Abstract
Motion sickness is associated with thermoregulation and metabolic control, but the underlying neural circuitry remains largely unknown. Here we show that neurons in the medial vestibular nuclei parvocellular part (MVePC) mediate the hypothermic responses induced by motion. Reactivation of motion-sensitive MVePC neurons recapitulates motion sickness in mice. We show that motion-activated neurons in the MVePC are glutamatergic (MVePCGlu), and that optogenetic stimulation of MVePCGlu neurons mimics motion-induced hypothermia by signalling to the lateral parabrachial nucleus (LPBN). Acute inhibition of MVePC-LPBN circuitry abrogates motion-induced hypothermia. Finally, we show that chronic inhibition of MVePCGlu neurons prevents diet-induced obesity and improves glucose homeostasis without suppressing food intake. Overall, these findings highlight MVePCGlu neurons as a potential target for motion-sickness treatment and obesity control.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$32.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to the full article PDF.
USD 39.95
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
All data generated or analysed during this study are included in this published article. No third-party materials were included in this paper. Further information and requests for resources and reagents should be directed to and will be fulfilled by Y.X. (yongx@bcm.edu). Source data are provided with this paper.
References
Dalamaga, M., Christodoulatos, G. S., Karampela, I., Vallianou, N. & Apovian, C. M. Understanding the co-epidemic of obesity and COVID-19: current evidence, comparison with previous epidemics, mechanisms, and preventive and therapeutic perspectives. Curr. Obes. Rep. 10, 214–243 (2021).
Löffler, M. C. et al. Challenges in tackling energy expenditure as obesity therapy: from preclinical models to clinical application. Mol. Metab. 51, 101237 (2021).
Tak, Y. J. & Lee, S. Y. Anti-obesity drugs: long-term efficacy and safety: an updated review. World J. Mens Health 39, 208–221 (2021).
Golding, J. F. & Gresty, M. A. Pathophysiology and treatment of motion sickness. Curr. Opin. Neurol. 28, 83–88 (2015).
Golding, J. F. Motion sickness susceptibility. Auton. Neurosci. 129, 67–76 (2006).
Nalivaiko, E., Rudd, J. A. & So, R. H. Motion sickness, nausea and thermoregulation: the “toxic” hypothesis. Temperature 1, 164–171 (2014).
Tu, L. et al. Alpha-9 nicotinic acetylcholine receptors mediate hypothermic responses elicited by provocative motion in mice. Physiol. Behav. 174, 114–119 (2017).
Ngampramuan, S. et al. Thermoregulatory correlates of nausea in rats and musk shrews. Oncotarget 5, 1565–1575 (2014).
Tu, L. et al. Brain activation by H(1) antihistamines challenges conventional view of their mechanism of action in motion sickness: a behavioral, c-Fos and physiological study in Suncus murinus (house musk shrew). Front. Physiol. 8, 412 (2017).
Tu, L. et al. The brain-penetrating, orally bioavailable, ghrelin receptor agonist HM01 ameliorates motion-induced emesis in Suncus murinus (house musk shrew). Br. J. Pharmacol. 177, 1635–1650 (2020).
Hemingway, A. Cold sweating in moiton sickness. Am. J. Physiol. 141, 172–175 (1944).
Ogata, K. & Sasaki, T. On the causes of diurnal body temperature rhythm in man, with reference to observations during voyage. Jpn. J. Physiol. 13, 84–96 (1963).
Nobel, G., Tribukait, A., Mekjavic, I. B. & Eiken, O. Effects of motion sickness on thermoregulatory responses in a thermoneutral air environment. Eur. J. Appl. Physiol. 112, 1717–1723 (2012).
Dutil, M. et al. The impact of obesity on balance control in community-dwelling older women. Age 35, 883–890 (2013).
Hromatka, B. S. et al. Genetic variants associated with motion sickness point to roles for inner ear development, neurological processes and glucose homeostasis. Hum. Mol. Genet. 24, 2700–2708 (2015).
Wang, S. C. & Chinn, H. I. Experimental motion sickness in dogs; importance of labyrinth and vestibular cerebellum. Am. J. Physiol. 185, 617–623 (1956).
Kennedy, R. S., Graybiel, A., McDonough, R. C. & Beckwith, F. D. Symptomatology under storm conditions in the North Atlantic in control subjects and in persons with bilateral labyrinthine defects. Acta Otolaryngol. 66, 533–540 (1968).
Cheung, B. S., Howard, I. P. & Money, K. E. Visually-induced sickness in normal and bilaterally labyrinthine-defective subjects. Aviat. Space Environ. Med. 62, 527–531 (1991).
Ossenkopp, K. P., Rabi, Y. J., Eckel, L. A. & Hargreaves, E. L. Reductions in body temperature and spontaneous activity in rats exposed to horizontal rotation: abolition following chemical labyrinthectomy. Physiol. Behav. 56, 319–324 (1994).
Ueno, S., Matsuki, N. & Saito, H. Suncus murinus as a new experimental model for motion sickness. Life Sci. 43, 413–420 (1988).
Horn, C. C. et al. Why can’t rodents vomit? A comparative behavioral, anatomical, and physiological study. PLoS ONE 8, e60537 (2013).
Horn, C. C., Meyers, K. & Oberlies, N. Musk shrews selectively bred for motion sickness display increased anesthesia-induced vomiting. Physiol. Behav. 124, 129–137 (2014).
Kaji, T., Saito, H., Ueno, S. & Matsuki, N. Comparison of various motion stimuli on motion sickness and acquisition of adaptation in Suncus murinus. Jikken Dobutsu 39, 75–79 (1990).
Tu, L. et al. Insights into acute and delayed cisplatin-induced emesis from a microelectrode array, radiotelemetry and whole-body plethysmography study of Suncus murinus (house musk shrew). Front. Pharmacol. 12, 746053 (2021).
Gordon, C. J. Thermal physiology of laboratory mice: defining thermoneutrality. J. Therm. Biol 37, 654–685 (2012).
Morrison, S. F. & Nakamura, K. Central mechanisms for thermoregulation. Ann. Rev. Physiol. 81, 285–308 (2019).
Tan, C. L. & Knight, Z. A. Regulation of body temperature by the nervous system. Neuron 98, 31–48 (2018).
Park, A. H. & Hu, S. Gender differences in motion sickness history and susceptibility to optokinetic rotation-induced motion sickness. Aviat. Space Environ. Med. 70, 1077–1080 (1999).
Zhou, W. et al. Sex and age differences in motion sickness in rats: the correlation with blood hormone responses and neuronal activation in the vestibular and autonomic nuclei. Front. Aging Neurosci. 9, 29 (2017).
Matsuki, N. et al. Male/female differences in drug-induced emesis and motion sickness in Suncus murinus. Pharmacol. Biochem. Behav. 57, 721–725 (1997).
Spinks, A. & Wasiak, J. Scopolamine (hyoscine) for preventing and treating motion sickness. Cochrane Database Syst. Rev. 2011, Cd002851 (2011).
Qi, R. et al. Anti-cholinergics mecamylamine and scopolamine alleviate motion sickness-induced gastrointestinal symptoms through both peripheral and central actions. Neuropharmacology 146, 252–263 (2019).
Cluny, N. L., Naylor, R. J., Whittle, B. A. & Javid, F. A. The effects of cannabidiol and tetrahydrocannabinol on motion-induced emesis in Suncus murinus. Basic Clin. Pharmacol. Toxicol. 103, 150–156 (2008).
Gregory, E. L. Thermoregulatory aspects of adipose tissue. Clin. Dermatol. 7, 78–92 (1989).
DeNardo, L. A. et al. Temporal evolution of cortical ensembles promoting remote memory retrieval. Nat. Neurosci. 22, 460–469 (2019).
Abe, C. et al. VGLUT2-expressing neurons in the vestibular nuclear complex mediate gravitational stress-induced hypothermia in mice. Commun. Biol. 3, 227 (2020).
Madden, C. J. & Morrison, S. F. Neurons in the paraventricular nucleus of the hypothalamus inhibit sympathetic outflow to brown adipose tissue. Am. J. Physiol. 296, R831–843 (2009).
Fukushima, A., Kataoka, N. & Nakamura, K. An oxytocinergic neural pathway that stimulates thermogenic and cardiac sympathetic outflow. Cell Rep. 40, 111380 (2022).
Nakamura, K. & Morrison, S. F. A thermosensory pathway that controls body temperature. Nat. Neurosci. 11, 62–71 (2008).
Nakamura, K. & Morrison, S. F. A thermosensory pathway mediating heat-defense responses. Proc. Natl Acad. Sci. USA 107, 8848–8853 (2010).
Idoux, E., Tagliabue, M. & Beraneck, M. No gain no pain: relations between vestibulo-ocular reflexes and motion sickness in mice. Front. Neurol. 9, 918 (2018).
López, M. Hypothalamic AMPK as a possible target for energy balance-related diseases. Trends Pharmacol. Sci. 43, 546–556 (2022).
Kashio, M. & Tominaga, M. TRP channels in thermosensation. Curr. Opin. Neurobiol. 75, 102591 (2022).
Lamas, J. A., Rueda-Ruzafa, L. & Herrera-Pérez, S. Ion channels and thermosensitivity: TRP, TREK, or both? Int. J. Mol. Sci. 20, 4302 (2019).
Bender, F. L. et al. The temperature-sensitive ion channel TRPV2 is endogenously expressed and functional in the primary sensory cell line F-11. Cell. Physiol. Biochem. 15, 183–194 (2005).
Togashi, K. et al. TRPM2 activation by cyclic ADP-ribose at body temperature is involved in insulin secretion. EMBO J. 25, 1804–1815 (2006).
Vriens, J. et al. TRPM3 is a nociceptor channel involved in the detection of noxious heat. Neuron 70, 482–494 (2011).
Lee, J. H. et al. Global and local fMRI signals driven by neurons defined optogenetically by type and wiring. Nature 465, 788–792 (2010).
Petreanu, L., Huber, D., Sobczyk, A. & Svoboda, K. Channelrhodopsin-2-assisted circuit mapping of long-range callosal projections. Nat. Neurosci. 10, 663–668 (2007).
Cano, G. et al. Anatomical substrates for the central control of sympathetic outflow to interscapular adipose tissue during cold exposure. J. Comp. Neurol. 460, 303–326 (2003).
Yoshida, K. et al. Neurons of the rat preoptic area and the raphe pallidus nucleus innervating the brown adipose tissue express the prostaglandin E receptor subtype EP3. Eur. J. Neurosci. 18, 1848–1860 (2003).
Schmäl, F. Neuronal mechanisms and the treatment of motion sickness. Pharmacology 91, 229–241 (2013).
Gavgani, A. M., Nesbitt, K. V., Blackmore, K. L. & Nalivaiko, E. Profiling subjective symptoms and autonomic changes associated with cybersickness. Auton. Neurosci. 203, 41–50 (2017).
Mazloumi Gavgani, A., Walker, F. R., Hodgson, D. M. & Nalivaiko, E. A comparative study of cybersickness during exposure to virtual reality and “classic” motion sickness: are they different? J. Appl. Physiol. 125, 1670–1680 (2018).
Crampton, G. H. Motion and Space Sickness (CRC Press, 1990).
Andrews, P. L. & Rudd, J. A. in Management of Chemotherapy-Induced Nausea and Vomiting: New Agents and New Uses of Current Agents 5–44 (Adis Cham, 2016).
Zhang, Z. H. et al. A new vestibular stimulation mode for motion sickness with emphatic analysis of pica. Front. Behav. Neurosci. 16, 882695 (2022).
Koslucher, F., Haaland, E., Malsch, A., Webeler, J. & Stoffregen, T. A. Sex differences in the incidence of motion sickness induced by linear visual oscillation. Aerosp. Med. Hum. Perform 86, 787–793 (2015).
Graeber, D. A. & Stanney, K. M. Gender differences in visually induced motion sickness. Proc. Hum. Factors Ergon. Soc. Annu. Meet. 46, 2109–2113 (2002).
Javid, F. A. & Naylor, R. J. Variables of movement amplitude and frequency in the development of motion sickness in Suncus murinus. Pharmacol. Biochem. Behav. 64, 115–122 (1999).
Lidell, M. E., Betz, M. J. & Enerbäck, S. Brown adipose tissue and its therapeutic potential. J. Intern. Med. 276, 364–377 (2014).
Del Vecchio, F., Nalivaiko, E., Cerri, M., Luppi, M. & Amici, R. Provocative motion causes fall in brain temperature and affects sleep in rats. Exp. Brain Res. 232, 2591–2599 (2014).
Machuca-Márquez, P. et al. Vestibular CCK signaling drives motion sickness-like behavior in mice. Proc. Natl Acad. Sci. USA 120, e2304933120 (2023).
Abe, C., Tanaka, K., Iwata, C. & Morita, H. Vestibular-mediated increase in central serotonin plays an important role in hypergravity-induced hypophagia in rats. J. Appl. Physiol. 109, 1635–1643 (2010).
Golding, J. F., Wesnes, K. A. & Leaker, B. R. The effects of the selective muscarinic M3 receptor antagonist darifenacin, and of hyoscine (scopolamine), on motion sickness, skin conductance & cognitive function. Br. J. Clin. Pharmacol. 84, 1535–1543 (2018).
Allen, W. E. et al. Thirst-associated preoptic neurons encode an aversive motivational drive. Science 357, 1149–1155 (2017).
Ye, H. et al. An estrogen-sensitive hypothalamus-midbrain neural circuit controls thermogenesis and physical activity. Sci. Adv. 8, eabk0185 (2022).
Haery, L. et al. Adeno-associated virus technologies and methods for targeted neuronal manipulation. Front. Neuroanat. 13, 93 (2019).
Yang, Y. et al. Hypothalamic steroid receptor coactivator-2 regulates adaptations to fasting and overnutrition. Cell Rep. 37, 110075 (2021).
Xue, M., Atallah, B. V. & Scanziani, M. Equalizing excitation-inhibition ratios across visual cortical neurons. Nature 511, 596–600 (2014).
Mina, A. I. et al. CalR: a web-based analysis tool for indirect calorimetry experiments. Cell Metab. 28, 656–666 (2018).
Müller, T. D., Klingenspor, M. & Tschöp, M. H. Revisiting energy expenditure: how to correct mouse metabolic rate for body mass. Nat. Metab. 3, 1134–1136 (2021).
Zhang, C. et al. Area postrema cell typeÿs that mediate nausea-associated behaviors. Neuron 109, 461–472 (2021).
Tu, L. et al. Anoctamin 4 channel currents activate glucose-inhibited neurons in the mouse ventromedial hypothalamus during hypoglycemia. J. Clin. Invest. 133, e163391 (2023).
Acknowledgements
The investigators are supported by grants from the NIH (P01DK113954, R01DK115761, R01DK117281, R01DK125480 and R01DK120858 to Y.X.; R01DK104901 and R01DK12665 to M.F.; R01MH117089 to M.X.); USDA/CRIS (51000-064-01S to Y.X.; 51000-064-02S to M.F.; 3092-51000-062-04(B)S to C.W.; 1F32DK13868501A1 to X.F.); the McKnight Foundation to M.X.; and an American Heart Association Postdoctoral Fellowship (2020AHA000POST000204188 to L.T.). The funders had no role in study design, data collection and analysis, decision to publish or preparation of the paper.
Author information
Authors and Affiliations
Contributions
L.T. was involved in experimental design and most procedures, data acquisition and analyses and writing the paper. X.F. conducted electrophysiological experiments and data analysis. Y.Y., M.Y., Hailan Liu, Hesong Liu, N.Y., J.C.B., K.M.C., M.W., Y.L., O.Z.G., Q.L., Y.S., J.H., Y.Z., M.F., Q.T., B.A., M.X., Y.H. and C.W. contributed to the generation of study mice and data analysis. Y.X. is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Metabolism thanks the anonymous reviewers for their contribution to the peer review of this work. Primary Handling Editors: Jean Nakhle and Ashley Castellanos-Jankiewicz, in collaboration with the Nature Metabolism team.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Motion elicits c-fos expression in the brain.
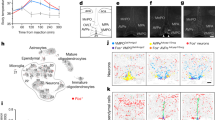
(a, b) Representative photomicrographs illustrating c-fos immunostaining in NTS, RPa, LC, CeA, αBNST and MPA from 8 for male/sham (a), 9 for male/motion (a), 7 for female/sham (b) and 8 for female/motion (b) mice. (c) Quantification of c-fos cells in NTS, RPa, LC, CeA, αBNST and MPA elicited by motion. n = 8 for male/sham, 9 for male/motion, 7 for female/sham and 8 for female/motion, two-sided student t test within the same sex. Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 1).
Extended Data Fig. 2 Validation of the mouse motion sickness model with the anti-motion sickness drug scopolamine.
(a) Effect of scopolamine on food intake in the presence or absence of motion. n = 6 mice, two-way ANOVA followed by Bonferroni post hoc test. (b–e) Effect of scopolamine on distance traveled (b), velocity (c), central zone duration (d) and representative heat-maps (e) in an open field test in the presence or absence of motion. n = 6 mice, one-way ANOVA followed by Bonferroni post hoc test. Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 1).
Extended Data Fig. 3 Validation of ‘TRAP’ed motion-specific neurons via c-fos immunostaining.
(a) Schematic timeline of TRAP protocol coupled with c-fos immnuostaining. (b) In the left panel, tdTomato-labeled neurons refer to ‘TRAP’ed motion-specific neurons, and c-fos positive cells indicate neurons were activated after mice being subjected to a second-round of motion. Percentage of colocalization between tdTomato-labeled neurons and c-fos positive cells in each specific brain region was shown in the right panel. n = 3 mice. Data are expressed as mean ± standard errors of the mean. Arrows point to co-localized cells between tdTomato and c-fos positive cells. (Relative to Fig. 2).
Extended Data Fig. 4 Re-activation of motion-specific PVH neurons.
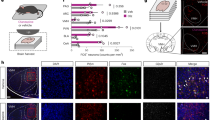
(a–d) Re-activation of motion-specific PVH neurons did not affect body temperature (a-b) or locomotor activity (c-d). n = 6 for control, and n = 7 for TRAP mice. (e–g) Re-activation of motion-specific PVH neurons inhibited food intake in fasting mice (e), but did not affect preferred ambient temperature (f-g). n = 6 for control, and n = 7 for TRAP mice, two-way ANOVA followed by Bonferroni post hoc test for (e). (h–k) Distance traveled (h), velocity (i), central zone duration (j), and representative heat-maps (k) in an open field test after motion-specific PVH neurons were re-activated via CNO injection. n = 6 for control, and n = 7 for TRAP mice. (l, m) Expression of hM3Dq-mCherry in the PVH that was validated by c-fos immunostaining after CNO injection, and quantification of c-fos cells (m). n = 6 for control, and n = 7 for TRAP mice, two-sided student t text for (m). Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 2).
Extended Data Fig. 5 Re-activation of motion-specific LPBN neurons.
(a–d) Re-activation of motion-specific LPBN neurons slightly decreased body temperature (a-b), but did not influence locomotor activity (c-d). n = 6 mice, one-way ANOVA followed by Bonferroni post hoc test for (b). (e–g) Re-activation of motion-specific LPBN neurons inhibited food intake in fasting mice (e), but did not affect preferred ambient temperature (f-g). n = 6 mice, two-way ANOVA followed by Bonferroni post hoc test for (e). (h–k) Distance traveled (h), velocity (i), central zone duration (j), and representative heat-maps (k) in an open field test after motion-specific LPBN neurons were re-activated via CNO injection. n = 6 mice, one-way ANOVA followed by Bonferroni post hoc test for (h) and (i). (l, m) Expression of hM3Dq-mCherry in the LPBN that was validated by c-fos immunostaining after CNO injection, and quantification of c-fos cells (m). n = 6 mice, two-sided student t text for (m). Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 2).
Extended Data Fig. 6 Effect of scopolamine on electrical responses of motion-specific MVePC neurons.
(a–d) Experimental illustration of a recorded motion-specific MVePC neuron that was labeled by hM3Dq-mCherry (a), scopolamine attenuated CNO-induced increase in firing frequency and membrane potential (b-c), and raw traces of a recorded hM3Dq-mCherry-expressing neuron among different treatments (d). n = 8 neurons from 2 mice, two-tail paired t test for (b) and (c). (e–g) After washout of scopolamine, CNO induced increase in firing frequency and membrane potential of hM3Dq-mCherry-expressing neurons (e-f), and raw traces of a recorded hM3Dq-mCherry-expressing neuron in response to CNO after scopolamine washout (g). n = 6 neurons from 2 mice, two-tail paired t test for (e) and (f). (h, i) Representative photomicrographs illustrating c-fos immunostaining and number of c-fos cells in the MVePC following scopolamine treatment against motion in female mice. n = 6 mice in each group, one-way ANOVA followed by Bonferroni post hoc test. Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 2).
Extended Data Fig. 7 Electrical responses of MVePC neurons exposed to different ambient temperatures.
(a) Experimental illustration of a recorded non-motion-specific MVePC neuron from 2 female TRAP2/Rosa26-LSL-tdTomato mice. (b–d) Firing frequency and membrane potential of non-motion-specific MVePC neurons during different ambient recording temperatures (b-c), and representative raw traces of one recorded non-motion-specific MVePC neuron (d). n = 7 neurons from 2 mice. (e, f) Membrane potential of motion-specific MVePC neurons during different ambient recording temperatures in the presence of a cocktail of synaptic blockers (TTX, CNQX, D-AP5 and bicuculline), and representative raw trace of one recorded neuron in this condition. n = 13 neurons from 2 mice. One-way ANOVA followed by Bonferroni tests for (e). (g, h) Membrane potential of non-motion-specific MVePC neurons during different ambient recording temperatures in the presence of a cocktail blockers of synaptic blockers (TTX, CNQX, D-AP5 and bicuculline), and representative raw trace of one recorded neuron in this condition. n = 6 neurons from 2 mice. Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 2).
Extended Data Fig. 8 Compound C abolishes excitation of MVePC neurons elicited by high ambient temperature.
(a, b) Firing frequency and membrane potential of motion-specific MVePC neurons exposed to different ambient temperatures in the presence of compound C (10 µM). n = 8 neurons from 2 mice. (c) Representative raw traces of one recorded neuron. Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 2).
Extended Data Fig. 9 Validation of hChR2 expression and real-time place preference test.
(a–d) Representative image showing fiber position and hChR2 (H134R)-EFYP expression in the MVePCGlu neurons (a), and time spent, velocity and distance travelled in each respective chamber that was coupled with MVePCGlu stimulation during the real-time place preference test (b-d). n = 7 mice, two-tail paired t test for (b). (e–h) Representative image showing fiber position and hChR2 (H134R)-EFYP expression in the MVePCVgat neurons (e), and time spent, velocity and distance travelled in each respective chamber that was coupled with MVePCVgat stimulation during the real-time place preference test (f-h). n = 7 mice, two-tail paired t test. (i–l) Representative image showing fiber position and terminals of hChR2 (H134R)-EFYP expression in the LPBN (i), and time spent, velocity and distance travelled in each respective chamber that was coupled with stimulation of terminals of MVePCGlu in the LPBN during the real-time place preference test (j-l). n = 6 mice, two-tail paired t test for (j). Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 3).
Extended Data Fig. 10 MVePCGlu neurons modulates BAT thermogenesis in female mice.
(a, b) Motion decreased BAT temperature in female mice. n = 6 mice, two-way ANOVA followed by Bonferroni tests for (a), and two-sided student t test for (b). (c, d) Experimental illustration of PRV-mediated retrograde polysynaptic tracing in BAT (c), and representative images showing RFP+ neurons in MVePC, RPa, PVH, but not LPBN (d) from 3 mice. (e–g) Activation of MVePCGlu neurons via blue light delivery decreased BAT temperature. n = 6 mice, two-way ANOVA followed by Bonferroni tests for (e), and two-tail paired t test for (g). (h–j) Inhibition of MVePCGlu neurons via CNO injection increased BAT temperature. n = 6 mice, two-way ANOVA followed by Bonferroni tests for (i), and student t test for (j). Data are expressed as mean ± standard errors of the mean. (Relative to Fig. 4).
Supplementary information
Supplementary Information (download PDF )
Supplementary Figs. 1–4 and Table 1.
Source data
Source Data Fig. 1 (download XLSX )
Statistical source data.
Source Data Fig. 2 (download XLSX )
Statistical source data.
Source Data Fig. 3 (download XLSX )
Statistical source data.
Source Data Fig. 4 (download XLSX )
Statistical source data.
Source Data Fig. 5 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 1 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 2 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 3 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 4 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 5 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 6 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 7 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 8 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 9 (download XLSX )
Statistical source data.
Source Data Extended Data Fig. 10 (download XLSX )
Statistical source data.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tu, L., Fang, X., Yang, Y. et al. Vestibular neurons link motion sickness, behavioural thermoregulation and metabolic balance in mice. Nat Metab 7, 742–758 (2025). https://doi.org/10.1038/s42255-025-01234-9
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s42255-025-01234-9