Abstract
Oral vaccines provide a non-invasive approach for cancer immunotherapy but face challenges in gastrointestinal stability, antigen presentation, and mucosal delivery. Here, we present an engineered probiotic-based oral vaccine system, BacOR-Fn-T+phiX174, featuring genetically encoded dual-antigen ferritin arrays and inducible bacterial lysis. Upon oral administration and arabinose induction, the probiotic strain lyses in situ, releasing OVA/TRP2-decorated ferritin nanoparticles that efficiently traverse the intestinal barrier via M-cell targeting and activate mucosal dendritic cells. This platform robustly stimulates CD8+ and CD4+ T-cell responses, enhances B-cell and macrophage activation, reduces regulatory T cells, and provides therapeutic efficacy against melanoma in both lung metastasis and subcutaneous tumor models. It also establishes durable immunological memory without disrupting systemic or mucosal homeostasis. This work offers a programmable bacterial chassis for precise antigen array presentation and controlled delivery, representing a promising strategy for next-generation, needle-free cancer vaccines.
Similar content being viewed by others
Introduction
Therapeutic cancer vaccines have emerged as promising strategies that harness the adaptive immune system to specifically recognize and eliminate tumor cells, thereby suppressing tumor growth and preventing metastasis progression1,2. The first therapeutic cancer vaccine approved by the U.S. Food and Drug Administration (FDA) in 2010, Sipuleucel-T, and the majority of therapeutic vaccines under clinical investigation rely on parenteral administration3,4. Despite their demonstrated clinical benefits, injectable vaccines are associated with limitations such as injection site pain, risk of local infection, and reduced patient compliance5,6. In contrast, oral vaccines offer significant advantages, including non-invasiveness, ease of administration, reduced medical burden, and potential to stimulate both systemic and mucosal immune responses7,8. Importantly, oral vaccination can elicit cytotoxic T lymphocyte (CTL) responses and humoral immunity, both essential for effective tumor clearance via direct killing and antibody-mediated cytotoxicity9.
Despite these advantages, the development of oral tumor vaccines—particularly protein-based vaccines—remains challenging due to multiple physiological and immunological barriers. These include degradation by gastric acid and proteases, poor absorption across the intestinal epithelium, and limited antigen presentation efficiency10,11,12. Although nanoparticle-based delivery platforms such as liposomes, micelles, dendrimers, and polymeric particles have been widely explored to protect antigens and enhance delivery to gut-associated lymphoid tissue (GALT)13,14, issues such as poor batch reproducibility, variable loading efficiency, and limited induction of robust cellular immunity continue to limit their translational potential.
Engineered bacteria have gained attention as next-generation delivery vehicles owing to their natural tropism for mucosal sites and inherent immunostimulatory properties15,16. Commensal bacteria colonizing the gastrointestinal (GI) tract are known to participate in regulating host digestive, immune, and nervous systems17, demonstrating their intrinsic stability and biocompatibility under GI conditions. Recent advances in synthetic biology have enabled the precise genetic programming of live bacteria to express specific antigens in situ and release them via controlled lysis, offering an integrated platform for antigen production, delivery, and release within the gut environment18,19,20. Such systems hold promise for overcoming GI degradation and improving vaccine bioavailability.
However, surviving the GI tract alone is not sufficient to induce potent antitumor responses. Efficient antigen transport across the intestinal epithelial barrier and enhancement of antigen immunogenicity are also essential21. Targeting microfold (M) cells in the Peyer’s patches, which specialize in antigen sampling and transport to underlying immune cells, has emerged as a promising strategy to facilitate vaccine uptake22,23. Meanwhile, protein-based nanostructures such as ferritin have gained interest as antigen scaffolds due to their uniform size, intrinsic stability, and self-assembling capacity, which allows for multivalent display of antigens. Ferritin-based vaccines have shown efficacy against several pathogens, including hepatitis B virus and SARS-CoV-224,25.
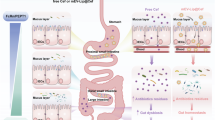
In this study, we engineered a programmable probiotic-based oral vaccine platform that integrates genetically encoded ferritin nanoparticle scaffolds for dual-antigen presentation with controllable mucosal delivery. This platform, termed BacOR-Fn-T+phiX174, is designed to survive GI transit and, upon exposure to arabinose in the intestine, undergo on-demand lysis to release ferritin nanoparticles (OR-Fn-T) that multivalently display tumor epitopes and carry an RGD motif for M-cell engagement. To provide a conceptual overview of the vaccine design and study rationale, a schematic summary is presented in Fig. 1.
Engineered bacteria were co-transformed with pET22b-OVA-RGD-Fn-TRP2 and pBAD33-phiX174 plasmids and termed BacOR-Fn-T+phiX174. The lac and ara promoters are IPTG- and arabinose-inducible, respectively. Upon oral administration with IPTG-induced BacOR-Fn-T+phiX174 and arabinose, the bacteria lyse in the gut, releasing the OR-Fn-T nanoparticles. OR-Fn-T crosses the intestinal barrier via RGD-mediated M cell targeting and induces robust humoral and cellular immune responses to eliminate tumors and provide long-term immune surveillance.
Upon oral administration of the engineered Escherichia coli strain (BacOR-Fn-T+PhiX174) with the arabinose inducer, bacteria undergo lysis in the intestine and release OR-Fn-T nanoparticles. The RGD peptide enables targeting to M cells via α5β1 integrin binding, promoting translocation across the intestinal epithelium and enhanced uptake by antigen-presenting cells. The multivalent display of dual antigens by ferritin facilitates strong B-cell activation and efficient DC maturation, leading to robust humoral and cellular immune responses. This orally administered platform demonstrated both prophylactic and therapeutic efficacy in a mouse melanoma model. By combining engineered probiotic vectors with structurally defined antigen-presenting nanostructures, our work provides a modular platform for oral tumor vaccine design. This strategy addresses key challenges in oral vaccine development—GI stability, mucosal delivery, and immunogenicity—and offers a promising avenue for the advancement of next-generation cancer immunotherapies.
Results
Construction and characterization of the Bac OR-Fn-T+phiX174 oral vaccine system
To implement the schematic design in Fig. 1, we engineered a recombinant ferritin nanoparticle (OR-Fn-T) displaying two different antigens alongside a mucosal targeting peptide. Specifically, OVA257–264 (CD8+ T cell epitope), OVA323–339 (B cell epitope), and an α5β1 integrin-targeting RGD peptide were fused to the N-terminus of ferritin, while the TRP2180–188 (CD8+ T-cell epitope) was fused to its C-terminus, allowing precise 24-meric antigen presentation. The corresponding gene was cloned into the pET22b vector, and the lysis gene phiX174E was inserted into the arabinose-inducible plasmid pBAD33. Co-transformation of these plasmids into E. coli Rosetta (DE3) yielded four strains expressing distinct antigenic configurations (Fig. 2A): BacR-Fn+phiX174 (G1) expressed ferritin with RGD only (R-Fn); BacTR-Fn+phiX174 (G2) expressed TRP2-RGD-fused ferritin (TR-Fn); BacOR-Fn+phiX174 (G3) expressed OVA-RGD-fused ferritin (OR-Fn); and BacOR-Fn-T+phiX174 (G4) expressed the full dual-antigen construct (OR-Fn-T). All strains co-expressed the phiX174 lytic module.
A Schematic representation of bacterial groups expressing various ferritin constructs. B Antibody tagging strategy for detection of dual-antigen OR-Fn-T expression. C Western blot analysis confirmed expression of OR-Fn-T and phiX174. D Size exclusion chromatography profile of ferritins on a Superdex 200 pg column. E TEM images and F hydrodynamic size distribution of ferritins. Representative results from three independent experiments are shown (E). Source data are provided as a Source Data file.
To facilitate downstream identification, HA, c-Myc, and Flag tags were fused to OVA, TRP2, and phiX174, respectively. Sequential western blot analysis using HA and c-Myc antibodies confirmed the successful dual display of OVA and TRP2 on ferritin in G4 (Fig. 2B, C), with the expected molecular weight of OR-Fn-T ~ 25 kDa, further validated by SDS-PAGE (Supplementary Fig. 1). Expression of the lytic protein phiX174 (~11 kDa) was confirmed in all four groups.
Purified ferritin proteins were obtained via ion exchange and size exclusion chromatography (Fig. 2D). Transmission electron microscopy (TEM) imaging confirmed their uniform spherical morphology (Fig. 2E), while dynamic light scattering (DLS) indicated an average hydrodynamic diameter of approximately 16 nm across all groups (Fig. 2F). Zeta potential analysis showed no significant difference between the constructs, with OR-Fn-T exhibiting a surface charge of −13.75 ± 2.1 mV (Supplementary Fig. 2 and Table S1).
Inducible bacterial lysis and intestinal distribution of Bac OR-Fn-T+phiX174
Following the structural and antigenic validation of the BacOR-Fn-T+phiX174 vaccine system, we next evaluated its functional properties—specifically the controllable bacterial lysis and biodistribution profile in the GI tract. To ensure the timely release of the ferritin vaccine following oral administration, the lytic function of phiX174 was first validated in vitro. After induction with 1 mg/mL arabinose (optimized via growth curve screening; Supplementary Fig. 3), more than 99% of BacOR-Fn-T+phiX174 were lysed within 8 h, as evidenced by bacterial cloning forming unit (CFU) enumeration (Fig. 3A, B). Consistently, western blot of the culture supernatant (Supplementary Fig. 4) showed that OR-Fn-T release was detectable as early as 2 h after arabinose induction, peaked at 4 h, and remained at a comparable level at 6 h. These data indicate that antigen release kinetics closely parallel bacterial lysis, supporting the effective and timely availability of ferritin antigens for immune activation.
A Colony-forming unit (CFU) image after arabinose induction. B Number of colonies quantification over time (n = 3 independent experiments; p values are determined with two-tailed unpaired Student’s t-test). C Bacterial growth curves in LB, SGF, and SIF ± arabinose via OD600nm measurement (n = 3 independent experiments). D TEM showing bacterial morphology after 6 h under different conditions. Scale bar = 1 µm. E In vivo bioluminescence imaging of the mouse GI tract after oral administration with BacOR-Fn-T+Luc and arabinose water. The reporter strain carries luciferase under control of the pBAD promoter, resulting in arabinose-inducible light emission but no lysis. F Quantitative analysis of luminescence intensity in different GI regions (n = 3 mice per group). G Bacterial colonies were recovered from feces on LB agar plates. H Quantification of viable BacOR-Fn-T+phiX174 in feces over time (n = 3 independent experiments). Data are presented as mean ± SD; analyzed via one-way ANOVA with a Sidak’s multiple comparisons test. Source data are provided as a Source Data file.
We then assessed whether this lysis system functioned effectively under physiological conditions. A crucial design criterion for live oral vaccines is that the bacteria’s growth and lysis be well-controlled within the host GI tract. We therefore evaluated the behavior of BacOR-Fn-T+phiX174 under simulated GI conditions and in live mice. First, we tested whether the phiX174E lysis circuit could be induced in the harsh environments of the stomach and gut. In simulated gastric fluid (SGF, pH~1.2) and simulated intestinal fluid (SIF, with bile salts and enzymes), BacOR-Fn-T+PhiX174 was cultured with or without arabinose, and bacterial growth was monitored. In SIF, the presence of arabinose significantly inhibited bacterial growth compared to SIF without arabinose, mirroring the growth suppression observed in standard LB broth with arabinose (Fig. 3C). This indicates that arabinose induction can effectively trigger bacterial lysis under intestinal conditions. In SGF, bacteria exhibited very limited growth in general; moreover, the addition of arabinose made little difference in viability. Since pBAD induction depends on energy-coupled arabinose uptake and active transcription and translation, extreme acid stress in SGF (pH ~1–2, pepsin) drives E. coli into a low-metabolic survival state26,27, Consequently, no obvious lysis occurred in SGF regardless of arabinose, whereas in SIF—where cells remain viable and metabolically active—arabinose-triggered lysis became apparent. In order to better simulate the digestive tract environment, BacOR-Fn-T+phiX174 were cultured sequentially in SGF and SIF with or without arabinose (Supplementary Fig. 5). Considering that the solution left the stomach quickly, approximately 20 min28. BacOR-Fn-T+phiX174 were incubated in the SGF for 0.5 h and then continued to be incubated in the SIF for 5.5 h. As expected, the OD600 of BacOR-Fn-T+phiX174 at 6 h with arabinose induction was significantly decreased compared to that without arabinose induction, indicating the efficient lysis of the engineered bacteria. We next visualized the morphological effects of lysis induction by performing scanning electron microscopy (SEM) on BacOR-Fn-T+phiX174 after 6 h of incubation under various conditions. Bacteria cultured in LB medium or in simulated GI fluids without arabinose maintained normal rod-shaped morphology with intact cell walls (Fig. 3D). In contrast, bacteria exposed to arabinose in either LB or SIF showed severe cell envelope disruption, with cell wall breach and collapse, consistent with phiX174E-mediated lysis and release of intracellular contents. These in vitro results confirmed that our engineered strain remains susceptible to arabinose-triggered lysis even in physiologic GI environments, which should enable on-demand antigen release after oral administration.
We then tracked the colonization, induction, and clearance of the vaccine strain in vivo using a bioluminescent reporter system. To distinguish bacterial colonization from antigen release, we constructed a reporter strain, BacOR-Fn-T+Luc, in which the phiX174E lysis gene on pBAD33 was replaced with the luciferase (luc) gene. Thus, while BacOR-Fn-T+phiX174 undergoes arabinose-induced lysis, BacOR-Fn-T+Luc retains arabinose-inducible gene expression but produces bioluminescence instead of lysis. Consistent with this design, luciferase expression was induced by arabinose both in vitro and in vivo, enabling us to track bacterial colonization and clearance without triggering lysis. We firstly verified that luciferase expression in BacOR-Fn-T+Luc could be induced by arabinose by analyzing fluorescence imaging of engineered bacteria in vitro (Supplementary Fig. 6). Next, we orally administered BacOR-Fn-T+Luc to C57BL/6 mice (108 CFU per mouse) along with continuous arabinose supplied in the drinking water, which allowed in vivo monitoring of bacterial distribution and clearance. In vivo imaging revealed that bioluminescent signals became strongly localized in the intestinal tract, particularly the colon region, by 4 h after administration (Fig. 3E, F). This indicates that the bacteria survived transit through the upper GI tract and reached the colon, and that sufficient arabinose reached the colon to further induce luc expression (Supplementary Fig. 7). Importantly, these bioluminescent signals reflect bacterial colonization rather than released antigens, as luciferase is expressed intracellularly in BacOR-Fn-T+Luc. By 6 h post-administration, the bioluminescence had largely disappeared, suggesting rapid elimination of the bacteria from the gut. Consistent with this, ex vivo imaging of dissected intestines at 4 h confirmed that the colon contents exhibited the brightest luminescence among all GI segments (Supplementary Fig. 8A, B), and viable counts of BacOR-Fn-T+Luc recovered from fecal pellets dropped by five orders of magnitude between 12 h and 48 h after administration (Fig. 3G). By 72 h, virtually no live bacteria could be detected in the feces (Fig. 3H), indicating complete clearance of the strain from the body. Together, these findings demonstrate that BacOR-Fn-T+phiX174 can successfully transit to the lower GI tract, express its antigen payload under external inducer control, and then be rapidly lysed and cleared in vivo. This tight control over bacterial fate alleviates concerns about long-term persistence or uncontrolled proliferation of the vaccine strain in the host. Furthermore, the release and stability of OR-Fn-T antigen were evaluated in vivo by gel permeation chromatography (GPC) analysis. The characteristic peaks of OR-Fn-T were still detectable in the colon contents at 6 h after oral administration of BacOR-Fn-T+phiX174 (Supplementary Fig. 9), confirming the release and retention of functional ferritin vaccine in the colon.
Bac OR-Fn-T+phiX174 delivers OR-Fn-T across the intestinal barrier and activates mucosal dendritic cells
Next, we assessed whether the released ferritin nanoparticles could cross the intestinal epithelial barrier and activate mucosal immune cells. We first assessed their mucosal transport capability in both in vitro and in vivo settings. An in vitro M cell co-culture model was established by seeding a Caco-2 intestinal epithelial monolayer with Raji B cells, which induces differentiation of M cell-like patches within the epithelial layer. Dendritic cells were added to the lower chamber after the formation of the simulated epithelial barrier (Fig. 4A). FITC-labeled ferritin nanoparticles were applied to the apical chamber, and uptake by dendritic cells in the basolateral compartment was measured. RGD-modified ferritins (R-Fn and OR-Fn-T) exhibited significantly enhanced transport across the epithelial layer compared to non-RGD control O-Fn-T, with OR-Fn-T showing the highest uptake by basolateral dendritic cells (Fig. 4B). Importantly, OR-Fn-T and R-Fn penetrated at similar levels, indicating that loading ferritin with tumor epitopes did not impede the RGD-mediated transport function. To further evaluate the overall penetration of ferritin across the intestinal epithelial barrier, we quantified the total fluorescence intensity of ferritin in the basolateral chamber. The results showed that OR-Fn-T and R-Fn exhibited comparable transport levels, indicating that the incorporation of tumor epitopes did not compromise the RGD-mediated transcytosis efficiency. Importantly, the penetration of OR-Fn-T was markedly enhanced in the M cell–containing Caco-2/Raji B co-culture model compared with the control Caco-2 monolayer, confirming that M cells play a predominant role in facilitating ferritin passage across the intestinal barrier (Supplementary Fig. 10).
A Schematic of the M cell-mediated transport model. B Flow cytometry analysis of DCs in the basolateral compartment after co-culture with Transwell systems. Fluorescence intensity reflects the uptake of FITC-labeled ferritins transported across the intestinal epithelial layer, thereby indicating the efficiency of antigen sampling by DCs. C Maturation of DCs in the basolateral chamber post-transport (n = 3 independent experiments). D DC2.4 cells were incubated with PBS, free peptides, or ferritins; mature DCs were quantified via flow cytometry (n = 3 independent experiments). E Confocal imaging of colon sections after FITC-labeled ferritin exposure. Scale bars: 100 µm (upper), 20 µm (lower). F Quantification of ferritin penetration (n = 3 independent experiments). G Flow cytometry of mature DCs in the intestinal lamina propria after oral vaccination. H Statistical comparison of mature DC proportions (n = 3 independent experiments). Data are presented as mean ± SD; p values are determined by one-way ANOVA with Sidak’s multiple-comparisons test. Source data are provided as a Source Data file.
However, only OR-Fn-T triggered substantial immune activation in the DCs after crossing the epithelial layer: in the basolateral chamber, ~40% of DCs that had been exposed to OR-Fn-T became mature CD86+ cells (Fig. 4C and Supplementary Fig. 11). In contrast, DCs receiving R-Fn (RGD-ferritin without antigens) remained mostly immature (comparable to DCs with PBS), highlighting that while RGD enhances ferritin delivery across the barrier, the presence of tumor antigens on the ferritin is required to stimulate immune cells. These in vitro results suggest that the combination of M-cell targeting and multivalent antigen display in OR-Fn-T leads to efficient uptake by antigen-presenting cells and robust activation of innate immune pathways.
To further validate the immunostimulatory properties of the ferritin constructs independent of epithelial transport, we directly incubated DC2.4 cells with free peptides (OVA, TRP2), R-Fn, or antigen-bearing ferritins (TR-Fn, OR-Fn, and OR-Fn-T). Flow cytometry revealed that free peptides had modest effects, while TR-Fn, OR-Fn, and especially OR-Fn-T significantly promoted CD80⁺, CD86⁺, and CD11c+ DCs (Fig. 4D and Supplementary Fig. 12). The R-Fn, which contains the RGD targeting motif but lacks any tumor antigen, failed to enhance DCs maturation beyond background levels, suggesting that RGD alone does not contribute to innate immune activation. The highest maturation (~40%) was induced by OR-Fn-T, validating that antigen valency and nanoparticle format—rather than RGD targeting alone—are responsible for innate immune activation.
To corroborate the enhanced mucosal penetration in vivo, we performed a colon loop uptake assay using fluorescently labeled ferritins. FITC-labeled ferritin nanoparticles were injected into isolated colon loops, and their penetration into the mucosa was evaluated via confocal microscopy (Fig. 4E). Fluorescence intensity within the tissue confirmed that RGD-containing ferritins, especially OR-Fn-T, exhibited superior mucosal translocation compared to non-RGD counterparts (Fig. 4F). These results demonstrate that the RGD motif facilitates efficient transcytosis of ferritin constructs through M cells into the intestinal immune environment, a critical prerequisite for effective oral immunization.
To determine whether orally delivered OR-Fn-T can activate local immune cells in vivo, we evaluated DC maturation in the colon lamina propria of mice following oral vaccination. Mice were treated with different engineered bacterial strains together with arabinose, and at 24 h post-administration, colon tissues were harvested for lymphocyte isolation. Flow cytometry analysis of lamina propria lymphocytes showed that OR-Fn-T treatment led to the highest proportion of mature CD80+CD86+CD11c+ DCs among all groups, significantly exceeding those in mice treated with R-Fn or O-Fn-T (Fig. 4G–H and Supplementary Fig. 13).
Together, these results demonstrate that orally released OR-Fn-T nanoparticles can traverse the gut barrier and stimulate innate immune cells at mucosal sites. This supports its utility as a robust oral nanovaccine platform capable of inducing mucosal immunity through a combination of targeted delivery and multivalent antigen display.
Therapeutic effects of Bac OR-Fn-T+phiX174 in a lung metastatic melanoma model
We next assessed the antitumor efficacy of the oral vaccine using an aggressive B16-F10-OVA melanoma lung metastasis model. C57BL/6 mice were injected intravenously with B16-F10-OVA cells (day 0) to establish disseminated lung tumors, then orally vaccinated on days 3, 7, and 14. Five treatment groups were evaluated: G1 received PBS control; G2 received BacR-Fn+phiX174; G3 received BacTR-Fn+phiX174; G4 received BacOR-Fn+phiX174; and G5 received BacOR-Fn-T+phiX174. All vaccine groups were given arabinose in the drinking water to induce bacterial lysis and antigen release in vivo. Mice were sacrificed on day 21 to evaluate lung tumor burden and immune responses (Fig. 5A). The BacOR-Fn-T+phiX174 treatment produced the strongest suppression of lung metastases among all groups. Representative images of excised lungs (Fig. 5B) and quantification of surface metastatic nodules (Fig. 5C) showed that mice in the G5 group had fewer tumor foci compared to the PBS-treated controls. The single-antigen ferritin groups (G3 and G4) exhibited a modest reduction in lung metastases relative to PBS, indicating a partial therapeutic benefit from oral vaccines carrying either TRP2 or OVA alone. However, the dual-antigen vaccine (G5) achieved a significantly greater inhibition of metastatic tumor growth than either single-antigen formulation, highlighting the advantage of the polyvalent antigen strategy. In addition, the lung metastasis levels in mice orally administered purified OR-Fn-T directly showed no significant difference compared to those in mice treated with PBS (Supplementary Fig. 14), due to the disruption of ferritin displayed OVA/TRP2 antigens by the harsh GI environment21,29.
A Experimental timeline, created in BioRender. Jiang, B. (2025) https://BioRender.com/anzggbm. B Representative lung images from each group. Scale bar = 1 cm. C Quantification of metastatic nodules (n = 5 mice per group). D–J Flow cytometry analysis of immune cell populations in spleens: CD8+ T cells, IFNγ+CD8+ T cells, OVA257-264 H2Kb tetramer+ cells in CD3+CD8+ cells, CD4+ T cells, B cells (CD45+CD19+), M1-like macrophage (F4/80+CD80+ cells), and Treg cells (CD4+CD25+ in CD3+ cells) (n = 3 mice per group). K ELISpot images of IFN-γ secretion by splenocytes after re-stimulation with OVA and TRP2 peptides. L Quantification of IFN-γ spots (n = 3 mice per group). M CD8+ T cell infiltration in lung tumor tissues. Scale bars: 1000 µm (upper), 50 µm (lower). Data shown as mean ± SD; analyzed by one-way ANOVA with a Sidak’s multiple comparisons test. Source data are provided as a Source Data file.
To elucidate the immune mechanisms underlying the observed antitumor effect, we performed comprehensive immunophenotyping of splenocytes from each group at the end of the study. Flow cytometry revealed that mice treated with BacOR-Fn-T+phiX174 mounted a broad and robust adaptive immune response that was not observed in the other groups. The G5 vaccine elicited a higher frequency of total CD3+ T cells in the spleen, driven primarily by an expansion of CD8+ CTLs (Fig. 5D and Supplementary Fig. 15). These vaccine-induced CTLs were highly functional, as indicated by a marked increase in interferon-γ–producing CD8+ T cells in G5 mice (Fig. 5E and Supplementary Fig. 16). Moreover, G5 vaccination generated a significantly larger pool of tumor antigen–specific CD8+ T cells (OVA257–264-H2Kb tetramer+) relative to the single-antigen and control groups (Fig. 5F and Supplementary Fig. 17). BacOR-Fn-T+phiX174 also stimulated CD4+ T helper cell responses (Fig. 5G and Supplementary Fig. 18), as well as increased levels of splenic B cells (CD19+; Fig. 5H and Supplementary Fig. 19) and M1-like proinflammatory macrophages (F4/80+ CD80+; Fig. 5I and Supplementary Fig. 20) compared to controls. Concurrently, the frequency of immunosuppressive regulatory T cells (CD3+ CD4+ CD25+) was significantly lower in the G5 group than in PBS or single-antigen groups (Fig. 5J and Supplementary Fig. 21), indicating that the oral vaccine helped relieve tumor-associated immunosuppression. Splenocytes from BacOR-Fn-T+phiX174-vaccinated mice also secreted the highest levels of IFN-γ upon ex vivo restimulation with OVA and TRP2 peptides (Fig. 5K, L), consistent with a potent systemic TH1 immune response.
In parallel, we assessed humoral and local immune responses. ELISA analysis revealed that BacOR-Fn-T+phiX174 vaccination induced the highest serum IgG titers against both OVA and TRP2 (Supplementary Fig. 22), further confirming the induction of strong systemic humoral immunity. Importantly, immunohistochemical analysis of lung tissue confirmed that BacOR-Fn-T+phiX174-treated mice had the greatest infiltration of CD8+ T cells and CD19+ B cells within the metastatic tumor foci (Fig. 5M and Supplementary Fig. 23), correlating with their superior tumor suppression.
Taken together, these data demonstrate that oral immunization with BacOR-Fn-T+phiX174 elicits a powerful multi-faceted immune response—activating cytotoxic T cells, helper T cells, B cells, and proinflammatory innate cells while reducing Treg cells—which drives effective suppression of melanoma lung metastases.
Antitumor efficacy of Bac OR-Fn-T+phiX174 oral vaccine in a subcutaneous melanoma model
To further validate the therapeutic potential of BacOR-Fn-T+phiX174, we tested it in a subcutaneous B16-F10-OVA melanoma model and compared its efficacy to a conventionally injected vaccine. Mice bearing established subcutaneous tumors were orally immunized on days 0, 3, and 7 after tumor inoculation with the same formulations as above (G1–G5). Group G6 received subcutaneous injections of OVA and TRP2 peptides adjuvanted with Poly(I:C) (a TLR3 agonist), which served as a positive control for potent systemic immunization (Fig. 6A). Tumor growth was monitored every two days, and tumors were collected on day 16 for analysis.
A Experimental timeline. B Representative tumor images on day 16. Scale bar = 1 cm. C Tumor volume growth curves (n = 5 mice per group). D Tumor inhibition rate calculated based on the tumor volume on day 16 (n = 5 mice per group). E Tumor weight at endpoint (n = 5 mice per group). F Mouse body weight over time (n = 5 mice per group). G–J Flow cytometry quantification of tumor-infiltrating immune cells: CTLs (CD3+CD8+ cells, G), T helper cells (CD3+CD4+ cells, H), B cells (CD19+ in CD45+, I), mature DCs (CD80+CD86+ in CD11c+, J) (n = 3 mice per group). K Representative immunofluorescence staining images of CD8+ T cells (yellow, white arrow indication) and CD19+ B cells (red) in the colon sections. The nucleus was stained with DAPI (blue). Scale bar = 50 µm. Data are shown as mean ± SD; analyzed by one-way ANOVA with a Sidak’s multiple comparisons test. Source data are provided as a Source Data file.
Oral vaccination with the BacOR-Fn-T+phiX174 platform again resulted in significant tumor inhibition, in agreement with the metastasis model findings. Mice receiving the dual-antigen oral vaccine (G5) displayed markedly slower tumor growth and smaller final tumor sizes compared to those receiving single-antigen oral vaccines or PBS. By the end of the study, the mean tumor volume in the G5 group was approximately one-fourth of that in the PBS group, corresponding to ~75% tumor growth inhibition (Fig. 6B–D). The average tumor weight at harvest was also lowest in G5, underscoring the superior anti-tumor effect of the polyvalent vaccine (Fig. 6E). In contrast, the monovalent ferritin vaccine groups (G3 and G4) showed only modest tumor suppression (Fig. 6B), and the RGD-only bacterial vector (G2) had no significant effect on tumor growth. Notably, the therapeutic efficacy of the oral BacOR-Fn-T+phiX174 vaccine approached that of the subcutaneous peptide vaccine: tumor volumes and weights in G5 were similar to those in the Poly(I:C)+peptides group (G6) by day 16, indicating that oral delivery can achieve a potent anti-tumor response comparable to a traditional adjuvanted vaccine. Throughout the treatment, none of the vaccine regimens caused significant body weight changes (Fig. 6F), and histological examination of major organs revealed no evidence of toxicity (Supplementary Fig. 24), demonstrating the safety of the oral ferritin vaccine.
To confirm that the oral vaccine activates anti-tumor immunity at the tumor site, we analyzed immune cell infiltration in the tumors by flow cytometry and immunofluorescence. Consistent with its strong efficacy, the BacOR-Fn-T+phiX174 oral vaccine induced a highly inflamed tumor microenvironment. Mice in the G5 group had the highest intratumoral frequencies of CD8+ CD3+ cytotoxic T cells among all orally treated groups (Fig. 6G and Supplementary Fig. 25), along with significantly elevated CD4+CD3+ T helper cells (Fig. 6H and Supplementary Fig. 26) and CD19+CD45+ B cells (Fig. 6I and Supplementary Fig. 27) within the tumor tissue. The proportion of mature phenotype CD80+CD86+CD11c+ dendritic cells was also increased in G5 tumors (Fig. 6J and Supplementary Fig. 28), indicating local activation of antigen-presenting cells. Moreover, we observed a higher presence of M1-like proinflammatory macrophages (F4/80+CD80+ cells) in the tumors of G5-treated mice (Supplementary Fig. 29). These immune changes were significantly less pronounced in tumors from G3 or G4 mice, correlating with their inferior tumor suppression. Impressively, when compared to the potent injected vaccine (G6), the oral BacOR-Fn-T+phiX174 vaccine achieved comparable levels of intratumoral CTLs and mature DCs. Interestingly, G5 induced even higher levels of tumor-infiltrating CD19+CD45+ B cells and CD4+CD3+ T cells than the Poly(I:C) + peptide vaccine (G6), consistent with the robust humoral and helper T cell activation observed in oral vaccination. Immunofluorescence staining of colon tissue on day 16 showed significantly increased infiltration of CD19+ B cells and CD3+ T cells in the intestinal mucosa of BacOR-Fn-T+phiX174–treated mice compared to PBS controls (Fig. 6K). This indicates that oral delivery not only triggers systemic anti-tumor immunity but also stimulates local mucosal immune responses, which may contribute to the overall therapeutic effect. Together, the subcutaneous tumor results demonstrate that the BacOR-Fn-T+phiX174 oral vaccine can significantly inhibit tumor growth and modulate the tumor microenvironment, achieving therapeutic outcomes comparable to conventional systemic vaccination strategies.
Systemic and mucosal safety evaluation of Bac OR-Fn-T+phiX174 oral vaccine
To thoroughly evaluate the biosafety of the BacOR-Fn-T+phiX174 oral vaccine, we conducted two complementary safety assessments: a systemic toxicity test in healthy mice and a mucosal safety study in tumor-bearing mice. These experiments respectively addressed potential off-target effects at the organismal and local intestinal levels.
For systemic safety assessment, healthy mice were orally administered BacOR-Fn-T+phiX174 with arabinose using the therapeutic dosing schedule of lung metastasis model (Supplementary Fig. 30A). Throughout the observation period, mice maintained stable body weight, and histopathological analysis revealed no signs of tissue injury or inflammation in major organs, including the liver, kidney, heart, lung, and intestine (Supplementary Fig. 30B, C). Moreover, serum biochemical indicators of liver (ALT, AST), kidney (Urea, creatinine), and cardiac function (CK-MB) remained within normal physiological ranges (Supplementary Fig. 30D–H). Although ALT and CREA analysis showed significant differences between oral vaccine–treated mice (G5) and PBS controls, these values still fell within the normal physiological range and did not reflect pathological changes, suggesting that they are attributable to inter-individual variability rather than toxicity. In addition, LDH results showed that mice treated with BacOR-Fn-T+phiX174 were indistinguishable from PBS-treated controls (Supplementary Fig. 30I). These data confirm that the oral vaccine does not elicit systemic toxicity or organ-level adverse effects under repeated administration.
We next assessed the mucosal safety of the oral vaccine during tumor therapy. An important consideration for live oral vaccines is their potential to disturb gut homeostasis. Although our data showed that the engineered bacteria are rapidly cleared from the GI tract, we conducted dedicated studies to evaluate any subtle adverse effects on the intestinal tissue or microbiota. This evaluation was conducted using mice bearing subcutaneous B16-F10-OVA tumors, which received the vaccine orally following the immunization schedule detailed in Fig. 7A. Importantly, this safety study was integrated into the therapeutic protocol to more accurately reflect vaccine behavior under pathological conditions. On day 16, colons were collected for structural and histological analysis. The vaccine did not cause signs of mucosal injury or inflammation: colon length and weight-to-length ratio remained normal, and were comparable to those in PBS-treated mice (Fig. 7B-D). Hematoxylin and eosin staining of colon sections showed intact mucosal architecture without epithelial erosion, ulceration, or inflammatory cell infiltration (Fig. 7E). These results indicate that BacOR-Fn-T+phiX174 does not induce physical damage to the GI tract, even in tumor-bearing hosts.
A Experimental timeline. B Representative colon images. C, D Colon length and weight/length ratio (n = 3 mice per group). Data shown as mean ± SD. E H&E images of colon tissues. Scale bars: 200 µm (upper), 50 µm (lower). F Evaluation of microbial community observed OTU (operational taxonomic unit) richness of feces from mice treated with PBS or BacOR-Fn-T+phiX174 oral vaccine (n = 5 mice per group). Data are shown as mean ± SD; p values are determined with a two-tailed unpaired Student’s t-test. G, H Principal component analysis (PCA) plot and H nonmetric multidimensional scaling (NMDS) plot illustrating the β-diversity of the intestinal microbiome, each point corresponds to one mouse based on a sample of OTUs (n = 5 mice per group). I Venn diagram of genus-level bacterial richness. J Changes in the relative abundance of intestinal microbiota in the top 30 genera (n = 5 biologically independent samples). Data shown as mean ± SD. Source data are provided as a Source Data file.
To further evaluate the effect of oral vaccination on gut microbiota composition, 16S rRNA gene sequencing of fecal samples was performed. Alpha diversity metrics showed that microbial richness and evenness were preserved following vaccination, with comparable operational taxonomic unit (OTU) counts between BacOR-Fn-T+phiX174–treated and control groups (Fig. 7F). However, some shifts in community structure were noted on principal component analysis (Fig. 7G) and non-metric multidimensional scaling (NMDS) plots (Fig. 7H), suggesting that the bacterial composition in vaccinated mice diverged modestly from that of controls. Interestingly, BacOR-Fn-T+phiX174–treated mice showed an increase in microbial richness at the genus level (Fig. 7I), including a notable enrichment of Ligilactobacillus species compared to PBS mice (Fig. 7J). Members of the genus Ligilactobacillus are known to produce short-chain fatty acids that support intestinal homeostasis30. The expansion of such potentially beneficial commensals implies that the oral vaccine did not induce dysbiosis; on the contrary, it may have promoted a gut microbiota profile associated with gut health.
A potential biosafety concern for live bacterial vaccines is horizontal gene transfer (HGT) of engineered elements to commensal microbes. Our system incorporates several features that minimize this risk. The plasmids used (pET22b and pBAD33) lack mobilization genes (tra/mob) or an oriT site, and the E. coli Rosetta (DE3) host strain is not naturally competent in the mammalian gut31. In addition, arabinose-induced lysis ensures rapid clearance of the bacteria in vivo, with virtually no viable cells detected after 72 h. This short persistence window, combined with the absence of antibiotic selection pressure in vivo, substantially reduces the likelihood of genetic exchange. While the risk of HGT is therefore expected to be extremely low, future refinements such as chromosomal integration of antigen genes or self-destruct DNA degradation modules could provide additional safety assurance for clinical translation.
Collectively, our combined safety analyses demonstrate that BacOR-Fn-T+phiX174 is well tolerated at both systemic and mucosal levels, exhibiting no signs of organ toxicity, intestinal damage, or microbiota disruption in either healthy or tumor-bearing hosts. These findings support the vaccine’s safety for oral administration and provide a solid foundation for its translational potential.
Immune responses and long-term immune memory induced by Bac OR-Fn-T+phiX174 oral vaccination
We finally examined the ability of the oral vaccine to induce durable adaptive immune responses, including antibody production and T-cell memory, that could provide long-term protection against tumors. Healthy mice were orally immunized three times (days 0, 3, and 7) with the various ferritin-expressing bacteria (G1–G5 as defined above). Serum was collected on days 14, 21, and 28 to measure antigen-specific IgG, and a tumor re-challenge was performed later to assess protective immunity (Fig. 8A). The polyvalent BacOR-Fn-T+phiX174 vaccine elicited remarkably high antibody titers against both TRP2 and OVA, far exceeding the titers in mice receiving single-antigen vaccines or PBS. By day 28, the G5 group showed the highest levels of anti-TRP2 IgG and anti-OVA IgG in circulation (Fig. 8B, C), indicating that oral delivery of the dual-antigen ferritin effectively engages the humoral immune system. Mice immunized with monovalent ferritin constructs generated antibodies primarily against their respective single antigen—BacTR-Fn (G3) induced a moderate anti-TRP2 IgG response, and BacOR-Fn (G4) induced anti-OVA IgG production—but these antibody titers were significantly lower than those achieved by the dual-antigen vaccine (G5). This trend aligns with our tumor studies, where the monovalent vaccines afforded only partial tumor protection, while the bivalent BacOR-Fn-T+phiX174 vaccine provoked a much stronger immune defense.
A Schematic of long-term immunity assessment. B, C TRP2- and OVA-specific serum IgG levels at different timepoints after three oral vaccinations detected by ELISA assay (n = 3 mice per group). D Flow cytometry plots of CD8+ memory T cells in spleens at day 50. E, F Quantification of effector (CD3+CD8+CD44+CD62−) (E) and central (CD3+CD8+CD44+CD62+) (F) memory T cells (n = 3 mice per group) in spleens at day 50. G Schematic and results of tumor rechallenge on day 50; metastatic nodules were quantified on day 65. Data are shown as mean ± SD; analyzed by one-way ANOVA with a Sidak’s multiple comparisons test. Source data are provided as a Source Data file.
To determine if the immune responses from BacOR-Fn-T+phiX174 vaccination were long-lived, we evaluated immunological memory at a later time point. On day 50 (six weeks after the initial immunization), half of the mice in each group were sacrificed to analyze memory T-cell subsets, and the remaining mice were intravenously challenged with B16-F10-OVA tumor cells to test protective immunity. Flow cytometric analysis of splenocytes on day 50 revealed that BacOR-Fn-T+phiX174–vaccinated mice had significantly higher proportions of CD8+ memory T cells compared to all other groups (Fig. 8D–F). Both the effector memory subset (CD3+CD8+CD44+CD62L−) and the central memory subset (CD3+CD8+CD44+CD62L+) were enriched in the G5 group, indicating that the oral vaccine established a strong reservoir of long-lived CD8+ T cells poised to respond to tumor antigen re-exposure. Correspondingly, when the remaining immunized mice were challenged with B16-F10-OVA tumor cells on day 50, the BacOR-Fn-T+phiX174 group showed the most effective protection against tumor growth. At 15 days post-challenge (day 65), mice that had received BacOR-Fn-T+phiX174 oral vaccine displayed the lowest number of lung metastatic nodules among all groups (Fig. 8G and Supplementary Fig. 31), demonstrating a pronounced protective effect attributable to the vaccine-induced immunity. In contrast, control mice developed a heavy metastatic tumor burden, and those immunized with single-antigen vaccines showed only partial protection. These results confirm that the immune responses raised by BacOR-Fn-T+phiX174 vaccination are not only robust but also durable, providing immunity that can significantly prevent tumor recurrence.
Encouragingly, we observed a similar immunogenic profile in a larger animal model (Supplementary Fig. 32A), suggesting the translational potential of this oral vaccine strategy. Rabbits that were orally immunized with BacOR-Fn-T+phiX174 developed high titers of antibodies against both OVA and TRP2, whereas rabbits receiving single-antigen ferritin vaccines generated strong antibody responses only to the corresponding single antigen (Supplementary Fig. 32B, C). The dual-antigen ferritin elicited the highest IgG levels to both targets, mirroring the trend seen in mice. This cross-species result indicates that the BacOR-Fn-T+phiX174 oral vaccine can effectively induce antigen-specific immunity in a non-murine model, highlighting the promise of this platform for broader application.
With the rapid advancement of immunology and synthetic biology, engineered bacteria such as E.coli, Salmonella have emerged as promising vaccine vectors32,33,34,35, due to their natural tumor-targeting capacity, ability to produce antigens in situ, and potential to modulate immune responses36. Despite these advantages, the clinical translation of bacteria-based vaccines has been limited by biosafety concerns, instability in the GI tract, and insufficient immunogenicity.
In this study, we developed BacOR-Fn-T+phiX174, a system that integrates genetically encoded dual-antigen ferritin arrays with arabinose-inducible bacterial lysis to address these limitations. Unlike previously reported probiotic vaccine systems, which often rely on single-antigen delivery and lack control over release kinetics37, our design ensures stable expression of structurally defined antigen nanoparticles and enables on-demand intestinal release. Moreover, compared with peptide vaccines or immune checkpoint blockade therapies—which may suffer from weak immunogenicity or immune-related toxicities38,39—our oral system targets the GALT, the largest immune organ, in a non-invasive manner. This approach not only improves safety and patient compliance but also provides clear advantages in accessibility and cost-effectiveness.
The antigen design further strengthens this platform. In our construct, the antigen OVA257–264 (a CD8+ T-cell epitope), OVA323–339 (a CD4+ T-cell epitope), and tyrosinase-related protein 2 (TRP2180–188), were fused to ferritin to generate a dual-antigen functional ferritin nanoparticle. As TRP2 was a representative antigen and OVA was a model antigen in the B16-F10-OVA melanoma model40,41. Treatment experiments demonstrated that the oral vaccine expressing dual-antigen ferritin elicited significantly stronger anti-tumor effects than the oral vaccine expressing single-antigen ferritin. These results highlight the potential of ferritin as a versatile platform for multi-epitope vaccine design, adaptable to diverse tumor types and clinical requirements.
Another key feature of our system is the use of L-arabinose, a natural dietary sugar, as an external inducer of bacterial lysis. L-arabinose not only provides a safe and easily administered trigger but has also been reported to beneficially modulate gut microbiota and strengthen intestinal barrier integrity in animal studies42,43,44. Incorporating such a benign inducer enables precise temporal control over antigen release while minimizing risks associated with uncontrolled bacterial persistence. Collectively, these features highlight the translational potential of BacOR-Fn-T+phiX174 as a safe, effective, and readily applicable oral cancer vaccine strategy.
In summary, we have developed a ferritin-based oral cancer vaccine that successfully navigates the challenges of the GI tract and induces a potent anti-tumor immune response. Through rational design—incorporating controlled bacterial lysis, M-cell targeting, and multivalent antigen presentation—our oral vaccine achieved strong activation of both mucosal and systemic immunity, leading to significant therapeutic effects against melanoma in mice. It also established immunological memory and exhibited an excellent safety profile. These findings highlight a promising avenue for oral immunotherapy: using engineered microbial factories to deploy nanoscopic antigen carriers at mucosal surfaces. With further optimization and testing, this strategy could be translated into next-generation cancer vaccines that are effective, needle-free, and easily administered, potentially transforming prophylactic and therapeutic vaccination in oncology.
Methods
Materials
RPMI 1640 (A4192301) medium, MEM (11095080), and FBS (A5256701) were obtained from Thermo Scientific. Trypsin-EDTA solution (T1300), L-Arabinose (L8060), and RIPA lysis buffer (R0010) were purchased from Solarbio Life Science. Simulated Intestinal Fluid (SIF, MSI9835) and Simulated Gastric Fluid (SGF, MSG0250) were purchased from MesGen Biotech. D-Luciferin potassium salt (L120798) was purchased from Aladdin Biochemical Technology. HA Tag Monoclonal Antibody (26183), c-Myc Monoclonal Antibody (MA1-980), and DYKDDDDK Tag Monoclonal Antibody (MA1-91878) were obtained from Thermo Scientific. HRP-conjugated Goat anti-Mouse IgG (AS003) and HRP-conjugated Goat anti-Rabbit IgG (AS014) were purchased from ABclonal Technology. APC anti-mouse CD11c (117310), FITC anti-mouse CD80 (104706), PE/Cy7 anti-mouse CD86 (159208), APC anti-mouse CD3 (100236), FITC-anti-mouse CD8α (100705), PE anti-mouse CD8α (100707), PE-anti-mouse CD4 (100408), PerCP/Cyanine5.5 anti-mouse IFN-γ (505821), APC anti-mouse CD19 (152409), APC anti-mouse F4/80 (123115), APC/Cy7 anti-mouse CD25 (101917), PE-anti-mouse CD44 (103008) and PE/Cy7-anti-mouse CD62L (104418) were purchased from BioLegend. H-2Kb OVA Tetramer-SIINFEKL-BV421 (TS-5001-4C) antibody was purchased from MBL Life Science. The mouse IFN-γ ELISpot kit (2210005) was obtained from Dakewe Biotech Company. Mouse Ovalbumin-specific IgG antibody (OVA-sIgG) ELISA kit (ml063584) and mouse Tyrosinase-related protein-2 ELISA Kit(ml037813) were purchased from Mlbio Biotechnology. OVA257–264 (SIINFEKL), OVA323–339 (ISQAVHAAHAEINEAGR), and TRP2180–188(SVYDFFVWL) were synthesized by Top Peptide (Shanghai, China).
Animals and cell lines
Female C57BL/6J (6–8-weeks-old) were obtained from SPF Biotechnology. Big-eared white rabbits were purchased from Songlin Farm, Zhengzhou, China. The animal studies were conducted in accordance with the ethical standards set by the Animal Ethics Committee of Zhengzhou University (approval number: GIR 2023-1407). All mice were group-housed (five mice per cage) in a specific pathogen-free (SPF) facility under controlled temperature (22–26 °C) and humidity (40–70%) conditions, with a 12 h light/12 h dark cycle. DC2.4 cells were obtained from Fenghui Biotechnology. B16-F10-OVA murine melanoma cells were generously provided by P. Zhao Xiao at the National Center for Nanoscience and Technology. Raji Burkitt’s lymphoma cells and Caco-2 cells were obtained from Wuhan Procell Life Science & Technology Co., Ltd. B16-F10-OVA and Raji cells were grown in RPMI-1640 medium with 10% FBS and 100 μg/mL penicillin/streptomycin. DC2.4 cells were grown in RPMI-1640 medium with 10% FBS, 10 ng/mL murine GM-CSF, and 100 μg/mL penicillin/streptomycin. Caco-2 cells were grown in MEM medium with 20% FBS and 100 μg/mL penicillin/streptomycin. Cells were cultured at 37 °C in a humidified atmosphere containing 5% CO2.
Plasmid construction and bacterial engineering
The genes encoding OR-Fn-T, OR-Fn, TR-Fn, O-Fn-T, and R-Fn were cloned into pET22b, respectively, to construct different functional ferritin plasmids (Genewiz, Suzhou, China). The genes PhiX174 or luciferase were cloned into the pBAD33 vector to construct a lysis or fluorescence plasmid (Genewiz, Suzhou, China). The ferritin plasmid was co-transformed with the lysis or fluorescence plasmid into Escherichia coli Transetta (DE3) to obtain bacterial vaccines. The engineered bacteria were inoculated into LB medium including ampicillin (60 μg/mL) and chloramphenicol (50 μg/mL) at 37 °C. When the OD600 of engineered bacteria reached 0.6–0.8, isopropyl-β-D-thiogalactoside (IPTG, Sigma) (1 mM) was added to induce fusion ferritin expression. All plasmids and bacterial strains generated in this study are available from the corresponding author upon request.
Purification and characterization of ferritin constructs
The engineered bacteria were harvested by 3300×g centrifugation for 20 min, and the pellets were resuspended in Tris buffer (20 mM Tris, pH 8.0). The resuspended E. coli cells were centrifuged at 13,800×g at 4 °C for 30 min. The supernatant was further heated to 80 °C to denature and remove most of the excess proteins. Ferritins were purified via ion-exchange chromatography (Q-Sepharose) and size-exclusion chromatography (Superdex 200). Hydrodynamic size and zeta potential were measured using DLS (Malvern). Morphology was confirmed by TEM (Talos L120CG2).
Western blot analysis of the release of OR-Fn-T by Bac OR-Fn-T+phiX174
BacOR-Fn-T+phiX174 were cultured in LB medium and induced with 1 mM IPTG at 30 °C for 8 h when OD600 reached 0.6–0.8. BacOR-Fn-T+phiX174 were centrifuged at 5000×g for 10 min, and the pellets were then suspended in LB medium containing 2 mg/mL arabinose and cultured at 37 °C with shaking (180 rpm). After different times of induction of arabinose (2, 4, and 6 h), the culture supernatant was collected, and the OR-Fn-T released in the supernatant was evaluated by western blot analysis. Samples were treated in a loading buffer with heating at 100 °C for 10 min and then resolved by SDS-PAGE. The targeted proteins OR-Fn-T were detected by WB analysis using an antibody against the HA tag (26183, Thermo Scientific).
Validation of the lysis efficiency of engineered bacteria
BacOR-Fn-T+phiX174 were cultured in LB medium, SGF, and SIF solution with or without Ara (2 mg/mL), respectively. The OD600 absorbance values of bacteria were monitored at preset time points (0, 1, 2, 3, 4, and 6 h), and the morphology of bacteria at 6 h after incubation was observed using SEM.
To further simulate the digestive tract environment, 5 mL of BacOR-Fn-T+phiX174 was added to 20 mL SGF solution with or without arabinose (2 mg/mL) and cultured for 0.5 h. After centrifugation, the bacterial pellets were briefly transferred into LB medium to remove residual SGF and then cultured in SIF for 5.5 h, with or without arabinose. OD600 of BacOR-Fn-T+phiX174 after incubation in SGF and SIF was measured.
The distribution and excretion of Bac OR-Fn-T+Luc in the digestive tract
To verify the expression of luciferase in vitro, BacOR-Fn-T+Luc were induced with arabinose and re-suspended in PBS including D-Luciferin potassium salt (15 mg/mL) for fluorescence imaging.
To analyze the distribution of BacOR-Fn-T+Luc in vivo, C57BL/6 J mice were orally administered BacOR-Fn-T+Luc (108 cells per mouse) and arabinose water (20 mg/mL). The digestive tract tissues of mice were excised at 1, 2, 4, and 6 h for fluorescence imaging. In addition, 20 mg of the contents from different parts of the digestive tract were collected and suspended in D-Luciferin potassium salt (15 mg/mL) solution to analyze fluorescence intensity. The arabinose concentration in the colon was measured by high-performance liquid chromatography (HPLC). Briefly, after oral administration of arabinose for 6 h, approximately 4 cm of the mouse colon was collected and lavaged with 1 mL of PBS. The lavage solution was collected for arabinose concentration detection.
The release of OR-Fn-T by BacOR-Fn-T+phiX174 in vivo was evaluated by GPC analysis. C57BL/6J mice were oral administration of BacOR-Fn-T+phiX174 (108 cells per mouse) and arabinose (20 mg/mL). The colon tissues were collected at 4 h and 6 h, respectively, and flushed using PBS. The colon flushing fluid was analyzed by GPC, and isolated OR-Fn-T was used as a standard sample.
For the excretion of BacOR-Fn-T+phiX174, C57BL/6J mice were orally administered BacOR-Fn-T-phiX174 cells (108 cells per mouse) and 20 mg/mL arabinose water. Fresh feces of mice were collected at different times and spread on solid agar plates for colony count.
Transwell and colon loop assays
The simulated intestinal epithelial barrier model containing M cells was constructed according to the previous report23. Briefly, 5.0 × 105 of Caco-2 cells suspended in MEM were seeded on the apical side of Transwell inserts and cultured for 14 days. Then, 5.0 × 105 of Raji B cells suspended in RPMI 1640 were added and co-cultured for another 6 days. In addition, a control Caco-2 monolayer without Raji B cells was constructed by culturing Caco-2 cells for 20 days. DC2.4 cells were cultured on the bottom side and then FITC-labeled OR-Fn-T, O-Fn-T, and R-Fn were added to the apical side and incubated for 48 h. The uptake of ferritins by DC2.4 cells and the proportion of mature DC2.4 cells were detected by flow cytometry. The total fluorescence intensity of ferritin in the basolateral chamber was analyzed by measuring the cell suspension using a multimode plate reader.
To further explore the ability of ferritin to penetrate the colonic epithelial barrier of mice, the colon (about 1 cm) was resected and incubated in FITC-labeled ferritin solution (2 mg/mL) for 2 h. After washing with PBS, colons were collected for further immunofluorescence analysis.
Lamina propria DC maturation assay
Mice were orally administered with PBS, BacR-Fn+phiX174, BacO-Fn-T+phiX174, or BacOR-Fn-T+phiX174 (108 cells per mouse) and were provided 20 mg/mL arabinose. After 24 h, mice were euthanized, and the colons were collected to isolate the lamina propria lymphocytes. The proportion of mature DCs (CD11c+CD80+CD86+) was analyzed using flow cytometry.
Lung metastasis melanoma model
C57BL/6 mice were injected with murine B16-F10-OVA melanoma cells (2 × 105 cells) via the tail vein on day 0. The mice were orally administered PBS, OR-Fn-T, BacR-Fn-phiX174, BacTR-Fn-phiX174, BacOR-Fn-phiX174, or BacOR-Fn-T-phiX174 (108cells per mouse) on days 3, 7, and 14 and were provided 20 mg/mL arabinose solution. The mice were euthanized on day 17, and the lungs and spleens were collected for further analysis. The number of pulmonary tumor metastases was counted, and lungs were fixed with 4% paraformaldehyde for CD8 and CD19 immunohistochemical staining.
The spleen tissues were ground into a single-cell suspension. T lymphocytes, B cells, and macrophages in splenocytes were analyzed by flow cytometry. In addition, splenocytes were seeded in a 96-well plate (105 cells per well) and incubated with OVA and TRP2 peptide for 24 h. The secretion of IFN-γ was detected using an IFN-γ ELISpot kit.
The blood samples were collected at the end of the treatment experiment. The OVA-specific IgG concentration and anti-TRP2-specific IgG concentration in serum were determined by ELISA kits.
Subcutaneous tumor model
The 1 × 106 murine B16-F10-OVA melanoma cells were injected subcutaneously into the right flank of C57BL/6 mice. Ten days after inoculation with the tumor cells, the mice were randomly divided into six experimental groups and were orally administered with PBS, BacR-Fn+phiX174, BacTR-Fn+phiX174, BacOR-Fn+phiX174, or BacOR-Fn-T+phiX174 on days 0, 3, and 7. Mice were provided with 20 mg/mL arabinose water after each vaccination. Mice subcutaneously immunized with a mixture of 50 µg adjuvant Poly(I:C) + 50 µg OVA + 50 µg TRP2 were used as a positive control group. The tumor volume was calculated every other day according to the following formula: (width2 × length)/2. The mice were weighed every other day during the study as a measurement of toxicity. The mice were euthanized on day 16, and tumors were excised, weighed, and digested into single-cell suspensions to detect the infiltrating immune cells using flow cytometry.
Systemic and mucosal safety evaluation of Bac OR-Fn-T+phiX174 oral vaccine
For systemic safety, healthy mice were treated orally with PBS or different bacterial vaccines (BacR-Fn+phiX174, BacTR-Fn+phiX174, BacOR-Fn+phiX174, or BacOR-Fn-T+phiX174) on day 0, 4, and 11. Mice were euthanized on day 18. The body weight of mice was monitored every other day. On day 18, the main organs of mice (heart, liver, spleen, lung, kidney, and colon) were collected for pathological analysis, and blood was collected for blood biochemical analysis.
At the end of the treatment of subcutaneous tumors, the colons were collected to measure length and weight. The major organs (heart, liver, lung, spleen, and kidney) and colons were harvested for H&E staining. Fecal samples of mice treated with PBS or BacOR-Fn-T-phiX174 were collected for intestinal microbiota analysis with the assistance of Majorbio Bio-Phar Technology Co., Ltd. (Shanghai, China).
Long-term immune memory
C57BL/6J mice were orally administered PBS, BacR-Fn+phiX174, BacTR-Fn+phiX174, BacOR-Fn+phiX174, or BacOR-Fn-T+phiX174 engineered bacteria (108cells per mouse) on days 0, 3, and 7, and were provided 20 mg/mL Ara solution after each vaccination. Blood samples were collected on days 14, 21, and 28. The concentrations of anti-TRP2 IgG and anti-OVA IgG in serum were quantified by the ELISA method according to the manufacturer’s protocols.
To analyze immune memory, splenocytes were collected from the vaccinated mice at day 50 and analyzed using flow cytometry. In addition, other vaccinated mice were injected intravenously with B16-F10-OVA melanoma cells (2 × 105 cells) on day 50 and sacrificed on day 65. The lungs were collected to analyze the lung metastases.
Rabbit immunization
Healthy big-eared white rabbits (2.5 ± 0.5 kg weight, both sexes) were individually caged and kept in a controlled temperature at 25 ± 2 °C with food and water provided ad libitum. Rabbits were orally administered PBS, BacR-Fn+phiX174, BacTR-Fn+phiX174, BacOR-Fn+phiX174, or BacOR-Fn-T+phiX174 (108 cells per rabbit) on days 0, 3, and 7 and were provided 20 mg/mL arabinose solution after each vaccination. Blood was collected through the auricular vein on days 14, 21, and 28, respectively. Anti-OVA-specific IgG titer and anti-TRP2-specific IgG titer in serum were determined by ELISA according to the manufacturer’s protocol (Mlbio Biotechnology). Antibody titers were calculated based on reciprocal serum dilution, giving O.D. values > 2 × background.
Statistical analysis
The data are presented as mean ± standard deviation (SD). Differences between the two groups were analyzed by a two-tailed unpaired Student’s t-test. A one-way analysis of variance (ANOVA) with Sidak’s multiple comparisons test was used for multiple comparisons by GraphPad Prism software. In the microscope and western blot experiments, three independent experiments were performed, and representative images were shown.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
Data supporting the findings of this work are available within the paper and its Supplementary Information files. Source data are available for Figs. 2–8 and Supplementary Figs. 2, 3, 5, 7, 8, 9, 10, 14, 22, 29, 30, and 32 in the associated source data file. Source data are provided with this paper.
References
Saxena, M., van der Burg, S. H., Melief, C. J. M. & Bhardwaj, N. Therapeutic cancer vaccines. Nat. Rev. Cancer 21, 360–378 (2021).
Chen, D. S. & Mellman, I. Oncology meets immunology: the cancer-immunity cycle. Immunity 39, 1–10 (2013).
Kantoff, P. W. et al. Sipuleucel-T immunotherapy for castration-resistant prostate cancer. N. Engl. J. Med. 363, 411–422 (2010).
Mitragotri, S. Immunization without needles. Nat. Rev. Immunol. 5, 905–916 (2005).
Amorij, J. P., Hinrichs, W., Frijlink, H. W., Wilschut, J. C. & Huckriede, A. Needle-free influenza vaccination. Lancet Infect. Dis. 10, 699–711 (2010).
Giudice, E. L. & Campbell, J. D. Needle-free vaccine delivery. Adv. Drug Deliv. Rev. 58, 68–89 (2006).
Kwong, K. W. et al. Oral vaccines: a better future of immunization. Vaccines 11, 1232 (2023).
Zafar, A., Arshad, R., Ur Rehman, A., Ahmed, N. & Akhtar, H. Recent developments in oral delivery of vaccines using nanocarriers. Vaccines 11, 490 (2023).
Wang, S., Liu, H., Zhang, X. & Qian, F. Intranasal and oral vaccination with protein-based antigens: advantages, challenges and formulation strategies. Protein Cell 6, 480–503 (2015).
Lycke, N. Recent progress in mucosal vaccine development: potential and limitations. Nat. Rev. Immunol. 12, 592–605 (2012).
Yun, Y., Cho, Y. W. & Park, K. Nanoparticles for oral delivery: targeted nanoparticles with peptidic ligands for oral protein delivery. Adv. Drug Deliv. Rev. 65, 822–832 (2013).
Zhang, Y. et al. A programmable oral bacterial hydrogel for controllable production and release of nanovaccine for tumor immunotherapy. Biomaterials 299, 122147 (2023).
Zhang, S., Langer, R. & Traverso, G. Nanoparticulate drug delivery systems targeting inflammation for treatment of inflammatory bowel disease. Nano Today 16, 82–96 (2017).
Lee, Y., Kamada, N. & Moon, J. J. Oral nanomedicine for modulating immunity, intestinal barrier functions, and gut microbiome. Adv. Drug Deliv. Rev. 179, 114021 (2021).
Li, Z. et al. Chemically and biologically engineered bacteria-based delivery systems for emerging diagnosis and advanced therapy. Adv. Mater. 33, e2102580 (2021).
Lin, X., Jiao, R., Cui, H., Yan, X. & Zhang, K. Physiochemically and genetically engineered bacteria: instructive design principles and diverse applications. Adv. Sci. 11, e2403156 (2024).
Abreu, M. T. Toll-like receptor signalling in the intestinal epithelium: how bacterial recognition shapes intestinal function. Nat. Rev. Immunol. 10, 131–144 (2010).
Chowdhury, S. et al. Programmable bacteria induce durable tumor regression and systemic antitumor immunity. Nat. Med. 25, 1057–1063 (2019).
Zhu, J. et al. Engineered Lactococcus lactis secreting Flt3L and OX40 ligand for in situ vaccination-based cancer immunotherapy. Nat. Commun. 13, 7466 (2022).
Raman, V. et al. Intracellular delivery of protein drugs with an autonomously lysing bacterial system reduces tumor growth and metastases. Nat. Commun. 12, 6116 (2021).
Haddadzadegan, S., Dorkoosh, F. & Bernkop-Schnürch, A. Oral delivery of therapeutic peptides and proteins: technology landscape of lipid-based nanocarriers. Adv. Drug Deliv. Rev. 182, 114097 (2022).
Tyrer, P. C., Ruth Foxwell, A., Kyd, J. M., Otczyk, D. C. & Cripps, A. W. Receptor mediated targeting of M-cells. Vaccine 25, 3204–3209 (2007).
Shen, Y., Hu, Y. & Qiu, L. Nano-vesicles based on phospholipid-like amphiphilic polyphosphazenes to orally deliver ovalbumin antigen for evoking anti-tumor immune response. Acta Biomater. 106, 267–277 (2020).
Wang, W. et al. Dual-targeting nanoparticle vaccine elicits a therapeutic antibody response against chronic hepatitis B. Nat. Nanotechnol. 15, 406–416 (2020).
Ma, X. et al. Nanoparticle vaccines based on the receptor binding domain (RBD) and heptad repeat (HR) of SARS-CoV-2 elicit robust protective immune responses. Immunity 53, 1315–1330.e1319 (2020).
Foster, J. W. Escherichia coli acid resistance: tales of an amateur acidophile. Nat. Rev. Microbiol. 2, 898–907 (2004).
Yildirim, N. Mathematical modeling of the low and high affinity arabinose transport systems in Escherichia coli. Mol. Biosyst. 8, 1319–1324 (2012).
Cao, F. et al. Artificial-enzymes-armed Bifidobacterium longum probiotics for alleviating intestinal inflammation and microbiota dysbiosis. Nat. Nanotechnol. 18, 617–627 (2023).
Cao, S. J. et al. Nanoparticles: oral delivery for protein and peptide drugs. AAPS PharmSciTech 20, 190 (2019).
Sun, M. et al. Microbiota-derived short-chain fatty acids promote Th1 cell IL-10 production to maintain intestinal homeostasis. Nat. Commun. 9, 3555 (2018).
Murciano-Brea, J., Garcia-Montes, M., Geuna, S. & Herrera-Rincon, C. Gut microbiota and neuroplasticity. Cells 10, 2084 (2021).
Nguyen, D. H. et al. Reprogramming the tumor immune microenvironment using engineered dual-drug loaded Salmonella. Nat. Commun. 15, 6680 (2024).
Guo, L. et al. Surface engineering Salmonella with pH-responsive polyserotonin and self-activated DNAzyme for better microbial therapy of tumor. Exploration 3, 20230017 (2023).
Qiao, L. et al. Engineered bacteria for near-infrared light-inducible expression of cancer therapeutics. Nat. Cancer 6, 612–628 (2025).
Xu, K. F. et al. Hyperbaric oxygen enhances tumor penetration and accumulation of engineered bacteria for synergistic photothermal immunotherapy. Nat. Commun. 15, 5147 (2024).
Jia, J., Wang, X., Lin, X. & Zhao, Y. Engineered microorganisms for advancing tumor therapy. Adv. Mater. 36, e2313389 (2024).
Yue, Y. et al. Antigen-bearing outer membrane vesicles as tumour vaccines produced in situ by ingested genetically engineered bacteria. Nat. Biomed. Eng. 6, 898–909 (2022).
Peng, M. et al. Neoantigen vaccine: an emerging tumor immunotherapy. Mol. Cancer 18, 128 (2019).
Li, Z., Zhang, H., Gong, Q. & Luo, K. Biomaterials nanoplatform-based tumor vaccines for immunotherapy. Bioact. Mater. 51, 924–961 (2025).
Schreurs, M. W. et al. Dendritic cells break tolerance and induce protective immunity against a melanocyte differentiation antigen in an autologous melanoma model. Cancer Res. 60, 6995–7001 (2000).
Yang, Y. et al. Tumor vaccine exploiting membranes with influenza virus-induced immunogenic cell death to decorate polylactic coglycolic acid nanoparticles. ACS Nano 19, 3115–3134 (2025).
Xu, M. et al. Arabinose confers protection against intestinal injury by improving integrity of intestinal mucosal barrier. Int. Immunopharmacol. 126, 111188 (2024).
Li, X. et al. Antiobesity effect of L-arabinose via ameliorating insulin resistance and modulating gut microbiota in obese mice. Nutrition 111, 112041 (2023).
Krog-Mikkelsen, I. et al. The effects of L-arabinose on intestinal sucrase activity: dose-response studies in vitro and in humans. Am. J. Clin. Nutr. 94, 472–478 (2011).
Acknowledgements
This work was supported by the National Nature Science Foundation of China (Nos. 32301187, Y.Y. and 32000996, B.J.) and the Henan Province Excellent Youth Science Foundation (no. 252300421143, Y.Y.), the Key Program of Nanozyme Laboratory in Zhongyuan (NLZ-KP2024NIC02, B.J.), the Henan AIMS Professional Development Fund (JBKY250304, B.J.), and the Grant for International Joint Research Project of the Institute of Medical Science, the University of Tokyo (no. Extension-2019-K3005, X.Y.).
Author information
Authors and Affiliations
Contributions
Y.Y. and Q.X. contributed equally to this work. X.Y. and B.J. conceptualized and designed the project. Y.Y., Q.X., and Y.Z. performed the research. All authors analyzed and interpreted the data. B.J. and X.Y. supervised the project. Y.Y. and B.J. wrote the paper.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks Songping Zhang and Stéphane Paul for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Yue, Y., Xin, Q., Zhu, Y. et al. Probiotic-based oral vaccine mucosal delivery system enabling genetically encoded dual-antigen arrays. Nat Commun 16, 11540 (2025). https://doi.org/10.1038/s41467-025-66622-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-025-66622-x