Abstract
During the recent yellow fever (YF) epidemics in Brazil, human cases were attributed to spillover infections via sylvatic mosquito transmission. Despite YF virus (YFV) transmission in major urban centers with insufficient vaccination coverage and abundant populations of the domestic vector, Aedes aegypti, there was no evidence of human-amplified transmission. Furthermore, the historic absence of YF in Asia, despite abundant Ae. aegypti and an immunologically naive human population, is unexplained. We tested the hypothesis that pre-existing, heterologous flavivirus immunity, specifically from dengue (DENV) and Zika (ZIKV) viruses, limits YFV viremia and transmission by Ae. aegypti. We infected cynomolgus macaques with DENV or ZIKV, then challenged them 6–9 months later with YFV. We then measured viremia and disease and allowed Ae. aegypti mosquitoes to feed during peak macaque viremia. Although prior heterologous immunity had variable effects on disease, DENV and ZIKV immunity consistently suppressed YFV viremia. Despite no statistical difference due to a small sample size, the suppression in viremia led to a significant reduction in Ae. aegypti infection and a lack of transmission potential. These results support the hypothesis that, in DENV- and ZIKV-endemic regions such as South America and Asia, human flavivirus immunity suppresses YFV human amplification potential, reducing the risk of urban outbreaks.
Similar content being viewed by others
Introduction
The conspicuous absence of yellow fever (YF) in highly vulnerable regions of Asia has been an enigma for over a century1. YF, a mosquito-borne disease, caused by yellow fever virus (YFV) (Flaviviridae, Orthoflavivirus) has a case-fatality rate of 20–50% in severely infected individuals2. While a live-attenuated YFV vaccine (17D and subtypes)3 confers long-term protection, there are certain limitations and concerns associated with it. In 2001, YF vaccine-associated viscerotropic disease (YEL-AVD) was reported questioning the safety of the vaccine, particularly during widespread vaccinations in the absence of outbreaks. Additionally, due to manufacturing limitations, there is a general lack of a vaccination program for YFV at a global level and major shortages have occurred in the face of outbreaks, together raising concerns regarding the ability to control future epidemics4.
YFV primarily circulates in two ecologically and evolutionarily distinct transmission cycles5. In the urban or epidemic cycle, the virus is transmitted between human amplification hosts by the principal mosquito vector, Aedes (Stegomyia) aegypti. This cycle was responsible for a recent, major epidemic in Angola6, which subsequently spread to the Democratic Republic of Congo7. In the sylvatic or enzootic/epizootic cycle, the virus is transmitted among non-human primates (NHPs) by sylvatic mosquitoes, including Haemogogus spp. and Sabethes spp. in South America and forest-dwelling Aedes spp. in Africa8,9. In the zone of emergence, the virus can spill over from enzootic vectors to both NHPs and humans as hosts, typically in rural areas bordering forests. Epizootics of YF among NHPs occur both in Africa and the Neotropics, and in Uganda, the same region has experienced both YF and Zika outbreaks10. Increased human activity and encroachment in these regions with high densities of enzootic vectors can result in epidemics, as occurred in Brazil from 2016–20198. Despite being the largest sylvatic outbreak there since 194211, and a current abundance of the urban vector Ae. aegypti (it was absent from Brazil from the 1950s to the 1970s during an eradication campaign)12, there were no reports of the establishment of a human-amplified urban transmission cycle8. Although vaccination coverage varies across Brazil13, YFV infections during this outbreak occurred in areas outside the recommended regions, where low herd immunity provided an ideal opportunity for Ae. aegypti-borne transmission. Thus, the failure to establish an urban cycle in Brazil (since 1942) and the complete historic lack of YF in Asia despite completely naïve populations and abundant vectors remains a mystery1.
Several theories have been proposed to explain the lack of YF in Asia1: 1) The paucity of introductions from Africa. This seems unlikely because chikungunya (CHIKV) and Zika (ZIKV) viruses, which also originated in sub-Saharan Africa and are transmitted by Aedes spp. mosquitoes have long histories of spread to Asia and the establishment of urban transmission there14. Furthermore, the well-documented introduction of YFV from workers traveling from Angola to China in 2016 failed to result in autochthonous transmission1,15. 2) Asian and South American Ae. aegypti strains are less competent vectors compared to African strains. However, laboratory experiments addressing this theory showed that Ae. aegypti populations from various Asian and South American countries are capable of YFV infection and transmission16,17,18. 3) Another theory suggests that pre-existing immunity from related flaviviruses, particularly dengue virus (DENV) and high seroprevalence in Asia could act as an immune barrier to prevent the establishment of a human-amplified YFV transmission cycle19,20. Supporting this hypothesis, a previous study showed that dengue-immune monkeys exhibit lower viremia in response to experimental South American and African YFV infection, compared to dengue-naïve animals19. Other studies in rhesus macaques and vervet monkeys suggest a partial protective role of previous flavivirus immunity on YFV infection, particularly in reducing viremia21. However, the possible effect of flavivirus immunity on prevention of epidemic transmission by Ae. aegypti was not addressed.
In addition to longstanding DENV circulation in South America and Asia, ZIKV recently caused a major epidemic in the Americas from 2014 to 2016, infecting over 50% of most neotropical human populations22. The peak of this ZIKV outbreak preceded the 2016 YF epidemic, raising the question of whether preexisting ZIKV immunity may also have influenced YFV infection dynamics by reducing viremia, which could reduce interhuman mosquito transmission as well as YF disease progression. Since ZIKV has been endemic to Asia for many decades23, its immunity could also have reduced the risk of YF there.
We tested the hypothesis that heterologous flavivirus immunity, specifically in response to DENV and ZIKV infection, modulates YFV infection of humans, reducing viremia and mosquito infection, thereby rendering people less competent as amplification hosts to initiate and sustain urban transmission. We used an NHP model with heterologous flavivirus immunity by assessing viremia, markers of YF disease, and infection of Ae. aegypti during periods of peak viremia. Our findings, based on a cohort of NHPs with distinct flavivirus immunity profiles, revealed that prior immunity to DENV and ZIKV generally reduces YFV viremia, as well as mosquito infection and subsequent transmission potential. Heterologous immunity also reduces the elevation of liver transaminases in most animals, suggesting protection against hepatic disease.
Results
Dengue virus type-2 (DENV-2) and ZIKV-immune non-human primates (NHPs) have modulated YFV viremia
We examined the effect of pre-existing DENV-2 and ZIKV immunity on YFV infection of cynomolgus macaques (Fig. 1a). The initial infections were described in a previous study to be published independently24; 23 animals were exposed to Ae. albopictus mosquitoes sham-infected with PBS (n = 3) or infected with one of the four virus strains: DENV-2 P8-1407 (n = 10) or ZIKV DakAr 41525 (n = 3) that represent sylvatic strains, DENV-2 NGC (n = 3) or ZIKV PRVABC59 (n = 4) that represent human endemic/epidemic strains. In our study, 6-9 months after primary exposure, all animals were challenged with a Brazilian YFV strain (YFV_BR_MG-2017NHP15, hereafter referred as YFV BR17) isolated in 2017, during the major YF epidemic. Prior to the YFV challenge, sera were assayed by foci-reduction neutralization test (FRNT) for antibodies against all three homologous and heterologous viruses. Flavivirus-naïve (sham-infected with uninfected mosquitoes) animals were seronegative for all four serotypes of DENV, as well as ZIKV, and YFV (Fig. 1b, c and Supplementary Table 1). Of the 10 DENV-2 P8-1407-exposed animals, eight had detectable neutralizing antibodies against DENV-2, whereas two animals were seronegative by FRNT (Fig. 1b). All animals exposed to DENV-2 NGC and ZIKV DakAr 41525 had detectable neutralizing antibodies against homologous viruses (Fig. 1b, c). One of the four animals exposed to ZIKV PRVABC59-infected mosquitoes also did not seroconvert by FRNT (Fig. 1c).
a Experimental design in cynomolgus macaques (Created in BioRender. Mirchandani, D. (2023) BioRender.com/t61o691). b Neutralizing antibody titer (FRNT50) against DENV-2 in flavivirus-naïve and DENV-2-exposed animals, prior to YFV challenge. c Neutralizing antibody titer against ZIKV in flavivirus-naïve and ZIKV-exposed animals. Animals with homologous FRNT50 titers below the limit of detection (1:20) were reclassified as seronegative (SN). YFV viremia levels in flavivirus-naïve and DENV-2-exposed (d) and ZIKV-exposed (e) animals from 2–5 DPI. Viremia levels were measured by focus-forming assays. Log10 transformed viremia values were analyzed for the flavivirus-naïve i.e., control group (n = 3), DENV-2 P8-immune (n = 8), DENV-2 NGC-immune (n = 3), DENV-2 SN (n = 2), ZIKV PR-immune (n = 3), and ZIKV DakAr-immune (n = 3) groups by two-way ANOVA with Tukey’s multiple comparison test, each group was compared against the other. A significant difference in DENV-2 P8-immune and DENV-SN groups was observed at 2 (p = 0.0039), 3 (p = 0.0203), and 4 (p = 0.0398) DPI. Data presented as mean values ± SD. Statistical significance (*) color is attributed to the significant difference between that group compared to the flavivirus-naïve group. Reported p-values are based on the results of the respective post-hoc tests. *p < 0.05, **p < 0.01. Source data are provided as a Source Data file.
Upon subcutaneous YFV infection with a dose of 104 focus-forming units (FFU), DENV-2- and ZIKV-immune animals with neutralizing antibodies detectable by FRNT had lower levels and shorter duration of YFV viremia compared to flavivirus-naïve animals (Fig. 1d, e and Supplementary Table 2, 3). We also compared the flavivirus-immune animals evaluated together (DENV and ZIKV groups) with flavivirus-naïve animals and did not find a significant difference in viremia levels (Supplementary Fig. 1). The DENV-seronegative animals (bitten by infected mosquitoes but without seroconversion as measured by FRNT) had comparable viremia levels to flavivirus-naïve animals. However, the ZIKV-seronegative animal (NHP ID: FR1565, exposed to the bite of a ZIKV-infected mosquito but FRNT-negative) had higher and longer viremia compared to the flavivirus-naïve animals (Fig. 1e). Surprisingly, unlike any other YFV-infected animal, FR1565 was laterally recumbent and had to be euthanized by day 9 post-challenge. No visible signs of illness were observed in any other of the infected animals. Since YFV infection in humans and primates present variability in pathogenesis ranging from mild to severe, we expected that our low passage, contemporary YFV strain, not highly adapted to cell culture or animal hosts, would mimic natural variation in outcomes. This was indeed seen in our data, as one of the naïve animals had a relatively mild infection and low viremia compared to the other two animals.
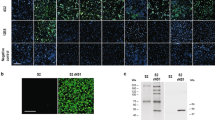
To investigate further if initial infections from mosquito feeding occurred with FRNT-seronegative animals, we performed ELISA to detect binding but non-neutralizing antibodies. Interestingly, both of the DENV-2 P8-1407-seronegative and the one ZIKV-seronegative animal (FR1565) had low levels of IgG antibodies by ELISA, suggesting that infection did occur despite the lack of homologous neutralizing antibody induction.
Mosquitoes fed on YFV-viremic NHPs with previous DENV and ZIKV immunity are refractory to YFV infection
The gold standard measure of human amplification competence is the ability of viremic people to infect Ae. aegypti, leading to efficient epidemic transmission. To mimic natural infection, we allowed naïve female Ae. aegypti mosquitoes, derived from a colony originating from collections in Salvador, Brazil, to feed on infected animals 1–5 days post-YFV infection; 100 mosquitoes were exposed to each animal per day. Fully engorged mosquitoes were then incubated under conditions simulating the tropics (28 °C, 75% relative humidity) for 14 days. Mosquito bodies, legs, and saliva were collected to represent the infection, disseminated infection, and transmission potential, respectively. Most mosquitoes (bodies) that fed on flavivirus-naïve animals had high rates of YFV infection on peak viremia days 3 (Fig. 2a) and 4 (Fig. 2b) post-infection. In contrast, most mosquitoes that fed on DENV- and ZIKV-immune animals were refractory to infection (Supplementary Table 4). Infection rates of mosquitoes that fed on flavivirus-naïve animals were significantly higher than those of mosquitoes that fed on DENV-2 NGC-, DENV-2 P8-1407-, ZIKV PRVABC-, and ZIKV DakAr 41525-immune animals (p < 0.0001; Supplementary Table 5). Significant differences were not observed between mosquitoes (bodies) that fed on flavivirus-naïve animals and DENV-2 seronegative animals at 3 days post-infection (DPI) (p = 0.2678), and the ZIKV seronegative animal at 4 DPI (p = 0.3132). Viral titers in mosquito bodies were variable (Fig. 2c, d) but differed significantly between the groups that fed on flavivirus-naïve and -immune NHPs, the former being higher (p < 0.0001). Dissemination from the digestive tract (YFV-positive legs) was observed primarily in the flavivirus-naïve and -seronegative groups (Supplementary Table 4) and transmission potential (YFV-positive saliva) was observed only for a mosquito that fed on a flavivirus-naïve animal.
Mosquitoes fed on infected NHPs were allowed to incubate for 14 days at 28 °C and 75% humidity. Mosquito infection rate (number of mosquito bodies infected/total number of engorged mosquitoes) is shown for mosquitoes fed on NHPs at day 3 (a) and day 4 (b) post-YFV infection. Each bar represents a cohort of mosquitoes fed on individual NHPs at respective time points. Values on top of each bar represent the number of mosquitoes tested positive/ total number of mosquitoes engorged. Log10 transformed viral titers in individual mosquito bodies at day 3 (c) and day 4 (d) post-YFV infection. Mosquito infectivity and viral titers have been shown for each animal since there is a variation in viremia levels despite a similar immune status. For statistical analyzes, the data for each group was combined and compared with the outcomes for the flavivirus-naïve group by two-tailed Fisher’s exact test. Similarly, viral titers have been shown for group of mosquitoes that fed on individual NHPs. For statistical analyzes, data from each group was combined and Log10 transformed values were analyzed by one-way ANOVA with Dunnett’s multiple comparison test. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001. The following significant difference compared to flavivirus-naïve (n = 3) group was observed: DENV-2 SN (n = 2) p = 0.2678 and ZIKV SN (n = 1) p = 0.0132 at 3 DPI, and DENV-2 SN (n = 2) p = 0.0026 and ZIKV SN (n = 1) p = 0.3132 at 4DPI. Source data are provided as a Source Data file.
Flavivirus-naïve animal NV 259, although YF-viremic, exhibited relatively low (4.19 log10 FFU/mL) viremia levels compared to the other two flavivirus-naïve animals (Supplementary Table 2). Based on the OID50 curve (Fig. 3), it appears that a viral titer of 5.7 log10 FFU/mL in flavivirus-naïve animals is required to infect 50% of mosquitoes and the infection rate drops to negligible levels with viremia below 4 log10 FFU/mL. This may explain the low infection rates among Ae. aegypti exposed to animal NV 259.
Mosquito infectivity (%) was analyzed against NHP viremia for flavivirus-naïve and DENV-immune groups and curve-fitting using non-linear regression. Despite higher viremia at certain timepoints, most mosquitoes that fed on DENV-immune animals were resistant to infection. Source data are provided as a Source Data file.
Upon comparing the mosquito infectivity with NHP viremia for flavivirus-naïve and DENV-2-immune groups, we observed that the infectivity for mosquitoes that fed on a DENV-2-immune animal (BC838) was lower with 3.7% and 6.5% infection at 3 and 4 DPI with viremia levels of 5.3 and 5.6 log10 FFU/mL respectively. In comparison, flavivirus-naïve animal with similar YFV viremia levels (5.3 Log10 FFU/ml) had 33.33% infection rate (Fig. 3). This suggested that another factor in the blood of the DENV-2-immune macaques affected infection rates. One possibility is that antibodies against the flaviviral NS1 protein, which is known to enhance infection of the mosquito midgut25, reduced YFV infection. To assess this hypothesis, we tested the ability of NS1 antibodies generated in response to DENV and ZIKV infection to react with the YFV NS1. As shown in Supplementary Fig. 2, these cross-reactions, although lower in magnitude than the homologous reactions in ELISA, were significantly above the levels of binding exhibited by naïve or seronegative sera. Since all ZIKV-immune animals had suppressed YFV viremia and an intuitively corresponding lower mosquito infection rate, we did not present the data in the OID50 graph.
Heterologous immunity has mild effect on clinical features following yellow fever virus infection
Upon inoculation with YFV, all animals were observed daily for signs of illness. Temperatures were recorded via implanted loggers at 15 min intervals. Additionally, weights and rectal temperatures were recorded from 1–5 and on 14 DPI and compared with baseline levels. No significant changes in weight (Fig. 4a,b) or rectal temperatures (Fig. 4c,d) were detected among the experimental groups. Blood was collected at the previously mentioned time points and tested for complete blood count (CBC) and serum chemistries. Most animals exhibited generalized leukopenia (22/23 animals) with specific populations of cells such as lymphocytes (23/23), neutrophils (22/23), and eosinophils (23/23) reduced from 2 to 5 DPI, compared to the baseline levels; leukopenia recovered by day 14 (Supplementary Figs. 3,4). As a correlate of liver damage, the enzymes alanine transaminase (ALT) and aspartate aminotransferase (AST) were measured, and high elevations were observed in flavivirus-naïve animals up to day 14. In contrast, most DENV-2- (10/11) (Fig. 4e, g) and ZIKV-immune (6/6) (Fig. 4f, h) animals had elevated liver enzymes that resolved by day 14, when the levels for DENV-2 seronegative animals also resolved. The flavivirus-immune animals showed no significant changes in levels of alkaline phosphatase (ALP), creatine (CRE), blood urea nitrogen (BUN), or total bilirubin (TBIL) compared to flavivirus-naïve animals (Supplementary Figs. 5, 6) up to day 5. After YFV infection, ZIKV-FRNT-negative but ELISA-positive animal FR1565 had a highly elevated neutrophil count, BUN, CRE, TBIL (Supplementary Figs. 4, 6), and liver enzymes (ALP, ALT, and AST) (Fig. 4f, h) on the day of euthanasia. Consistent with human cohort studies showing that high viral load, neutrophils, elevated liver enzymes, and bilirubin are associated with fatal YF26, animal FR1565 exhibited all the signs of fulminant fatal YF.
Animal weights (a, b), rectal temperatures (c, d), serum alanine transaminase (ALT) (e, f), and serum aspartate aminotransferase (AST) (g, h) were measured from 1–5 and on 14 DPI and compared to baseline (day 0) values. Data were analyzed by two-way ANOVA with Dunnett’s multiple comparison test. The means of groups DENV-2 P8-immune (n = 8), DENV-2 NGC-immune (n = 3), DENV-2 SN (n = 2), ZIKV PR-immune (n = 3), and ZIKV DakAr-immune (n = 3) were compared with the flavivirus-naïve, i.e., control group (n = 3) at each time point. Flavivirus-naïve group had significantly higher AST levels compared to DENV-2 NGC-immune group (p = 0.0092) at 2DPI, and DENV-2 P8-immune group (p = 0.0043) at 3DPI. Data are presented as mean values ± SD. Statistical significance (*) color is attributed to the significant difference between that group compared to the flavivirus-naïve group. Source data are provided as a Source Data file.
Prior heterologous immunity does not affect cytokine responses
The levels of certain cytokines and chemokines like interleukin-6 (IL-6), monocyte chemoattractant protein-1 (MCP-1), interferon-inducible protein (IP-10), tumor necrosis factor-α (TNF-α), and IL-1 receptor antagonist (IL-1ra) are significantly higher in humans when fatal cases are compared to non-fatal YF27. To understand the impact of heterologous flavivirus immunity on serum cytokine and chemokine levels after YFV infection, we conducted a Milliplex assay on samples collected at 5 DPI and prior to euthanasia [day 14 for all animals except day 9 for FR1565 (euthanasia based on clinical scoring)] and compared them to baseline levels. Of the 23 cytokines and chemokines measured, 18 remained below the limit of detection for all animals, except FR1565 (Fig. 5a). IL-1ra is an anti-inflammatory cytokine that binds to the IL-1 receptor and can suppress pro-inflammatory cytokines like IL-1, TNF-α, and type I interferon. All 23 animals had elevated IL-1ra on day 5. At euthanasia, most animals had either reduced or maintained IL-1ra levels with the exception of animal FR1565, which had a 1674-fold increase compared to baseline (43.94 pg/mL on day 0 vs. 73,568 pg/mL on day 9) (Fig. 5b). Increased levels of IL-1ra in the early stages of infection indicate a modulation of the inflammatory response. However, extremely high production of IL-1ra (as seen in animal FR1565) could affect the overinduction of anti-viral cytokines, which may contribute to the switch from a balanced immune environment to inflammation-induced tissue damage28. MCP-1 is a chemoattractant for monocytes as well as other immune cells like T lymphocytes and NK cells and can be secreted in response to activated pathogen recognition receptors, or by other cytokines like IL-6, IFN-β, and TNFα29. Levels of MCP-1 were elevated on day 5 in all animals, but declined by day 14 except in FR1565, which had a 4.8-fold increase compared to baseline levels (consistent with fatal human YF) (Fig. 5c). Soluble CD40L (sCD40L) is primarily released by platelets upon viral activation, and high levels have been associated with disease progression in HIV, DENV, and Influenza A virus infection30. In hemorrhagic DENV infection, sCD40L levels are significantly decreased in patients with plasma leakage compared to those with no leakage, an indication of thrombocytopenia31. Most of the 23 animals we infected with YFV had slight changes in sCD40L levels, except FR1565, which had a 42-fold decrease compared to baseline levels, suggesting destruction of platelets (Fig. 5d). IL-8 (CXCL8) is a chemokine that plays a key role in inflammation by attracting neutrophils and T cells. For majority of animals, IL-8 levels remained unchanged or declined slightly after YFV infection, consistent with previous studies on macaques32 (Fig. 5e). Interestingly, IL-8 levels were substantially elevated in ZIKV-immune animals. High levels of IL-8 have been reported in convalescent ZIKV patients33, suggesting that prior ZIKV immunity could be an important factor in elevating IL-8 levels post-YFV-infection. Although not conclusive, one possible explanation could be the long-term persistence of ZIKV potentially resulting in persistent immune activation and predisposition to pro-inflammatory state. Since viral persistence is not observed in DENV infection, that could mark the difference between the two groups.
Log2 fold-change in 23 different cytokines and chemokines measured in sera of FR1565 (ZIKV-exposed, seronegative animal) on days 5 and 9 post-YFV infection and compared with baseline levels (a). Log2 fold-change in IL-1ra (b), MCP-1 (c), sCD40L (d), IL-8 (e), and VEGf (f) at 5 DPI and euthanasia timepoints (14 DPI for all animals, 9 DPI for FR1565). Data shown for 23 animals; groups from left to right divided by dotted line are as followed: Flavivirus-naïve, DENV-2-seronegative, DENV-2 P81407-immune, DENV-2 NGC-immune, ZIKV-seronegative, ZIKV PRVABC59-immune, ZIKV DakAr-immune.
Discussion
Mosquito-borne viruses infect hundreds of millions of humans each year, resulting in substantial health, economic, and societal impacts34. The capacity of arboviruses to mutate, potentially expanding their host range, the expansion of the geographic range of mosquito vectors due to climate change, the lack or shortage of vaccines and therapeutics, and the existence of immunologically susceptible populations, raise profound concerns regarding the continued emergence of epidemics or pandemics14. Given that more than 2 billion individuals reside in Asian countries infested by Ae. aegypti34, the potential consequences of YFV establishing itself in this region are grave, particularly since other mosquito-borne viruses like CHIKV and ZIKV arising from African enzootic cycles have repeatedly and efficiently established urban transmission cycles in Asia14. The reasons that YFV has not emerged into Asia in the same manner remain poorly understood.
An intriguing observation arose during the 2016–2019 YFV outbreak in South America. Despite the occurrence of the largest South American YFV epidemic in decades in areas with high human and Ae. aegypti population densities, and with limited vaccine coverage, no evidence was reported of an urban epidemic cycle involving this vector and human amplification. To attempt to explain this conundrum and the historic lack of YF in Asia, we investigated potential immune barriers preventing the urban emergence of YFV. We demonstrated that pre-existing immunity to DENV-2 or ZIKV in NHPs reduces YFV viremia, dramatically reducing mosquito infectivity. To ensure that our study was reflective of typical convalescent flavivirus immunity, and not an acute phase response, we allowed the immunity to develop for at least 6–9 months post-primary infection. Overall, the hyperendemicity of DENV in Asia and South America, but lower seroprevalence in Africa, where urban Ae. aegypti-borne outbreaks continue6,35, further supports the hypothesis that prior flavivirus immunity, especially DENV, plays a major role in preventing urban YFV emergence by limiting the number of competent human amplifying hosts. However, this cross-protection may vary, as suggested by the finding of a major YF epizootic in Uganda just 18 months after a Zika amplification that resulted in an estimated 50% seropositivity. The greater interval (18 versus 6–9 months) between infections comparing this natural outbreak to our experimental infections could be partially responsible for this finding, possibly along with the greater susceptibility of sylvatic African vectors versus Ae. aegypti.
Intriguingly, we also observed that the infectivity for mosquitoes that fed on a DENV-2-immune animal was 20-30% lower compared to flavivirus-naïve animals with similar YFV viremia levels. This suggests the possibility that, in addition to directly reducing viremia, prior DENV-2 exposure could have a secondary blocking effect against YFV infection in mosquitoes. Previous studies have shown that mosquito-borne flaviviruses utilize NS1 proteins produced in the serum to enhance oral infection of the mosquito vector25. As a part of the same study, they showed that anti-NS1 antibodies may not necessarily affect viremia levels but may affect the susceptibility of a mosquito to infection by interfering with midgut infection. Thus, with prior immunity to a heterologous flavivirus, it is possible that YFV NS1 is partially neutralized by heterologous NS1 antibodies, further reducing mosquito infection. Our finding of cross-binding antibodies by ELISAs from DENV and ZIKV-immune sera suggest a role for NS1 antibodies in restricting mosquito infection to limit human amplification potential. Additional experiments with controlled primary infections are needed to further test this hypothesis.
Despite significant differences in mosquito infectivity, we did not observe a striking difference in YF disease outcomes, as indicated by signs of disease, serum chemistries, and cytokine levels, in naive versus flavivirus-immune animals. Since South American strains of YFV are milder compared to African strains in laboratory NHP models, we did not expect to see fatal outcomes in flavivirus-naïve or -immune animals36. The elevated liver enzyme levels in most flavivirus-immune animals appeared to resolve by day 14, suggesting faster recovery and less liver damage. In ZIKV-FRNT-negative but ELISA-positive animal FR1565, all parameters corresponded with fatal human YF. The low levels of ZIKV non-neutralizing IgG we detected suggested the possibility of antibody-dependent enhancement, as has been reported in sequential flavivirus infections (mainly DENV)37. However, with only one animal with a severe outcome and an immunological profile of this kind in our study, we cannot conclude that low-level ZIKV immunity exacerbated the YF outcome; future studies are required to investigate this hypothesis.
While the goal of our study was to investigate the role of heterologous flavivirus immunity on urban emergence of YFV, additional work is needed to determine the impacts of various levels of pre-existing flavivirus immunity on the severity of YF disease, including additional intervals between sequential infections. Of the 720 mosquitoes from which we harvested saliva at 3 and 4 DPI, only one had detectable YFV. Due to restrictions on the number of mosquitoes that can be fed on any one animal, and to maximize the sample size, we decided to harvest mosquitoes at a single timepoint. For future work, multiple timepoints, including greater periods of extrinsic incubation, can be chosen to specifically address the transmission potential. However, as noted previously, relatively low YFV transmission efficiency of Ae. aegypti populations, even those clearly incriminated in epidemics, is not uncommon38.
We did not determine the mechanism of cross-protection exhibited by flavivirus-immune NHPs, other than to rule out cross-reactive neutralizing antibodies. A Pearson’s correlation coefficient was computed to assess the relationship between neutralizing antibody levels and YFV viremia (Supplementary Fig. 7). There was a moderately negative, weak negative, and strong negative correlation between DENV-2 P8 (r = −0.481), DENV-2 NGC (−0.083), and ZIKV PR (−0.973) -immune groups respectively. However, the relationship was not significant (p > 0.05). Similarly, a Pearson’s coefficient was computed to assess the relationship between anti-NS1 ELISA antibodies and YFV viremia (Supplementary Fig. 8). There was a weak negative, moderately negative, strong negative, and moderately positive correlation between DENV-2 P8(r = −0.274), DENV-2 NGC (r = −0.793), ZIKV PR (r = −0.946), and ZIKV DakAr (r = 0.737) -immune groups respectively, but no significance (p > 0.05). Since primary exposure to DENV-2 or ZIKV was variable (via mosquito bites), future animal experiments with controlled primary exposure should be executed to determine true correlation. The role of each arm of adaptive immunity (humoral and cell-mediated) in cross-protection against YF should be investigated in murine models, as well as the potential role of flavivirus NS1 antibodies in blocking mosquito infections to limit the emergence of urban epidemics. Additionally, it is important to investigate the implications for reciprocal effects on DENV and ZIKV infection following YF vaccination or infection. Although our central hypothesis reflected the assumption that human flavivirus immunity, especially for DENV and ZIKV, is lower in Africa than in Asia or South America35,39,40,41,42, it would be useful to know more about seroprevalence in locations such as Angola, which has recently experienced urban YF. In addition, further studies utilizing African strains of YFV and African Ae. aegypti mosquitoes could expand the implications of our work. Although primarily a rural disease43,44, possible cross-protective immunity from Japanese encephalitis (JE), which is endemic in parts of Asia, or from JE vaccination, should also be studied.
In summary, our study indicates that prior immunity in DENV- or ZIKV-endemic regions likely plays a major role in preventing urban YFV emergence by reducing the population of amplification-competent people who can infect Ae. aegypti mosquitoes. These findings have major implications for future risks of YF as flaviviruses continue to spread with anthropogenic changes including further urbanization and climate alterations45. Moreover, the expansion of Ae. aegypti due to climate change increases the risk of YFV transmission in areas such as Southern USA that haven’t experienced YF epidemics in over a century with a population has little to no flavivirus immunity45.
Methods
No statistical methods were used to predetermine the sample size as the NHPs were originally utilized in a separate experiment in keeping with the ethical goal of reducing the total number of animals utilized in research. The experiments were not randomized since the animals were repurposed from another study (published separately). The investigators were not blinded to allocation during experiments and outcome assessment.
Animals, study design, and ethics statement
Twenty-three healthy adolescent cynomolgus macaques (11 males and 12 females, 2.5–5.5 years old, 3–5.5 kg) were transferred from a previous study24, where they were exposed to Ae. albopictus mosquitoes inoculated with PBS (3/23), DENV-2 NGC (3/23), DENV-2 P8-1407 (10/23), ZIKV PRVABC59 (4/23), and ZIKV DakAr 41525 (3/23). After primary exposure, animals transferred to our study were allowed to develop immunity for 6–9 months. Since the primary infections were conducted under a previous, separately published study, we did not determine the sample size and virus strains. To ensure that all animals exposed to homologous viruses during the previous study, were truly infected, we measured the presence of neutralizing antibodies in the baseline sera. All animals were then inoculated subcutaneously with 0.5 ml of YFV BR17 at a final dose of 1 × 104 FFU. The dose and route of inoculation were used to maximize infection and viremia and mimic a mosquito bite. The duration between primary and secondary infection was selected to ensure convalescence, satisfy IACUC limitations on logger surgery, and to account for cost of animal maintenance in containment facilities and available animal resource services.
Temperatures were recorded throughout the course of the study at 15 min intervals on loggers (Star Oddi, Iceland) placed in the abdominal cavity. Animals were individually housed in cages at the UTMB ABSL-3 facility. Animals were fed twice a day with commercial chow, 5045 High Protein Monkey Diet (LabDiet, St. Louis, Missouri). For enrichment, animals were fed an additional item like fruit or vegetable. Health checks were performed at least twice daily from the day of infection until the end of the study. Body weight and rectal temperatures were measured on study days 1–5 and 14. On specified days, animals were anesthetized by intramuscular injection with Ketamine (5–20 mg/kg). Blood samples were collected into serum separator tubes (SST, Greiner Bio-one) and tubes containing ethylenediaminetetraacetic acid (K2-EDTA, BD Vacutainer). Whole blood was analyzed for various parameters using a HEMAVET 950 multispecies hematology instrument (Drew Scientific, Miami, FL). Serum was analyzed using a Preventative Care Profile Plus rotor on a VetScan VS2 Chemistry Analyzer (Abaxis, Union City, CA). A cardboard carton with a mesh top containing 100 female Ae. aegypti (2–4 days-old mosquitoes from Salvador, Brazil, maintained for 18 generations at the UTMB Insectary) were allowed to feed on NHP ears for 5–15 min. Engorged mosquitoes were incubated at 28 °C for 14 days. Animals were humanely euthanized at the end of the study by pentobarbital overdose. All experiments were performed in full compliance with the guidelines established by the Animal Welfare Act for the housing and care of laboratory animals and conducted as laid out in the University of Texas Medical Branch Institutional Animal Care and Use Committee (UTMB-IACUC) approved protocol (protocol #2101002, approved 21 January 2021; protocol #2208052, approved 02 September 2022). UTMB is an Association for Assessment and Accreditation of Laboratory Animal Care International-accredited facility.
Cells
African green monkey kidney epithelial (Vero E6) and Ae. albopictus (C6/36) cells were provided by the World Reference Center for Emerging Viruses and Arboviruses (WRCEVA). Vero E6 cells were grown in minimal essential medium (MEM, Gibco, Grand Island, NY) supplemented with 10% fetal bovine serum (FBS, Atlanta Biologics, Atlanta, GA), 1% penicillin streptomycin (PennStrep, Gibco, Grand Island, NY), 1% sodium bicarbonate (Gibco, Grand Island, NY), and 1% glutamax (Gibco, Grand Island, NY). C6/36 cells were grown in MEM and L-15 media at a ratio of 1:1, supplemented with 10% FBS, 1% PennStrep, 1% glutamax, 1% sodium bicarbonate, 10% tryptose phosphate broth solution (TPB, Sigma, St Louis, MO), 2% non-essential amino acid solution (Sigma, St Louis, MO). Cells were maintained at 37 °C with 5% CO2.
Viruses
The YFV BR17 stock was generated at the WRCEVA (originally acquired from Dr. Betânia Drumond, Universidade Federal de Minas Gerais, Brazil). The virus was isolated from an infected Alouatta guariba in 2017 in Minas Gerais during the YF epidemic. The virus was passaged three times in C6/36 cells (Ae. albopictus cell line) to generate a low passage contemporary YFV BR17 stock that was utilized for the primate challenge.
Stocks of DENV-1 16007, DENV-3 D83-144, DENV-4 703-4, DENV-2 NGC, DENV-2 P8-1407, ZIKV PRVABC59, and ZIKV DakAr 41525 were acquired from WRCEVA and passaged once in C6/36 cells (for DENV-2 strains) and Vero E6 (for ZIKV strains). These viral stocks were used for foci reduction neutralization test (FRNT). DENV-1 16007 was originally isolated from a human in 1964 in Thailand (known passage history: once in C6/36 cells), DENV-2 NGC was originally isolated from human serum in 1944 in New Guinea (known passage history: once in monkeys and five times in C6/36 cells), DENV-2 P8-1407 was originally isolated from a sentinel macaque in 1968 in Malaysia (known passage history: two times in C6/36 cells), DENV-3 D83-144 was originally isolated form human plasma in 1983 in Thailand (known passage history: two times in C6/36 cells), DENV-4 703-4 was originally isolated from a human in Thailand and was acquired by the WRCEVA in 2014 with an unknown date of original isolation (known passage history: three times in C6/36 cells). ZIKV PRVABC59 was originally isolated from a human in 2015 in Puerto Rico (known passage history: four times in Vero E6 cells) and ZIKV DaKAR 41525 was originally isolated from Aedes africanus mosquitoes in 1984 in Senegal (known passage history: once in AP61 cells, two times in C6/36 cells and once in Vero cells).
Mosquito feeding assay
Aedes aegypti obtained from Salvador, Brazil, were maintained in the UTMB Insectary and utilized at generation F18. Female mosquitoes (100 in each cup) were sucrose-starved for approximately 16 h. On days 1–5 post-YFV infection, one separate cup of mosquitoes was exposed to individual NHPs on the ear(s) for 5–15 min, to make a total of five separate cups per animal (one per day) and 115 cups for the entire study of 23 animals. After feeding, the cardboard carton containing the mosquitoes was placed in the refrigerator until the mosquitoes were fully anesthetized. The carton was transferred to a glove box and placed on ice. The mosquitoes were then placed in a petri dish and visually engorged (bloated red abdomen) mosquitoes were transferred to a fresh petri dish on ice and counted. The non-engorged mosquitoes were eliminated from the study by dropping them in 70% ethanol. Fully engorged mosquitoes were maintained at 28 °C with a 16 h light/8 h dark cycle with ad libitum access to 10% sucrose. At 14 days post-feeding, legs and wings were removed from cold-anesthetized mosquitoes and collected in 0.5 ml homogenization media (DMEM supplemented with 2% FBS, 1% antibiotic-antimycotic) with 5 mm stainless steel sterile bead (Glen Mills, Clifton, NJ). Mosquitoes were force-salivated by inserting the proboscis in a 10 µl pipette tip containing 10 µl FBS for approximately 30 min. Saliva-containing FBS was then collected in 0.1 ml homogenization media and the remaining mosquito body was collected in 0.5 ml homogenization media. All samples were stored at −80 °C until the day of processing. Prior to the focus-forming assay to determine the titer and infectivity, samples were thawed and homogenized at a frequency of 26/s for 1 min in a TissueLyser II (Qiagen, Germantown, MD) and centrifuged at 16,500 × g for 5 min. Unfortunately, due to technical difficulties with an incubator that prevented the mosquitoes from surviving for the full 14 days post-feed, we could not complete the harvests of mosquitoes that fed on 5 DENV-2 P81407 immune NHPs (NHP ID: UG253A, FR 423 A, SB 393, CP 60, SB 395). Therefore, mosquito assay data is only available for 18 animals.
Focus-forming assays
Vero E6 cells were seeded in each well of 12 well or 96 well plates and cultured at 37 °C, 5% CO2 for 24 h until 95% confluency. To determine the viremia, serum samples were serially diluted with Vero maintenance media (MEM, 2% FBS, 1% Penn-Strep, 1% Glutamax, 1% sodium bicarbonate) and transferred to the pre-seeded Vero E6 cells in 12 well plates. The samples were incubated at 37 °C for 1 h. After incubation, 1 ml of overlay media (Opti-MEM (Gibco, Grand Island, NY) supplemented with 1% carboxymethyl cellulose (Sigma Aldrich, St. Louis, MO), 2% FBS, 1% Penn-Strep was added to each well. After a 5-day incubation, formalin was added to fix the infected plates. After three washes with 1X DPBS (Gibco, Grand Island, NY), wells were blocked with the blocking buffer i.e., 1 ml of non-fat dry milk (Apex Chemicals and Reagents, Houston, TX) in 1X DPBS (5% w/v) for 30 min on a plate rocker. The blocking buffer was discarded, and plates were primarily stained with anti-YFV primary antibody (mouse immune ascitic fluid acquired from WRCEVA) diluted at 1:1000 in block buffer and was used for staining overnight at a volume of 300 µl per well. The following day, plates were washed (3x with 1X DPBS) and stained with a secondary antibody (affinity purified antibody peroxidase labeled goat anti-mouse IgG, SeraCare, Milford, MA) diluted at 1:2000 in blocking buffer at a volume of 300 µl per well and incubated on the plate rocker for 1 h. Following a final three washes, plates were stained using KPL TrueBlue Peroxidase Substrate (SeraCare, Milford, MA) at a volume of 150 µl per well, and foci were counted to determine the final infectious viral load expressed as FFU/mL. For mosquito titrations, homogenized samples were titrated on 96-well plates with Vero E6 cells, fixed at day 4, and stained with 40 µl primary and secondary antibodies and 25 µl TrueBlue. Foci were manually counted from images obtained on Cytation 7 plate reader (Agilent Life Sciences, Santa Clara, CA). For mosquito infectivity, 100 µl of homogenate was used to infect Vero E6 cells in 96-well plates without dilution, fixed at day 7, and stained as with mosquito titrations.
Foci reduction neutralization test (FRNT)
To determine the neutralizing capacity of antibodies in sera, FRNTs were conducted on baseline samples (prior to YFV infection). Samples from primates that were exposed to DENV-2 NGC or P8-1407 were tested against all four serotypes of DENV (using the strains mentioned above) and YFV (BR17). Neutralizing antibodies from DENV-2 exposed animals were measured against homologous strains. Samples from animals exposed to ZIKV PRVABC59 or DakAr 41525 were tested against ZIKV and YFV. Briefly, sera were serially diluted two-fold and mixed with 800 FFU of the respective virus. Serum-virus mixture was incubated at 37 °C for 1 h followed by infection of Vero E6 cells on 12 well plates. Samples tested against DENV1, 3, and 4 were fixed on day 4, and DENV-2 and YFV were fixed on day 5, and ZIKV was fixed on day 3. Plates were stained as mentioned above with the respective primary antibodies. The neutralizing titer was represented as the reciprocal of the highest dilution of serum that inhibited 50% of foci (FRNT50). Samples that scored below the limit of detection (<1:20) were considered seronegative.
ELISA
To determine if binding antibodies were present against homologous and heterologous virus, baseline sera was tested against DENV-2 and ZIKV Envelope protein (MyBioSource, San Diego, CA), and cross-binding was tested against YFV NS1 recombinant protein (MyBioSource, San Diego, CA). Briefly, on day one, flat-bottom immune plates 96-well (Thermo Fisher, Waltham, MA), were coated with respective recombinant proteins and incubated at 4 °C, overnight. On day 2, plates were washed and blocked with 3% non-fat milk in PBS-T for 2 hours. Diluted serum samples (started with 1:100, and serially diluted by 1:2, up to 6 dilutions) were added to washed plates and incubated for 1 h. Secondary antibody (anti-monkey IgG, HRP, Thermo Fisher) was added at a dilution of 1:10,000 to washed plates and incubated for 1 h. Binding was visualized by adding OPD substrate (Thermo Fisher) and the plates were read at 490 nm on a VersaMax Microplate Reader (Molecular Devices, San Jose, CA).
Cytokine and chemokines
Sera samples collected on day 5 and on the euthanasia day (14 or 9), were analyzed for 23 cytokines and chemokines using the Milliplex NHP Cytokine Magnetic Bead Panel (Millipore Sigma, Burlington, MA) following the manufacturer’s protocol. Results were analyzed on Bio-Plex 200 (Biorad, Hercules, CA). Standard curves of known concentrations of cytokines were used to convert fluorescence units into cytokine concentration units (pg/mL).
Statistical analysis
Descriptive statistics have been provided in figure legends. Log10 transformed viremia titers in each group were analyzed by two-factor repeated measures ANOVA with Tukey’s multiple comparison test. Mosquito infection rates were analyzed by two-tailed Fisher’s exact test by combining the data in each group and comparing with the flavivirus-naïve group. Log10 transformed viral titers in mosquito groups were compared with flavivirus-naïve group by one-way ANOVA with Dunnet’s multiple comparison test. Samples that had viremia and viral loads below the limit of detection were graphed as ½ of LOD and the same value was used for statistical analyzes. For comparisons between more than two groups and more than two timepoints, analyzes by two-way ANOVA repeated measures and appropriate post-hoc tests were conducted. All statistical analysis and graphing was performed with GraphPad Prism Version 10.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
The source data generated in this study are provided in the Supplementary Information/Source Data file. Source data are provided with this paper.
References
Kuno, G. The absence of yellow fever in Asia: history, hypotheses, vector dispersal, possibility of YF in Asia, and other enigmas. Viruses 12, 1349 (2020).
Monath, T. P. & Barrett, A. D. T. Pathogenesis and pathophysiology of yellow fever. in Advances in Virus Research, Vol. 60 343–395 (Elsevier, 2003).
Norrby, E. Yellow fever and Max Theiler: the only Nobel Prize for a virus vaccine. J. Exp. Med. 204, 2779–2784 (2007).
Gershman, M. D. Addressing a yellow fever vaccine shortage—United States, 2016–2017. MMWR Morb. Mortal Wkly. Rep. 66, (2017).
Hanley, K. A. et al. Fever versus fever: the role of host and vector susceptibility and interspecific competition in shaping the current and future distributions of the sylvatic cycles of dengue virus and yellow fever virus. Infect. Genet. Evol. 0, 292–311 (2013).
Angola: Epidemic (Yellow Fever) Emergency Plan of Action Preliminary Final Report (MDRAO006) - Angola | ReliefWeb. https://reliefweb.int/report/angola/angola-epidemic-yellow-fever-emergency-plan-action-preliminary-final-report-mdrao006.
Ingelbeen, B. et al. Urban yellow fever outbreak—Democratic Republic of the Congo, 2016: towards more rapid case detection. PLoS Negl. Trop. Dis. 12, e0007029 (2018).
de Abreu, F. V. S. et al. Haemagogus leucocelaenus and Haemagogus janthinomys are the primary vectors in the major yellow fever outbreak in Brazil, 2016–2018. Emerg. Microbes Infect. 8, 218–231 (2019).
Saluzzo, J. F., Gonzalez, J. P., Hervé, J. P. & Digoutte, J. P. Isolements du virus de la fièvre jaune à partir de moustiques du groupe Aedes (Stegomyia) Africanus (theobald) en République Centrafricaine au cours de l’année 1978. Annales de. l’Institut Pasteur/Virologie 131, 313–321 (1980).
McCrae, A. W. R. & Kirya, B. G. Yellow fever and Zika virus epizootics and enzootics in Uganda. Trans. R. Soc. Trop. Med. Hyg. 76, 552–562 (1982).
Sacchetto, L. et al. Neighbor danger: yellow fever virus epizootics in urban and urban-rural transition areas of Minas Gerais state, during 2017-2018 yellow fever outbreaks in Brazil. PLoS Negl. Trop. Dis. 14, e0008658 (2020).
Löwy, I. Leaking containers: success and failure in controlling the mosquito aedes aegypti in Brazil. Am. J. Public Health 107, 517–524 (2017).
Shearer, F. M. et al. Global yellow fever vaccination coverage from 1970 to 2016: an adjusted retrospective analysis. Lancet Infect. Dis. 17, 1209–1217 (2017).
Weaver, S. C., Charlier, C., Vasilakis, N. & Lecuit, M. Zika, chikungunya, and other emerging vector-borne viral diseases. Annu. Rev. Med. 69, 395 (2018).
Cui, S. et al. Detection of yellow fever virus genomes from four imported cases in China. Int. J. Infect. Dis. 60, 93–95 (2017).
de G. de Lataillade, L. et al. Risk of yellow fever virus transmission in the Asia-Pacific region. Nat. Commun. 11, 5801 (2020).
Mutebi, J.-P. et al. Yellow fever virus infectivity for Bolivian Aedes aegypti mosquitoes. Emerg. Infect. Dis. 10, 1657–1660 (2004).
Couto-Lima, D. et al. Potential risk of re-emergence of urban transmission of yellow fever virus in Brazil facilitated by competent Aedes populations. Sci. Rep. 7, 4848 (2017).
Theiler, M. & Anderson, C. R. The relative resistance of dengue-immune monkeys to yellow fever virus. Am. J. Trop. Med. Hyg. 24, 115–117 (1975).
Agampodi, S. B. & Wickramage, K. Is there a risk of yellow fever virus transmission in South Asian countries with hyperendemic dengue? BioMed. Res. Int. 2013, e905043 (2013).
Henderson, B. E., Cheshire, P. P., Kirya, G. B. & Lule, M. Immunologic studies with yellow fever and selected African group B arboviruses in rhesus and vervet monkeys. Am. J. Trop. Med. Hyg. 19, 110–118 (1970).
Ikejezie, J. et al. Zika Virus Transmission—Region of the Americas, May 15, 2015–December 15, 2016. 66, (2017).
Duong, V., Dussart, P. & Buchy, P. Zika virus in Asia. Int. J. Infect. Dis. 54, 121–128 (2017).
Hanley, K. A. et al. Trade-offs shaping transmission of sylvatic dengue and Zika viruses in monkey hosts. Nat. Commun. 15, 2682 (2024).
Liu, J. et al. Flavivirus NS1 protein in infected host sera enhances viral acquisition by mosquitoes. Nat. Microbiol 1, 16087 (2016).
Kallas, E. G. et al. Predictors of mortality in patients with yellow fever: an observational cohort study. Lancet Infect. Dis. 19, 750–758 (2019).
ter Meulen, J. et al. Activation of the cytokine network and unfavorable outcome in patients with yellow fever. J. Infect. Dis. 190, 1821–1827 (2004).
Zhao, Y. et al. Longitudinal COVID-19 profiling associates IL-1RA and IL-10 with disease severity and RANTES with mild disease. JCI Insight 5, e139834 (2022).
Ruiz Silva, M., van der Ende-Metselaar, H., Mulder, H. L., Smit, J. M. & Rodenhuis-Zybert, I. A. Mechanism and role of MCP-1 upregulation upon chikungunya virus infection in human peripheral blood mononuclear cells. Sci. Rep. 6, 32288 (2016).
Ostermeier, B., Soriano-Sarabia, N. & Maggirwar, S. B. Platelet-released factors: their role in viral disease and applications for extracellular vesicle (EV) therapy. Int J. Mol. Sci. 23, 2321 (2022).
Tramontini Gomes de Sousa Cardozo, F. et al. Serum from dengue virus-infected patients with and without plasma leakage differentially affects endothelial cells barrier function in vitro. PLoS One 12, e0178820 (2017).
Engelmann, F. et al. Pathophysiologic and transcriptomic analyses of viscerotropic yellow fever in a rhesus macaque model. PLoS Negl. Trop. Dis. 8, e3295 (2014).
Tappe, D. et al. Cytokine kinetics of Zika virus-infected patients from acute to reconvalescent phase. Med. Microbiol. Immunol. 205, 269–273 (2016).
Leta, S. et al. Global risk mapping for major diseases transmitted by Aedes aegypti and Aedes albopictus. Int J. Infect. Dis. 67, 25–35 (2018).
Simo, F. B. N. et al. Dengue virus infection in people residing in Africa: a systematic review and meta-analysis of prevalence studies. Sci. Rep. 9, 13626 (2019).
Shinde, D. P., Plante, J. A., Plante, K. S. & Weaver, S. C. Yellow fever: roles of animal models and arthropod vector studies in understanding epidemic emergence. Microorganisms 10, 1578 (2022).
Halstead, S. B. Dengue antibody-dependent enhancement: knowns and unknowns. Microbiol. Spectr. 2 (2014).
Miller, B. R., Monath, T. P., Tabachnick, W. J. & Ezike, V. I. Epidemic yellow fever caused by an incompetent mosquito vector. Trop. Med. Parasitol. 40, 396–399 (1989).
Gake, B. et al. Low seroprevalence of Zika virus in Cameroonian blood donors. Braz. J. Infect. Dis. 21, 481–483 (2017).
Marchi, S. et al. Zika virus in West Africa: a seroepidemiological study between 2007 and 2012. Viruses 12, 641 (2020).
Chiaravalloti-Neto, F. et al. Seroprevalence for dengue virus in a hyperendemic area and associated socioeconomic and demographic factors using a cross-sectional design and a geostatistical approach, state of São Paulo, Brazil. BMC Infect. Dis. 19, 441 (2019).
Ng, R. J., Chong, Z. L., Abdul Mutalip, M. H. & Ng, C.-W. Dengue seroprevalence and factors associated with dengue seropositivity in Petaling district, Malaysia. Int J. Environ. Res. Public Health 19, 7170 (2022).
Keiser, J. et al. Effect of irrigated rice agriculture on Japanese encephalitis, including challenges and opportunities for integrated vector management. Acta Trop. 95, 40–57 (2005).
Di Francesco, J. et al. Comparison of the dynamics of Japanese encephalitis virus circulation in sentinel pigs between a rural and a peri-urban setting in Cambodia. PLoS Negl. Trop. Dis. 12, e0006644 (2018).
Jácome, R. et al. A yellow flag on the horizon: the looming threat of yellow fever to North America. Int. J. Infect. Dis. 87, 143–150 (2019).
Acknowledgements
The research was supported by the World Reference Center for Emerging Viruses and Arboviruses, NIH grants R24AI120942 (SCW), by the Centers for Research in Emerging Infectious Diseases (CREID); the West African Center for Emerging Infectious Diseases (WAC-EID) U01-AI151801 (SCW) and The Coordinating Research on Emerging Arboviral Threats Encompassing the Neotropics (CREATE-NEO) U01 AI151807 (NV) and R01 AI145918 (NV). R.K.C. was supported by NIH grant K99AI168484. B.P.D is a research fellow of National Council for Scientific and Technological Development (CNPq)/Brazil. D.P.S was supported by the Center for Vector-borne and Zoonotic Diseases and the Jeane B. Kempner Fellowship from University of Texas Medical Branch. We thank the Animal Resource Center at UTMB for their assistance with primate work, and the Insectary staff (Ruimei Yun, Jiehua Zhou) at UTMB for providing mosquitoes from the colony.
Author information
Authors and Affiliations
Contributions
Conceptualization, D.P.S., K.S.P., J.A.P., N.V., S.C.W. Methodology, D.P.S., K.S.P., J.A.P., S.C.W. Investigation, D.P.S., J.A.P., D.S., B.M., J.W., S.R.A., R.K.C., L.S., B.D., N.V., K.S.P., S.C.W. Writing-original draft, D.P.S., S.C.W. Writing-review and editing, D.P.S., J.A.P., D.S., B.M., J.W., S.R.A., R.K.C., L.S., B.D., N.V., K.S.P., S.C.W. Funding acquisition, N.V., S.C.W.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Carlos Sariol and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Shinde, D.P., Plante, J.A., Scharton, D. et al. Potential role of heterologous flavivirus immunity in preventing urban transmission of yellow fever virus. Nat Commun 15, 9728 (2024). https://doi.org/10.1038/s41467-024-54146-9
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-024-54146-9
This article is cited by
-
Pre-existing YFV-17D immunity mediates T cell cross-protection against dengue virus serotype 2 infection in mice
Communications Biology (2025)
-
Yellow Jack: a modern threat to Asia-Pacific countries?
npj Viruses (2025)