs was measured using Philips Intellispace portal version 9.0. A standardized region of interest (ROI) of 2.3 mm2 was applied, with two independent measurements performed and averaged to ensure accuracy.
Tissue harvesting
After MRI examinations, the rats are fasted overnight. Following anesthesia, a midline abdominal incision is made to open the abdominal cavity and mediastinum, exposing the heart and venous sinus. Venous blood is collected by puncturing the venous sinus. One aliquot of blood was collected using EDTA tubes for haematological analysis, and an equal volume of blood is collected to obtain serum which was separated by centrifugation at 3000 r/min for 10 min at 4℃. Immediately following blood collection, the tail was amputated at its base for disc tissue harvesting. The coccygeal spine containing Co6/7, Co7/8 and Co8/9 intervertebral discs was carefully dissected with removal of surrounding soft tissues. A scalpel soaked in DEPC is used to cut the Co6/7 and Co7/8 discs, which are quickly placed in liquid nitrogen for preservation. Additionally, the Co8/9 disc with adjacent vertebral bodies was fixed in formaldehyde.
Haematological test
Hemoglobin concentration (Hb), red blood cell count (RBC), mean corpuscular volume (MCV), and hematocrit (Hct) were measured using an automated haematology analyzer BC-7500 (Mindray, Shenzhen, China). Serum iron (SI) and total iron binding capacity (TIBC) levels were determined using biochemical assay kits (Nanjing Jiancheng Bioengineering Institute). The serum hepcidin concentration was determined using enzyme-linked immunosorbent assay (ELISA) kits. The transferrin saturation (TS) was calculated using the formula: (Serum Iron/Total Iron Binding Capacity) × 100%.
Histopathologic analysis
The specimen was fixed with formaldehyde for 48 h, and then decalcified in EDTA for 4 weeks, after that dehydrated and embedded in paraffin. The tissues were cut into 4 μm sections. The midsagittal sections of the coccygeal disc were stained with safranin O‐fast green (S‐O) and hematoxylin‐eosin (HE). The structure of discs was observed by a microscope.
Three researchers independently evaluated the degree of intervertebral disc degeneration (IVDD) in using the histological scoring system established by Ji et al.30. This scoring system consists of five components: nucleus pulposus morphology, nucleus pulposus cell morphology, annulus fibrosus morphology, annulus fibrosus cell morphology, and the border between the annulus fibrosus and the nucleus pulposus. Each parameter was scored from 0 (normal) to 3 (severe degeneration), yielding a total possible score ranging from 0 (completely normal disc) to 15 (maximal degeneration). The final degeneration score for each specimen represented the mean value of the three independent assessments. The detailed scoring criteria are provided in Table 1. Since this scoring system does not incorporate endplate evaluation, we measured the thickness of the cartilaginous endplates in the four groups of rats. The measurement was based on the study by Abdel Fattah et al31. First, the morphology of the endplate cartilage was outlined, and then its thickness was measured at five equidistant points, with the average thickness expressed in micrometers (mm).
Immunohistochemistry
Firstly, sections are blocked with 10% goat serum albumin for 50 min. Then, they are incubated overnight at 4 °C with primary antibodies, including anti-Aggrecan, anti-Collagen II, anti-MMP13 and anti-FTL. Following incubation, the sections are washed with PBS and then incubated with secondary antibodies for 50 min at room temperature. Finally, the sections are washed again, and nucleus was stained by DAPI. Observe and capture images under a fluorescence microscope using a panoramic tissue cell quantitative scanner.
RT-qPCR
Collected the Co6/7 and Co7/8 discs from each rat and combine them into one sample. Total RNA was isolated using TRIzol Reagent (Invitrogen, USA) according to the manufacturer’s instructions. Total RNA (1 μg) of from each sample was used to synthesize cDNA. For PCR amplification, 20 μl of reaction volume included 10 μL of Ultra SYBR Mixture, 0.4 μL of each primer, 0.4 μL of diluted cDNA and 5.2 μL of RNase Free Water. The cycle threshold (CT) values were collected and normalized to the housekeeping gene β-actin. The ΔΔCt method was used to compare fold changes in mRNA expression between ID and non-ID groups (LN and CN, LP and CP). Primer sequences are listed in Table 2.
TdT-mediated dUTP nick end labeling (TUNEL) assay
Apoptosis was analyzed by TUNEL to detect DNA fragmentation according to the manufacturer’s instructions (Vazyme). The stained cells were measured by flow cytometry (BD, USA). Images were acquired with the fluorescence microscope (Nikon, Japan). The quantification of positive cells was obtained by Image-J.
Statistical analysis
All data were presented as mean ± standard deviation and analyzed by the SPSS 21.0 statistical software (IBM Corp., Armonk, NY). Comparisons of data between two groups were analyzed by independent sample t -test, and those among multiple groups were tested by one-way analysis of variance (ANOVA) or repeated measures ANOVA. The χ2-test was used for categorical variables. p < 0.05 was regarded as statistically significant.
Results
Successful establishment of iron deficiency anemia (IDA) model
Within 4 weeks of initiating the iron-deficient diet, characteristic signs of anemia became evident, including marked pallor of the nasal mucosa, pinnae, and periocular tissues (Fig. 1A), consistent with developing iron deficiency. After 12 weeks of feeding with the low-iron diet, the mean RBC count, mean Hb level, mean Hct value, and MCV in the LN and LP groups of rats were significantly lower than those in the corresponding control groups (Fig. 1B–E, P < 0.05). In addition, the mean SI level, mean TS level, and mean hepcidin level in the LN and LP groups of rats were significantly lower than those in the control group (Fig. 1F, G, H P < 0.05), while the mean TIBC was significantly higher than that of the control group (Fig. 1I, P < 0.05). These results satisfy established diagnostic criteria for IDA in rodent models.
The appearance of the rats and the hematological test results confirmed the successful establishment of the IDA model. (A) The color of the rats’ noses, ears, and eyelids turns light pink within 4-wk consuming an iron-deficient diet. After 12 weeks of feeding with the low-iron diet, (B–E) the mean RBC count, mean Hb level, mean Hct value, and MCV in the LN and LP groups of rats were significantly lower than those in the corresponding control groups which suggested that the rats exhibited microcytic hypochromic anemia. Besides, (F–H) the mean SI level, mean TS level, and mean hepcidin level in the LN and LP groups of rats were significantly lower than those in the control group, (I) the mean TIBC was significantly higher than that of the control group. Data are presented as mean ± SD (n = 5). *P < 0.05, **P < 0.01, ***P < 0.001.
Iron deficiency impairs the structural development of coccygeal intervertebral discs
After 12 weeks of iron-deficient feeding, MRI analysis revealed significantly reduced T2 signal intensity in the nucleus pulposus of Co6/7 and Co10/11 discs (Fig. 2A, P < 0.05) and a higher incidence of degenerative gray banding (12/18 vs 5/18 in controls, P < 0.05) (Fig. 2B). Histological examination demonstrated marked microstructural alterations, including decreased vacuolated notochordal cells with increased chondrocyte-like cell proliferation (Fig. 2C, D), disrupted annulus fibrosus organization exhibiting tearing and distortion, and significantly thinner cartilaginous endplates. (0.05 ± 0.01 mm vs 0.11 ± 0.01 mm in controls, P < 0.001) (Fig. 2E, F). The histological score of the intervertebral disc in the LN group (4.60 ± 0.89) was significantly higher than that in the control group (3.20 ± 0.84) (Fig. 2G, P < 0.05). These results demonstrate that iron deficiency adversely affects intervertebral disc development prior to skeletal maturity.
The MRI and histological results suggested that the development of the coccygeal intervertebral disc was affected. (A) The T2 signal intensity of the Co6/7 and Co10/11 nucleus pulposus in the LN group was significantly lower than the CN group. Data are presented as mean ± SD (n = 3). *P < 0.05. (B) The incidence of gray banding on T2 images of the LN group was significantly higher than that in the control group (77.8% vs. 27.8%, *P < 0.05). (C, D) The number of vacuolated notochordal cells in the caudal discs of LN group was less than that in the CN group. Instead, non-vacuolated chondrocyte-like cells were frequently observed in the LN group. Scale bar = 100 μM and 200 μM. (E, F) The average cartilage endplate thickness in the LN group was significantly thinner than that in the CN group. Scale bar = 100 μM. Data are presented as mean ± SD (n = 5). ***P < 0.001. (G) The histological score in the LN group was significantly higher than that in the control group. Data are presented as mean ± SD (n = 5). *P < 0.05.
Iron deficiency suppresses the expression of type II collagen in caudal intervertebral discs
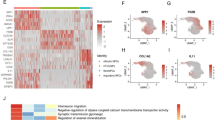
After 12 weeks of feeding with a low-iron diet, the LN group exhibited upregulated transferrin receptor 1 (TfR1) gene expression and downregulated ferroportin 1 (FPN1) expression (Fig. 3A, B, P < 0.05), indicating compensatory iron regulatory mechanisms, while immunofluorescence revealed significantly reduced ferritin light chain (FTL) expression in nucleus pulposus cells (Fig. 3C, P < 0.05). Importantly, these iron metabolism disturbances were associated with markedly decreased type II collagen (Col2) expression at both mRNA (Fig. 3D, P < 0.05) and protein levels (Fig. 3E, P < 0.05) in the nucleus pulposus, though no significant differences were observed in aggrecan (Agg) or matrix metalloproteinase 13 (MMP13) expression between groups (Fig. 3F, G). These findings demonstrate that iron deficiency specifically impairs type II collagen synthesis in intervertebral discs.
Iron deficiency in the IVD leads to restricted synthesis of type II collagen. (A, B) the expression of the transferrin receptor 1 (TfR1) gene in the LN group was significantly higher than that in the CN group, while the expression of the ferroportin 1 (FPN1) gene was significantly lower than that in the CN group. (C) Compared to the CN group, the expression of ferritin light chain (FTL) in the nucleus pulposus cells (NPCs) was significantly reduced in the LN group. These findings suggested that the ID condition existed in intervertebral discs. (D, E) The type II collagen (Col2) expression in the nucleus pulposus of the LN group was significantly lower than that in the CN group. (F, G) No significant differences were found with regard to the expression of aggrecan (Agg) and matrix metalloproteinase 13 (MMP13) between the two groups. Data are presented as mean ± SD (n = 3). *P < 0.05, **P < 0.01.
The apoptosis of NPCs in iron-deficient anemia rats is not markedly exacerbated
Quantitative analysis of TUNEL staining demonstrated comparable apoptotic signal intensities between the LN and CN groups (Fig. 4). These findings suggest that the pathological changes induced by iron deficiency may primarily involve alterations in extracellular matrix metabolism rather than significant cellular loss through apoptotic pathways.
The TUNEL staining results showed that there was no significant difference in the intensity of apoptotic signals in the NPCs between the LN and CN group. Data are presented as mean ± SD (n = 3).
Anemia did not worsen the histological score of IVDs following acupuncture intervention
After 4 weeks of modeling, MRI assessment demonstrated comparable degrees of disc degeneration between LP and CP groups, with no statistical differences in either overall degeneration (Pfirrmann grades III-V) or severe degeneration (grades IV-V) incidence (Table 3). Histological analysis confirmed degenerative changes in both groups post-puncture (Fig. 5A, B), though the LP group exhibited significantly thinner cartilage endplates (0.05 ± 0.01 mm vs 0.07 ± 0.01 mm, P < 0.01) (Fig. 5C, D). Notably, histological scoring showed no significant difference between groups (LP: 9.40 ± 4.40 vs CP: 11.20 ± 4.40) (Fig. 5E), indicating that while iron deficiency may affect endplate morphology, it does not appear to exacerbate the overall histopathological severity of puncture-induced disc degeneration.
The histopathologic results after 4 weeks of puncture modeling. (A, B) both groups of rats showed signs of degeneration in the intervertebral discs, such as: collapse of the intervertebral space, disordered arrangement of the annulus fibrosus structure, unclear boundary between the nucleus pulposus and the annulus fibrosus, significant reduction or even disappearance of the nucleus pulposus, fewer nucleus pulposus cells with clustered aggregation, and a marked decrease in extracellular matrix content. Scale bar = 100 μM and 200 μM. (C, D) The cartilage endplate thickness in the LP group was significantly thinner than that in the CP group. Scale bar = 100 μM. Data are presented as mean ± SD (n = 5). **P < 0.01. (E) No significant difference was found in the histological scores between the LP and CP group. Data are presented as mean ± SD (n = 5).
The effect of intervertebral disc degeneration on the expression of iron metabolism related genes and type II collagen, AGG and MMP13 expression
The results indicate that four weeks after acupuncture modeling, the LP group exhibited upregulated TfR1 gene expression (Fig. 6A, P < 0.05), and downregulated FPN1 gene expression (Fig. 6B, P < 0.05), accompanied by significantly reduced FTL levels (Fig. 6C, P < 0.05), collectively indicating impaired iron homeostasis in degenerated discs. While apoptosis sensitivity remained comparable between groups (no significant difference in Bcl2/Bax ratio) (Fig. 6D), the LP group demonstrated significantly decreased type II collagen (Col2) gene expression (Fig. 6E, P < 0.05), with a similar but non-significant trend at the protein level (Fig. 6F). Notably, neither Agg nor MMP13 expression showed significant intergroup differences (Fig. 6G, H), highlighting the selective impact of iron dysregulation on collagen metabolism during disc degeneration.
The effects of puncture-induced IVD degeneration on the expression of iron metabolism related genes and type II collagen, AGG and MMP13 expression. (A) The expression of the TfR1 gene in the LP group was significantly higher than that in the CP group, while (B) the expression of the FPN1 gene was significantly lower than that in the CP group. (C) Compared to the CP group, the expression of FTL in the LP group was significantly reduced. These findings suggest that the iron level in the IVDs of rats in the LP group were lower than that in the CP group. (D) No significant difference was found in the Bcl2/Bax ratio between the two groups, suggesting that there was no notable difference in the sensitivity to apoptosis in the IVDs of the two groups. (E, F) The LP group showed significantly lower Col2 gene expression compared to the CP group, and a similar trend was observed at the protein level, although without significant difference. (G, H) No significant difference was identified in Agg and MMP13 expression between the two groups. Data are presented as mean ± SD (n = 3). *P < 0.05, **P < 0.01.
ID did not exacerbate the disc degeneration caused by acute injuries
The TUNEL staining analysis revealed comparable apoptotic signal intensities between the LP and CP groups following puncture modeling (Fig. 7), demonstrating that iron deficiency did not significantly alter cellular apoptosis rates in degenerated discs. When integrated with our histological and PCR findings, these results collectively indicate that while iron deficiency impairs normal intervertebral disc development, it does not appear to exacerbate the degenerative changes induced by mechanical puncture injury.
TUNEL staining results showed that, after puncture modeling, the intensity of apoptotic signals in the LP group was not significantly different from that of the CP group. Data are presented as mean ± SD (n = 3).
Discussion
This study successfully established an iron-deficiency anemia (IDA) rat model to systematically investigate the impact of iron deficiency (ID) on intervertebral disc development and degeneration. Our findings demonstrate that ID significantly impairs normal disc development, as evidenced by multiple pathological indicators: quantitative MRI revealed markedly decreased T2 signal intensity and significantly higher incidence of degenerative gray-level bands in IDA rats compared to controls. Histopathological examination showed characteristic developmental abnormalities, including notable depletion of notochordal cells and significantly reduced cartilage endplate thickness. At the molecular level, we observed substantial downregulation of Col2 gene expression (P < 0.05), indicating impaired extracellular matrix synthesis. To evaluate whether ID exacerbates disc degeneration, we subsequently induced mechanical degeneration using a standardized needle puncture protocol. While both groups developed comparable degrees of puncture-induced degeneration based on MRI Pfirrmann grading and histological scoring, our results unexpectedly revealed that the pre-existing ID condition did not significantly worsen the degenerative progression.
Iron plays a crucial role in biological processes. For bone and cartilage tissues, the condition of iron deficiency primarily affects collagen synthesis and osteoblast mineralization function32. Iron is a component of prolyl 4-hydroxylase (P4H), which converts proline into hydroxyproline, a critical element for collagen cross-linking33. Iron deficiency may impair collagen cross-linking, leading to increased bone fragility. Medeiros et al.12 fed rats a low-iron diet, and the results showed that the experimental rats had reduced cortical bone in the femur and tibia, with increased medullary cavity width. Micro-CT imaging revealed that, compared to the control group, iron-deficient rats had reduced total bone mass, fewer and thinner trabeculae in cancellous bone, and increased trabecular spacing. These results indicate that iron deficiency not only affects overall bone mass but also leads to osteoporosis. Additionally, a study by Diaz-Castro et al.34 showed that iron-deficient anemic rats had reduced levels of N-terminal propeptide of type I procollagen in their blood, suggesting a decrease in bone matrix content.
Unlike bone tissue, the intervertebral disc lacks a vascular structure. Nutrients required by the nucleus pulposus cells primarily enter through diffusion from the blood vessels surrounding the disc. The main pathways for nutrient delivery are the cartilage endplate-nucleus pulposus (CEP-NP) pathway and the peripheral annulus fibrosus (AF) pathway35. The CEP-NP pathway mainly supplies nutrients to the cells in the nucleus pulposus and the inner annulus fibrosus, while the outer annulus region is primarily nourished through the AF pathway36,37. When the nutrient supply to the intervertebral disc decreases to a critical level, the number of cells within the disc will decrease accordingly38,39. Prior studies reported that both iron deficiency or iron overload accelerate disc degeneration25,40,41,42,43. Zhang et al.25 conducted serum iron measurements on 96 patients with intervertebral disc degeneration. The study found that as the degree of disc degeneration increased, the serum iron levels of the patients gradually decreased, suggesting that patients with severe lumbar disc degeneration may experience iron deficiency. In vitro experiments indicated that using deferoxamine and knockdown of DMT-1 and TfR1, can lead to decreased PolE expression and increased expression of apoptosis-related genes in nucleus pulposus cells. Shan et al.40 found that the iron level in herniated nucleus pulposus was significantly higher than that in the control group, mainly due to the formation of new blood vessels, leading to heme iron deposition and inducing ferroptosis of nucleus pulposus cells and disc degeneration. Wang et al.41 reported that patients with severe single-level disc degeneration had significantly higher serum ferritin levels compared to patients with mild disc degeneration. In vivo experiments have further confirmed that iron overload can lead to degeneration and calcification of the cartilage endplate via oxidative stress and ferroptosis, thereby causing disc degeneration. Lu et al.42 detected the expression of FTL and FPN in degenerated and normal nucleus pulposus. The study found that the expression of FTL in the degenerated nucleus pulposus was significantly higher than that in the normal nucleus pulposus, while the expression of FPN was significantly lower. The authors suggested that the reduced expression of FPN in the degenerated nucleus pulposus leads to intracellular iron overload, which is an important cause of intervertebral disc degeneration.
To our knowledge, this is the first in vivo study specifically examining the impact of iron deficiency (ID) on intervertebral disc biology. Our molecular analyses revealed significant dysregulation of iron metabolism in the caudal discs of iron-deficient anemic (IDA) rats, with the LN and LP groups demonstrating markedly elevated transferrin receptor 1 (TfR1) expression and substantially reduced ferroportin 1 (FPN1) expression compared to controls. Immunofluorescence staining revealed that ferritin expression in the intervertebral discs of the LN and LP groups was significantly lower than that in the control group. This comprehensive demonstration of altered iron homeostasis in the intervertebral disc microenvironment establishes a crucial foundation for understanding the role of iron metabolism in disc pathophysiology and suggests potential mechanisms underlying the observed developmental impairments in IDA rats.
MRI scans revealed that the T2 signal intensity in the caudal discs of the LN group was lower than that of the control group, with a significantly higher incidence of gray-level bands within the discs. According to the Pfirrmann grading system, the appearance of gray-level bands corresponds to grade II degeneration. This suggests that, at this point, the caudal intervertebral discs in the LN group had already begun to show mild degeneration. We acknowledge that although statistical significance was only observed at specific segments (C06/7 and C010/11), other segments exhibited a similar degenerative trend. The lack of statistical significance at other levels may partly result from limited sample size or short duration of intervention.
Further histological examinations revealed that the number of notochordal cells with vacuole structures in the nucleus pulposus of the LN group was significantly reduced, while the number of round cells had increased. Previous research suggests that notochordal cells are closely related to intervertebral disc degeneration. Notochordal cells perform various functions, such as generating chondrocyte-like cells44, recruiting chondrocytes from the cartilage endplate into the nucleus pulposus45, stimulating the differentiation of mesenchymal stem cells into chondrocytes46, and inhibiting the invasion of nerve or endothelial cells into the disc47. In some vertebrates, notochordal cells persist throughout life, significantly delaying disc degeneration48. Compared to chondrocyte-like cells, notochordal cells are more susceptible to nutritional deficiencies49. Therefore, we thought that iron deficiency may be one of the causes of the reduction in notochordal cell numbers, though the exact mechanism behind this reduction requires further investigation.
Previous histological scoring systems for intervertebral disc degeneration have overlooked changes in the morphology of the cartilage endplate. In this study, we measured the thickness of the cartilage endplates in the various groups. We found that the cartilage endplate thickness in the LN group was significantly smaller than that of the control group. This indicates that iron deficiency affects the development of the cartilage endplate. It was postulated that the cartilage endplate is more susceptible to the effects of iron deficiency due to its proximity to surrounding blood supply compared to the nucleus pulposus.
This study further examined the expression of genes related to IVDD. The results showed that the expression of Agg in the LN group did not differ significantly from that of the control group. However, the expression of the Col2 gene was significantly reduced, which is consistent with the immunofluorescence results. Previous studies have indicated that Col2 protein provides essential structural integrity to the extracellular matrix of the NP, helping to retain proteoglycans and thereby maintain hydration50,51. In our study, despite no significant changes in aggrecan expression, the marked reduction in Col2 could impair the structural integrity of the NP matrix, potentially affecting its ability to retain water and consequently resulting in decreased MRI signal intensity and the appearance of gray-level bands.
This study not only explored the effects of ID on the development of caudal discs but also investigated its impact on disc degeneration. While we confirmed that ID significantly impairs normal disc development, our acupuncture-induced degeneration model yielded unexpected findings: contrary to our initial hypothesis, IDA (LP) rats showed comparable degenerative outcomes to controls (CP) in terms of MRI parameters, histological scores, and protein expression patterns—with LP group scores even trending slightly lower than CP. This paradox may be explained by fundamental differences between clinical disc degeneration and experimental models. Human disc degeneration typically progresses through chronic, multifactorial processes where sustained iron deficiency and tissue hypoxia likely disrupt normal metabolic homeostasis over time. In contrast, our needle puncture model represents an acute injury paradigm characterized by rapid inflammatory cascades—evidenced by postoperative tail swelling and well-documented upregulation of pro-inflammatory cytokines (IL-1β, TNF-α, IL-6) within days of injury52,53. We postulate that in this acute setting, iron deficiency may exert protective effects by attenuating iron-dependent oxidative stress and subsequent inflammatory responses, consistent with established roles of iron chelators in mitigating oxidative damage54,55. These findings highlight the complex, context-dependent nature of iron’s role in disc pathophysiology and underscore the need for future longitudinal studies examining ID effects on spontaneous age-related degeneration to better approximate clinical progression.
This study has several limitations. Firstly, although altered expression of iron-related genes was observed, the downstream functional effects on specific cellular pathways such as hypoxia response, extracellular matrix (ECM) turnover, and inflammation were not fully investigated. Further studies exploring these molecular pathways in detail are needed. Secondly, the histological scoring system applied in this study did not include evaluation of the cartilage endplate, which is notably affected under iron deficiency conditions. Lastly, certain critical analyses, especially molecular assays, were based on a limited sample size (n = 3), weakening the statistical robustness. Subsequent investigations with larger sample sizes are necessary to validate these findings.
Conclusion
This study successfully established an iron deficiency anemia (IDA) rat model to systematically investigate the impact of iron deprivation on intervertebral disc pathophysiology. Our findings demonstrate that iron deficiency adversely affected intervertebral discs development, characterized by three key pathological alterations: (1) morphological transformation of nucleus pulposus cells from vacuolated notochordal to chondrocyte-like phenotypes, (2) substantial thinning of cartilage endplates, and (3) marked suppression of type II collagen synthesis. However, in our needle puncture-induced degeneration model, pre-existing iron deficiency did not exacerbate traumatic disc degeneration, as evidenced by comparable Pfirrmann grades and histological scores between IDA and control groups.
Data availability
All major data supporting the findings of this study are available within the article. Raw data supporting the findings are available from HR.C. and YZ.C. upon reasonable request.
References
Pasricha, S. R., Tye-Din, J., Muckenthaler, M. U. & Swinkels, D. W. Iron deficiency. Lancet (Lond., Engl.) 397, 233–248. https://doi.org/10.1016/s0140-6736(20)32594-0 (2021).
Ropele, S. & Langkammer, C. Iron quantification with susceptibility. NMR Biomed. https://doi.org/10.1002/nbm.3534 (2017).
Fleming, R. E. & Ponka, P. Iron overload in human disease. N. Engl. J. Med. 366, 348–359. https://doi.org/10.1056/NEJMra1004967 (2012).
Andrews, N. C. Disorders of iron metabolism. N. Engl. J. Med. 341, 1986–1995. https://doi.org/10.1056/nejm199912233412607 (1999).
Kassebaum, N. J. et al. A systematic analysis of global anemia burden from 1990 to 2010. Blood 123, 615–624. https://doi.org/10.1182/blood-2013-06-508325 (2014).
Namaste, S. M. et al. Adjusting ferritin concentrations for inflammation: Biomarkers reflecting inflammation and nutritional determinants of anemia (BRINDA) project. Am. J. Clin. Nutr. 106, 359s–371s. https://doi.org/10.3945/ajcn.116.141762 (2017).
Mei, Z. et al. Assessment of iron status in US pregnant women from the national health and nutrition examination survey (NHANES), 1999–2006. Am. J. Clin. Nutr. 93, 1312–1320. https://doi.org/10.3945/ajcn.110.007195 (2011).
Vos, T. et al. Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the global burden of disease study 2016. Lancet (Lond., Engl.) 390, 1211–1259. https://doi.org/10.1016/s0140-6736(17)32154-2 (2017).
Grote Beverborg, N. et al. Differences in clinical profile and outcomes of low iron storage vs defective iron utilization in patients with heart failure: Results From the DEFINE-HF and BIOSTAT-CHF studies. JAMA Cardiol. 4, 696–701. https://doi.org/10.1001/jamacardio.2019.1739 (2019).
Perera, C. A., Biggers, R. P. & Robertson, A. Deceitful red-flag: angina secondary to iron deficiency anaemia as a presenting complaint for underlying malignancy. BMJ Case Rep. https://doi.org/10.1136/bcr-2019-229942 (2019).
Musallam, K. M. et al. Preoperative anaemia and postoperative outcomes in non-cardiac surgery: A retrospective cohort study. Lancet (Lond., Engl.) 378, 1396–1407. https://doi.org/10.1016/s0140-6736(11)61381-0 (2011).
Medeiros, D. M., Plattner, A., Jennings, D. & Stoecker, B. Bone morphology, strength and density are compromised in iron-deficient rats and exacerbated by calcium restriction. J. Nutr. 132, 3135–3141. https://doi.org/10.1093/jn/131.10.3135 (2002).
Medeiros, D. M., Stoecker, B., Plattner, A., Jennings, D. & Haub, M. Iron deficiency negatively affects vertebrae and femurs of rats independently of energy intake and body weight. J. Nutr. 134, 3061–3067. https://doi.org/10.1093/jn/134.11.3061 (2004).
Parelman, M., Stoecker, B., Baker, A. & Medeiros, D. Iron restriction negatively affects bone in female rats and mineralization of hFOB osteoblast cells. Exp. Biol. Med. (Maywood, N.J.) 231, 378–386. https://doi.org/10.1177/153537020623100403 (2006).
Edwards, D. F. 3rd. et al. Differential iron requirements for osteoblast and adipocyte differentiation. JBMR Plus 5, e10529. https://doi.org/10.1002/jbm4.10529 (2021).
Zhao, G. Y. et al. A comparison of the biological activities of human osteoblast hFOB1.19 between iron excess and iron deficiency. Biol. Trace Elem. Res. 150, 487–495. https://doi.org/10.1007/s12011-012-9511-9 (2012).
Abraham, R. et al. Dietary determinants of post-menopausal bone loss at the lumbar spine: A possible beneficial effect of iron. Osteoporos. Int. 17, 1165–1173. https://doi.org/10.1007/s00198-005-0033-6 (2006).
Cesari, M. et al. Bone density and hemoglobin levels in older persons: results from the InCHIANTI study. Osteoporos. Int. 16, 691–699. https://doi.org/10.1007/s00198-004-1739-6 (2005).
Zheng, J., Mao, X., Ling, J., He, Q. & Quan, J. Low serum levels of zinc, copper, and iron as risk factors for osteoporosis: A meta-analysis. Biol. Trace Elem. Res. 160, 15–23. https://doi.org/10.1007/s12011-014-0031-7 (2014).
Ikeda, H., Wu, G. Y. & Wu, C. H. Evidence that an iron chelator regulates collagen synthesis by decreasing the stability of procollagen mRNA. Hepatology (Baltimore, MD) 15, 282–287. https://doi.org/10.1002/hep.1840150218 (1992).
Hill, C. H. et al. Dietary iron deficiency compromises normal development of elastic fibers in the aorta and lungs of chicks. J. Nutr. 137, 1895–1900. https://doi.org/10.1093/jn/137.8.1895 (2007).
Rowe, L. B. & Schwarz, R. I. Role of procollagen mRNA levels in controlling the rate of procollagen synthesis. Mol. Cell. Biol. 3, 241–249. https://doi.org/10.1128/mcb.3.2.241-249.1983 (1983).
Hunt, J., Richards, R. J., Harwood, R. & Jacobs, A. The effect of desferrioxamine on fibroblasts and collagen formation in cell cultures. Br. J. Haematol. 41, 69–76. https://doi.org/10.1111/j.1365-2141.1979.tb03682.x (1979).
Theruvath, A. J. et al. Ascorbic acid and iron supplement treatment improves stem cell-mediated cartilage regeneration in a Minipig model. Am. J. Sports Med. 49, 1861–1870. https://doi.org/10.1177/03635465211005754 (2021).
Zhang, C. et al. Iron deficiency accelerates intervertebral disc degeneration through affecting the stability of DNA polymerase epsilon complex. Am. J. Transl. Res. 10, 3430–3442 (2018).
Chang, H. et al. Association between anemia and lumbar disc degeneration in patients with low back pain: An observational retrospective study. Eur. Spine J.: Off. Publ. Eur. Spine Soc., Eur. Spinal Deform. Soc. Eur. Sec. Cerv. Spine Res. Soc. 32, 2059–2068. https://doi.org/10.1007/s00586-023-07652-1 (2023).
Chang, H., Gao, X., Li, X., Zhao, R. & Ding, W. Anemia was associated with multilevel lumbar disc degeneration in patients with low back pain: a single-center retrospective study. Eur. Spine J.: Off. Publ. Eur. Spine Soc., Eur. Spinal Deform. Soc. Eur. Sec. Cerv. Spine Res. Soc. 31, 1897–1905. https://doi.org/10.1007/s00586-022-07259-y (2022).
Diet, C. B., Diet, U. & Diet, N. P. Report of the American Institute of Nurtition ad hoc Committee on Standards for Nutritional Studies. J. Nutr. 107, 1340–1348. https://doi.org/10.1093/jn/107.7.1340 (1977).
Pfirrmann, C. W., Metzdorf, A., Zanetti, M., Hodler, J. & Boos, N. Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine 26, 1873–1878. https://doi.org/10.1097/00007632-200109010-00011 (2001).
Ji, M. L. et al. Preclinical development of a microRNA-based therapy for intervertebral disc degeneration. Nat. Commun. 9, 5051. https://doi.org/10.1038/s41467-018-07360-1 (2018).
Abdel Fattah, I. O. & Nasr El-Din, W. A. Granulocyte-colony stimulating factor improves intervertebral disc degeneration in experimental adult male rats: A microscopic and radiological study. Anat. Rec. (Hoboken, N.J.:2007) 304, 787–802. https://doi.org/10.1002/ar.24519 (2021).
Medeiros, D. M. Copper, iron, and selenium dietary deficiencies negatively impact skeletal integrity: A review. Exp. Biol. Med. (Maywood, N.J.) 241, 1316–1322. https://doi.org/10.1177/1535370216648805 (2016).
Gorres, K. L. & Raines, R. T. Direct and continuous assay for prolyl 4-hydroxylase. Anal. Biochem. 386, 181–185. https://doi.org/10.1016/j.ab.2008.11.046 (2009).
Díaz-Castro, J. et al. Severe nutritional iron-deficiency anaemia has a negative effect on some bone turnover biomarkers in rats. Eur. J. Nutr. 51, 241–247. https://doi.org/10.1007/s00394-011-0212-5 (2012).
Urban, J. P., Holm, S. & Maroudas, A. Diffusion of small solutes into the intervertebral disc: as in vivo study. Biorheology 15, 203–221. https://doi.org/10.3233/bir-1978-153-409 (1978).
van der Werf, M., Lezuo, P., Maissen, O., van Donkelaar, C. C. & Ito, K. Inhibition of vertebral endplate perfusion results in decreased intervertebral disc intranuclear diffusive transport. J. Anat. 211, 769–774. https://doi.org/10.1111/j.1469-7580.2007.00816.x (2007).
Rajasekaran, S. et al. ISSLS prize winner: A study of diffusion in human lumbar discs: A serial magnetic resonance imaging study documenting the influence of the endplate on diffusion in normal and degenerate discs. Spine 29, 2654–2667. https://doi.org/10.1097/01.brs.0000148014.15210.64 (2004).
Zhu, Q., Jackson, A. R. & Gu, W. Y. Cell viability in intervertebral disc under various nutritional and dynamic loading conditions: 3d finite element analysis. J. Biomech. 45, 2769–2777. https://doi.org/10.1016/j.jbiomech.2012.08.044 (2012).
Shirazi-Adl, A., Taheri, M. & Urban, J. P. Analysis of cell viability in intervertebral disc: Effect of endplate permeability on cell population. J. Biomech. 43, 1330–1336. https://doi.org/10.1016/j.jbiomech.2010.01.023 (2010).
Shan, L. et al. Increased hemoglobin and heme in MALDI-TOF MS analysis induce ferroptosis and promote degeneration of herniated human nucleus pulposus. Mol. Med. (Cambridge, Mass) 27, 103. https://doi.org/10.1186/s10020-021-00368-2 (2021).
Wang, W. et al. Iron overload promotes intervertebral disc degeneration via inducing oxidative stress and ferroptosis in endplate chondrocytes. Free Radical Biol. Med. 190, 234–246. https://doi.org/10.1016/j.freeradbiomed.2022.08.018 (2022).
Lu, S. et al. Ferroportin-dependent iron homeostasis protects against oxidative stress-induced nucleus pulposus cell ferroptosis and ameliorates intervertebral disc degeneration in vivo. Oxid. Med. Cell. Longev. 2021, 6670497. https://doi.org/10.1155/2021/6670497 (2021).
Li, Y. et al. Silencing ATF3 might delay TBHP-induced intervertebral disc degeneration by repressing NPC ferroptosis, apoptosis, and ECM degradation. Oxid. Med. Cell. Longev. 2022, 4235126. https://doi.org/10.1155/2022/4235126 (2022).
Kim, J. H. et al. Differentiation of intervertebral notochordal cells through live automated cell imaging system in vitro. Spine 34, 2486–2493. https://doi.org/10.1097/BRS.0b013e3181b26ed1 (2009).
Kim, K. W. et al. Notochordal cells stimulate migration of cartilage end plate chondrocytes of the intervertebral disc in in vitro cell migration assays. Spine J.: Off. J. N. Am. Spine Soc. 9, 323–329. https://doi.org/10.1016/j.spinee.2008.05.003 (2009).
Korecki, C. L., Taboas, J. M., Tuan, R. S. & Iatridis, J. C. Notochordal cell conditioned medium stimulates mesenchymal stem cell differentiation toward a young nucleus pulposus phenotype. Stem Cell Res. Ther. 1, 18. https://doi.org/10.1186/scrt18 (2010).
Purmessur, D. et al. Intact glycosaminoglycans from intervertebral disc-derived notochordal cell-conditioned media inhibit neurite growth while maintaining neuronal cell viability. Spine J.: Off. J. N. Am. Spine Soc. 15, 1060–1069. https://doi.org/10.1016/j.spinee.2015.02.003 (2015).
Wang, F. et al. Formation, function, and exhaustion of notochordal cytoplasmic vacuoles within intervertebral disc: current understanding and speculation. Oncotarget 8, 57800–57812. https://doi.org/10.18632/oncotarget.18101 (2017).
Guehring, T. et al. Notochordal intervertebral disc cells: sensitivity to nutrient deprivation. Arthritis Rheum. 60, 1026–1034. https://doi.org/10.1002/art.24407 (2009).
Sivan, S. S., Wachtel, E. & Roughley, P. Structure, function, aging and turnover of aggrecan in the intervertebral disc. Biochem. Biophys. Acta. 3181–3189, 2014. https://doi.org/10.1016/j.bbagen.2014.07.013 (1840).
Mwale, F., Roughley, P. & Antoniou, J. Distinction between the extracellular matrix of the nucleus pulposus and hyaline cartilage: A requisite for tissue engineering of intervertebral disc. Eur. Cells Mater. 8, 58–63. https://doi.org/10.22203/ecm.v008a06 (2004).
He, M. et al. P14ARF inhibits regional inflammation and vascularization in intervertebral disc degeneration by upregulating TIMP3. Am. J. Physiol. Cell Physiol. 318, C751-c761. https://doi.org/10.1152/ajpcell.00271.2019 (2020).
Zhang, Y. et al. Effect of hyperlipidaemia to accelerate intervertebral disc degeneration in the injured rat caudal disc model. J. Orthop. Sci.: Off. J. Jpn. Orthop. Assoc. 24, 42–49. https://doi.org/10.1016/j.jos.2018.08.006 (2019).
Arent, C. O. et al. Synergist effects of n-acetylcysteine and deferoxamine treatment on behavioral and oxidative parameters induced by chronic mild stress in rats. Neurochem. Int. 61, 1072–1080. https://doi.org/10.1016/j.neuint.2012.07.024 (2012).
Khoshlahni, N., Sagha, M., Mirzapour, T., Zarif, M. N. & Mohammadzadeh-Vardin, M. Iron depletion with deferoxamine protects bone marrow-derived mesenchymal stem cells against oxidative stress-induced apoptosis. Cell Stress Chaperones 25, 1059–1069. https://doi.org/10.1007/s12192-020-01142-9 (2020).
Funding
This research was funded by the Hebei Natural Science Foundation Youth Fund (No. H2023206329).
Author information
Authors and Affiliations
Contributions
Conceptualization, H.R.C. and Y.Z.C.; methodology, H.R.C., S.M.K., H.R.L. and L.H.W.; software, S.M.K. and C.C.L.; validation, L.H.W. and C.C.L.; formal analysis, H.R.C.; investigation, H.R.C. and S.M.K.; resources, H.R.C.; data curation, H.R.C. and D.Z.; writing—original draft preparation, H.R.C.; writing—review and editing, Y.Z.C.; visualization, D.Z.; supervision, Y.Z.C.; funding acquisition, H.R.C. All authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Chang, H., Kang, S., Li, C. et al. The dual effects of iron deficiency on intervertebral disc development and on acute injury-induced disc degeneration. Sci Rep 15, 19323 (2025). https://doi.org/10.1038/s41598-025-04388-4
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-04388-4
Keywords
This article is cited by
-
Establishment of rabbit models of lumbar disc degeneration using three methods monitored via X-ray: a comparative study
Journal of Orthopaedic Surgery and Research (2025)