Abstract
Pancreatic cancer has a dismal prognosis due to the rapid progression and inefficiency of chemotherapy. To ameliorate this inefficiency of chemotherapy drug, we developed a long-circulating PEGylated nanoliposome (ORI@PD-Lipo) with 1,2-distearoylphosphoethanolamine- polyethyleneglycol-amine (DSPE-PEG2000-NH2) to deliver oridonin, one of the active ingredients in Rabdosia rubescens (R. rubescens) in this study. For improving tumor-targeting delivery of oridonin, a pancreatic cancer targeting CKAAKN peptide was used to modify the nanoliposome (ORI@CPD-Lipo). Our results showed that ORI@CPD-Lipo had good stability and biosafety with average particle size of about 100 nm, which could selectively internalize into pancreatic cancer cells BxPC-3 during the short incubation time (1–4 h) in vitro under the mediation of CKAAKN peptide, compared with HPDE6-C7 cells. Furtherly, significantly higher uptake of ORI@CPD-Lipo nanoparticles by BxPC-3 tumors (positive-CKAAKN) than normal pancreatic tissue was observed in vivo during the whole experiment process (1–48 h), with increased ratio on experiment time. Our data also indicated the treatment of BxPC-3 cells with ORI@CPD-Lipo nanoparticles showed significantly enhanced antitumor effect and therapeutic efficacy than the treatment with the free ORI, non-targeting ORI@Lipo and CKAAKN-blocking ORI@CPD-Lipo. The enhanced antitumor activity to BxPC-3 cells should be attributed to the enhanced drug cellular uptake mediated by ORI@CPD-Lipo nanoparticles, chemical toxicity of the released ORI from the nanoparticles. Our study provided a valuable reference and strategy of CKAAKN-mediated targeting cancer chemotherapy based on ORI@CPD-Lipo against the pancreatic tumor.
Similar content being viewed by others
Introduction
Pancreatic cancer remains a highly lethal malignancy. It is projected to become the second leading cause of cancer-related deaths over the next 20 to 30 years and has been termed the “king of cancers” by the medical community1. Currently, the 5 years relative survival rate for patients with pancreatic cancer is approximately 10%, while 80% to 85% of patients with unresectable or metastatic tumors2. Even among those with surgically resectable pancreatic tumors, the 5 years post-surgical survival rate is only 20%3. Clinically, the insidious onset of pancreatic cancer means that by the time of diagnosis, most patients already have advanced disease and are prone to metastasis to the liver and other distant organs, thereby losing the opportunity for radical surgical resection. Despite significant advances in the understanding of pancreatic cancer biology, improvements in surgical techniques, and the development of new therapeutic agents4, the 5 years survival rate for pancreatic cancer remains below 8%5.
Surgical resection is the primary treatment for pancreatic cancer. However, due to the lack of specific clinical manifestations, most patients present with metastatic disease or invasion of peripancreatic blood vessels at the time of initial diagnosis, resulting in a low surgical resection rate. Even for those who undergo resection, the postoperative recurrence rate is high, and the overall prognosis remains extremely poor. Only about 20% of patients are eligible for surgery, and among them, only approximately 50% are cured6. Local recurrence is the primary reason for failure of surgical treatment. Chemotherapy, which employs first-line anticancer drugs such as paclitaxel and cisplatin7, represents the principal method to alleviate clinical symptoms and improve quality of life in patients with advanced pancreatic cancer. However, its application is severely limited by significant clinical challenges, including toxicity and drug resistance8,9. Furthermore, the development of multidrug resistance in tumor cells constitutes a major obstacle to cancer therapy and often leads to treatment failure10. Therefore, the development of new, low-toxicity, and highly effective anti-tumor drugs that can specifically target cancer cells is of great practical importance for the treatment of pancreatic cancer.
Rabdosia rubescens (Hemsl.) Hara, a traditional Chinese medicinal plant belonging to the family Lamiaceae (formerly Labiatae), has stems and leaves that are used medicinally for their anti-inflammatory, analgesic, heat-clearing, fire-purging, qi-activating, blood-invigorating, and anti-tumor properties. Oridonin (ORI), one of its active components, is a natural carbon-containing compound belonging to the class of tetracyclic diterpenoids of the class of mesquiterpenoids (Entkaurene), with a chemical formula of C20H26O711. Clinical studies have shown that ORI inhibits tumor cell activity and can significantly suppress the growth and proliferation of more than 20 types of common cancer cells in vivo. It is primarily used in the treatment of several cancers, including pancreatic, liver, gastric cardia, breast, ovarian, and esophageal cancers12,13. Research indicates that ORI inhibits the growth of pancreatic cancer cell line PANC-1 by inducing G2/M cell cycle arrest and promoting apoptosis. The underlying mechanism may involve altering the Bax/Bcl-2 expression ratio and activating caspase-314. Importantly, a recent study further supports its translational potential, particularly highlighting its value in pancreatic cancer research and diagnosis15. It is expected to be an excellent drug candidate for the treatment of pancreatic cancer. However, like many first-line chemotherapeutic agents, ORI suffers from poor solubility, low bioavailability, and potential biotoxicity. There is an urgent need to develop novel delivery systems to transport ORI to tumor sites, thereby minimizing its toxic side effects, improving bioavailability, and achieving effective treatment of pancreatic cancer.
The advancement of nanotechnology has demonstrated significant potential in biomedical fields such as drug delivery and gene therapy. Various nano-delivery systems, including liposomes16, nanoemulsions17, magnetic nanoparticles18, gold nanoparticles19, polymer micelles20, as well as chitosan21 and hyaluronic acid22-based nano-delivery systems, are essentially drug carriers that enhance drug efficacy upon administration23. A key advantage of these carriers lies in their ability to control the site, rate, and mode of drug release with high selectivity. Among them, nanoliposomes represent an amphiphilic drug delivery system characterized by a phospholipid bilayer structure. They are capable of encapsulating both hydrophilic and lipophilic drugs, exhibit good cell affinity and histocompatibility, and can improve drug stability24,25. However, conventional liposomes are prone to rapid uptake by the mononuclear phagocyte system. In contrast, long-circulating liposomes modified with DSPE-PEG2000-NH2—an amphiphilic phospholipid conjugate composed of DSPE (1,2-distearoyl-sn-glycerol-3-phosphoethanolamine) and polyethylene glycol 2000 (PEG2000)—provide a promising strategy to reduce phagocytic clearance, prolong systemic circulation, and enhance the bioavailability of encapsulated drugs. Nevertheless, although PEGylation extends the circulation time, these liposomes still lack active tumor-targeting capability and require further surface functionalization with specific targeting ligands.
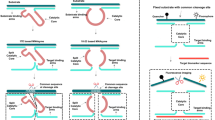
Tumor homing peptides are a class of high-affinity peptides screened by phage display technology, serving as specific targeting ligands. They exhibit advantages such as low molecular weight, ease of synthesis, low immunogenicity, abundant source materials, and metabolites that are readily degraded in vivo26. Among them, CKAAKN is a novel phage-derived tumor homing peptide, a linear amino acid sequence capable of targeting both tumor cells and neovascular endothelial cells. The binding mechanism of CKAAKN to tumor cells primarily mimics the specific interaction between Wnt proteins and pancreatic cancer cell membrane receptors via the Wnt-2 signalling pathway, with minimal binding to normal pancreatic tissue27,28,29. To enhance the tumor targeting of liposomes, the CKAAKN peptide was conjugated to DSPE-PEG2000-NH2 via an amidation reaction. In this study, we constructed CKAAKN-functionalized long-circulating liposomes for the delivery of ORI (ORI@CPD-Lipo). This system shows potential for targeted ORI delivery into tumor cells, enabling efficient and precise treatment of pancreatic cancer (Fig. 1).
Schematic illustration of the CKAAKN peptide-conjugated long-circulating nanoliposome (ORI@CPD-Lipo) for targeted delivery of oridonin to pancreatic cancer.
Results
Synthesis and characterization of CKAAKN-NH-PEG2000-DSPE
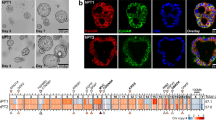
In this study, a pancreatic cancer-targeting peptide, CKAAKN, screened by phage display technology, was selected30,31,32,33. CKAAKN exhibited two characteristic peaks at 4.18–4.37 ppm and 2.82–3.01 ppm. The signal at 4.18–4.37 ppm corresponds to the methine proton of a-amino acid moiety (–CH–) in CKAAKN (Fig. 2a), while the peak at 2.82–3.01 ppm was attributed to the methylene protons adjacent to the imine group (-CH2-) (Fig. 2d). DSPE-PEG2000–NH2 showed three characteristic peaks at 3.98–4.22 ppm, 3.42–3.68 ppm and 1.13–1.34 ppm. The signal at 3.98 ~ 4.22 ppm arised from the methylene protons (–CH2–) linked to an ether bond at one end and an amide bond at the other (Fig. 2b). The peak at 3.42–3.68 ppm corresponds to the methylene protons adjacent to the ether bond (–CH2–) in the PEG chain (Fig. 2c), and the signal at 1.13–1.34 ppm was assigned to the methylene protons in the aliphatic hydrocarbon chains of DSPE (–CH2–) (Fig. 2e). As shown in the spectra, the product CKAAKN-NH-PEG2000-DSPE retained all characteristic peaks at positions consistent with those of both CKAAKN and DSPE-PEG2000-NH2 (Fig. 2a–e), confirming the successful synthesis of the targeted phospholipid conjugate CKAAKN-NH-PEG2000-DSPE (Fig. 2).
1H-NMR spectra of CKAAKN, DSPE-PEG2000-NH2, CKAAKN-NH-PEG2000-DSPE.
Establishment of a method for the determination of ORI content
To accurately determine the encapsulation efficiency and drug loading capacity of liposomes, the optimal detection wavelength for ORI was identified as 240 nm using high-performance liquid chromatography (HPLC). Specificity tests confirmed that neither solvents nor excipients interfered with the interfered ORI. Both the control solution and test solutions exhibited satisfactory peak shapes and consistent retention times, indicating high specificity of the analytical method (Fig. S1A). The standard curve for ORI was established as Y = 33.756X-131.59 (r = 0.9999), demonstrating good linearity over the mass concentration range of 5–500 μg/mL (Fig. S1B).
Precision testing demonstrated good intraday repeatability, with relative standard deviations (RSD) of peak areas measured at 0.59%, 0.08%, and 0.13% for ORI at low, medium, and high mass concentrations (5, 50, and 250 μg/mL), respectively (Table S1). The interday precision RSD for three batches of non-targeted liposomes (ORI@Lipo) and targeted liposomes (ORI@CPD-Lipo) were 1.18%, 0.65%, 1.14%, 1.41%, 0.35%, and 0.20%, respectively (Table S2, S3), confirming satisfactory instrument precision. Repeatability experiments showed an RSD of 0.07% for the ORI peak area (Table S4), indicating high methodological reproducibility. Stability testing revealed that the ORI@Lipo solution remained stable over 24 h, with a peak area RSD of 0.53% (Table S5). In addition, the average recovery experiment of ORI@Lipo was 97.09% with a RSD of 0.98% (Tables S6-S8), confirming that the method meets the required standards.
Preparation and characterization of ORI@CPD-Lipo
The preparation process of ORI@CPD-Lipo is influenced by several factors. We investigated the effects of phospholipid type, phospholipid-to-cholesterol mass ratio, phospholipid concentration, and hydration time on the particle size and encapsulation efficiency of liposomes.
Effect of phospholipid type
Liposomes prepared using hydrogenated soybean lecithin and lecithin via the membrane dispersion method were found to be difficult to pass through a 0.22 μm microporous filter. The measured particle size was excessively large and did not fall within the nanoscale range, suggesting that nanoparticles may not have formed successfully. When egg yolk lecithin was used, the liposomes remained stable even after the addition of methanol as an emulsion-breaking agent. In contrast, liposomes prepared from soybean lecithin exhibited stable particle size characteristics, with an average size of (120 ± 1.2) nm, a PDI of (0.238 ± 0.001), and an encapsulation efficiency of (85.73 ± 1.82) %. Furthermore, these liposomes effectively release ORI upon emulsion disruption. Based on these results, soybean lecithin was selected as the phospholipic for ORI loading.
Effect of phospholipid-to-cholesterol mass ratio
Evaluation of the phospholipid-to-cholesterol mass ratio demonstrated that a 6:1 ratio of soybean phospholipids-to-cholesterol resulted in a higher encapsulation efficiency, the smallest particle size, as well as the lowest zeta potential and PDI. The incorporation of cholesterol enhanced the stability of the lipid bilayer and reduced drug leakage from the liposome; however, excessive cholesterol could hinder liposome formation. Based on these findings, a soybean phospholipid to cholesterol mass ratio of 6:1 was selected for the subsequent single-factor experiment (Fig. S2).
Effect of phospholipid concentration
Phospholipid concentration influences the zeta potential of liposomes, which reflects their surface charge properties. Liposomes are generally considered stable when the zeta potential exceeds + 30 mV or is less than –30 mV, as a strong surface charge helps prevents aggregation34,35. In this study, the evaluation of different phospholipid concentrations revealed that at 7%, the zeta potential reached its minimum value below − 30 mV, while the encapsulation efficiency was highest, and the particle size and PDI were the smallest. Therefore, a phospholipid concentration of 7% was selected for subsequent studies, under which the liposomes exhibited optimal stability (Fig. S3).
Effect of hydration time
In the thin-film dispersion method, an orderly rearrangement of the dried phospholipid films has occurred. Upon hydration, the ordered phospholipid layers detach from the vessel surface and curl to form liposomes. Regardless of the preparation method used, hydration was a critical step, making it essential to control appropriate hydration conditions. Hydration must be performed above the phase transition temperature of the phospholipid, and the duration of hydration influences both the structure of the resulting liposome, and the drug encapsulation efficiency. Insufficient hydration time can lead to incomplete hydration of phospholipids, resulting in uneven particle size distribution or even phospholipid precipitation, which severely compromises product quality. Conversely, excessively long hydration may promote drug degradation. Evaluation of hydration time revealed that a duration of 45 min yielded liposomes with the highest encapsulation efficiency, the smallest particle size and PDI, and a relatively low zeta potential (Fig. S4).
Box-Behnken response surface analysis
Based on the results of the single-factor experiments, phospholipid amount (X1), phospholipid concentration (X2), and hydration time (X3) were selected as independent variables, with encapsulation efficiency (Y) as the response index. The cholesterol amount was fixed at 10 mg, and the range of each factor was determined accordingly. The liposome formulation process was subsequently optimized using Box-Behnken design combined with response surface methodology. The factors examined, experimental design, and corresponding results are summarized (Table 1), and the analysis of variance ANOVA is provided (Table 2).
The encapsulation efficiency data (Table 1) were analyzed using Design-Expert 8.0.6.1 software to obtain the fitted equation: Y = 96.48–2.65X1-2.10X2 + 1.40X3-6.12X12-7.37X22-6.64X32(r = 0.9360, P < 0.05). Significance testing indicated that X1, X12, X22, and X32 in the model had a significant effect on the value of Y (P < 0.05), while the lack-of-fit term was not significant (P ≥ 0.05), indicating that the regression model fits well across the experimental domain and possesses good predictive capability. The order of factor effects on encapsulation efficiency was X1 > X2 > X3, that is, phospholipid amount > phospholipid concentration > hydration time. Response surface and contour plots for the factor interactions were generated using Design-Expert 8.0.6.1 (Fig. 3). The optimal process conditions predicted by the software for ORI@CPD-Lipo were as follows: phospholipid amount 55.67 mg, phospholipid concentration 6.86%, hydration time 46.58 min, with a predicted encapsulation efficiency of 96.99%.
Contour and response surface plots for encapsulation efficiency of ORI@CPD-Lipo. (A–B) Phospholipid amount vs. phospholipid concentration; (C–D) Phospholipid amount vs. hydration time; (E–F) Phospholipid concentration vs. hydration time.
Validation of the optimized process
The optimal formulation of ORI@CPD-Lipo was determined as follows: phospholipid amount of 55.67 mg, phospholipid concentration 6.86%, and hydration time 46.58 min. Three batches of ORI@Lipo and ORI@CPD-Lipo were prepared according to these optimized conditions. The encapsulation efficiencies of ORI@Lipo were 94.74%, 94.94%, 95.34%, while those of ORI@CPD-Lipo were 94.70%, 95.82%, 96.74%, respectively. These experimental results were compared with the predicted values from the fitted model. The relative deviation was calculated according to the formula [relative deviation = (predicted value—measured value)/predicted value]. All relative deviations between measured and predicted values were less than 5%, indicating that the optimized formulation process was stable and feasible.
In addition, both ORI@Lipo and ORI@CPD-Lipo liposomes remained stable in aqueous suspension, exhibiting bluish opalescence and a clear Tyndall effect (Fig. 4A). The mean particle sizes of ORI@Lipo and ORI@CPD-Lipo were (100.6 ± 1.5) nm and (100.3 ± 0.8) nm, respectively (Table 3), which are basically consistent with the particle size distribution observed by TEM (Fig. 4C). Both types of liposomes have a narrow particle size distribution (PDI < 0.2) and a Zeta potential of approximately − 30 mV, indicating their excellent colloidal stability.
Preparation, characterization, and stealth properties of ORI-loaded liposomal formulations. (A) Visual appearance under daylight and Tyndall light scattering of ORI@Lipo and ORI@CPD-Lipo. (B) Particle size distribution of ORI@CPD-Lipo. (C) Representative TEM images of (a) ORI@Lipo and (b) ORI@CPD-Lipo. (D) Coomassie Brilliant Blue-stained SDS-PAGE gel. The full, uncropped image of this gel is provided in the Supplementary Material. (E) Grayscale analysis of major opsonin bands (37–50 kDa) using ImageJ. (F) In vitro drug release profiles of free ORI, ORI@Lipo, and ORI@CPD-Lipo in PBS (pH 7.4).
Characterization and stealth properties of ORI@CPD-Lipo
ORI@Lipo and ORI@CPD-Lipo were prepared using the thin-film dispersion method. Transmission electron microscopy (TEM) revealed that both ORI@Lipo (Fig. 4Ca) and ORI@CPD-Lipo (Fig. 4Cb) displayed spherical or near-spherical bilayer structures, with no apparent particle aggregation and a homogeneous size distribution. The particle sizes were approximately 100 nm, consistent with the dynamic light scattering (DLS) results (Fig. 4B). Both liposomal formulations exhibited zeta potentials below − 30 mV, indicating negatively charged surfaces. Such a surface charge helps reduce aggregation and fusion, thereby enhancing colloidal stability. Compared with ORI@Lipo, ORI@CPD-Lipo appeared more transparent and exhibited stronger bluish opalescence with a more distinct Tyndall effect. This observation may be attributed to the presence of PEG chains, which form a hydrophilic protective layer on the liposome surface, improving stability and homogeneity. As a stealth liposome, ORI@CPD-Lipo contains flexible polyethylene glycol (PEG) that helps evade immune cell recognition. The PEG layer forms a hydration barrier on the surface of liposomes, which inhibits the adsorption of plasma proteins and reduces uptake by the reticuloendothelial system, thereby prolonging systemic circulation time. Additionally, the hydrophilic PEG chains enhance the cytocompatibility of the liposomes, further mitigating immune-mediated clearance.
Rapid clearance of liposomes has been attributed to their extensive uptake by the reticuloendothelial system (RES)36,37. Upon introduction into a biological medium, liposomes rapidly adsorb various proteins, forming a protein corona (PC) that facilitates recognition and capture by the RES38. Polyethylene glycolisation (PEG) modification modulates the amount and composition of proteins adsorbed onto liposomal surfaces39. To evaluate the stealth properties and potential long-circulating behavior of ORI@CPD-Lipo, liposome-protein complexes were generated by incubating ORI@Lipo and ORI@CPD-Lipo with fetal bovine serum. The stealth effect was assessed by analyzing the expression of major opsonin proteins. SDS-PAGE revealed notable differences in the PC composition between ORI@CPD-Lipo and ORI@Lipo after serum incubation (Fig. 4D). The fibrinogen gamma chain (48 KDa), a major opsonin in the liposome protein corona, migrates within the 37–50 kDa region. Densitometric analysis showed that the band intensity in this region for ORI@CPD-Lipo was 1.40-fold lower than that of non-PEGylated ORI@Lipo (Fig. 4E). These results indicated that ORI@CPD-Lipo adsorbed significantly less protein in the 37–50 kDa range, suggesting that its stealth properties may stem from reduced protein adsorption, supporting its potential as a long-circulating nanocarrier in vivo.
Stability studies indicated ORI@CPD-Lipo stored at 4 °C for 21 days exhibited no significant changes in appearance or physicochemical properties, and the solution remained homogeneous and stable. Only minor variations were observed in average particle size, PDI, zeta potential, and drug encapsulation efficiency (Fig. S5), with small variations, confirming the formulation stability over 21 days at 4 °C. In serum stability tests, the absorbance of ORI@CPD-Lipo incubated with foetal bovine serum for 24 h remained consistent at 0.1879 ± 0.0014. Furthermore, as can be seen (Fig. S6), particle size, PDI, and zeta potential showed no notable changes throughout the 24 h incubation period. Minor fluctuations in zeta potential were observed, which might be attributed to the adsorption of trace amounts of serum proteins during measurement. These results collectively demonstrate that ORI@CPD-Lipo retains its structural integrity and exhibits good stability in the presence of serum. In vitro drug release studies (Fig. 4F) showed that among all groups, the free ORI group released most rapidly, which showed near-complete release within 8 h and a cumulative release rate of (98.57 ± 0.35)%. In contrast, both ORI@Lipo and ORI@CPD-Lipo exhibited sustained release profiles, with cumulative release rates of (23.84 ± 1.02)% and (25.15 ± 1.52)%, respectively, after 48 h. These results demonstrate that liposomal encapsulation significantly prolongs drug release compared to the free ORI solution.
To elucidate the in vitro release mechanism of ORI@Lipo and ORI@CPD-Lipo, their release profiles were fitted using zero-order, one-order, Higuchi, Ritger-Peppas, and Weibull models. The Weibull model exhibited the highest correlation coefficient (R) and was therefore selected to characterize the drug release behavior. The corresponding release kinetic parameters for ORI from both liposomal formulations are summarized (Table 4), where Q represents the drug release percentage and t denotes the sampling time. No burst release was observed from either liposomes within 48 h, indicating that the drug is encapsulated within the liposomal core rather than adsorbed on the surface.
In vitro targeting of ORI@CPD-Lipo
To evaluate the specific binding of CKAAKN peptide-modified ORI@CPD-Lipo to BxPC-3 cells, we investigated the time-dependent cellular uptake of coumarin 6-labeled ORI@Lipo and ORI@CPD-Lipo in both BxPC-3 and HPDE6-C7 cells. The results demonstrated that ORI@CPD-Lipo (targeted group) was internalized more efficiently into BxPC-3 cells than ORI@Lipo (non-targeted group) within a short incubation period (< 1 h) (Fig. 5A), as confirmed by quantitative analysis using ImageJ software (Fig. 5E). Furthermore, the fluorescence intensity in BxPC-3 cells was significantly higher than that in HPDE6-C7 cells for both liposomal formulations after 24 h incubation (Fig. 5A), with quantitative results provided (Fig. 5C, D). The difference in cellular uptake between ORI@Lipo and ORI@CPD-Lipo by BxPC-3 cells increased with prolonged incubation time (1–4 h) (Fig. 5A, E). However, after 4 h of uptake, the difference in internalization between the two formulations gradually diminished. Further analysis confirmed that after 1 h of incubation, ORI@CPD-Lipo exhibited significantly enhanced cellular uptake in BxPC-3 cells compared to both HPDE6-C7 cells (p < 0.001) and the non-targeted ORI@Lipo group (p < 0.001). Moreover, the presence of free CKAAKN peptide competitively inhibited the cellular uptake of ORI@CPD-Lipo in BxPC-3 cells (p < 0.001). These results indicate that the CKAAKN peptide promotes specific binding of ORI@CPD-Lipo to CKAAKN-positive BxPC-3 cells and facilitates cellular internalization via a Wnt protein-mediated pathway (Fig. 5B, F).
Cellular uptake of coumarin 6-labeled liposomes in BxPC-3 and HPDE6-C7 cells. (A) Time-dependent uptake of ORI@Lipo and ORI@CPD-Lipo. (B) Fluorescence microscopy images after 1 h incubation. (C–D) Quantitative analysis of (A) for ORI@Lipo (C) and ORI@CPD-Lipo (D). (E) Semi-quantitative comparison of uptake in BxPC-3 cells. (F) Quantitative analysis of fluorescence intensity in (B). (G) Competitive uptake in BxPC-3 (white arrows, PKH26-labeled membrane) and HPDE6-C7 cells (yellow arrows) after 1 h co-incubation; nuclei stained with DAPI. (H) Quantitative analysis of (G). Data represent mean ± SD (n = 3); ***p < 0.001.
As shown in Fig. 5G, cellular uptake of ORI@CPD-Lipo was evaluated in a co-culture system of BxPC-3 and HPDE6-C7 cells. After 1 h of incubation, significantly stronger fluorescence was observed in CKAAKN-positive BxPC-3 cells (indicated by white arrowheads) compared to CKAAKN-negative HPDE6-C7 cells (yellow arrowheads). In contrast, this differential uptake was diminished when using non-targeted ORI@Lipo or when ORI@CPD-Lipo was co-incubated with free CKAAKN peptide (Fig. 5G). Semi-quantitative analysis using ImageJ software under the same conditions further confirmed these observations (Fig. 5H). The relative fluorescence intensities in BxPC-3 and HPDE6-C7 cells were 5.86 ± 0.29 and 0.87 ± 0.04, respectively, for ORI@CPD-Lipo alone. Upon addition of free CKAAKN peptide, these values changed to 3.08 ± 0.15 and 1.82 ± 0.09, respectively. For the non-targeted ORI@Lipo group, the fluorescence values were 3.32 ± 0.17 in BxPC-3 cells and 1.92 ± 0.10 in HPDE6-C7 cells.
These results demonstrate that free CKAAKN peptide competitively blocks specific binding to Wnt receptor-positive BxPC-3 cells, thereby reducing the cellular uptake of ORI@CPD-Lipo. The consistency between quantitative analysis and fluorescence microscopy observations supports the conclusion that ORI@CPD-Lipo selectively targets CKAAKN-positive BxPC-3 cells via Wnt protein-mediated endocytosis (Fig. 5G).
In vitro biosafety of ORI@CPD-Lipo
The in vitro biosafety of Free Lipo and CPD-Lipo was assessed in BxPC-3 and HPDE6-C7 cells using the MTT assay. After 48 h of incubation, both liposomal formulations maintained cell viability above 80% in each cell line, indicating good biocompatibility (Fig. 6A, B). Hemolysis tests further demonstrated that ORI@Lipo and ORI@CPD-Lipo exhibited hemolysis rates below 5% at high, medium, and low (2.5, 1.25, and 0.625 mg/mL), confirming their suitability for intravenous administration (Fig. 6C, D).
Biocompatibility and hemocompatibility of liposomal formulations. (A) Viability of BxPC-3 and HPDE6-C7 cells after 48 h incubation with Free Lipo. (B) Viability of BxPC-3 and HPDE6-C7 cells after 48 h incubation with CPD-Lipo. (C) Hemolysis rates of ORI@Lipo and ORI@CPD-Lipo at 0.625, 1.25, and 2.5 mg/mL. (D) Quantitative analysis of hemolysis rates. Data represent mean ± SD (n = 4).
In vitro anti-tumor activity of ORI@CPD-Lipo
Free ORI, ORI@Lipo, and ORI@CPD-Lipo all effectively inhibited the proliferation of the BxPC-3 cells in a dose-dependent manner, with the inhibitory rate increasing alongside drug concentration (Fig. 7A). Both liposomal formulations exhibited stronger cytotoxic effects than Free ORI. After 48 h of incubation with BxPC-3 cells at mass concentrations of 0.1, 0.5, 1, 2.5, 5, and 10 μg/mL, the half-maximal inhibitory concentrations (IC50) were calculated for Free ORI, ORI@Lipo, and ORI@CPD-Lipo, which were 7.305 μg/mL, 1.803 μg/mL, and 1.230 μg/mL, respectively. The IC50 value serves as an indicator of a drug to induce apoptosis, with lower values reflecting stronger potency. Compared with free ORI (IC50 = 7.305 μg/mL), both liposomal formulations showed enhanced inhibitory effects on BxPC-3 cell proliferation, with ORI@Lipo and ORI@CPD-Lipo exhibiting IC50 values of 1.803 μg/mL and 1.230 μg/mL, respectively. The inhibitory activity of ORI@CPD-Lipo was attenuated after blocking with the CKAAKN peptide, as evidenced by an increase in the IC50 value to 2.513 μg/mL. This suggests that the CKAAKN peptide competitively inhibits the targeting and cytotoxic efficacy of ORI@CPD-Lipo.
In vitro antitumor activity evaluation. (A) Viability of BxPC-3 cells treated with various drug concentrations. (B) Cell migration assessed by scratch assay in BxPC-3 and HPDE6-C7 cells. (C) Live/Dead staining of BxPC-3 and HPDE6-C7 cells after treatment with different formulations (green: live cells, red: dead cells). (D) Quantitative analysis of cell migration rates from (B). (E) Fluorescence-based viability quantification from (C). Data represent mean ± SD; (A, E) n = 4; (D) n = 3; *p < 0.05, **p < 0.01, ***p < 0.001.
The results of the cell scratch assay are presented in Fig. 7B and D. Over time, scratch closure was observed in the control groups of both HPDE6-C7 and BxPC-3 cells. The BxPC-3 cells demonstrated a higher migration rate compared to HPDE6-C7 cells, which is consistent with the greater migratory capacity of this pancreatic cancer cell line relative to the normal pancreatic ductal epithelial cells. When BxPC-3 cells were treated with the drug formulations, an increase in scratch area was noted in the ORI@Lipo (ORI 5 μg/mL), ORI@CPD-Lipo (ORI 5 μg/mL), and ORI@CPD-Lipo plus CKAAKN (ORI 5 μg/mL) groups compared to the control, indicating that the drug-loaded liposomes suppressed BxPC-3 cell migration. After 24 h of incubation, the scratch area in the ORI@CPD-Lipo group was significantly larger than that in the ORI@Lipo group. Throughout the 24 h incubation period, the cell migration rate under ORI@CPD-Lipo treatment was lower than that under ORI@Lipo treatment, demonstrating a stronger inhibitory effect of ORI@CPD-Lipo on BxPC-3 cell migration. The addition of CKAAKN peptide reduced the migration-inhibitory effect of ORI@CPD-Lipo on BxPC-3 cells. These findings suggest that the cellular uptake of ORI@CPD-Lipo is facilitated by the CKAAKN modification, which mimics the specific binding of Wnt proteins to pancreatic cancer cell membrane receptors via the Wnt signaling pathway.
The in vitro antitumor efficacy of ORI@CPD-Lipo was assessed using a Live/Dead cell staining assay. Representative inverted fluorescence microscopy images of BxPC-3 and HPDE6-C7 cells following 24 h treatment with CPD-Lipo, free ORI (5 μg/mL), ORI@Lipo (5 μg/mL), ORI@CPD-Lipo (5 μg/mL), or ORI@CPD-Lipo plus CKAAKN (5 μg/mL) are shown in Fig. 7C and E. Treatment with CPD-Lipo resulted in minimal BxPC-3 cell death, indicating low cytotoxicity and supporting its biosafety profile in vitro. In contrast, both ORI@Lipo and ORI@CPD-Lipo induced substantially higher levels of cell death in BxPC-3 cells compared to free ORI. Among all ORI-containing formulations, ORI@CPD-Lipo produced the greatest reduction in cell viability. The addition of the CKAAKN peptide along with ORI@CPD-Lipo reduced the extent of BxPC-3 cell death compared to ORI@CPD-Lipo alone. This result suggests that CKAAKN competes for receptor binding and partially attenuates the cytotoxicity of ORI@CPD-Lipo. Together with previous cytotoxicity and cell scratch assays, these data support the proposed mechanism that CKAAKN facilitates targeted internalization of ORI@CPD-Lipo into BxPC-3 cells via Wnt pathway-mediated binding.
In vivo biodistribution of targeted long-circulating liposomes
To simultaneously investigate the accumulation of non-targeted liposomes and targeted long-circulating liposomes in hormonal BxPC-3 tumor-bearing nude mice, we established an orthotopic pancreatic cancer model using BxPC-3 tumor-bearing nude mice. After intravenous injection of DiR-labeled ORI@Lipo and ORI@CPD-Lipo, we recorded the distribution of fluorescent signals of drug-carrying liposomes in vivo throughout the body of the BxPC-3 tumor-bearing nude mice.
After administration of DiR-labeled ORI@Lipo, a weak DiR fluorescence signal was observed in orthotopic BxPC-3 tumors in the in situ pancreatic cancer BxPC-3 tumor-bearing model within a short period of time, and no notable enhancement of DiR fluorescence signal was observed with the increase of time (Fig. 8A), and at this time, more passive targeting of ORI@Lipo (DiR-labeled) was accumulated into the tumor tissues, which reflects passive accumulation in tumor tissue mediated by the EPR effect. The results of fluorescence distribution in various tissues of the nude mice with BxPC-3 tumor-bearing after 48 h of execution (ex vivo fluorescence imaging of major organs at 48 h post-injection) (Fig. 8B) showed that the distribution of ORI@Lipo (DiR labeling) was the highest in the liver, and the distribution was minimal in other organs (Fig. 8C).
In vivo biodistribution of DiR-labeled liposomes in an orthotopic pancreatic cancer model. (A) Whole-body fluorescence imaging at different time points after intravenous injection. (B) Ex vivo tissue distribution at 48 h post-injection of ORI@Lipo. (C) Quantitative tissue accumulation (%ID/g) of ORI@Lipo. (D) Representative images at 48 h after ORI@CPD-Lipo injection: (a) whole-mouse photograph, (b) corresponding fluorescence image, (c) tumor and normal pancreatic tissue, (d) fluorescence of tumor and pancreas. (E) Ex vivo tissue distribution at 48 h post-injection of ORI@CPD-Lipo. (F) Quantitative tissue accumulation (%ID/g) of ORI@CPD-Lipo. Fluorescence intensity reflects liposome concentration; %ID/g denotes percentage of injected dose per gram of tissue.
In contrast, after administration of DiR-labeled ORI@CPD-Lipo, the DiR fluorescence signals in the orthotopic BxPC-3 tumors were significantly enhanced compared with those of ORI@Lipo (DiR-labeled), and the targeted distribution of ORI@CPD-Lipo (DiR-labeled) into the in situ pancreatic BxPC-3 tumors was significant, especially at 8–24 h. The BxPC-3 tumors with increasing DiR fluorescence signals, which still had a high accumulation at 48 h (Fig. 8A), indicating that due to the incorporation of the targeting phospholipid CKAAKN-NH-PEG2000-DSPE, the ORI@CPD-Lipo (DiR-labeled) has a certain degree of targeting and long-circulating function, and has a certain degree of tumor selectivity in addition to the EPR effect. This enhanced and sustained accumulation can be attributed to the incorporation of the targeting phospholipid CKAAKN-NH-PEG2000-DSPE, which confers active tumor targeting and long-circulating properties in addition to the EPR effect, with prolonged retention in the tumor region.
The fluorescence distribution results of various tissues in nude mice with in situ loaded BxPC-3 tumors after 48 h of execution (Ex vivo tissue imaging at 48 h) (Fig. 8D) showed (Fig. 8E) that ORI@CPD-Lipo (DiR-labeled) was most distributed in the liver and spleen, and low levels distributed in other organs (Fig. 8F). This suggests that we utilize this target long-circulating up to the body for in vivo tracing to explore its targeting effects in vivo and in vitro, which is expected to provide new ideas for early targeted therapy of pancreatic cancer. These findings demonstrate that the targeted long-circulating liposomes enable effective in vivo tracing and evaluation of targeting efficacy, offering a promising strategy for early targeted therapy of pancreatic cancer.
Discussion
Pancreatic cancer is a highly malignant tumor characterized by insidious onset, difficulty in early diagnosis, rapid progression, and short patient survival, making it one of the malignancies with the poorest prognosis. Although chemotherapy plays a crucial role in pancreatic cancer treatment, its ability to improve survival remains limited40. The emergence of nanomedicine has provided new opportunities for the diagnosis and treatment of pancreatic cancer. Beyond their ability to accumulate at tumor sites, nanomedicines offer several advantages, including targeted delivery, sustained release, and versatility in dosage forms and routes of administration. Additionally, nanomedicines can reduce drug-related toxic side effects and protect bioactive substances from enzymatic degradation during delivery, thereby preserving their structural integrity and biological activity. Among various nanocarriers, liposomes represent one of the major and most successfully translated classes of nanomedicines in clinical applications for anti-tumor therapy41.
However, the majority of nanomedicine-based therapeutics remain in the stage of basic research or clinical trials and face several challenges and dilemmas. A major point of debate revolves around the enhanced permeability and retention (EPR) effect of nanomedicines in solid tumors. The EPR effect describes the phenomenon in which certain macromolecules of a specific size—such as liposomes, nanoparticles, and some macromolecular drugs—permeate more readily into tumor tissues and are retained there longer compared to normal tissues. At the time of its discovery, the EPR effect was considered an Achilles’ heel of cancer, expected to enable efficient accumulation of nanomedicines at tumor sites and thereby improve oncology treatments42. However, recent evidence indicates that the average tumor uptake of nanomedicines is only about 0.7% of the injected dose. In fact, the delivery of nanomedicines into tumor tissues and cells constitutes a complex and multistep process. First, nanomedicines must evade the host’s immune surveillance to avoid opsonization by serum proteins. Second, they need to be selectively delivered to the tumor site, overcome barriers such as cancer cell endocytosis, penetrate the tumor stroma, escape macrophage uptake, cope with high interstitial fluid pressure, and achieve uniform distribution throughout the tumor via slow diffusion43. Compared to this intricate in vivo journey, conventional EPR models appear oversimplified and inadequate for accurately predicting nanodrug accumulation in tumors. Furthermore, tumor accumulation of nanomedicines is not solely governed by passive targeting mechanisms like the EPR effect, but is also significantly influenced by active targeting strategies mediated by functional groups on the nanocarriers. Most importantly, the type and size of the tumor also play critical roles in determining the extent of nanomedicine accumulation and subsequent therapeutic efficacy.
Liposomes represent a class of biodegradable carrier systems capable of surface functionalization and internal modification. They exhibit high biocompatibility and can encapsulate both hydrophobic and hydrophilic drugs44. With increasing research on liposomes, significant progress has been made in achieving targeted delivery. Targeted liposomes serve as ideal drug carriers due to their high specificity, low toxicity, and capacity for sustained release, making them a focus in tumor-targeted therapy research in recent years45. These systems are designed to deliver therapeutic agents specifically to diseased tissues, thereby minimizing off-target effects. Advances in scientific tools and technology have expanded the application of targeted liposomes to various fields, including drug delivery, gene therapy, and immunotherapy. However, a major challenge hindering their clinical translation remains the low drug concentration ultimately reaching the tumor site. Therefore, functionalizing liposomes to enhance targeting has become a key research priority. A single type of targeted liposome formulation often fails to simultaneously meet the requirements for both efficacy and safety46,47. Polyethylene glycol (PEG) is the most widely used hydrophilic polymer for constructing long-circulating liposomes. While PEGylation prolongs blood circulation and promotes cellular uptake—particularly when combined with cell-penetrating peptides—its steric hindrance can also impede liposome targeting. The therapeutic efficacy of PEGylated liposomes depends on the release efficiency of the encapsulated drug. After accumulating in tumor tissue, PEGylated liposomes often remain external to tumor cells without being internalized. For drugs to exert their effect, they must first be released into the tumor interstitium before diffusing into tumor cells. The presence of transmembrane barriers significantly reduces drug uptake, underscoring the importance of studying the interaction between PEGylated liposomes and tumor cells48,49. Moreover, conventional PEG derivatives coupled to liposomes via non-degradable chemical bonds may resist breakdown in vivo, further impairing phagocytosis by target cells and limiting drug bioavailability50.
To address these limitations, structural modifications were applied to liposomes in this study using stealth and targeting strategies, enabling prolonged systemic circulation and active tumor targeting. In this study, ORI@Lipo and ORI@CPD-Lipo were prepared via the thin-film dispersion method. The resulting liposomes exhibited a particle size of approximately 100 nm and an encapsulation efficiency exceeding 90%, which favors complete drug release within tumor tissue. Liposomes prepared under the optimized formulation demonstrated improved stability and a sustained release profile. Furthermore, the incorporation of the functionalized phospholipid CKAAKN-NH-PEG2000-DSPE aided in evading clearance by the reticuloendothelial system, thereby preserving both long-circulating properties and targeted recognition capabilities. Meanwhile, the targeted long-circulating liposome facilitates the transport of drugs into the tumor vasculature, enhancing tumor suppression. This approach also helps minimize drug leakage in the bloodstream prior to reaching tumor tissue, effectively improving drug stability and promoting drug accumulation at the tumor site.
The ORI@Lipo and ORI@CPD-Lipo prepared in this study exhibited hemolysis rates below 5% at high, medium, and low concentrations, indicating their suitability for intravenous administration. Meanwhile, both Free Lipo (non-targeted empty liposomes) and CPD-Lipo (targeted empty liposomes) also demonstrated good biosafety. After 48 h of incubation with various concentrations of Free Lipo and CPD-Lipo, the viability of BxPC-3 and HPDE6-C7 cells remained above 80%. Liposomal encapsulation significantly enhanced the cellular uptake of ORI by pancreatic cancer cells, and ORI@CPD-Lipo showed higher uptake in BxPC-3 cells compared to ORI@Lipo. Since ORI lacks intrinsic fluorescent properties, coumarin 6-labeled ORI@Lipo and ORI@CPD-Lipo were used for in vitro targeting studies (removed “in this experiment”). Previous reports have shown that nanoparticles functionalized with the CKAAKN peptide can enter tumor cells via Wnt protein-mediated endocytosis30,31, suggesting that the targeting ability of ORI@CPD-Lipo may be attributed to the mechanism by which CKAAKN binds to tumor cells. This mechanism primarily mimics the specific binding of Wnt proteins to membrane receptors of pancreatic cancer cells through the Wnt pathway, thereby facilitating greater uptake of ORI into tumor tissues. These findings support the potential of CKAAKN-modified nanoliposomes to enhance affinity and transport efficiency for pancreatic cancer BxPC-3 cells.
In the cellular uptake assay, the ORI@CPD-Lipo plus CKAAKN group shows reduced uptake compared to the ORI@CPD-Lipo group alone. ORI@CPD-Lipo can be selectively internalised into CKAAKN-positive pancreatic cancer cells through specific binding between the CKAAKN peptide and corresponding membrane receptors, as demonstrated by time-dependent uptake studies, short-term, and competitive uptake studies consistently. Cytotoxicity assays, cell scratch assay, and dead and live cell staining further indicated that ORI@CPD-Lipo, a CKAAKN peptide-modified liposome, could specifically enter BxPC-3 cells and exert enhanced chemotherapeutic effects. To monitor in vivo distribution, liposomes were loaded with the near-infrared dye DiR and administered to tumor-bearing mice. Real-time imaging revealed that CKAAKN-functionalized long-circulating liposomes efficiently targeted BxPC-3 xenografts, with a pronounced long-circulation effect observed within 48 h. Moreover, CKAAKN-modified DiR liposomes showed enhanced accumulation at the tumor site, indicating improved targeting capability. This effect can be attributed to the combined action of the enhanced permeability and retention (EPR) effect and active targeting mediated by CKAAKN. The in vitro antitumor activity results were consistent with those of the targeting studies, suggesting that the enhanced inhibitory effect of drug-loaded liposomes on tumor cell proliferation may be associated with increased cellular uptake of ORI@CPD-Lipo. Together, these findings demonstrate that targeted liposomal delivery enables more effective treatment of pancreatic cancer. In summary, this study successfully constructed a tumor-homing peptide-based nano-delivery system using ORI as a model drug, achieving a safer and more efficient nanotherapeutic strategy for the precise treatment of pancreatic cancer.
In this study, we successfully constructed CKAAKN-modified stealth liposomes with significant pancreatic cancer-targeting ability and systematically verified their active targeting performance at the tumor site through a series of experiments. Meanwhile, we conducted a preliminary exploration of the Wnt pathway-mediated internalization mechanism and obtained strong indirect evidence based on competitive inhibition experiments, which provides a clear direction for subsequent molecular mechanism research. The current study mainly focuses on verifying the targeting ability and preliminary anti-tumor effect of this delivery system. Experimental results also show that the modified liposomes can significantly enhance drug accumulation at the tumor site and exhibit good anti-tumor activity in in vitro experiments. Of course, we acknowledge some limitations of this study, such as the lack of in vivo efficacy verification, which will be the focus of our next research. Additionally, we plan to further clarify the mechanism of Wnt pathway-mediated tumor targeting in future work by detecting key signaling molecules such as β-catenin and using specific pathway inhibitors. Nevertheless, we still believe that this study can provide new ideas and lay a solid foundation for the targeted therapy of pancreatic cancer, and is expected to promote the clinical translation of pancreatic cancer-targeted formulations.
Conclusion
Pancreatic cancer is a devastating disease with a high mortality rate. Chemotherapy is the main treatment modality for pancreatic cancer. However, the limited efficacy of most chemotherapeutic agents severely restricts their clinical utility. In this study, we developed a long-circulating and pancreatic cancer-targeting nanoliposome, ORI@CPD-Lipo, to deliver oridonin, an active component of Rabdosia rubescens (R. rubescens), in order to overcome the inefficiency of conventional chemotherapy on cancer. Our results demonstrate that ORI@CPD-Lipo exhibits favorable stability and biosafety, which could selectively internalize into pancreatic cancer cells BxPC-3 both in vitro and in vivo through CKAAKN peptide mediation. In addition, ORI@CPD-Lipo nanoparticles significantly enhanced antitumor efficacy compared with the free ORI, non-targeted ORI@Lipo, and CKAAKN-blocked ORI@CPD-Lipo, which could be attributed to improved drug cellular uptake mediated by ORI@CPD-Lipo nanoparticles and the cytotoxic effects of the released ORI from the nanoparticles. Our study offers a promising targeted reference and strategy of CKAAKN-mediated targeting of cancer chemotherapy based on ORI@CPD-Lipo against the pancreatic tumor for the treatment of pancreatic cancer.
Materials and methods
Materials
Soybean lecithin was purchased from Shanghai Sarn Chemical Technology Co. Cholesterol and 1-(3-dimethylaminopropyl)-3-ethylcarbodiimide hydrochloride (EDC) were purchased from Aladdin Biochemical Technology Co. (Shanghai, China). Lecithin, hydrogenated lecithin, and N-hydroxybutanediimide (NHS) were purchased from McLean Biochemical Technology Co (Shanghai, China). Oridonin (98% purity) was purchased from Dongkangyuan Science and Technology Co. (Wuhan, China). CKAAKN peptides were purchased from Dangang Biological Technology Co. (Wuhan, China). DSPE-PEG2000-NH2 was purchased from Aivito Pharmaceutical Technology Co. (Shanghai, China). 2% phosphotungstic acid negative staining solution, egg yolk lecithin, PBS phosphate buffer solution, and tetramethyl azole salt (MTT) were purchased from Solepol Technology Co. (Beijing, China). RPMI.1640 culture medium and DMEM high sugar culture medium were purchased from Senrui Biotechnology Co. (Zhejiang, China). Fetal bovine serum (FBS) was purchased from Biotech. (Germany). A Live-dead cell staining kit was purchased from Thermo Fisher Scientific. (USA). Chloroform and glacial acetic acid were purchased from Sinopharm Group Co. (Shanghai, China). Other reagents are analytically pure.
Animals and cell culture
BALB/c-nu nude mice (specific pathogen-free [SPF] grade, female, weighing 20–25 g) were purchased from Biotechnology Co. Ltd (Beijing, China) (Certificate No. SCXK (Jing) 2019–008). Upon arrival, the mice were housed in individually ventilated cage (IVC) systems under SPF conditions at the Animal Research Institute of Guizhou University of Traditional Chinese Medicine. The ambient temperature was maintained at 22–25 °C with a relative humidity of 40–70%. All animals had ad libitum access to food and water and were kept under a standard light–dark cycle. The animal study protocol was approved by the Animal Ethics Committee of Guizhou University of Traditional Chinese Medicine (Grant No. 20230022). The BxPC-3 (human pancreatic cancer cell lines) and HPDE6-C7 (human normal pancreatic ductal epithelial cell line) cells were purchased from Wuhan Punosai Life Science and Technology Co. (Wuhan, China). The cells were cultured in RPMI 1640 medium containing 10% FBS and dual 1% antipenicillin-streptomycin, and were placed in a continuous culture in a carbon dioxide incubator containing 5% CO2 at a saturated humidity of 37 °C.
Synthesis of CKAAKN-NH-PEG2000-DSPE
CKAAKN peptide (11.60 mg) was accurately weighed and dissolved in 4 mL of deionized water. Subsequently, 34.16 mg of EDC and 6.00 mg of NHS were added to activate carboxylic acid groups on the peptide for 2 h at room temperature. Then, 50.20 mg of DSPE-PEG2000-NH2 was introduced, and the reaction mixture was stirred magnetically for 24 h. The resulting solution was dialyzed for 48 h and lyophilized to obtain the CKAAKN-modified phospholipid, CKAAKN-NH-PEG2000-DSPE. The structure of the conjugate was verified by 1H nuclear magnetic resonance (1HNMR) spectroscopy.
Preparation of ORI@CPD-Lipo
ORI@CPD-Lipo was prepared using the thin-film dispersion method. Precisely weighed amounts of CKAAKN-NH-PEG2000-DSPE (1.36 mg), soybean lecithin (54.31 mg), cholesterol (9.27 mg), and oridonin (2 mg) were transferred into a round-bottom flask and dissolved in a chloroform–methanol mixture (1:1, v/v) to form a homogeneous solution. The organic solvent was removed by rotary evaporation at 45 °C to form a uniform lipid film, which was further dried overnight under vacuum at 40 °C. The film was hydrated with 10 mL phosphate buffer (pH 7.2–7.4) under sonication for 40 min, followed by shaking until complete dispersion. The resulting suspension was probe-sonicated (JY series, Ningbo, China) for 50 cycles (100 W, pulse on 2 s, off 3 s) and then passed through a 0.22 μm microporous filter membrane twice to obtain ORI@CPD-Lipo. The encapsulation efficiency and drug loading of ORI@CPD-Lipo were determined by the ultrafiltration centrifugation. The content of ORI was quantified via HPLC, and the mass of encapsulated ORI (M1) was used to calculate EE and DL according to the following Eqs. (1) and (2).
where M1, M2, and M3 represent the mass of ORI in liposomes (mg), the total mass of ORI added (mg), and the total mass of soybean lecithin, cholesterol and, ORI added (mg), respectively.
Establishment of a method for the determination of ORI content
Chromatographic conditions
The content of ORI was determined by high-performance liquid chromatography (HPLC) using a Wondasil C18 column (5.46 mm × 250 mm, 5 μm). The mobile consisted of methanol–water (56:44, v/v), delivered at a flow rate of 0.8 mL/min. The column temperature was maintained at 30 °C, and detection was performed at 240 nm with an injection volume of 20 μL.
Specificity
Accurately weigh 10 mg of ORI reference standard in a 10 mL volumetric flask, add methanol, and dissolve by sonication. Dilute to volume with methanol to obtain a stock solution with a mass concentration of 1 mg/mL. Appropriately dilute the stock solution with a mass concentration of 100 μg/mL as the control solution. Transfer 0.5 mL of ORI@Lipo and ORI@CPD-Lipo into separate containers, add appropriate methanol to disrupt the liposomal structure, and mix by vortexing and sonication until a clear solution is obtained, indicating complete disruption. Filter the test solutions through a 0.22 μm microporous membrane. Take the blank liposome (Free Lipo) and the targeting blank liposome (CPD-Lipo). Prepare negative control solutions in the same manner using blank liposomes (Free Lipo) and targeted blank liposomes (CPD-Lipo). Using the negative control as a blank, analyze the control and test solutions under the chromatographic conditions specified in the “Chromatographic conditions“ section, and record the resulting chromatograms.
Linearity
Accurately pipette an appropriate volume of the ORI reference stock solution (as described in the “Specificity” section) and dilute with methanol to form a series of standard solutions with mass concentrations of 5, 10, 50, 250, and 500 μg/mL. Analyze each solution following the chromatographic conditions outlined in the “Chromatographic conditions” section and record the corresponding peak areas. A standard curve was constructed by plotting the mass concentration of ORI (X) against the peak area integral (Y).
Precision
Intraday precision: Appropriate volumes of the ORI reference stock solution were accurately pipetted and diluted with methanol to prepare working solutions at low, medium, and high mass concentrations (5, 50, and 250 μg/mL). Each solution was injected 6 times under the chromatographic conditions described in the “Chromatographic conditions”, and the precision was evaluated based on the repeatability of peak areas. Interday precision: 3 batches each of ORI@Lipo and ORI@CPD-Lipo were analyzed over 3 consecutive days. The relative standard deviation (RSD) of the ORI peak area was calculated to assess interday precision.
Repeatability
Six replicates from the same batch of ORI@Lipo were processed into test solutions as described in the “Specificity” section and analyzed under the designated Chromatographic conditions; the relative standard deviation (RSD) of ORI peak area was calculated to evaluate method repeatability.
Stability
The stability of the disrupted ORI@Lipo solution was assessed by HPLC analysis at 0, 2, 4, 8, 16, and 24 h. The peak area of ORI@Lipo was recorded at each time point, and its RSD value was calculated to evaluate sample stability.
Recovery
Six aliquots (0.6 mL each) of ORI@Lipo were spiked with 0.4 mL of ORI reference solution (1 mg/mL), and the resulting mixtures were processed into test solutions, following the procedure described in the “Specificity” section. Analysis was performed under the designated chromatographic conditions, and the spike was calculated accordingly.
Optimization of ORI@CPD-Lipo preparation process
Single-factor experiments
Multiple factors influence the preparation of ORI@CPD-Lipo. In this study, single-factor experiments were conducted to systematically evaluate the effects of phospholipid type, phospholipid to cholesterol mass ratio, phospholipid concentration, and hydration time on the particle size, polydispersity index (PDI), zeta potential, and encapsulation efficiency of the liposomes.
Screening of phospholipid type
The quality of film formation is critical in liposome preparation via the thin-film dispersion method. Under fixed conditions where the phospholipid-to-cholesterol mass ratio was 3:1 and a hydration volume of 10 mL, different types of phospholipids were selected according to their appropriate film-forming temperatures. Liposomes were prepared as described in Sect. 2.5. Particle size, PDI, and zeta potential were measured using a nanoparticle analyzer (BECKMANK DelsaMax, USA), and encapsulation efficiency was determined following the method outlined in “Determination of liposome encapsulation rate and drug loading capacity”.
Effect of phospholipid-to-cholesterol mass ratio
With the hydration solvent volume set at 10 mL, and other formulation components and process conditions held constant, liposomes were prepared at phospholipids-to-cholesterol mass ratios of 1:1, 2:1, 3:1, 4:1, 5:1, 6:1, and 7:1, according to the method described in “Preparation of ORI@Lipo and ORI@CPD-Lipo”. Encapsulation efficiency was calculated as outlined in “Determination of liposome encapsulation rate and drug loading capacity”, while particle size, polydispersity index (PDI), and zeta potential were measured using a nanoparticle size analyzer.
Effect of phospholipid concentration
With other formulation components and process conditions held constant, the influence of phospholipid concentration on liposome formation was investigated by adjusting the hydration volume. Phospholipid concentrations were tested at 4%, 5%, 6%, 7%, 8%, and 10%. Liposomes were prepared as described in the “Preparation of ORI@Lipo and ORI@CPD-Lipo” section. Particle size, polydispersity coefficient (PDI), and zeta potential under nanoparticle size analyzer, and encapsulation efficiency were determined according to the method in “Determination of liposome encapsulation rate and drug loading capacity”.
Effect of hydration time
With other process conditions and formulation composition held constant, hydration time was varied as 15, 30, 45, 60, 75, 90, and 105 min. Liposomes were prepared as described in “Preparation of ORI@Lipo and ORI@CPD-Lipo”. Particle size, polydispersity coefficient (PDI), and zeta potential were measured using a nanoparticle size analyzer, and encapsulation efficiency was determined according to the method in “Determination of liposome encapsulation rate and drug loading capacity”.
Box-Behnken response surface analysis
A response surface design was established using Design Expert 8.0.6.1 software. Based on the single-factor experiments, significant variables and their optimal ranges were identified. Three factors exhibiting pronounced effects were selected as independent variables, with encapsulation efficiency (Y) as the response variable. The liposome formulation process was optimized using a Box-Behnken design combined with response surface methodology. The optimal preparation conditions were determined and subsequently validated through confirmation experiments.
Characterization of ORI@CPD-Lipo
Morphological analysis
A small amount of ORI@CPD-Lipo suspension was diluted with distilled water to an appropriate concentration, and a drop of the sample was applied onto a copper grid. After air-drying, the sample was stained with 2% phosphotungstic acid negative stain for 2 min and subsequently observed under a transmission electron microscope to examine the liposomal morphology.
Particle size and zeta potential measurement
Liposome samples were diluted fivefold with deionized water, and the particle size, polydispersity index (PDI), and zeta potential were measured using a nanoparticle sizer.
Stability study
Storage stability
The liposomes obtained after encapsulation efficiency measurement were stored at 4 °C and sampled on days 1, 2, 4, 8, 14, and 21 to monitor changes in appearance, encapsulation efficiency, particle size, and zeta potential for stability assessment.
Serum stability
An appropriate amount of ORI@CPD-Lipo solution was mixed with fetal bovine serum in a 96-well plate, and the absorbance at 490 nm was measured using a microplate reader (MULTISKAN Sky 1530, Thermo Fisher, USA) at 0, 1, 4, 8, 12, and 24 h. Serum stability was evaluated by monitoring changes in absorbance. Additionally, the stability of liposomes in serum was assessed by measuring particle size changes. Liposomes with a phospholipid concentration of 2.5 mg/mL were mixed with an equal volume of fetal bovine serum and then incubated at 37 °C under physiological conditions. Aliquots of 100 μL were collected at 0, 1, 4, 8, 12, and 24 h for particle size determination.
In vitro release study
The in vitro release behavior of ORI@CPD-Lipo was evaluated using the dialysis bag diffusion method. Precisely 1 mL of ORI@CPD-Lipo, ORI@Lipo, or free ORI solution was transferred into a dialysis bag (molecular weight cutoff: 3500 Da), which was then sealed and immersed in 10 mL of phosphate buffer (pH 7.4) maintained at (37.0 ± 0.5) °C under constant shaking at 80 rpm. At predetermined time intervals (0.5, 1, 2, 4, 6, 8, 10, 12, 24, and 48 h), 10 mL of the release medium was collected and simultaneously supplemented with an equal volume of fresh pre-warmed medium. Each sample was tested in triplicate. The drug concentration in the collected samples was quantified by HPLC as described previously, and the cumulative drug release (Q) at each time point was calculated according to Eq. (3). The release profile was plotted based on the calculated results.
V0 represents the total volume of the release medium (mL), Cn and Ci denote the drug mass concentration (mg/mL) measured at the nth and ith sampling time points, respectively, V is the sample volume withdrawn (mL), and m indicates the total mass of ORI in the sample.
In vitro steganization studies of ORI@CPD-Lipo
The DSPE-PEG2000 in ORI@CPD-Lipo helps evade phagocytosis by blood macrophages after intravenous administration and enhances liposomal stability. Western blotting was employed to evaluate the protein expression levels of the liposome-protein complex, confirming the stealth functionality of ORI@CPD-Lipo.
Protein corona (PC) preparation
Liposome-protein complexes were formed by incubating ORI@Lipo and ORI@CPD-Lipo separately with fetal bovine serum (1:1 v/v) at 37 °C for 1 h. Experimental parameters, including plasma concentration, temperature, and incubation time, were selected in accordance with previous reports35,51,52,53. After incubation, the complexes were isolated by centrifugation at 12,000 r/min for 15 min, followed by three washes with PBS to remove unbound proteins.
SDS-PAGE analysis
The composition of the liposome–protein complexes was analyzed by sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE). A 5 μL aliquot of each complex was resuspended in 20 μL of 1 × SDS-PAGE loading buffer and boiled at 100 °C for 5 min. Then, 10 μL of each sample was loaded and separated on a 10% SDS–polyacrylamide gel run at 100 V for approximately 100 min. After electrophoresis, the gel was stained overnight with Coomassie Brilliant Blue (CBB) R250. When protein bands became clearly visible, the staining solution was removed and replaced with a destaining solution containing 10% glacial acetic acid and 45% methanol. Gel images were acquired using a ChemiDoc system (Bio-Rad, USA), and band intensities were quantified graymetrically using Image J software to compare protein expression profiles between groups.
In vitro tumor targeting and transient cellular uptake study of ORI@CPD-Lipo
Coumarin-6-labeled ORI@Lipo and ORI@CPD-Lipo were used for cellular uptake studies. BxPC-3 and HPDE6-C7 cells in the logarithmic growth phase were harvested and detached with 0.25% trypsin–EDTA. The cells were resuspended in complete medium (RPMI-1640 for BxPC-3, DMEM for HPDE6-C7), supplemented with 10% fetal bovine serum and 1% penicillin–streptomycin, and diluted to a density of 3 × 104 cells/mL. The cell suspensions were seeded into 24-well plates and incubated with coumarin-6-labeled ORI@Lipo or ORI@CPD-Lipo. After incubation, the drug-containing medium was aspirated, and the cells were washed three times with PBS. Cellular uptake was monitored at 1, 2, 4, 10, and 24 h using an inverted fluorescence microscope (IX73, Olympus, Japan), and fluorescence intensity was quantified with ImageJ software.
Experimental study of cell colocalization by ORI@CPD-Lipo
Coumarin 6-labeled ORI@Lipo and ORI@CPD-Lipo were used in this experiment. Three experimental groups were established: group A (non-targeted ORI@Lipo), group B (targeted ORI@CPD-Lipo), and group C (ORI@CPD-Lipo plus CKAAKN peptide as a blocking group). BxPC-3 pancreatic cancer cells and HPDE6-C7 normal pancreatic cells in logarithmic growth phase were detached using trypsin–EDTA and seeded into 24-well plates containing coverslips at a density of 5 × 103 cells/mL. Cells were cultured at 37 °C in a 5% CO2 incubator until adherence. After cell attachment, group C was pretreated with CKAAKN peptide for 30 min, followed by incubation with coumarin 6-labeled ORI@CPD-Lipo. Meanwhile, groups A and B were treated with equivalent amounts of the corresponding liposomes. All groups were incubated for 1 h. Subsequently, cells were stained with DAPI nuclear stain for 30 min, washed with PBS (pH 7.4), fixed with 4% paraformaldehyde for 30 min, and mounted on slides. Fluorescence signals were visualized using an inverted fluorescence microscope, and intracellular fluorescence intensity was quantified with ImageJ software.
Competitive cellular uptake in co-culture system
BxPC-3 cells were stained with the fluorescent membrane dye PKH26 and co-cultured with unlabeled HPDE6-C7 cells at equal density in the same wells of a 24-well plate. After 24 h of incubation to allow cell adhesion, a BxPC-3/ HPDE6-C7 co-culture system was established.
The experiment included three groups: non-targeted liposome(coumarin 6-labeled ORI@Lipo), targeted liposome (coumarin 6-labeled ORI@CPD-Lipo), and a blocking group (coumarin 6-labeled ORI@CPD-Lipo plus CKAAKN peptide). Following cell attachment, the blocking group was pre-incubated with CKAAKN peptide for 30 min, followed by the addition of ORI@CPD-Lipo. Meanwhile, the other groups received corresponding liposomes at equivalent concentrations, and all groups were incubated for 1 h. Cells were then stained with DAPI for 30 min, washed with PBS (pH 7.4), fixed with 4% paraformaldehyde for 30 min, and mounted. Competitive cellular uptake of liposomes in the two cell types was visualized using an inverted fluorescence microscope, and fluorescence intensity was semi-quantitatively analyzed with ImageJ software.
In vitro safety evaluation
Cytocompatibility
The in vitro biosafety of Free Lipo and CPD-Lipo was assessed in BxPC-3 and HPDE6-C7 cells using the MTT assay. Cells were seeded into 96-well plates at 5 × 103 cells/well and cultured for 24 h at 37 °C in a 5% CO2 incubator. Then, 10 μL of Free Lipo or CPD-Lipo at mass concentrations of 0.1, 1, 10, 20, 50, 100, 200, 500, 1000, and 1400 μg/mL was added to respective wells, followed by incubation for 48 h under the same conditions. After treatment, 20 μL of MTT solution (5 mg/mL) was added to each well and incubated for 4 h. The supernatant was carefully removed, 100 μL of DMSO was added to dissolve the formazan crystals, and the plates were shaken for 5 min. Absorbance was measured at 490 nm using a microplate reader. Cell viability was calculated according to Eq. (4):
In the Equation, Asample represents the absorbance of cells treated with different concentrations of Free Lipo or CPD-Lipo and subsequently incubated with MTT; Acontrol denotes the absorbance of cells cultured in complete medium with MTT; Ablank corresponds to the absorbance of complete medium supplemented with MTT alone.
Hemolysis assay
Blood (2 mL) was collected from the posterior vena cava of C57/BL 6 J mice into anticoagulant tubes and centrifuged at 3000 r/min for 10 min at 4 °C. The supernatant was removed, and the erythrocytes were washed with 0.9% saline by repeated centrifugation until the supernatant became colorless. A 4% erythrocyte suspension was prepared using 0.9% saline as diluent. Lyophilized ORI@Lipo and ORI@CPD-Lipo were weighed and dissolved in 0.9% saline to obtain 3 mass concentrations (2.5, 1.25, and 0.625 mg/mL). Each solution was filtered through a 0.22 μm membrane and transferred into clean tubes. Equal volumes (1:1) of each liposome solution and the 4% erythrocyte suspension were mixed and incubated at 37 °C for 2 h in a water bath. After centrifugation at 3000 r/min for 5 min, the absorbance of the supernatant was measured at 540 nm. A mixture of 4% erythrocyte suspension with 0.9% saline served as the negative control, and with double-distilled water as the positive control. The haemolysis rate (HR) was calculated as follows:
A0, A1, and A2 represent the absorbance values of the negative control, experimental sample, and positive control, respectively.
In vitro anti-tumor activity
Cytotoxicity assay
The cytotoxicity of ORI@CPD-Lipo was assessed using the MTT assay. BxPC-3 cells were seeded in 96-well plates at a density of 5 × 104 cells/mL and incubated at 37 °C under 5% CO2. After cell attachment, Free ORI, ORI@Lipo, ORI@CPD-Lipo, and ORI@CPD-Lipo plus CKAAKN were added at ORI concentrations of 0.1, 0.5, 1, 2.5, 5, and 10 μg/mL, with untreated cells serving as the control (n = 3 per group). Following 48 h of incubation, 20 μL of MTT solution (5 mg/mL) was added to each well and incubated for 4 h. The supernatant was then removed, and 100 μL of DMSO was added to dissolve the formazan crystals. Plates were shaken for 30 min, and absorbance was measured at 490 nm. The cell inhibition rate was calculated using Eq. (6).
where It% represents the 48 h cell inhibition rate, Atreated is the absorbance of the treated group, and Acontrol is the absorbance of the control group.
Cell migration assay
BxPC-3 and HPDE6-C7 cells were seeded into 24-well plates at a density of (5–10) × 105 cells/mL and cultured in RPMI-1640 medium supplemented with 10% fetal bovine serum for 16–24 h to form confluent monolayers. A uniform scratch wound was created in each monolayer using a 10 μL pipette tip, and the cells were gently washed three times with PBS. The cells were then divided into four treatment groups: Control, ORI@Lipo, ORI@CPD-Lipo, ORI@CPD-Lipo plus CKAAKN. In the blocking group (ORI@CPD-Lipo plus CKAAKN), cells were pre-treated with CKAAKN peptide for 30 min before adding ORI@CPD-Lipo. The ORI concentration was maintained at 5 μg/mL in all ORI-containing groups, with three replicates per group. After treatment, the culture medium was aspirated, and the cells were washed three times with PBS. Cell migration was monitored and photographed under an inverted microscope at 0, 6, 12, and 24 h.
Live/Dead cell staining
The antitumor efficacy of liposomes was evaluated in vitro using a Live/Dead cell staining assay. BxPC-3 and HPDE6-C7 cells in the logarithmic growth phase were detached with trypsin and resuspended in RPMI-1640 medium containing 10% fetal bovine serum to form a single-cell suspension at a density of 5 × 104 cells/mL. The cells were seeded into 96-well plates and incubated for 24 h at 37 °C under 5% CO2. After cell attachment, equivalent volumes of he following formulations were added: CPD-Lipo, Free ORI, ORI@Lipo, ORI@CPD-Lipo, and ORI@CPD-Lipo plus CKAAKN, with the ORI concentration kept consistent at 5 μg/mL across all treatment groups. Following 24 h of incubation, the cells were stained using a Live/Dead staining solution (EthD-1: Calcein AM = 20 μL: 0.5 μL). After 30 min of staining, cell viability was visualized and imaged under a fluorescence inverted microscope, and the numbers of live and dead cells were quantified using ImageJ software.
In Vivo biodistribution and tumor targeting
Establishment of subcutaneous and orthotopic pancreatic cancer models
A subcutaneous pancreatic cancer model was established by injecting a BxPC-3 cell suspension (1 × 106 cells) into the right axilla of two BALB/c-nu mice. For the orthotopic model, one BAL B/c-nu mouse was anesthetized via inhalation of isoflurane using an open-circuit system (5% for induction and 2–3% for maintenance in 100% oxygen at a flow rate of 1 L/min) and placed in a supine position with all limbs gently secured. After shaving and disinfecting the surgical site, a 1.5 cm longitudinal incision was made in the left upper abdomen. The spleen was carefully lifted to expose the pancreas, and 50 μL of cell suspension (1 × 106 cells) was slowly injected into the pancreatic parenchyma using an insulin syringe with a needle depth of approximately 3 mm. To prevent leakage, the needle was held at the injection site for 30 s before withdrawal. The spleen and pancreas were returned to the abdominal cavity, and the incision was closed with layered silk sutures.
In vivo imaging
Following tail vein injection of near-infrared fluorescent DiR-labeled untargeted DiR@Lipo and targeted long-circulating liposomes (DiR@CPD-Lipo), whole-body fluorescence imaging was performed under isoflurane anesthesia using an IVIS Lumina II in vivo imaging system (Caliper Life Science, USA) at 1, 2, 4, 8, 12, 24, 36, and 48 h post-injection. At the end of the experiment, mice were euthanized by cervical dislocation under deep isoflurane anesthesia. Major organs were then excised and subjected to ex vivo fluorescence imaging to analyze the temporal distribution of targeted long-circulating liposomes in tumor-bearing mice.
Statistical analysis
Statistical analyses were performed using GraphPad Prism 8 (Graphpad Software Inc., La Jolla, CA, USA). P-values were calculated using a two-tailed Student’s t-test.
Data availability
All data generated or analysed during this study are included in this published article (and its Supplementary Information files).
References
Tang, D. et al. Identification of key pathways and genes changes in pancreatic cancer cells (BXPC-3) after cross-talk with primary pancreatic stellate cells using bioinformatics analysis. Neoplasma 66(5), 681–693 (2019).
Gyoten, M. et al. Lovastatin treatment inducing apoptosis in human pancreatic cancer cells by inhibiting cholesterol rafts in plasma membrane and mitochondria. Int J Mol Sci. 24(23), 16814 (2023).
Nerwal, A. et al. Neoadjuvant chemotherapy with chemoradiotherapy for patients with borderline resectable or locally advanced pancreatic ductal adenocarcinoma-retrospective review from a tertiary care hospital. Asia Pac. J. Clin. Oncol. 21(4), 392–398 (2025).
Yang, L. et al. Intratumoral microbiota: roles in cancer initiation, development and therapeutic efficacy. Signal. Transduct Target Ther. 8(1), 35 (2023).
Drizyte-Miller, K. et al. KRAS: the Achilles’ heel of pancreas cancer biology. J. Clin. Invest. 135(16), e191939 (2025).
Satoi, S. et al. Role of adjuvant surgery for patients with initially unresectable pancreatic cancer with a long-term favorable response to non-surgical anti-cancer treatments: results of a project study for pancreatic surgery by the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J. Hepatobiliary Pancreat Sci. 20(6), 590–600 (2013).
Jameson, G. S. et al. Response rate following albumin-bound paclitaxel plus gemcitabine plus cisplatin treatment among patients with advanced pancreatic cancer: a phase 1b/2 pilot clinical trial. JAMA Oncol. 6(1), 125–132 (2020).
Calabretta, S. et al. Modulation of PKM alternative splicing by PTBP1 promotes gemcitabine resistance in pancreatic cancer cells. Oncogene 35(16), 2031–2039 (2016).
Browning, R. J. et al. Combining sonodynamic therapy with chemoradiation for the treatment of pancreatic cancer. J. Control Release. 337, 371–377 (2021).
Zhou, G. et al. A biomimetic dual-targeting nanomedicine for pancreatic cancer therapy. J. Mater. Chem. B. 13(11), 3716–3729 (2025).
Li, X. et al. Oridonin: a review of its pharmacology. Pharmacokinetics and Toxicity. Front Pharmacol. 12, 645824 (2021).
Liu, R. et al. Erianin inhibits the progression of pancreatic cancer by directly targeting AKT and ASK1. Cancer Cell Int. 24(1), 348 (2024).
Shao, B. et al. Autophagy-dependent apoptosis induction by oridonin are mediated by ROS-dependent AMPK-mTOR-ULK1 pathway in colon cancer. Am. J. Cancer Res. 15(4), 1902–1918 (2025).
Qi, X. et al. Oridonin nanosuspension was more effective than free oridonin on G2/M cell cycle arrest and apoptosis in the human pancreatic cancer PANC-1 cell line. Int. J. Nanomedicine. 7, 1793–1804 (2012).
Zhao, X. et al. Oridonin induces autophagy-mediated cell death in pancreatic cancer by activating the c-Jun N-terminal kinase pathway and inhibiting phosphoinositide 3-kinase signaling. Ann. Trans. Med. 9(13), 1084 (2021).
Li, P. et al. Hypoxia-responsive liposome enhances intracellular delivery of photosensitizer for effective photodynamic therapy. J. Control. Release. 377, 277–287 (2025).
Sharma, G. et al. Revolutionizing Parkinson’s treatment: Harnessing the potential of intranasal nanoemulsions for targeted therapy. Drug. Deliv. Trans. Res. 15(8), 2589–2607 (2025).
Lim, S. H. et al. Nanoparticle-based combinational strategies for overcoming the blood-brain barrier and blood-Tumor barrier. Int. J. Nanomedicine. 19, 2529–2552 (2024).
Li, Y. et al. Nanomaterials based on hollow gold nanospheres for cancer therapy. Regen Biomater. 11, rbae126 (2024).
Shah, T. et al. Computational design to experimental validation: molecular dynamics-assisted development of polycaprolactone micelles for drug delivery. J. Mater. Chem. B. 13(13), 4166–4178 (2025).
El-Saadony, M. T. et al. Chitosan, derivatives, and its nanoparticles: Preparation, physicochemical properties, biological activities, and biomedical applications—a comprehensive review. Int. J. Biol. Macromol. 313, 142832 (2025).
Pashkina, E. et al. Hyaluronic acid-based drug delivery systems for cancer therapy. Cells 14(2), 61 (2025).
Liu, L. et al. Nanobody-based drug delivery systems for cancer therapy. J. Control. Release. 381, 113562 (2025).
van der Koog, L. et al. Liposomes and extracellular vesicles as drug delivery systems: a comparison of composition, pharmacokinetics, and functionalization. Adv. Healthc Mater. 11(5), e2100639 (2022).
Odel, H. A. C. et al. Liposomes and niosomes: new trends and applications in the delivery of bioactive agents for cancer therapy. Int J Pharm. 668, 124994 (2025).
Yu, B. et al. Empowering healthcare with phage display technology. ACS Biomater. Sci. Eng. 11(6), 3228–3248 (2025).
Zhou, C. et al. Serine/threonine/tyrosine kinase 1 drives pancreatic carcinogenesis via GSK3β sequestration-mediated Wnt/β-catenin pathway hyperactivation. Signal Transduct Target Ther. 10(1), 205 (2025).
Zhou, C. et al. B-lymphoid tyrosine kinase-mediated FAM83A phosphorylation elevates pancreatic tumorigenesis through interacting with β-catenin. Signal Transduct Target Ther. 8(1), 66 (2023).
Hu, C. M. et al. Innovative cyclic peptide disrupts IL-17RB-MLK4 interaction for targeted pancreatic cancer therapy. Biomed. Pharmacother. 184, 117892 (2025).
Zhu, X. et al. Targeting pancreatic cancer cells with peptide-functionalized polymeric magnetic nanoparticles. Int. J. Mol. Sci. 20(12), 2988 (2019).
Lu, L. et al. Preparation and characterization of PLGA-based magnetic polymer nanoparticles for targeting pancreatic adenocarcinoma. Curr. Pharm. Des. 29(9), 686–696 (2023).
Valetti, S. et al. Peptide-functionalized nanoparticles for selective targeting of pancreatic tumor. J. Control. Release. 192, 29–39 (2014).
Valetti, S. et al. Peptide conjugation: before or after nanoparticle formation?. Bioconjug Chem. 25(11), 1971–1983 (2014).
Hou, L. et al. Effects of phytosterol butyrate ester on the characteristics of soybean phosphatidylcholine liposomes. J. Oleo Sci. 70(9), 1295–1306 (2021).
Hong, C. et al. One stone four birds: a novel liposomal delivery system multi-functionalized with ginsenoside Rh2 for tumor targeting therapy. Nanomicro Lett. 12(1), 129 (2020).
Sun, X. et al. Improved tumor uptake by optimizing liposome based RES blockade strategy. Theranostics. 7(2), 319–328 (2017).
Papi, M. et al. Clinically approved PEGylated nanoparticles are covered by a protein corona that boosts the uptake by cancer cells. Nanoscale 9(29), 10327–10334 (2017).
Bigdeli, A. et al. Exploring cellular interactions of liposomes using protein corona fingerprints and physicochemical properties. ACS Nano 10(3), 3723–3737 (2016).
Corbo, C. et al. Effects of the protein corona on liposome-liposome and liposome-cell interactions. Int. J. Nanomedicine. 11, 3049–3063 (2016).
Smith, C. et al. Tumor microenvironment in pancreatic ductal adenocarcinoma: Implications in immunotherapy. World J. Gastroenterol. 28(27), 3297–3313 (2022).
Liu, Q. et al. Current research trends of nanomedicines. Acta Pharm. Sin B. 13(11), 4391–4416 (2023).
Fang, J. et al. Exploiting the dynamics of the EPR effect and strategies to improve the therapeutic effects of nanomedicines by using EPR effect enhancers. Adv. Drug. Deliv Rev. 157, 142–160 (2020).
Krishnan, N. et al. Cell membrane-coated nanoparticles for the treatment of cancer. Clin Transl. Med. 13(6), e1285 (2023).
Jain, A. et al. Advances in tumor targeted liposomes. Curr. Mol. Med. 18(1), 44–57 (2018).
Wang, S. et al. Liposomes for tumor targeted therapy: a review. Int. J. Mol. Sci. 24(3), 2643 (2023).
Fathi, S. et al. Liposomal drug delivery systems for targeted cancer therapy: is active targeting the best choice?. Future Med. Chem. 8(17), 2091–2112 (2016).
Belfiore, L. et al. Towards clinical translation of ligand-functionalized liposomes in targeted cancer therapy: Challenges and opportunities. J. Control. Release. 277, 1–13 (2018).
Deodhar, S. et al. Long circulating liposomes: challenges and opportunities. Ther. Deliv. 9(12), 857–872 (2018).
Gao, C. et al. Preparation, characterization, and anti-colon cancer activity of oridonin-loaded long-circulating liposomes. Pharm. Dev. Technol. 26(10), 1073–1078 (2021).
Allen, T. M. Long-circulating (sterically stabilized) liposomes for targeted drug delivery. Trends Pharmacol Sci. 15(7), 215–220 (1994).
Tenzer, S. et al. Rapid formation of plasma protein corona critically affects nanoparticle pathophysiology. Nat. Nanotechnol. 8(10), 772–781 (2013).
Barrán-Berdón, A. L. et al. Time evolution of nanoparticle-protein corona in human plasma: relevance for targeted drug delivery. Langmuir 29(21), 6485–6494 (2013).
Mahmoudi, M. et al. Temperature: the “ignored” factor at the NanoBio interface. ACS Nano 7(8), 6555–6562 (2013).
Funding
The research was supported by grants from the National Natural Science Foundation of China (82360852). Guizhou Province Graduate Student Research Fund Project (QiankeheYJSKYJJ[2021]171). Shaoxing Science and Technology Planning Project (2023A14013). Science and Technology Program of Guizhou Province (Qiankehe Basics ZK [2023] Key 046). Natural Science Research Project of Guizhou Department of Education (Qianjiaoji [2023] 069). High-level Innovative Talents of Guizhou Province (QianKeHe platform talents-GCC [2023] 047). Guizhou Province Innovation Talent Team Construction (Platform Talent-CXTD[2023]020). The State Administration of Traditional Chinese Medicine high-level key discipline construction project (zyyzdxk-2023185). Guizhou Key Laboratory of Modern Traditional Chinese Medicine Creation (Qian Ke He Platform ZSYS [2025] 019).Nano-drug Technology Research Center of Guizhou University of Traditional Chinese Medicine (Guizhongyi ZX Hezi [2024] 070).
Author information
Authors and Affiliations
Contributions
Kunshun Luo: Writing—original draft, Visualization, Conceptualization, Formal Analysis, Visualization, Review and Editing, Funding Acquisition; Fangxia Zhang: Writing-original draft, Visualization, Conceptualization, Formal Analysis, Visualization, Review and Editing; Teng Chen: Formal Analysis; Zhiyong Chen: Conceptualization, Formal Analysis; Jing Yang: Conceptualization; Ying Zhou: Funding Acquisition, Project Administration, Resources; Shaoyan Xuan: Funding Acquisition, Project Administration, Resources; Tingting Feng: Funding Acquisition, Project Administration, Resources; Yue Zhu: Conceptualization, project Administration, Resources, Formal Analysis; Zuhua Wang: Funding Acquisition, Project Administration, Resources, Conceptualization, Review and Editing.
Corresponding authors
Ethics declarations
Competing interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Institutional review board statement
All experimental procedures presented in this manuscript were approved and carried out in accordance with the China Veterinary Animal Care Office Animal Experimental Ethics Committee of Guizhou University of Traditional Chinese Medicine (Grant No.20230022). This study was reported in accordance with ARRIVE guidelines.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhang, F., Luo, K., Xuan, S. et al. CKAAKN peptide-conjugated long-circulating nanoliposomes for the targeted delivery of oridonin to pancreatic cancers. Sci Rep 16, 6065 (2026). https://doi.org/10.1038/s41598-026-36920-5
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-026-36920-5