Abstract
Degeneration of intervertebral discs is a significant factor in chronic lower back pain, impacting millions annually. Existing studies propose a potential link between lipids and disc disease, though causal relationships remain unclear. The objective of this study is to explore the causal connections between lipids, lower back pain, disc degeneration, and the risk of sciatica In this research, we utilized a comprehensive GWAS dataset encompassing 179 lipid traits to explore the causal connections between lipids and the susceptibility to conditions such as lower back pain (LBP), intervertebral disc degeneration (IVDD), and sciatica. To establish causality, we employed two-sample Mendelian randomization, supplemented by Bayesian model averaging for verification. Our assessment of diversity and mutual influence involved Cochran’s Q test, MR-Egger intercept assessment, and MR-PRESSO. Additionally, we performed a sensitivity analysis by systematically excluding individual elements to gauge their impact on outcomes in Mendelian randomization. Lastly, bidirectional Mendelian randomization was conducted to explore potential inverse associations between lipids and IVDD. Analyzing 179 lipidomic features as exposures and IVDD, LBP, and sciatica as outcomes, this study reveals significant causal relationships of glycerophospholipids, sterols, and glycerolipids with the risk of IVDD, LBP, and sciatica. Phosphatidylcholine, triglycerides, and sterols consistently exerted risk influences on IVDD, while phosphatidylethanolamine (O-16:1_18:2) among glycerophospholipids exhibited a protective effect (OR: 0.927–0.998, P < 0.05). Regarding LBP, sphingomyelin (d38:2) in sphingolipids demonstrated a protective effect (OR: 0.925–0.997, P < 0.05). For sciatica, triglycerides exhibited a risk influence, with varying effects observed for phosphatidylcholine and sterols with different molecular structures. Notably, sterol ester (27:1/16:1) consistently showed a risk effect across all three conditions. Our research provides valuable insights into how certain lipids are linked to the risks of LBP, IVDD, and sciatica. Our findings indicate that phosphatidylcholine and triglycerides may increase the incidence of IVDD, LBP, and sciatica, suggesting potential adverse effects. In contrast, sphingomyelin appears to reduce the occurrence of LBP and sciatica, indicating a protective role. Sterol esters also show a protective effect against sciatica; however, the sterol ester (27:1/16:1) consistently demonstrates a detrimental impact on IVDD, LBP, and sciatica. Additionally, our study underscores the intricate nature of lipid metabolism concerning IVDD, LBP, and sciatica. It uncovers a range of structural variations among lipids and explores how these variations may lead to different effects across various molecular subtypes.
Similar content being viewed by others
Introduction
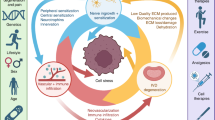
Intervertebral disc degeneration (IVDD) is a common degenerative spine condition marked by the progressive reduction of proteoglycans, type II collagen, and water content in the nucleus pulposus and annulus fibrosus1. Clinically, IVDD primarily presents with two main symptoms: low back pain (LBP) and sciatica2. LBP occurs due to rupture of the degenerated disc’s fibrous ring, leading to posterior protrusion of the nucleus pulposus and subsequent compression of spinal nerves, often resulting in radiculopathy (IVDD with radiculopathy)3. Moreover, IVDD impacting lumbar nerves L4 or L5 and sacral nerve S1 can lead to sciatica, characterized by pain in the lower limbs4,5. IVDD significantly contributes to the global burden of lower back pain and sciatica, affecting nearly two-thirds of adults worldwide and presenting substantial healthcare challenges6. Despite its impact, the causes and mechanisms of IVDD remain unclear, influenced by a complex interplay of genetic predisposition and environmental factors such as aging, obesity, cumulative trauma, and smoking7,8,9,10. Current treatment strategies for IVDD include rest, non-steroidal anti-inflammatory drugs (NSAIDs), conservative therapies involving traction, and surgical interventions11. Therefore, elucidating IVDD’s pathogenesis is pivotal for advancing the development of effective, minimally invasive treatment strategies devoid of side effects.
Liposomes are defined as spherical vesicles containing one or more concentric phospholipid bilayers surrounding an aqueous core12. They represent a significant category of lipid-based nanocarriers used in nanomedicine13. Their biodegradable and non-toxic properties render them versatile platforms for delivering therapeutic agents. Liposomes not only stabilize compounds but also surmount cellular and tissue absorption barriers, thereby improving drug pharmacokinetics and biodistribution to targeted body sites, enhancing therapeutic efficacy, and minimizing systemic toxicity14. Liposomes are widely acknowledged and extensively researched, serving crucial roles in various health domains as essential carriers for small molecules, peptides, genes, and monoclonal antibodies15,16,17,18,19.
In immature IVDD tissue, vascularization extends into approximately one-third of the fibrous outer ring. However, a hallmark of IVDD associated with LBP is the invasion of neovascularization and neural structures from the outer annulus fibrosus into the nucleus pulposus20. The impact of IVDD on plasma liposome concentrations and metabolite levels remains uncertain. Furthermore, there is a critical need to broaden the range of metabolites linked to IVDD. Nevertheless, the confirmation of the association between plasma lipidome and IVDD awaits evidence from randomized controlled trials (RCTs).
Mendelian randomization (MR) is a notable method in genetic epidemiology for examining causal relationships between exposures and outcomes. When RCTs are impractical, MR serves as a valuable alternative, offering robust evidence on causal links between exposures and disease risks21,22,23. By utilizing single nucleotide polymorphisms (SNPs) as instrumental variables (IVs), MR assesses the causal impact of exposures on outcomes24.Genetic variations are randomly assigned during gamete formation, and gene types typically remain unaffected by external environmental factors. Thus, well-designed MR studies can effectively address concerns about confounding and reverse causation. This investigation seeks to establish a definitive causal relationship between lipidome and IVDD through compelling evidence presentation. Ultimately, the study aims to enhance early detection and treatment of IVDD.Thus, the suggestion is to use Two-Sample Mendelian Randomization (TSMR) to investigate the potential link between lipidome and IVDD, followed by validation through Bayesian Model Averaging Mendelian Randomization (BMA-MR).
Methods
Data sources
The summary statistics for a Genome-wide Association Study (GWAS) on the lipidome were obtained from entries in the GWAS Catalog (https://www.ebi.ac.uk/gwas/, accession codes GCST90277238-GCST90277416). Our study cohort consisted of 7174 unrelated individuals of Finnish descent, drawn from the GeneRISK cohort. We conducted an analysis focusing on SNPs linked to 179 lipid species spanning 13 lipid classes and categorized into 4 groups (refer to Supplementary Table 1)25. The study identifies outcomes related to disc diseases: intervertebral disc degeneration (41,669 cases and 294,770 controls), low back pain (32,845 cases and 294,770 controls), and sciatica (46,707 cases and 365,474 controls). These results are based on the latest data release (R10) from the FinnGen consortium26. Diagnostic criteria were primarily classified under ICD-10: M51 for intervertebral disc degeneration, M54.5 for low back pain, and M54.3/M54.4 for sciatica. Furthermore, summary statistics related to intervertebral disk degeneration, low back pain, and sciatica were obtained from the R10 edition of the FinnGen GWAS findings. The phenotypic classification for intervertebral disk degeneration was designated as ‘M13_INTERVERTEB’, while low back pain and sciatica were classified under “M13_LOWBACKPAINORANDSCIATICA.” These traits showed minimal GWAS overlap with lipids (less than 5%), thereby mitigating potential bias (https://r10.finngen.fi)26.
Instrumental variable extraction
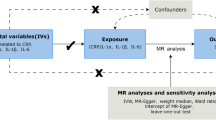
To assess the impact of lipidome on IVDD using SNPs as instrumental variables, adherence to three Mendelian randomization (MR) assumptions is essential. Firstly, there must be a significant genetic association with lipidome. Secondly, chosen instrumental variables should be free from confounding factors, ensuring they reliably influence the liposome-IVDD relationship. Lastly, these variables should exclusively affect IVDD through lipidome. Specific criteria guided SNP selection: initial selection based on robust correlation with lipidome (P < 5 × 10^-8), independence from linkage disequilibrium (LD) effects (excluding SNPs with LD r^2 ≥ 0.001 and those within 10,000 kb), and exclusion of SNPs with minor allele frequencies not in Hardy–Weinberg equilibrium. To curtail the influence of correlated SNP associations, linkage disequilibrium (LD) scrutiny was performed using the European 1000 Genomes Project Phase 3 as a reference, with an r2 threshold of < 0.001 and a clumping distance set at 10,000 kb. Palindromic SNPs were omitted to avoid inconsistencies in allelic interpretations that could skew causal inferences. SNPs with strong associations to the outcome were also discarded. The MR Steiger filter was applied to eliminate SNPs with an incorrect direction of effect. The IVs for lipid species were evaluated using the variance explained (R2) and the F-statistic, with those yielding an F-statistic below 10 being eliminated. The F-statistic is calculated using the formula R2(N-K-1)/[K(1-R2)], where R2 is the variance of the exposure explained by the IVs, N is the effective sample size, and K is the number of variants in the IV model. Instrumental variables were identified using the PhenoScanner website. Prior to MR analysis, SNPs directly associated with IVDD were excluded. Comprehensive evaluation, including MR-Egger regression and MR-PRESSO outlier tests27, assessed potential pleiotropic effects. No SNPs were removed post-assessment. Two-Sample MR analysis was subsequently employed to explore exposure-outcome relationships.
Two samples of MR analysis
Inverse variance weighting (IVW) is a widely employed method for effectively amalgamating multiple random variables to decrease overall variance. This technique assigns weights based on the dispersion of each variable within the ensemble, facilitating the integration of outcomes across diverse studies. IVW stands as the primary analytical approach when considering all genetic variations as valid instruments, yielding the most precise and dependable estimates28. To ensure study precision, diverse methodologies such as MR-Egger, weighted median, and both simple and weighted models were utilized. These supplementary analyses function as safeguards, ensuring sturdy and trustworthy outcomes. For instance, consistent directional findings across multiple methodologies enhance confidence in causal relationships. Furthermore, this study utilized MR-BMA to validate the causal impact of exposure on outcomes, mitigating biases and allowing for simultaneous modeling of multiple interrelated risk factors. MR-BMA proves especially suitable for datasets characterized by high throughput and strong correlations29.
Sensitivity analysis
Sensitivity analyses were conducted to ensure the robustness of our study findings. Initially, we assessed the intercept term of the MR-Egger regression model to evaluate potential pleiotropic effects30. A P-value greater than 0.05 for the intercept term indicated minimal influence from genetic pleiotropy, supporting the conclusion that instrumental variables exclusively affect IVDD risk through lipids. Cochran’s Q test was utilized to investigate heterogeneity among instrumental variables and their potential impact on causal estimates31. Funnel plots were employed to visually assess data heterogeneity. Additionally, leave-one-out analysis iteratively conducted Mendelian randomization by sequentially excluding one SNP at a time to assess result sensitivity. Subsequently, MR-PRESSO tests were applied to detect discrepancies in MR analysis outcomes pre- and post-correction. The combined use of MR-Egger intercept tests and MR-PRESSO tests provided comprehensive sensitivity analysis from various perspectives. In cases where MR-Egger intercept tests indicated directional pleiotropy, MR-PRESSO helped identify and rectify potential bias-inducing outliers. Collectively, these methodologies ensured thorough sensitivity analysis, thereby enhancing the reliability and validity of our study’s findings.
Results
Causal effects of lipidomes and IVDD
Using Two-Sample Mendelian Randomization (TSMR), our study investigates the role of lipids in Intervertebral Disc Degeneration (IVDD). The findings suggest that sterol esters, phosphatidylcholine, phosphatidylethanolamine, and triglycerides potentially influence IVDD risk. Specifically, sterol esters, triglycerides, and certain phosphatidylcholine structures exhibit protective effects, whereas phosphatidylethanolamine is associated with increased IVDD risk (Fig. 1). Detailed results from various analytical methods are presented in Supplementary Table 2. The Inverse-Variance Weighted (IVW) method serves as the primary indicator. Consistency among causal relationships identified by the remaining four analytical methods with IVW findings, achieving a significance level of P < 0.05, would enhance confidence in these relationships. Overall, alignment between TSMR and Bayesian Model Averaging Mendelian Randomization (BMA-MR) analyses was observed, with exceptions noted for specific instances involving Phosphatidylethanolamine (O-16:1_18:2), Phosphatidylcholine (16:0_20:3), and Phosphatidylcholine (18:2_0:0).
Examines the impact of lipids on intervertebral disc degeneration using Mendelian randomization forest plots and Bayesian model averaging. The IVW method computed odds ratios (OR), P-values (P-val), and 95% confidence intervals (CI). Bayesian odds ratios (B-OR) and Bayesian P-values (B-Pval) were derived from MR-BMA analysis, while IVW outcomes were depicted visually via forest plots. Phosphatidylcholine (O-16:1/20:3), characterized by specific molecular structure, comprises a choline head group linked to the glycerol backbone, incorporating a 16-carbon unsaturated fatty acid at the first position and a 20-carbon unsaturated fatty acid at the second position. The arrangement and composition of these components are pivotal for the structural and functional integrity of phospholipids within biological membranes. This naming convention similarly applies to phosphatidylethanolamine and phosphatidylinositol. In lipid terminology, "triacylglycerol 58:7" specifies the composition of triacylglycerol molecules, where “58” denotes the total carbon atoms in the three fatty acid chains, and "7" represents the total double bonds within these chains.
Causal effects of lipidomes and LBP
TSMR analysis identified potential causal effects on LBP, highlighting sterol esters, phosphatidylcholine, sphingomyelin, and glycerides. Protective effects were observed specifically with sterol esters and sphingomyelin, whereas various phosphatidylcholine variants indicated risk factors. Triacylglycerol within the glyceride family showed a risk effect on LBP (Fig. 2). For a comprehensive overview of various analytical approaches, please refer to Supplementary Material 3. IVW findings are pivotal as our main benchmark. Consistency in causal direction among the remaining four methods alongside IVW outcomes, coupled with achieving statistical significance (P < 0.05), would substantially enhance confidence in confirming causal associations. Overall, findings from TSMR and BMA-MR analyses exhibit substantial consistency (Fig. 2).
Presents forest plots illustrating the outcomes of Mendelian randomization (MR) and Bayesian model averaging (BMA-MR) analyses evaluating the effects of lipids on LBP. The results include odds ratios (OR), P-values (P-val), and 95% confidence intervals (CI) derived from the IVW method. Furthermore, the outcomes of MR-BMA analysis are illustrated by B-OR and B-Pval, complemented by the forest plot that encapsulates the results of IVW investigations. Specifically, sphingomyelin (d38:2) refers to a distinct category of sphingomyelin lipids characterized by the fatty acid composition "d38:2," indicating a primary chain of 38 carbons with 2 double bonds within the sphingomyelin molecule.
Causal effects of lipidomes and sciatica
The TSMR analysis highlights significant influences of glycerophospholipids, sphingolipids, glycerides, and sterols on sciatica. Certain sterols show correlations with sciatica incidence, their risk and protective effects contingent upon molecular structure (Fig. 3). This pattern extends to phosphatidylcholine; Phosphatidylcholine (16:1_18:0) and Phosphatidylcholine (18:1_20:2) consistently indicate risk factors. Triacylglycerols among glycerides are associated with increased risk, while sphingolipids consistently exhibit protective effects against breast cancer incidence. Detailed results from various analytical methods are provided in Supplementary Material 4, with IVW results serving as the primary reference metric. Alignment of directional causal relationships from the other four analytical methods with IVW results, achieving P < 0.05, would significantly enhance confidence in establishing causality. Overall, findings from TSMR and BMA-MR analyses demonstrate considerable consistency (Fig. 3), though exceptions exist notably with Sterol ester (27:1/18:0) and Triacylglycerol (48:2).
Presents a Forest Plot depicting the findings from Mendelian randomization (MR) and Bayesian model averaging (BMA) analyses assessing the impact of lipids on sciatica. The plot displays OR (odds ratio), P-val (P-value), and 95% CI (confidence interval) derived from the IVW (inverse variance weighted) method. Results from MR-BMA analysis are denoted as B-OR and B-Pval, though the plot exclusively features IVW outcomes.
Sensitivity analysis
Sensitivity analyses, detailed in Supplementary Tables 2–4, were conducted to ensure result robustness within the IVDD framework. Both IVW and MR-Egger tests revealed no evidence of heterogeneity. Similarly, no heterogeneity was observed in IBP and sciatica. The MR-Egger intercept test resulted in a P-value exceeding 0.05, suggesting no evidence of horizontal pleiotropy. Additionally, the MR-PRESSO test confirmed result accuracy by detecting no pleiotropy. Scatter plots illustrating the MR analysis can be found in Supplementary Material 2–4. Funnel plot examination revealed no significant heterogeneity across these figures. Furthermore, leave-one-out analysis demonstrated that no single SNP had a significant influence on the MR estimates. While certain SNPs may have influenced outcomes in IBP and sciatica, their odds ratios consistently aligned on one side of the null line as depicted in Supplementary Supplementary Material 3 and 4. Supplementary Table 5 in Supplementary Material 1 lists the F-statistics, R2 and SNP counts for each lipid class.
Discussion
This study represents a pioneering investigation into the impact of structurally diverse lipidome on intervertebral disc degeneration (IVDD), low back pain (LBP), and sciatica, drawing on an analysis of 179 liposome studies. Our study explores 179 liposome characteristics as exposures linked to IVDD, LBP, and sciatica outcomes, uncovering intricate causal relationships. We identify significant impacts of glycerophospholipids, sterols, and glycolipids on these conditions. Specifically, phosphatidylcholine and phosphatidylinositol within glycerophospholipids emerge as key factors in IVDD, with phosphatidylcholine posing a risk and phosphatidylinositol offering protection. Sterols and glycolipids are also implicated as contributing risk factors. In the context of LBP, glycerophospholipids, sterols, and glycolipids not only exert influence but also demonstrate a protective effect of sphingomyelin. Notably, different structural forms of phosphatidylcholine and sterols exhibit variable impacts on sciatica.
Mendelian randomization (MR) techniques have become increasingly important in studying potential causal connections between exposures and outcomes32. By mitigating confounding factors and reverse causation biases, MR analysis provides more reliable assessments of causal associations than conventional observational studies33. Li et al. utilized MR methods to uncover an inverse relationship, indicating that higher interleukin-6 levels are associated with a decreased likelihood of experiencing low back pain34. Meanwhile, Jinfeng Luo et al. conducted MR analysis on lipid levels and LBP incidence, uncovering a negative association between high-density lipoprotein cholesterol (HDL-C) and LBP prevalence in European populations. However, they did not establish causal links between low-density lipoprotein cholesterol (LDL-C) / total cholesterol (TG) and LBP risk35. These investigations did not delve into specific lipoprotein subtypes or comprehensively examine the interplay among intervertebral disc degeneration (IVDD), low back pain (LBP), and sciatica.
In our study, we consistently observed a positive correlation between serum triglyceride levels and the risk of intervertebral disc degeneration (IVDD), lower back pain (LBP), and sciatica. Previous research has highlighted elevated cholesterol levels as one of the most prevalent risk factors for atherosclerotic lesions36. Notably, the independent role of triglycerides in atherosclerosis formation has also been documented37. Atherosclerosis affecting the lumbar region is considered a significant contributor to both intervertebral disc degeneration and sciatica38,39, a finding reinforced by our study. From a molecular standpoint, the interplay between triglycerides (TG) and intervertebral disc degeneration (IVDD) can be examined across several biological layers. In vitro studies demonstrate that hypertriglyceridaemia predominantly facilitates disc cell apoptosis and extracellular matrix breakdown via the MAPK signalling cascade, with the ERK pathway being a key contributor40. Moreover, excessive TG accumulation may provoke inflammatory cascades, aggravating IVDD pathogenesis. TG and its metabolic byproducts could stimulate inflammatory cytokine secretion by activating pathways such as NF-κB, thereby inciting localised inflammation within disc tissues and progressively compromising their structural integrity41. Dysregulated TG metabolism may additionally disrupt the equilibrium between extracellular matrix synthesis and degradation in intervertebral discs. Notably, matrix metalloproteinases (MMPs) are pivotal in degenerative disc disorders42, and aberrant TG metabolism may dysregulate MMP activity, accelerating matrix degradation and undermining disc biomechanical properties43. Oxidative stress emerges as a critical mediator in TG-associated IVDD. Hypertriglyceridaemia may precipitate oxidative stress44, inflicting cellular damage and degenerative alterations within discs. This oxidative imbalance depletes endogenous antioxidant defences, inducing lipid peroxidation, protein carbonylation, and genomic instability – collectively eroding disc cellular homeostasis and tissue resilience45. Further investigation is crucial to fully elucidate the specific underlying mechanisms linking lipid levels to the onset of lumbar disc herniation.
Sterol esters, formed by combining sterols with fatty acids through esterification, are essential lipid components found in plant and animal cells, crucial for cellular membrane structure46. These compounds significantly influence membrane fluidity and architecture, thereby affecting vital cellular interactions involved in signal transmission across membranes. Lower levels of sterol esters could disrupt the lipid composition of membranes, potentially impacting the functionality of cell surface receptors. Such changes in receptor activity might interfere with signaling pathways governed by growth factors, potentially contributing to the development of sciatica, as supported by our study. Notably, Sterol ester (27:1/16:1) consistently demonstrates protective effects against these conditions, contrasting with other forms of sterol esters that may exhibit varying effects due to structural differences. Further research is necessary to fully elucidate the specific molecular mechanisms and clinical implications arising from these observations.
Phosphatidylethanolamine and phosphatidylcholine constitute essential components within cellular membranes. Despite the absence of comprehensive research directly linking these phospholipids to intervertebral disc degeneration (IVDD), low back pain (LBP), and sciatica on a large scale, our investigations consistently associate phosphatidylcholine with these conditions. Notably, specific subtypes such as Phosphatidylcholine (O-16:1_18:1) and Phosphatidylethanolamine (O-16:1_18:2) present exceptions. These connections potentially involve mechanisms of immune response. It is significant that phosphatidylethanolamine and phosphatidylcholine are recognized by natural killer cells and T lymphocytes, potentially promoting T lymphocyte proliferation and augmenting protein kinase C (PKC) activity in diverse cellular contexts47,48. Studies suggest that heightened levels of phospholipids can significantly enhance immune system function through modulation of membrane-associated signaling pathways, directly impacting T cell activation and proliferation49. Increased phospholipids enhance membrane fluidity and receptor organization, facilitating interactions between cell surface receptors and ligands, thereby expediting immune cell responses and amplification50,51. Research demonstrates that phospholipid derivatives (e.g., lysophosphatidylcholine) activate cell-surface Toll-like receptor 4 (TLR4), inducing NF-κB-mediated upregulation of interleukin-6 (IL-6) and tumour necrosis factor-α (TNF-α)52. These pro-inflammatory cytokines exacerbate extracellular matrix (ECM) breakdown by elevating matrix metalloproteinase-3 (MMP-3) and ADAMTS-5 expression10. Notably, murine studies reveal that intra-articular LPC (16:0) administration induces chronic pain and anxiety-like behaviours, implicating this lipid species as a potential driver of persistent joint pain in both sexes53. Clinical correlations exist in fibromyalgia patients, where elevated LPC (16:0) levels correlate with pain severity54, while murine fibromyalgia models show concomitant increases in LPC (18:1)55. These observations substantiate our findings that Phosphatidylcholine (16:0_20:3) and (16:0_18:3) constitute IVDD risk factors, whereas Phosphatidylcholine (18:1_20:2) associates specifically with low back pain (LBP).Mechanistically, phospholipid derivatives like lysophosphatidic Acid stimulate neuronal sprouting via Trk receptors56, with pathological nerve ingrowth into degenerated discs contributing to LBP57. lysophosphatidic Acid induces inflammation and programmed cell death through the activation of G-protein-coupled receptors . In contrast, rhBMP2/7 indirectly diminishes LPA generation by reinstating BMP/Smad signalling, mitigating inflammatory responses and degenerative processes58. Such evidence positions lipid metabolism as a shared pathogenic axis in IVDD, LBP, and sciatica. Our work particularly underscores how distinct phosphatidylcholine subspecies differentially modulate IVDD risk, revealing a nuanced lipid-disease relationship that warrants deeper investigation into metabolic pathways underlying these spinal disorders.
Sphingomyelin(SM) is crucial for modulating mammalian membrane properties and acts as a significant reservoir of bioactive compounds. SM hydrolyses to produce sphingosine-1-phosphate (S1P), which binds to the S1PR1 receptor, inhibiting NF-κB nuclear translocation, and reducing the expression of IL-1β and TNF-α. Concurrently, ceramide derived from SM upregulates autophagy-related genes (such as LC3 and Beclin-1) via PPARγ, promoting the clearance of damaged mitochondria and misfolded proteins, thereby maintaining cellular homeostasis59. SM is also an important component of lipid rafts, and its enrichment maintains the aggregation and signal transduction efficiency of membrane receptors (such as growth factor receptors)60. A reduction in SM in the degenerated intervertebral disc leads to disruption of lipid raft structure, exacerbating non-specific activation of inflammatory receptors (such as TLR4), amplifying injury signals. Despite this pivotal role, comprehensive studies directly associating sphingomyelin with IVDD, LBP, and sciatica risk remain limited. Our investigation uncovered consistent protective benefits of Sphingomyelin (d34:2) and Sphingomyelin (d38:2) against IVDD, LBP, and sciatica, providing valuable insights into potential mechanisms and therapeutic avenues.
Clinical relevance, The effects presented by statin drugs are consistent with the results of our research. Statins, including simvastatin, atorvastatin, and lovastatin. Research indicates that the oral administration of statins can slow down the harmful processes associated with disc degeneration61. For instance, a study revealed that a hydrogel containing 5 mg/mL of simvastatin improved disc conditions in SD rats with disc injuries62. Similarly, discs treated with 5 and 10 μM concentrations of lovastatin showed increased levels of glycosaminoglycans, S100 proteins, collagen II, and BMP263. Rosuvastatin has been found to mitigate ECM degradation, cell aging, and pyroptosis linked to TNFα by inhibiting the HMGB1 and NF-κB pathways, effectively hindering the progression of intervertebral disc degeneration (IDD)64. Consequently, these lipid-lowering agents demonstrate protective benefits against the advancement of IVDD. These investigations have further yielded novel insights for our clinical studies, including the potential modulation of intervertebral disc degeneration progression via lipid-lowering pharmacological interventions. Existing metabolomic and lipidomic profiling of both healthy and degenerated discs65, when synthesised with our findings, indicates that lipidomic signatures may serve as promising biomarkers for assessing IVDD risk.
Strengths and limitations
This study demonstrates multiple strengths. Firstly, we innovatively applied the TSMR method to thoroughly explore how lipids relate to IVDD, LBP, and sciatica. Our genetic data collection was meticulous, with rigorous efforts to minimize any potential confounding factors. Secondly, we employed the BMA-MR method to corroborate our findings, thereby improving the precision of our results. Thirdly, by investigating these three interrelated conditions, we expanded our comprehension of back pain, thereby enhancing the significance of our conclusions. However, our research faces limitations. Firstly, there is a slight (< 5%) overlap between exposure and outcome samples, which facilitated database analysis but necessitates future expansion. In addition, obstacles in acquiring reliable SNPs crucial for Multivariable Mendelian Randomization (MVMR) have impeded the interpretation of findings. Our objective is to enhance algorithms in forthcoming research endeavors to tackle this issue effectively. Furthermore, Mendelian randomization (MR) analysis presupposes that genetic variations’ influence on outcomes is entirely mediated through exposure66. Moreover, differences in the assessment of importance in Two-Sample Mendelian Randomization (TSMR) compared to Bayesian Model Averaging-Mendelian Randomization (BMA-MR) may stem from distinct analytical methodologies. TSMR employs frequentist statistical methods, while BMA-MR incorporates Bayesian approaches, leveraging prior and posterior distributions for parameter estimation and uncertainty handling. However, this divergence can lead to associations considered significant in frequentist analyses being non-significant in Bayesian frameworks67,68. In specific instances, BMA-MR might necessitate stronger evidence for causal inference compared to conventional methods. Consequently, while MR techniques enable the assessment of causal relationships, they do not fully elucidate the mechanisms by which lipids may prevent Intervertebral Disc Degeneration (IVDD), Low Back Pain (LBP), and sciatica.Therefore, additional research is essential to clarify the underlying processes highlighted by our findings. Lastly, we refrained from implementing multiple analysis corrections because our primary focus was identifying potential biomarkers or therapeutic targets. Avoiding the Bonferroni correction due to its strictness was crucial to prevent excluding meaningful indicators.
Conclusion
Our study offers significant insights into the relationship between specific lipids and the risks associated with intervertebral disc degeneration (IVDD), low back pain (LBP), and sciatica. Our findings indicate that phosphatidylcholine and triglycerides may increase the incidence of IVDD, LBP, and sciatica, suggesting potential adverse effects. Conversely, sphingomyelin appears to reduce the occurrence of LBP and sciatica, implying a protective role. Sterol esters also exhibit a protective effect against sciatica, but the sterol ester (27:1/16:1) consistently demonstrates detrimental effects on IVDD, LBP, and sciatica within the Sterols category. Furthermore, our research highlights the complex nature of lipid metabolism in IVDD, LBP, and sciatica, uncovering diverse structural variations among lipids and their potentially varying impacts across molecular subtypes. These discoveries deepen our comprehension of how lipids, including phosphatidylcholine and triglycerides, impact the risk factors associated with IVDD, LBP, and sciatica. This underscores the necessity for additional research to uncover the mechanisms at play.
Data availability
The datasets [Exposure/Outcome] for this study can be found in the [IEU Open GWAS] [https://gwas.mrcieu.ac.uk/].
Abbreviations
- LBP:
-
Lower back pain
- IVDD:
-
Intervertebral disc degeneration
- MR:
-
Mendelian randomization
- RCTs:
-
Randomized controlled trials
- SNPs:
-
Single nucleotide polymorphisms
- IVs:
-
Instrumental variables
- TSMR:
-
Two-sample mendelian randomization
- FDR:
-
False discovery rate
- BMA-MR:
-
Bayesian model averaging multivariate mendelian randomization
- GWAS:
-
Genome-wide association study
- LD:
-
Linkage disequilibrium
- MR-PRESSO:
-
MR pleiotropy residual sum and outlier
- IVW:
-
Inverse variance weighting
References
Vergroesen, P. P. et al. Mechanics and biology in intervertebral disc degeneration: A vicious circle. Osteoarthr. Cartil. 23, 1057–1070 (2015).
Freemont, A. J. The cellular pathobiology of the degenerate intervertebral disc and discogenic back pain. Rheumatol (Oxford) 48, 5–10 (2009).
Khan, A. N. et al. Inflammatory biomarkers of low back pain and disc degeneration: A review. Ann. NY Acad. Sci. 1410, 68–84 (2017).
Ropper, A. H. & Zafonte, R. D. Sciatica. N. Engl. J. Med. 372, 1240–1248 (2015).
Porchet, F. et al. Relationship between severity of lumbar disc disease and disability scores in sciatica patients. Neurosurgery 50, 1253–1259 (2002).
Deyo, R. A. & Mirza, S. K. Clinical Practice. Herniated lumbar intervertebral disk. N Engl J Med 374, 1763–1772 (2016).
Kalichman, L. & Hunter, D. J. The genetics of intervertebral disc degeneration. Familial predisposition and heritability estimation. Joint Bone Spine 75, 383–387 (2008).
Francisco, V. et al. A new immunometabolic perspective of intervertebral disc degeneration. Nat. Rev. Rheumatol. 18, 47–60 (2022).
Ulrich, J. A., Liebenberg, E. C., Thuillier, D. U. & Lotz, J. C. ISSLS prize winner: Repeated disc injury causes persistent inflammation. Spine 32, 2812–2819 (2007).
Wang, F., Cai, F., Shi, R., Wang, X. H. & Wu, X. T. Aging and agerelated stresses: A senescence mechanism of intervertebral disc degeneration. Osteoarthr. Cartil. 24, 398–408 (2016).
Xin, J. et al. Treatment of intervertebral disc degeneration. Orthop. Surg. 14, 1271–1280 (2022).
Liu, G., Hou, S., Tong, P. & Li, J. Liposomes: Preparation, characteristics, and application strategies in analytical chemistry. Crit. Rev. Anal. Chem. 52, 392–412 (2022).
Shah, S., Dhawan, V., Holm, R., Nagarsenker, M. S. & Perrie, Y. Liposomes: Advancements and innovation in the manufacturing process. Adv. Drug Deliv. Rev. 154–155, 102–122 (2020).
Guimaraes, D., Cavaco-Paulo, A. & Nogueira, E. Design of liposomes as drug delivery system for therapeutic applications. Int. J. Pharm. 601, 120571 (2021).
Shah, S. M. et al. Liposomes for targeting hepatocellular carcinoma: Use of conjugated arabinogalactan as targeting ligand. Int. J. Pharm. 477, 128–139 (2014).
Shah, S. M., Pathak, P. O., Jain, A. S., Barhate, C. R. & Nagarsenker, M. S. Synthesis, characterization, and in vitro evaluation of palmitoylated arabinogalactan with potential for liver targeting. Carbohydr. Res. 367, 41–47 (2013).
Dutta, R. & Mahato, R. I. Recent advances in hepatocellular carcinoma therapy. Pharmacol. Ther. 173, 106–117 (2017).
Yu, B., Zhao, X., Lee, L. J. & Lee, R. J. Targeted delivery systems for oligonucleotide therapeutics. AAPS J. 11, 195–203 (2009).
Eloy, J. O., Petrilli, R., Trevizan, L. N. F. & Chorilli, M. Immunoliposomes: A review on functionalization strategies and targets for drug delivery. Colloids. Surf. B Biointerfaces. 159, 454–467 (2017).
Koroth, J. et al. Macrophages and intervertebral disc degeneration. Int. J. Mol. Sci. 24(2), 1367 (2023).
Shin, S.-Y. et al. An atlas of genetic influences on human blood metabolites. Nat. Genet. 46(6), 543–550. https://doi.org/10.1038/ng.2982 (2014).
Murphy, N. et al. Insulin-like growth factor-1, insulin-like growth factor-binding protein-3, and breast cancer risk: Observational and Mendelian randomization analyses with approximately 430 000 women. Ann. Oncol. 31, 641–649 (2020).
Khoei, N. S. S. et al. Genetically raised circulating bilirubin levels and risk of ten cancers: A mendelian randomization study. Cells 10(2), 394. https://doi.org/10.3390/cells10020394 (2021).
Davies, N. M., Holmes, M. V. & Davey Smith, G. Reading mendelian randomisation studies: A guide, glossary, and checklist for clinicians. BMJ 362, k601 (2018).
Ottensmann, L. et al. Genome-wide association analysis of plasma lipidome identifies 495 genetic associations. Nat. Commun. 14, 6934 (2023).
Kurki, M. I. et al. FinnGen provides genetic insights from a well-phenotyped isolated population. Nature 613, 508–518 (2023).
Verbanck, M., Chen, C. Y., Neale, B. & Do, R. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat. Genet. 50, 693–698 (2018).
Lawlor, D. A., Harbord, R. M., Sterne, J. A., Timpson, N. & Davey Smith, G. Mendelian randomization: Using genes as instruments for making causal inferences in epidemiology. Stat Med 27, 1133–1163 (2008).
Zuber, V., Colijn, J. M., Klaver, C. & Burgess, S. Selecting likely causal risk factors from high-throughput experiments using multivariable Mendelian randomization. Nat. Commun. 11, 29 (2020).
Bowden, J., Davey Smith, G. & Burgess, S. Mendelian randomization with invalid instruments: Effect estimation and bias detection through Egger regression. Int. J. Epidemiol. 44, 512–525 (2015).
Burgess, S., Zuber, V., Valdes-Marquez, E., Sun, B. B. & Hopewell, J. C. Mendelian randomization with fine-mapped genetic data: Choosing from large numbers of correlated instrumental variables. Genet. Epidemiol. 41, 714–725 (2017).
Lv, Z., Cui, J. & Zhang, J. Smoking, alcohol and coffee consumption and risk of low back pain: A Mendelian randomization study. Eur. Spine J. 31(11), 2913–2919 (2022).
Qian, Y. et al. Genetically determined circulating levels of cytokines and the risk of rheumatoid arthritis. Front Genet. 13, 802464 (2022).
Li, W. et al. Assessing the causal relationship between genetically determined inflammatory biomarkers and low back pain risk: A bidirectional two-sample Mendelian randomization study. Front Immunol. 14, 1174656 (2023).
Zhong, Y., Li, Y., Sun, W. & Xiao, M. Liposomes have a direct effect on multiple myeloma: A Mendelian randomization study. Front Oncol. 14, 1404744 (2024).
Steinberg, D. Atherogenesis in perspective: Hypercholesterolemia and inflammation as partners in crime. Nat. Med. 8, 1211–1217 (2002).
Austin, M. A., Hokanson, J. E. & Edwards, K. L. Hypertriglyceridemia as a cardiovascular risk factor. Am. J. Cardiol. 81(4A), 7B-12B (1998).
Rutsch, F. & Terkeltaub, R. Deficiencies of physiologic calcification inhibitors and low-grade inflammation in arterial calcification: Lessons for cartilage calcification. Joint, Bone, Spine:revue du rhumatisme. 72, 110–118 (2005).
Mehta, J. L., Chen, J., Hermonat, P. L., Romeo, F. & Novelli, G. Lectin-like oxidized low-density lipoprotein receptor-1 (LOX-1): A critical player in the development of atherosclerosis and related disorders. Cardiovasc. Res. 69, 36–45 (2006).
Zhang, X. et al. Obesity mediates apoptosis and extracellular matrix metabolic imbalances via MAPK pathway activation in intervertebral disk degeneration. Front Physiol. 10, 1284 (2019).
Lu, Y., Qie, D., Yang, F. & Wu, J. LncRNA MEG3 aggravates adipocyte inflammation and insulin resistance by targeting IGF2BP2 to activate TLR4/NF-κB signaling pathway. Int. Immunopharmacol. 121, 110467 (2023).
Glaeser, J. D. et al. NF-κB inhibitor, NEMO-binding domain peptide attenuates intervertebral disc degeneration. Spine J. 20, 1480–1491. https://doi.org/10.1016/j.spinee.2020.04.025 (2020).
Kozakova, M. et al. Cardiovascular organ damage in type 2 diabetes mellitus: The role of lipids and inflammation. Cardiovasc. Diabetol. 18, 61 (2019).
Li, T., Guo, W. & Zhou, Z. Adipose triglyceride lipase in hepatic physiology and pathophysiology. Biomolecules 12, 57 (2021).
Wang, Y. et al. Oxidative stress in intervertebral disc degeneration: Molecular mechanisms, pathogenesis and treatment. Cell Prolif. 56, e13448 (2023).
Ho, W. Y., Hartmann, H. & Ling, S. C. Central nervous system cholesterol metabolism in health and disease. IUBMB Life 74, 826–841 (2022).
Shahine, A. et al. A molecular basis of human T cell receptor autoreactivity toward self-phospholipids. Sci. Immunol. 2, eaao1384 (2017).
Sasagawa, T., Okita, M., Murakami, J., Kato, T. & Watanabe, A. Abnormal serum lysophospholipids in multiple myeloma patients. Lipids 34, 17–21 (1999).
Hirata, F. & Axelrod, J. Phospholipid methylation and biological signal transmission. Science 209, 1082–1090 (1980).
Shahine, A. et al. A T-cell receptor escape channel allows broad T-cell response to CD1b and membrane phospholipids. Nat. Commun. 10, 56 (2019).
Calder, P. C., Yaqoob, P., Harvey, D. J., Watts, A. & Newsholme, E. A. Incorporation of fatty acids by concanavalin A-stimulated lymphocytes and the effect on fatty acid composition and membrane fluidity. Biochem. J. 300, 509–518 (1994).
Sharma, N., Akhade, A. S., Ismaeel, S. & Qadri, A. Serum-borne lipids amplify TLR-activated inflammatory responses. J. Leukoc. Biol. 109(4), 821–831 (2021).
Jacquot, F. et al. Lysophosphatidylcholine 16 0 mediates chronic joint pain associated to rheumatic diseases through acid-sensing ion channel 3. Pain 163, 1999–2013 (2022).
Hung, C. H. et al. Activation of acid-sensing ion channel 3 by lysophosphatidylcholine 16:0 mediates psychological stress-induced fibromyalgia-like pain. Ann. Rheum. Dis. 79, 1644–1656 (2020).
Clos-Garcia, M. et al. Gut microbiome and serum metabolome analyses identify molecular biomarkers and altered glutamate metabolism in fibromyalgia. EBioMedicine 46, 499–511 (2019).
Moughal, N. A. et al. Protean agonism of the lysophosphatidic acid receptor-1 with Ki16425 reduces nerve growth factor-induced neurite outgrowth in pheochromocytoma 12 cells. J. Neurochem. 98(6), 1920–1929 (2006).
Staszkiewicz, R. et al. Pathomechanism of the IVDs degeneration and the role of neurotrophic factors and concentration of selected elements in genesis of low back pain. Curr. Pharm. Biotechnol. 24(9), 1164–1177 (2023).
Xie, S. et al. Recombinant human bone morphogenetic protein 2 and 7 inhibit the degeneration of intervertebral discs by blocking the Puma-dependent apoptotic signaling. Int. J. Biol. Sci. 17(9), 2367–2379 (2021).
Maceyka, M., Harikumar, K. B., Milstien, S. & Spiegel, S. Sphingosine-1-phosphate signaling and its role in disease. Trends Cell Biol. 22(1), 50–60 (2012).
Simons, K. & Toomre, D. Lipid rafts and signal transduction. Nat. Rev. Mol. Cell. Biol. 1(1), 31–39 (2000).
Shi, S., Wang, C., Yuan, W., Wang, X. & Zhou, X. Potential prevention: Orally administered statins may retard the pathologic process of disc degeneration. Med. Hypotheses 76(1), 125–127 (2011).
Gologorsky, Y. & Chi, J. Statins for disc degeneration. Neurosurgery 74(4), N18–N19 (2014).
Hu, M.-H., Yang, K.-C., Chen, Y.-J., Sun, Y.-H. & Yang, S.-H. Lovastatin prevents discography-associated degeneration and maintains the functional morphology of intervertebral discs. Spine J.: Off. J. North Am. Spine Soc. 14(10), 2459–2466 (2014).
Chen, W. et al. Rosuvastatin suppresses TNF-α-induced matrix catabolism, pyroptosis and senescence via the HMGB1/NF-κB signaling pathway in nucleus pulposus cells. Acta. Biochim. Et. Biophys. Sin. 55(5), 795–808 (2023).
Francisco, V. et al. Metabolomic signature and molecular profile of normal and degenerated human intervertebral disc cells. Spine J. 23(10), 1549–1562 (2023).
Weng, H. et al. Association between uric acid and risk of venous thromboembolism in East Asian populations: A cohort and Mendelian randomization study. Lancet. Reg. Health West Pac. 39, 100848 (2023).
Kruschke, J.K. Doing Bayesian data analysis: A tutorial with R and BUGS. Brain 1 (2010).
Gelman, A., Carlin, J.B., Stern, H.S., Dunson, D.B. & Rubin, D.B. Bayesian data analysis, third edition. J. Am. Stat. Assoc. 45 (2003).
Acknowledgements
We express our gratitude to the IEU Open GWAS database (https://gwas.mrcieu.ac.uk/) for providing publicly available summary-level GWAS data for our study. We would like acknowledge the following financial support: National Natural Science Foundation of China (No. 81774333, No. 82074453 and No. 82205154); We would also like to extend a special thanks to Dr. Li Pei for his invaluable guidance and help in developing our research methodology and approach. His insights and expertise were instrumental in shaping the direction of this study.
Funding
This work was supported by grants from the Natural Science Foundation of China (No. 82272553); China Postdoctoral Science Foundation (2022TQ0397, 2022MD723744); Natural Science Foundation of Chongqing, China (CSTB2024NSCQ-MSX0532); Natural Science Foundation of Chongqing(CSTB2024NSCQ-MSX0335). Chongqing Young and Middle-aged Medical Talents Project; Postdoctoral scholarship project in Chongqing(220901334472992). Joint Medical Research Project of Health Commission & Science and Technology Bureau of Chongqing, China (2024QNXM032); Disciplines Construction Program of The Third Affiliated Hospital of Chongqing Medical University (KY23035, KY23041).
Author information
Authors and Affiliations
Contributions
All authors made a significant contribution to the work reported and agreed to be accountable for all aspects of the work. P.Z.Y and Z.Y.B.T designed the experiments. P.Z.Y, H.J.X, L.X.X, G.Y.J, and Z.Y.B performed the experiments. P.Z.Y, Z.Y.B, and H.J.X prepared the initial draft of the manuscript. L.P, W.Y.Yand Z.Q gave critical feedback during the study or during the submission of the manuscript. All authors had given final approval of the version to be submitted and agreed on the journal to be published.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The data used in this paper are publicly available, ethically approved, and the subjects have given their informed consent.
Consent for publication
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Pang, ZY., Zhu, YB., Hu, JX. et al. The impact of lipidome on intervertebral disk degeneration, low back pain, and sciatica: a Mendelian randomization study. Sci Rep 15, 18045 (2025). https://doi.org/10.1038/s41598-025-99914-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-99914-9