Abstract
Existing guidelines on the preparation (Planning Research and Experimental Procedures on Animals: Recommendations for Excellence (PREPARE)) and reporting (Animal Research: Reporting of In Vivo Experiments (ARRIVE)) of animal experiments do not provide a clear and standardized approach for refinement during in vivo cancer studies, resulting in the publication of generic methodological sections that poorly reflect the attempts made at accurately monitoring different pathologies. Compliance with the 3Rs guidelines has mainly focused on reduction and replacement; however, refinement has been harder to implement. The Oncology Best-practices: Signs, Endpoints and Refinements for in Vivo Experiments (OBSERVE) guidelines are the result of a European initiative supported by EurOPDX and INFRAFRONTIER, and aim to facilitate the refinement of studies using in vivo cancer models by offering robust and practical recommendations on approaches to research scientists and animal care staff. We listed cancer-specific clinical signs as a reference point and from there developed sets of guidelines for a wide variety of rodent models, including genetically engineered models and patient derived xenografts. In this Consensus Statement, we systematically and comprehensively address refinement and monitoring approaches during the design and execution of murine cancer studies. We elaborate on the appropriate preparation of tumor-initiating biologicals and the refinement of tumor-implantation methods. We describe the clinical signs to monitor associated with tumor growth, the appropriate follow-up of animals tailored to varying clinical signs and humane endpoints, and an overview of severity assessment in relation to clinical signs, implantation method and tumor characteristics. The guidelines provide oncology researchers clear and robust guidance for the refinement of in vivo cancer models.
Similar content being viewed by others
Introduction
The term cancer comprises a heterogeneous group of complex pathologies that clinically present with different tumor (sub)types, stages and metastatic niches. Many cancers display diverse mechanisms of resistance, either intrinsically developed or acquired under therapeutic pressure. Fostered by emerging technologies, a substantial expansion of available treatment modalities contributed to a paradigm shift from one-size-fits-all toward precision oncology1,2,3,4. Taken together, this highlights the need for a diverse and well-characterized toolbox of preclinical models in the cancer research area. To reliably recapitulate a cancer patient, accurately study tumor biology and test the efficacy and safety of anticancer agents, a variety of in vitro and in vivo model systems have been generated.
Despite the availability of many nonanimal methods and ongoing efforts to further develop animal-free alternatives, the need for complex and heterogeneous animal models recapitulating various aspects of the disease of interest persists. This is clearly observed in the steady number of laboratory animals used across basic, translational and applied research worldwide and in the European Union (EU)5. Approximately 1 million mice were utilized in the EU in oncology research in 2019, representing one of the top four disciplines for animals used across basic and translational research applications (EU 2019 report5). Indeed, preclinical models are integral to the development of new treatment options3,6,7,8, investigating systemic metastasis9, exploring side effects or resistance upon demanding treatment regimens10,11 and studying the interplay between the tumor and its micro-environment12,13.
Reproducibility and replicability of experiments and results are often challenging in biomedical research14,15,16,17. As recently demonstrated by a large reproducibility study in preclinical cancer biology, only 46% of published results could be successfully reproduced18. Indeed, several ‘natural’ inescapable hurdles contribute to the limited reproducibility of preclinical findings including innate biological heterogeneity as well as the use of nonstandardized methods or materials. Moreover, poor study design, insufficient statistical power and lack of adherence to reporting standards contribute to bias and poor reproducibility. To maximize the likelihood of successful clinical translation, preclinical biomedical studies require stringent design. This should include appropriate research planning and proper study design, standardization of methods, protocols and disease models, and thorough and transparent reporting. Previous efforts to increase reproducibility have been made via the Planning Research and Experimental Procedures on Animals: Recommendations for Excellence (PREPARE) and Animal Research: Reporting of In Vivo Experiments (ARRIVE) guidelines. The PREPARE guidelines provide guidance on how to plan animal experiments that are reproducible and scientifically robust. In addition, PREPARE addresses animal welfare issues and provides resources for additional guidance on more specific topics19. The ARRIVE guidelines aim to improve the reporting of animal research by providing a checklist of information to include in publications describing in vivo experiments20,21. Thus, whereas the PREPARE guidelines19 provide guidance on how to plan animal experiments, the ARRIVE guidelines mainly focus on the proper reporting of animal experiments20,21. Despite the many topics covered in both comprehensive checklists, clear and standardized guidelines on the monitoring of animals during the experiment are rather scarce.
As highlighted in the EU Parliament in 2022, there is a tendency of the EU and its Member States to focus on reduction and replacement, whereas the third R, refinement, is under considered and lagging behind22. The 3Rs concept as originally described by Russell and Burch defined refinement as ‘any decrease in the incidence or severity of inhumane procedures applied to those animals which still have to be used’23. In addition, the 3Rs state that the ‘object of refinement is simply to reduce to an absolute minimum the amount of distress imposed on those animals that are still used’. In many cases, an additional definition is attributed to refinement as the reduction or elimination of distress and pain. In general, the ethical aim of humane use and care of animals in research is to spare them from all substantial unpleasant experiences not necessary for the purpose of research and to enhance animal well-being24.
With the inherent use of a large number of animals and a variety of animal models in oncology, there are numerous opportunities for refinement. Nevertheless, it is remarkable that practical guidelines on this topic are rather sparse. Publications remain either very general, providing only specific guidelines for the subcutaneous (SC) models25,26,27 or are highly specific for one particular model28,29,30,31,32,33,34,35. Therefore, in line with IMPROVE36— a guideline for in vivo ischemic models—the Oncology Best-practices: Signs, Endpoints and Refinements for in Vivo Experiments (OBSERVE) guidelines aim to bridge this gap, offering a comprehensive set of practical and specific recommendations on refinement in murine cancer models for scientists, veterinarians and animal care staff.
In addition to mice and rats, several other mammalian models are used in cancer research such as pigs, dogs and nonhuman primates, in addition to some nonmammalian models including drosophila and zebrafish2,37,38,39,40,41. The spontaneous canine, feline and nonhuman primate tumor models41,42,43,44 provide a unique platform for evaluating novel therapeutic regimens in the context of an intact immune system. Other, nonspontaneous models, however, require genetic modification45,46,47,48,49. Similar to murine models, genetic manipulation and transgenesis (e.g., clustered regularly interspaced short palindromic repeats (CRISPR)) is applied to generate severe combined immune-deficient animals for xenotransplantation studies50 or models that are capable of developing tumors in various organs51,52,53,54. Although some of the clinical signs in patients associated with a specific tumor type may be similar in other mammals, refinement during implantation, induction and importantly during tumor development may differ notably between species. Therefore, these guidelines focus on murine models and do not include other species, as broadening to other species would be beyond the expertise of the authors and European consortia involved in drafting the OBSERVE guidelines.
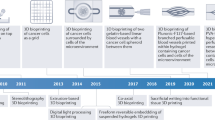
Commonly used murine model systems include patient-derived xenografts (PDX), cell line- or organoid-based xenografts, humanized mice and autochthonous models such as spontaneous, chemically induced or genetically engineered models (GEM) (Fig. 1). Whereas syngeneic cells can be transplanted into fully immunocompetent mice, xenogeneic human cells and allogeneic mouse cells must be transplanted into immunocompromised mice to avoid rejection by the host. Indeed, immune-deficient animals are more vulnerable to a variety of pathogens and opportunists and are thus best housed and manipulated in a specific pathogen-free environment. Immune competence therefore directly impacts and has practical consequences on design, preparation and execution of animal experiments.
a, A carcinogenic model: cancer model established in immunocompetent animals by applying a physical and/or chemical carcinogen(s) inducing genetic alterations causing tumor growth. b, A genetically engineered model: cancer model based on the genetic alteration of oncogenes or tumor suppressor genes or administration of exogenous activating agents for organ-specific tumor development. c, A syngeneic model and allogeneic model: engraftment of mouse or rat tumor cells or organoids in, respectively, a genetically identical, immune competent strain or a genetically different, immune deficient strain of the same species. Cell lines can be generated from a chemically induced or genetically engineered model. d, A xenograft model: xenograft in immune deficient animals of a cell line, a tissue piece or organoids generated from a cancer biopsy, usually from human origin. e, A humanized model: xenograft model in immunodeficient mice previously engrafted with human immune cells. CLX, cell line xenograft; PDX, patient-derived xenograft.
Irrespective of the immune status and the route of tumor induction, whether spontaneous or via orthotopic transplantation, the main signs of disease and adverse effects due to tumor development are likely to manifest in a similar manner. For example, ascites can be expected to develop in ovarian cancer models, whether human tumor fragments are implanted orthotopically55, murine cells are injected intraperitoneally or tumor development occurs spontaneously in GEMs56,57. In contrast, SC implanted tumors will generate a different but very specific set of clinical signs driven by replication rate, invasiveness, tendency to ulcerate and site of inoculation. Although in general the set of clinical signs will be similar in SC models regardless of the tumor type, aggressiveness directly linked to tumor (sub)type will also have an impact. Likewise, therapeutics such as cisplatin will exhibit similar side effects in treatment studies of different tumor types10.
In a stepwise approach, the OBSERVE guidelines aim to address multiple aspects of an in vivo cancer study. First, we address appropriate preparation and refinement of specific implantation methods. Then, we describe the clinical signs which may be associated with a specific tumor type and how these signs can be assessed. Finally, we focus on refinement during tumor growth using a two-pronged approach: how to monitor tumor growth (Box 1) on the one hand and how to follow-up on the animal on the other hand (for example when dealing with loss of appetite and consequent body weight (BW) loss; Fig. 2). The latter is done by providing a comprehensive and specific set of monitoring sheets for different clinical signs including the description of specific humane endpoints (HEPs). HEPs are specific timepoints at which measures to alleviate pain and distress are taken, and ultimately offer criteria for humanely killing of the animals. HEPs must be tailored to the objective of the study and aim to reduce overall severity. Therefore, to facilitate definition and use of HEPs, we have developed generic and specific monitoring sheets that stratify HEPs into ‘actions to be taken’ and ‘criteria for humane killing’. A clear overview of severity assessment in relation to clinical signs, implantation method and tumor specificities is provided. Of note, HEPs and prospective severity assessment of an experimental protocol must be defined upfront, and thus guide decision-making policy of an animal study.
When rodents are anorexic, providing easy to reach food and/or appetent food might stimulate their appetite. When BW loss is expected, providing appetent food early on allows to overcome the classical neophobic response. In case of not eating or dehydration, parenteral fluids should be given. Considering variation in food may influence your outcome, control animals should receive the same feeding regimen.
Method
The OBSERVE guidelines were developed by an expert group of laboratory animal veterinarians, animal welfare officers and researchers involved in preclinical research with an interest in murine cancer studies. The generation of the OBSERVE guidelines was supported by a steering committee, a larger expert panel and two consortia in animal research, EurOPDX (www.europdx.eu) and INFRAFRONTIER (www.infrafrontier.eu). EurOPDX, the European consortium on PDX models, is actively developing standard operating procedures for quality control and in vivo drug efficacy studies, thereby fostering reproducibility and replicability in preclinical research. INFRAFRONTIER, the European Research Infrastructure for the generation, phenotyping, archiving and distribution of model mammalian genomes, largely addresses the issue of reproducibility and replicability by developing internal quality principles58 for its different service areas. As such, they provide a quality framework for its operational activities.
The steering committee established four key objectives for the guidelines:
-
1.
Comprehensible for a diverse audience, including animal caretakers and researchers with minimal experience in animal studies.
-
2.
Practical and precise with specific guidelines per tumor type or site of growth, including suggested endpoints, using tables and monitoring sheets
-
3.
Focus on refinement and reproducibility, avoiding housing and husbandry, description of specific cancer models, cell types, etc.
-
4.
Applicable to a wide-range of tumor models
The steering committee’s initial draft was based on the committee members’ experience and literature focused on refinement and reproducibility. The guidelines were further refined with the addition of experts in specific areas of needs. In parallel, draft guidelines were reviewed by EurOPDX and INFRAFRONTIER.
The OBSERVE guidelines are designed to guide researchers in a step-by-step approach. First, the researcher is encouraged to refine the animal study by proper preparation and optimizing the method of implantation. Then, we list which clinical signs and/or adverse effects may be expected in a specific tumor model (Table 1). Next we explain these clinical signs in more detail: their etiology, recognition and monitoring (Table 2). This is followed by selecting the most appropriate method to follow-up tumor growth (Table 3) combined with comprehensive monitoring sheets (Tables 4–12) specifically for each model. The latter include clear actions to be taken as well as the description of discrete HEPs. Finally, a severity classification (Table 13) is given for the different cancer models.
Refinement during implantation or induction of tumors
The following points should be considered when selecting an appropriate animal model: for previously established models, consult existing literature and experienced colleagues to better comprehend the model. Factors to be considered include tumor growth pattern, likelihood of metastasis and development of paraneoplastic syndromes such as cachexia. If a novel model is to be generated, pilot studies should be conducted to analyze the model-specific features before using a larger cohort of animals.
When transplanting tumors into animals, precautions should be taken to ensure long-lasting engraftment, avoid host-versus-graft reaction and prevent the development of infectious disease of the host. These considerations include (a) careful selection of the correct mouse strain (genetic background and immune status) and suitable tumor characteristics, (b) PDX tumor transplants should be actively dividing cells derived from a nonulcerated, nonhemorrhagic and nonnecrotic tumor59, (c) cell lines should be viable and proliferating and less than 80% confluent prior engraftment, (d) it must be ensured that cells are not contaminated with mycoplasma or other pathogens as this may compromise experimental results or cause disease outbreaks among laboratory animals. Therefore, screening of tumors for rodent and human pathogens (in case of PDX) is strongly recommended60,61,62,63 .
Tumor implantation should be performed by appropriately trained staff using aseptic techniques and peri-operative care must include the appropriate administration of anesthetic and analgesic regimens (Box 2). The size of incisions (when required) should be minimized to reduce postprocedure pain and appropriate needle sizes and injection volumes should be utilized64,65. Tumor transplantations should be performed expeditiously following donor tissue collection. Co-injection of a dye to ensure correct tumor localization may help in training of injectable transplantation techniques66,67. The use of a separate set of surgical instruments for the manipulation of tumor tissue—distinct from instrumentation used to manipulate nontumor tissue—is strongly recommended to prevent the spread of tumor cells by surgical instruments.
Note that orthotopic growth better models the human condition as compared with SC implantation, as demonstrated in breast cancer68,69,70. In addition, orthotopic implantation seems to achieve better engraftment rates compared with SC engraftment71.
General as well as specific recommendations for tumor implantation are provided.
SC tumor transplantation
SC tumors should be implanted on the dorsum or flank. These sites are less likely to result in site-related morbidity or interfere with normal body functions (locomotion, breathing, etc.). Other implantation sites, e.g., around the head, footpad and inside of the thigh should be avoided unless there is particular scientific purpose. In general, a single site should be used; however, no more than two sites should be implanted. Implanting more than one tumor per flank will increase the risk of side effects such as locomotor issues in case tumors are implanted further apart from each other or fusion of the different tumors if implanted too close to each other. Furthermore, scientifically there is usually no added value of implanting more than two tumors.
Mammary gland tumor transplantation
Tumors should preferentially be implanted in the third or fourth mammary glands as these sites are less likely to cause site-related morbidity or interfere with normal body functions. The most cranial (first) and caudal mammary glands (fifth in mice, sixth in rats) should be avoided, unless there is a clear scientific need, as growth at this site can hamper movement of the animal. Depending on the research question, a specific mammary gland can be better suited than another69. Implantation in the mammary fat pad can be refined by using a technique wherein the mammary fat pad is no longer cleared for endogenous mammary tissue and tumor cell suspension is injected by slightly pulling out and exposing the fat pad through an incision size <3 mm instead of through a large V-shaped incision72. A variety of injection volumes have been reported; however, the maximum volume of Matrigel or Cultrex to be injected in the mammary fat pad of mice without spillage is 20–30 µl (second to fourth mammary fat pad, respectively)73. In case of tissue fragment transplantation, fragments should not exceed 3 × 3 mm (ref. 74). Intraductal injection does not necessitate cutting the teat. A stereoscope and fine needle (30–34G) should be used to inject tumor cells directly into the teat canal. Dead skin covering the teat canal opening should be removed to facilitate insertion of the needle75. In mice, volumes of 10–20 µl can be injected intraductally75. In rats, 60 µl can be injected as the ductal tree is much larger76. Overall, no more than two mammary glands should be implanted.
Intracerebral tumor implantation/injection
Injection or implantation into the cranium requires the use of a stereotaxic frame. Stereotactic surgery can be refined by using appropriate multimodal analgesia including local anesthesia prior skin incision (of note: local anesthetics containing adrenalin will diminish intra-operative bleeding). Ear bars not puncturing the tympanic membrane should be used77,78. The implantation site can have an important effect on tumor growth, survival and histologic characteristics and therefore must be carefully considered79. Especially in rats where skull thickness can vary as a function of age, the reference point for the calculation of the depth can be taken from the dura78. Needles specifically designed for intracranial use allow the delivery of microvolumes while minimizing tissue damage. Consider wiping the needle tip before needle positioning for aggressive cell lines to ensure no tumor cells adhere to the surrounding skull. Following needle insertion, allow 1–2 min for brain tissue to acclimatize. Reduce the volume of injection to the minimum with a maximum of 5 µl at maximum speed of 1 µl/min. Following completion of injection, allow tumor cells to accumulate in the bottom of the needle tract for 1–2 min, before slow needle withdrawal. Washing the skull (with 0.9% NaCl) will avoid ectopic tumor growth.
Intrapulmonary tumor implantation
To develop orthotopic lung cancer models, tumor cells have been injected in the lung percutaneously80,81. However, this surgical technique can lead to major adverse effects including thoracic bleeding and pneumothorax81. In contrast, the implantation of cells through the trachea prevents the development of such undesired adverse effects. Administration of cells in the trachea can be achieved through surgical tracheostomy82. However, nonsurgical instillation based on standard intubation methods for rodent ventilation83,84 is the most refined and thus preferred technique. Nonsurgical instillation results in a single well-defined tumor instead of multifocal lesions83,84, making tumor measurement easier and more accurate. Several aids are described to facilitate the visualization of the vocal cords: a fiberoptic light85, an intubation standard83, a surgical microscope84 or an external light source86 (the choice which can be based on personal preference). To avoid damage of the laryngeal structures and obtain optimal refinement, cannulae should be as atraumatic and small as possible. Therefore, it is preferable to utilize a plastic (e.g., intravenous catheter) rather than a metal cannula. Moreover, it is important to have sufficient experience to intubate and ensure minimal trauma quickly and proficiently. The length of the cannula should be adapted to the size of the mice to avoid puncturing the lung. The maximum cell suspension recommended for intratracheal injection is 30–50 µl for mice and neonatal rats, and 100 µl for adult rats.
Tumor implantation into the abdomen
Orthotopic implantation of cancer cells and/or tissue into the abdominal organs (intestines, pancreas, liver, urogenital organs) may require laparotomy. Standard refinement for surgical procedures are described in Box 3. When performing a laparotomy, ensure incision length is minimized. Handle all abdominal organs, particularly the intestines, gently using nontraumatizing instruments or cotton buds and avoid the application of pressure to the organs. Inappropriate/rough handling may induce ileus or other gastrointestinal (GI) problems. When organs are exteriorized (placed outside the body cavity), maintain moisture by applying warm sterile NaCl solution. Gently reinsert the organs into the abdomen following cell-suspension injection or tumor-fragments implantation before closing the abdominal wall in two layers (peritoneum/muscle and skin) Avoid accidental spillage of cells into the abdominal cavity by injection of the appropriate volume and use a proper gauge needle, depending on the species and organ. The use of a dissecting microscope may assist in visualization. A laparotomy is a painful procedure87 so apply appropriate multimodal analgesia for minimum 48–72 h following surgery. Other than laparotomy, implantation in abdominal organs can be achieved through non- or minimally invasive and thus more refined methods. For intestinal tumors, nonsurgical implantation in the distal rectum88,89 or implantation through endoscopy90 have been described. Hite et al. compared the intrarectal (not requiring laparotomy) and intracecal injection performed via laparotomy. While the intrarectal injection group had a mortality rate of 4%, the mortality rate in the intracecal injection group was 17%. Both methods had a 100% tumor uptake91. Also for implantation in the liver, spleen, pancreas, adrenal and subcapsular region of the kidney, alternative and more refined injection methods through ultrasound guidance have been validated thereby avoiding the more invasive injection method through laparotomy92,93,94,95. Tumor take rates were high (up to 100%) in all organs and authors stated the procedure to be short and easy to perform. For inoculation in the bladder, both injection through ultrasound guidance96 as well as transurethral injection97,98 do not require a laparotomy.
Intravenous tumor injection
Typically, the lateral tail vein is used for intravascular delivery of agents in rodents. Similar principles apply for intravenous injection of tumor cells as for intravenous injection of other compounds. Briefly: use the smallest needle possible (may depend on tumor cell size), preheat the tail of the animal to ±37 °C to promote peripheral vasodilatation and use the correct restrainer. A useful alternative to tail vein injection is the technique of retro-orbital injection of the venous sinus in the adult and neonatal mouse. This easily mastered technique is a refined method for bone marrow transplantation, leukemia induction, administration of experimental compounds and gene therapy, creating less distress with a lower failure rate99,100. Note that although bone marrow cells have traditionally been injected intravenously, engraftment of bone marrow cells have a higher success rate when injected directly in the bone marrow101,102 (see below).
HDTVI
Hydrodynamic tail vein injection (HDTVI) is a technique wherein a high volume (up to 10% of BW) of a (cell/vector/plasmid) suspension is rapidly (usually within no more than 10 s) injected intravenously to facilitate uptake of tumor cells in the liver. HDTVI causes a massive expansion of the liver, an increase in pressure in the vena cava and massive drop in arterial pressure accompanied by electrocardiogram abnormalities. High injection volumes can cause respiratory arrest103,104. Therefore, close monitoring post procedure is mandated (at least 1 h after injection) and analgesics are required. The use of anesthesia for HDTVI is under debate as it may increase mortality.
Intracardiac tumor injection
Intracardiac injection may be used to study brain or bone metastasis. This technique, however, entails a substantial risk of mortality. Campbell et al. describe how this injection should be performed technically105. Using ultrasound guidance to correctly position the needle will increase success rate and decrease mortality94,106. Some (larger) tumor cells may cause thrombo-embolism and injecting a low-molecular heparin intravenously before intracardiac injection will reduce this risk107.
Intramuscular tumor implantation/injection
Implantation in the muscle should be avoided whenever possible. Muscle distention is painful and there is a risk of affecting locomotion. A maximum of 50 µl should be injected with the finest needle possible (e.g., 27G or smaller) in the quadriceps or caudal thigh muscle108.
Intrabone marrow/intra-osseous tumor injection
Recent evidence has demonstrated that intrafemoral injection in mice significantly decreases the degree of impairment and distress postoperative compared with intratibial injection109. Nevertheless, when performing an intratibial injection, a 30G (rather than 26G) needle is recommended as a refinement. Moreover, the patellar tendon should be avoided109. The risk of impairment and lameness dictates that intrabone marrow transplantation should be limited to one leg per animal. In bone tumor models, intra-osseous implantation (versus para-tibial) results in a more clinically faithful disease model, despite a potentially reduced tumor growth. Nevertheless, this method is frequently associated with a dissemination of cells in the bloodstream, which can be partly prevented by slowly retracting the needle after injection and reducing the number of cells injected110.
Para-tibial tumor implantation
To stimulate seeding of the tumor cells, the periost should be activated with the tip of a needle (periosteum denudation). Use the finest (e.g., 30–31G) needle possible to avoid soft tissue injury and inflammation as much as possible110. Note that the periost is very sensitive and sufficient analgesia should thus be provided.
Carcinogenic tumor models
More than in implanted tumors, carcinogen-induced tumors may occur unpredictably in terms of timing, location and number of lesions. Variable responses to carcinogens may not only depend on type and dosage of carcinogen but also on strain, age, sex or even individual animals111,112,113,114,115. Therefore, it is important to start with a robust literature study and a pilot toxicity study before study commencement. Pilot studies should determine the lowest effective carcinogen dose while limiting adverse effects (e.g., bone marrow suppression or diarrhea in radiation-induced models116) and the optimal administration route. Moreover, pilot studies facilitate the assessment of negative effects on animal welfare, carcinogen-related health issues and definition of appropriate endpoints.
Tumor resection models
Surgical resection of primary tumors (grafted or GEM) can be performed in several settings including models of spontaneous metastasis and models of advanced disease in tumors wherein resection is usually the first treatment (e.g., brain117). Specifically in the context of metastases, tumor resection assists where HEPs limit the duration of the study either due to tumor size (e.g., breast cancer118 or osteosarcoma119) or clinical condition of the animals in aggressive cancers (e.g., pancreas120). While it is beyond the scope of this manuscript to provide details on all such models, the following general steps are recommended. First, perform a pilot study to assess whether recurrence occurs, metastasis develops and survival increases following tumor resection121. Second, if resection is necessary to answer the scientific question, assess the optimal time for primary resection to limit welfare impairment as much as possible. It is usually not necessary to wait until the tumor approaches maximum size. Of note tumor resection timepoints differ per organ. Should tumor volume measurements be unavailable, resection upon reaching exponential growth phase, as determined by bioluminescence, is a suitable approach to ensure recurrence122. In contrast to surgical implantation of tumors wherein animals are usually healthy, in surgical resection models, animals are tumor bearing and thus by definition not healthy. Peri-operative care should therefore be adapted accordingly.
Humanized mouse models
In general, three different methods are used to reconstitute human immune lineage in immune deficient mice: (1) direct infusion of mature human immune cells, most commonly used source are peripheral blood mononuclear cells, (2) engraftment with human CD34+ hematopoietic stem and progenitor cells upon host preconditioning to deplete endogenous immune cells and (3) co-engraftment of human fetal thymus tissue and liver CD34+ hematopoietic stem and progenitor cells. Depending on the method of humanization, various adverse effects can be expected of which graft-versus-host-disease (GVHD), tumor growth inhibition, efficiency impairment of lymphocytes and anemia are the most common ones123. These adverse effects can mostly be prevented by selecting the optimal engraftment strategy and immune deficient mouse for answering the experimental question. For example, a model with delayed GVHD should be used when study duration is longer. Models with rapid onset of GVHD should not be used when study duration is longer (than 4–5 weeks). See also intravenous injection and intra-abdominal implantation for main points of refinement in developing humanized mice.
Clinical consequences of different cancer models
As discussed, adverse effects and clinical consequences for the animal can differ substantially depending on the tumor model. Therefore, animal monitoring procedures, refinement options and HEPs should be adapted accordingly. Table 1 describes which clinical signs or adverse effects may be expected in different tumors regardless of the model (primary versus metastatic, orthotopic implantation versus carcinogen, for example). We decided to distinguish pain into ‘demonstrated’ when studies have shown that these tumors are painful and ‘assumed’ when studies specifically aimed at measuring pain are lacking but when these tumor types are known to be painful in human patients. Anorexia/BW loss and altered appearance/behavior are usually not expected in certain tumor types. However, depending on the aggressiveness of the tumor, these characteristics may be observed (Box 4).
In Table 2, the clinical signs or adverse effects are further outlined. We also elaborate on how these signs can be recognized in rodents and why these may occur in a cancer setting. To assess certain clinical signs, specific tests are recommended. While we chose to recommend easy to perform and minimally invasive tests, such as the stress-test for the assessment of labored breathing (Fig. 3), other more invasive tests or tests requiring specific equipment could be used to assess the animal. We therefore acknowledge that these recommendations are not exhaustive.
a,b, A stress-test should be performed by restraining the mouse as demonstrated in a and pressing the xyphoid with the finger of the dominant hand as demonstrated in b. Gentle-to-moderate pressure should be applied for 3 s. The red circle in a indicates the xyphoid where pressure should be applied. The arrows in b and c indicate the important features when holding the mice.
Refinement during tumor development
Refinement of an ongoing in vivo study should be performed in a twofold manner. First by adapting the monitoring of the animals to the expected adverse effects (i.e., choice of which signs to monitor and the frequency of the monitoring) and second by taking appropriate action based on adverse effects. It is important to note that monitoring the animals implies monitoring the tumor itself (mainly size and/or appearance) and, in parallel, observing the clinical condition of the animal.
Monitoring of tumors
Depending on the location and type of model, different methods can be employed to determine tumor characteristics (e.g., size). Table 3 provides an overview of tumor assessment over time. We will not discuss in detail the different techniques for tumor assessment, rather we will focus on aspects affecting animal welfare or study outcome and reproducibility. The criteria for animal killing are solely based on tumor aspect and not on the clinical condition of the animal. The latter are described in the other monitoring sheets (Tables 4–12).
Monitoring of animals with different tumor models
As discussed above and listed in Table 2, different tumor types may manifest different adverse effects, mainly depending on their location. Although some adverse effects are general and occur in most models (Table 4), others may greatly differ between different models and are very specific, for example, postoperative care (Table 5). Here, we provide clear guidelines on how to monitor animals throughout the study based on expected adverse effects. As scoresheets imply annotating numerical scores to clinical parameters and often require the calculation of a final score to make an informed decision on the animal’s fate; we chose to propose monitoring sheets without numerical scores, which can more easily be combined with a complete monitoring sheet adapted for the varying adverse effects across a variety of tumor models. Monitoring sheets include which parameters to observe, the frequency of monitoring and actions to be taken. In addition, refinement options and criteria for humane methods of killing are described.
Monitoring animals for model-specific adverse effects
For cases in which adverse effects occur predominantly in specific tumor models, we present monitoring sheets that group signs by clinical category. Animals may suffer respiratory difficulties (Table 6), neurological changes (Table 7), locomotor issues (Table 8), GI issues (Table 9) and/or urinary signs (Table 10).
Monitoring animals with tumors causing ascites
Ascites—a condition in which fluid accumulates in the abdomen—is a rare adverse effect, and animals should be culled as soon as possible once this condition develops. When ascites is the main research objective, however, the monitoring sheet in Table 11 may be used.
Correct drainage of ascitic fluid or ascitic taps
When ascitic fluid needs draining, a series of points need to be followed:
-
The mouse needs to be manually restrained, held in a vertical position with the head pointing upward. Inexperienced personnel may anesthetize the mice by using isoflurane
-
The abdominal surface needs to be shaved and disinfected before the insertion of the needle
-
The size of the sterile needle should be the smallest possible (25–22G) to allow good flow. Needle insertion should be in the lower left or right quadrant of the abdomen
-
The ascites fluid needs to be allowed to drip from the needle hub (aspirating fluid may cause circulatory decompression and shock). Rotation of the needle and adjusting the depth of insertion will allow for optimizing the rate of collection. When the ascites is viscous, collection is more efficient if the needle is removed and the fluid is allowed to drip from the puncture. Indicatively, one drop every 3 or 4 s is considered a good flow rate
-
When collection is completed, the puncture site needs to be disinfected again before the animal is returned to its cage
-
The animal should be observed for 30 min after tap for signs of shock or discomfort
Monitoring animals with cutaneous ulcerating tumors
The ulceration of tumors is usually considered an endpoint (Table 3). However, there are exceptional circumstances where ulcers are tolerated and premature killing is postponed, thereby avoiding the loss of potential important data. Exceptions should be only considered if:
-
Models are known to be prone to ulceration
-
Late-stage cancer models that often present with ulcerating tumors
-
Ulcerated tumors that are healed following therapeutic intervention
Noteworthy, erroneously intradermal instead of SC engraftment could lead to fast necrosis and ulcerative tumors. Appropriate training and proper SC injection could limit ulcer development. In Table 12, the different ulcerative lesions are described, including a score for each type of lesion, the necessary interventions and the mandatory monitoring frequency.
Monitoring animals with tumors causing cachexia
Cachexia is a condition where a tumor (or other chronic illness) causes weakness and wasting of the body. Animals should be killed before they become cachectic unless in models wherein cancer cachexia is the main research objective124,125. In all other cancer models, HEPs should be applied to avoid cachexia. Animals in cancer cachexia studies should be culled no later than having reached 25% BW loss, also taking into account the measurement of tumor volume126,127.
Monitoring animals with tumors causing icterus
Icterus (jaundice) is a sign of advanced disease, animals should be humanely killed when diagnosed.
Monitoring animals with tumors causing anemia
When anemia is detected on visual assessment of the animal, the animals should be humanely killed as this is a sign of advanced disease.
Severity assessment
According to the EU directive 2010/63/EU, all animal procedures need to be classified as mild, moderate or severe. However, severity assessment of animal procedures and models remains a difficult task and unfortunately few resources exist on how to consistently classify mouse cancer models, in particular orthotopic and complex models with multiple adverse effects are particularly difficult to consistently classify.
Therefore, in Table 13, we propose a severity classification for a variety of cancer models based on clinical signs, tumor characteristics and implantation method. Note that the severity assessment should take into account all of the above and that the HEPs described throughout the guidelines are crucial in this assessment. If endpoints are exceeded, severity must be scored higher than what was proposed prospectively. Importantly, as some models are always accompanied by severe adverse effects, these models are classified as severe by default, e.g., models requiring ascitic tap or cancer pain models.
Conclusions
The OBSERVE guidelines bridge the existing gap between appropriate preparation and reporting of in vivo cancer studies in rodents. By focusing on refinement during animal experiments, researchers and animal care staff are provided with precise and practical guidance on how to implement the optimal preparation and implantation methods. Also, expected adverse effects and clinical signs associated with organ-specific tumor development are clearly described including etiology and guidelines for assessment. In addition, hands-on tools and precise monitoring criteria during tumor development are provided at two levels: how to monitor tumor proliferation and how to follow-up the animal. The latter is done by providing a comprehensive and specific set of monitoring sheets for rodents with a variety of clinical signs, regardless of their origin, and incorporate HEPs that are based on expected adverse effects per tumor type. At last, a robust guidance on severity assessment is provided based on clinical consequences, implantation method and characteristics of the tumor.
Since reliable animal-free alternatives are not yet widely available, in vivo experiments remain an important step in unravelling complex biological questions. Nevertheless, animal experiments that are still required must be performed in the most optimal and ethical way. Therefore, the current refinement guidelines fill an important gap by providing a practical resource for a large number of cancer research laboratories. We strongly believe major improvements can be generated in workflows of in vivo experimentation, thereby minimizing the level of severity in the most common murine models and reducing unnecessary distress and pain. The guidelines can largely contribute to animal welfare and the refinement of animal studies in cancer research.
References
O’Brien, S. G. et al. Imatinib compared with interferon and low-dose cytarabine for newly diagnosed chronic-phase chronic myeloid leukemia. N. Engl. J. Med. 348, 994–1004 (2003).
Fazio, M., Ablain, J., Chuan, Y., Langenau, D. M. & Zon, L. I. Zebrafish patient avatars in cancer biology and precision cancer therapy. Nat. Rev. Cancer 20, 263–273 (2020).
Pauli, C. et al. Personalized in vitro and in vivo cancer models to guide precision medicine. Cancer Discov. 7, 462–477 (2017).
Le Magnen, C., Dutta, A. & Abate-Shen, C. Optimizing mouse models for precision cancer prevention. Nat. Rev. Cancer 16, 187––196 (2016).
Animals used for scientific purposes. European Commission https://ec.europa.eu/environment/chemicals/lab_animals/alures_en.htm (2022).
Guillen, K. P. et al. A human breast cancer-derived xenograft and organoid platform for drug discovery and precision oncology. Nat. Cancer 3, 232–250 (2022).
Honkala, A., Malhotra, S. V., Kummar, S. & Junttila, M. R. Harnessing the predictive power of preclinical models for oncology drug development. Nat. Rev. Drug Discov. 21, 99–114 (2022).
Cuppens, T. et al. Potential targets’ analysis reveals dual PI3K/mTOR pathway inhibition as a promising therapeutic strategy for uterine leiomyosarcomas—an ENITEC group initiative. Clin. Cancer Res. 23, 1274–1285 (2017).
Hebert, J. D., Neal, J. W. & Winslow, M. M. Dissecting metastasis using preclinical models and methods. Nat. Rev. Cancer 23, 391–407 (2023).
Perse, M. Cisplatin mouse models: treatment, toxicity and Translatability. Biomedicines 9, 1406 (2021).
Karkampouna, S. et al. Patient-derived xenografts and organoids model therapy response in prostate cancer. Nat. Commun. 12, 1117 (2021).
Patton, E. E. et al. Melanoma models for the next generation of therapies. Cancer Cell 39, 610–631 (2021).
Zitvogel, L., Pitt, J. M., Daillere, R., Smyth, M. J. & Kroemer, G. Mouse models in oncoimmunology. Nat. Rev. Cancer 16, 759–773 (2016).
Gardner, E. E. & Rudin, C. M. Drug therapy: preclinical oncology—reporting transparency needed. Nat. Rev. Clin. Oncol. 13, 8–9 (2016).
Amaral, O. B. & Neves, K. Reproducibility: expect less of the scientific paper. Nature 597, 329–331 (2021).
Pritt, S. L. & Hammer, R. E. The interplay of ethics, animal welfare, and IACUC oversight on the reproducibility of animal studies. Comp. Med. 67, 101–105 (2017).
Cheleuitte-Nieves, C. & Lipman, N. S. Improving replicability, reproducibility, and reliability in preclinical research: a shared responsibility. ILAR J. 60, 113–119 (2019).
Errington, T. M. et al. Investigating the replicability of preclinical cancer biology. eLife 10, e.71601 (2021).
Smith, A. J., Clutton, R. E., Lilley, E., Hansen, K. E. A. & Brattelid, T. PREPARE: guidelines for planning animal research and testing. Lab. Anim. 52, 135–141 (2018).
Kilkenny, C., Browne, W. J., Cuthill, I. C., Emerson, M. & Altman, D. G. Improving bioscience research reporting: the ARRIVE guidelines for reporting animal research. PLoS Biol. 8, e1000412 (2010).
Percie du Sert, N. et al. The ARRIVE guidelines 2.0: updated guidelines for reporting animal research. PloS Biol. 18, e3000410 (2020).
EU Parliament event on animal research. European Animal Resarch Association https://www.eara.eu/post/eu-parliament-event-on-animal-research (2022).
Russell, W. M. S. & Burch, R. L. The Principles of Humane Experimental Technique. (Methuen, 1959).
Tannenbaum, J. & Bennett, B. T. Russell and Burch’s 3Rs then and now: the need for clarity in definition and purpose. J. Am. Assoc. Lab. Anim. Sci. 54, 120–132 (2015).
Workman, P. et al. Guidelines for the welfare and use of animals in cancer research. Br. J. Cancer 102, 1555–1577 (2010).
Wallace, J. Humane endpoints and cancer research. ILAR J. 41, 87–93 (2000).
Workman, P. et al. UKCCCR guidelines for the welfare of animals in experimental neoplasia. Lab. Anim. 22, 195–201 (1988).
Winn, C. B. et al. Automated monitoring of respiratory rate as a novel humane endpoint: a refinement in mouse metastatic lung cancer models. PLoS ONE 16, e0257694 (2021).
Aldred, A. J., Cha, M. C. & Meckling-Gill, K. A. Determination of a humane endpoint in the L1210 model of murine leukemia. Contemp. Top. Lab. Anim. Sci. 41, 24–27 (2002).
Paster, E. V., Villines, K. A. & Hickman, D. L. Endpoints for mouse abdominal tumor models: refinement of current criteria. Comp. Med. 59, 234–241 (2009).
Helgers, S. O. A. et al. Body weight algorithm predicts humane endpoint in an intracranial rat glioma model. Sci. Rep. 10, 9020 (2020).
Oliveira, M. et al. Implementation of humane endpoints in a urinary bladder carcinogenesis study in rats. Vivo 31, 1073–1080 (2017).
Silva-Reis, R. et al. Refinement of animal model of colorectal carcinogenesis through the definition of novel humane endpoints. Animals 11, 985 (2021).
Akladios, C., Ignat, M., Mutter, D. & Aprahamian, M. Survival variability of controls and definition of imaging endpoints for longitudinal follow-up of pancreatic ductal adenocarcinoma in rats. J. Cancer Res. Clin. Oncol. 143, 29–34 (2017).
Kobaek-Larsen, M., Rud, L., Oestergaard Soerensen, F. & Ritskes-Hoitinga, J. Laparoscopy of rats with experimental liver metastases: a method to assess new humane endpoints. Lab. Anim. 38, 162–168 (2004).
Percie du Sert, N. et al. The IMPROVE guidelines (ischaemia models: procedural refinements of in vivo experiments). J. Cereb. Blood Flow. Metab. 37, 3488–3517 (2017).
Mirzoyan, Z. et al. Drosophila melanogaster: a model organism to study cancer. Front. Genet. 10, 51 (2019).
Yamamura, R., Ooshio, T. & Sonoshita, M. Tiny Drosophila makes giant strides in cancer research. Cancer Sci. 112, 505–514 (2021).
Robertson, N., Schook, L. B. & Schachtschneider, K. M. Porcine cancer models: potential tools to enhance cancer drug trials. Expert Opin. Drug Discov. 15, 893–902 (2020).
Oh, J. H. & Cho, J. Y. Comparative oncology: overcoming human cancer through companion animal studies. Exp. Mol. Med. 55, 725–734 (2023).
Deycmar, S., Gomes, B., Charo, J., Ceppi, M. & Cline, J. M. Spontaneous, naturally occurring cancers in non-human primates as a translational model for cancer immunotherapy. J. Immunother. Cancer 11, e005514 (2023).
Cannon, C. M. Cats, cancer and comparative oncology. Vet. Sci. 2, 111–126 (2015).
Overgaard, N. H. et al. Of mice, dogs, pigs, and men: choosing the appropriate model for immuno-oncology research. ILAR J. 59, 247–262 (2018).
LeBlanc, A. K. & Mazcko, C. N. Improving human cancer therapy through the evaluation of pet dogs. Nat. Rev. Cancer 20, 727–742 (2020).
Schook, L. B. et al. A genetic porcine model of cancer. PLoS ONE 10, e0128864 (2015).
Kalla, D. et al. The missing link: cre pigs for cancer research. Front. Oncol. 11, 755746 (2021).
Kalla, D., Kind, A. & Schnieke, A. Genetically engineered pigs to study cancer. Int. J. Mol. Sci. 21, 488 (2020).
Astell, K. R. & Sieger, D. Zebrafish in vivo models of cancer and metastasis. Cold Spring Harb. Perspect. Med. 10, a037077 (2020).
Jiang, H., Kimura, T., Hai, H., Yamamura, R. & Sonoshita, M. Drosophila as a toolkit to tackle cancer and its metabolism. Front. Oncol. 12, 982751 (2022).
Hendricks-Wenger, A. et al. Employing novel porcine models of subcutaneous pancreatic cancer to evaluate oncological therapies. Methods Mol. Biol. 2394, 883–895 (2022).
Callesen, M. M. et al. A genetically inducible porcine model of intestinal cancer. Mol. Oncol. 11, 1616–1629 (2017).
Boas, F. E. et al. Induction and characterization of pancreatic cancer in a transgenic pig model. PLoS ONE 15, e0239391 (2020).
Saur, D. & Schnieke, A. Porcine cancer models for clinical translation. Nat. Rev. Cancer 22, 375–376 (2022).
Jarvis, S. et al. Non-rodent animal models of osteosarcoma: a review. Cancer Treat. Res. Commun. 27, 100307 (2021).
Penet, M. F. et al. Ascites volumes and the ovarian cancer microenvironment. Front. Oncol. 8, 595 (2018).
Sale, S. & Orsulic, S. Models of ovarian cancer metastasis: murine models. Drug Discov. Today Dis. Models 3, 149––154 (2006).
Zakarya, R., Howell, V. M. & Colvin, E. K. Modelling epithelial ovarian cancer in mice: classical and emerging approaches. Int. J. Mol. Sci. 21, 4806 (2020).
Ehlich, H. et al. INFRAFRONTIER quality principles in systemic phenotyping. Mamm., Genome 33, 120–122 (2022).
Meehan, T. F. et al. PDX-MI: minimal information for patient-derived tumor xenograft models. Cancer Res. 77, e62–e66 (2017).
Peterson, N. C. From bench to cageside: risk assessment for rodent pathogen contamination of cells and biologics. ILAR J. 49, 310–315 (2008).
Nicklas, W., Kraft, V. & Meyer, B. Contamination of transplantable tumors, cell lines, and monoclonal antibodies with rodent viruses. Lab. Anim. Sci. 43, 296–300 (1993).
Geraghty, R. J. et al. Guidelines for the use of cell lines in biomedical research. Br. J. Cancer 111, 1021–1046 (2014).
Chateau-Joubert, S. et al. Spontaneous mouse lymphoma in patient-derived tumor xenografts: the importance of systematic analysis of xenografted human tumor tissues in preclinical efficacy trials. Transl. Oncol. 14, 101133 (2021).
Diehl, K. H. et al. A good practice guide to the administration of substances and removal of blood, including routes and volumes. J. Appl. Toxicol. 21, 15–23 (2001).
Turner, P. V., Brabb, T., Pekow, C. & Vasbinder, M. A. Administration of substances to laboratory animals: routes of administration and factors to consider. J. Am. Assoc. Lab. Anim. Sci. 50, 600–613 (2011).
Glascock, J. J. et al. Delivery of therapeutic agents through intracerebroventricular (ICV) and intravenous (IV) injection in mice. J. Vis. Exp. https://doi.org/10.3791/2968 (2011).
Blair-Handon, R., Mueller, K. & Hoogstraten-Miller, S. An alternative method for intrathymic injections in mice. Lab. Anim. 39, 248–252 (2010).
Okano, M. et al. Orthotopic implantation achieves better engraftment and faster growth than subcutaneous implantation in breast cancer patient-derived xenografts. J. Mammary Gland Biol. Neoplasia 25, 27–36 (2020).
Rashid, O. M. et al. An improved syngeneic orthotopic murine model of human breast cancer progression. Breast Cancer Res. Treat. 147, 501–512 (2014).
Zhang, G. L., Zhang, Y., Cao, K. X. & Wang, X. M. Orthotopic injection of breast cancer cells into the mice mammary fat pad. J. Vis. Exp. https://doi.org/10.3791/58604 (2019).
Byrne, A. T. et al. Interrogating open issues in cancer precision medicine with patient-derived xenografts. Nat. Rev. Cancer 17, 254–268 (2017).
Tavera-Mendoza, L. E. & Brown, M. A less invasive method for orthotopic injection of breast cancer cells into the mouse mammary gland. Lab. Anim. 51, 85–88 (2017).
Katsuta, E. et al. Modified breast cancer model for preclinical immunotherapy studies. J. Surg. Res. 204, 467–474 (2016).
Martinez-Sabadell, A., Ovejero Romero, P., Arribas, J. & Arenas, E. J. Protocol to generate a patient derived xenograft model of acquired resistance to immunotherapy in humanized mice. STAR Protoc. 3, 101712 (2022).
Krause, S., Brock, A. & Ingber, D. E. Intraductal injection for localized drug delivery to the mouse mammary gland. J. Vis. Exp. https://doi.org/10.3791/50692 (2013).
Bu, W. & Li, Y. Intraductal injection of lentivirus vectors for stably introducing genes into rat mammary epithelial cells in vivo. J. Mammary Gland Biol. Neoplasia 25, 389–396 (2020).
Barahona, M. J., Rojas, J., Uribe, E. A. & Garcia-Robles, M. A. Tympanic membrane rupture during stereotaxic surgery disturbs the normal feeding behavior in rats. Front. Behav. Neurosci. 14, 591204 (2020).
Ferry, B. & Gervasoni, D. Improving stereotaxic neurosurgery techniques and procedures greatly reduces the number of rats used per experimental group—a practice report. Animals 11, 2662 (2021).
Irtenkauf, S. M. et al. Optimization of glioblastoma mouse orthotopic xenograft models for translational research. Comp. Med. 67, 300–314 (2017).
Onn, A. et al. Development of an orthotopic model to study the biology and therapy of primary human lung cancer in nude mice. Clin. Cancer Res. 9, 5532–5539 (2003).
Boehle, A. S., Dohrmann, P., Leuschner, I., Kalthoff, H. & Henne-Bruns, D. An improved orthotopic xenotransplant procedure for human lung cancer in SCID bg mice. Ann. Thorac. Surg. 69, 1010–1015 (2000).
Kang, Y. et al. Development of an orthotopic transplantation model in nude mice that simulates the clinical features of human lung cancer. Cancer Sci. 97, 996–1001 (2006).
Buckle, T. & van Leeuwen, F. W. Validation of intratracheal instillation of lung tumour cells in mice using single photon emission computed tomography/computed tomography imaging. Lab. Anim. 44, 40–45 (2010).
Nakajima, T. et al. Orthotopic lung cancer murine model by nonoperative transbronchial approach. Ann. Thorac. Surg. 97, 1771–1775 (2014).
Das, S., MacDonald, K., Chang, H. Y. & Mitzner, W. A simple method of mouse lung intubation. J. Vis. Exp. 73, e50318 (2013).
Brown, R. H., Walters, D. M., Greenberg, R. S. & Mitzner, W. A method of endotracheal intubation and pulmonary functional assessment for repeated studies in mice. J. Appl. Physiol. 87, 2362–2365 (1999).
Roughan, J. V., Bertrand, H. G. & Isles, H. M. Meloxicam prevents COX-2-mediated post-surgical inflammation but not pain following laparotomy in mice. Eur. J. Pain. 20, 231–240 (2016).
Kashtan, H. et al. Intra-rectal injection of tumour cells: a novel animal model of rectal cancer. Surg. Oncol. 1, 251–256 (1992).
Richon, S., Zajac, O., Perez Gonzalez, C. & Matic Vignjevic, D. Optimized protocol for the generation of an orthotopic colon cancer mouse model and metastasis. STAR Protoc. 4, 102022 (2023).
Zigmond, E. et al. Utilization of murine colonoscopy for orthotopic implantation of colorectal cancer. PLoS ONE 6, e28858 (2011).
Hite, N. et al. An optimal orthotopic mouse model for human colorectal cancer primary tumor growth and spontaneous metastasis. Dis. Colon Rectum 61, 698–705 (2018).
McVeigh, L. E. et al. Development of orthotopic tumour models using ultrasound-guided intrahepatic injection. Sci. Rep. 9, 9904 (2019).
Huynh, A. S. et al. Development of an orthotopic human pancreatic cancer xenograft model using ultrasound guided injection of cells. PLoS ONE 6, e20330 (2011).
Camara Serrano, J. A. Ultrasound guided surgery as a refinement tool in oncology research. Animals 12, 3445 (2022).
RA, V. A. N. N. et al. Tissue-directed implantation using ultrasound visualization for development of biologically relevant metastatic tumor xenografts. Vivo 31, 779–791 (2017).
Jager, W. et al. Ultrasound-guided intramural inoculation of orthotopic bladder cancer xenografts: a novel high-precision approach. PLoS ONE 8, e59536 (2013).
Hadaschik, B. A. et al. A validated mouse model for orthotopic bladder cancer using transurethral tumour inoculation and bioluminescence imaging. BJU Int. 100, 1377–1384 (2007).
Watanabe, T. et al. An improved intravesical model using human bladder cancer cell lines to optimize gene and other therapies. Cancer Gene Ther. 7, 1575–1580 (2000).
Yardeni, T., Eckhaus, M., Morris, H. D., Huizing, M. & Hoogstraten-Miller, S. Retro-orbital injections in mice. Lab. Anim. 40, 155–160 (2011).
Leon-Rico, D. et al. Comparison of haematopoietic stem cell engraftment through the retro-orbital venous sinus and the lateral vein: alternative routes for bone marrow transplantation in mice. Lab. Anim. 49, 132–141 (2015).
Li, Q. et al. Analyses of very early hemopoietic regeneration after bone marrow transplantation: comparison of intravenous and intrabone marrow routes. Stem Cells 25, 1186–1194 (2007).
Kushida, T. et al. Intra-bone marrow injection of allogeneic bone marrow cells: a powerful new strategy for treatment of intractable autoimmune diseases in MRL/lpr mice. Blood 97, 3292–3299 (2001).
Sawyer, G. J. et al. Cardiovascular function following acute volume overload for hydrodynamic gene delivery to the liver. Gene Ther. 14, 1208–1217 (2007).
Suda, T., Gao, X., Stolz, D. B. & Liu, D. Structural impact of hydrodynamic injection on mouse liver. Gene Ther. 14, 129–137 (2007).
Campbell, J. P., Merkel, A. R., Masood-Campbell, S. K., Elefteriou, F. & Sterling, J. A. Models of bone metastasis. J. Vis. Exp. 4, e4260 (2012).
Zhou, H. & Zhao, D. Ultrasound imaging-guided intracardiac injection to develop a mouse model of breast cancer brain metastases followed by longitudinal MRI. J. Vis. Exp. https://doi.org/10.3791/51146 (2014).
Stocking, K. L. et al. Use of low-molecular-weight heparin to decrease mortality in mice after intracardiac injection of tumor cells. Comp. Med. 59, 37–45 (2009).
Gehling, A. M. et al. evaluation of volume of intramuscular injection into the caudal thigh muscles of female and male BALB/c mice (Mus musculus). J. Am. Assoc. Lab. Anim. Sci. 57, 35–43 (2018).
Pfeiffenberger, U. et al. Assessment and refinement of intra-bone marrow transplantation in mice. Lab. Anim. 49, 121–131 (2015).
Uluckan, O., Segaliny, A., Botter, S., Santiago, J. M. & Mutsaers, A. J. Preclinical mouse models of osteosarcoma. Bonekey Rep. 4, 670 (2015).
Abel, E. L., Angel, J. M., Kiguchi, K. & DiGiovanni, J. Multi-stage chemical carcinogenesis in mouse skin: fundamentals and applications. Nat. Protoc. 4, 1350–1362 (2009).
Tolba, R., Kraus, T., Liedtke, C., Schwarz, M. & Weiskirchen, R. Diethylnitrosamine (DEN)-induced carcinogenic liver injury in mice. Lab. Anim. 49, 59–69 (2015).
Zeng, L., Li, W. & Chen, C. S. Breast cancer animal models and applications. Zool. Res. 41, 477–494 (2020).
Rivina, L., Davoren, M. J. & Schiestl, R. H. Mouse models for radiation-induced cancers. Mutagenesis 31, 491–509 (2016).
Scholten, D., Trebicka, J., Liedtke, C. & Weiskirchen, R. The carbon tetrachloride model in mice. Lab. Anim. 49, 4–11 (2015).
Duran-Struuck, R. & Dysko, R. C. Principles of bone marrow transplantation (BMT): providing optimal veterinary and husbandry care to irradiated mice in BMT studies. J. Am. Assoc. Lab. Anim. Sci. 48, 11–22 (2009).
Tang, B., Foss, K., Lichtor, T., Phillips, H. & Roy, E. Resection of orthotopic murine brain glioma. Neuroimmunol. Neuroinflamm. 8, 64–69 (2021).
Gast, C. E., Shaw, A. K., Wong, M. H. & Coussens, L. M. Surgical procedures and methodology for a preclinical murine model of de novo mammary cancer metastasis. J. Vis. Exp. https://doi.org/10.3791/54852 (2017).
Ren, L., Huang, S., Beck, J. & LeBlanc, A. K. Impact of limb amputation and cisplatin chemotherapy on metastatic progression in mouse models of osteosarcoma. Sci. Rep. 11, 24435 (2021).
Mallya, K., Gautam, S. K., Aithal, A., Batra, S. K. & Jain, M. Modeling pancreatic cancer in mice for experimental therapeutics. Biochim. Biophys. Acta Rev. Cancer 1876, 188554 (2021).
Linxweiler, J. et al. Primary tumor resection decelerates disease progression in an orthotopic mouse model of metastatic prostate cancer. Cancers 14, 737 (2022).
Sweeney, K. J. et al. Validation of an imageable surgical resection animal model of glioblastoma (GBM). J. Neurosci. Methods 233, 99–104 (2014).
Chuprin, J. et al. Humanized mouse models for immuno-oncology research. Nat. Rev. Clin. Oncol. 20, 192–206 (2023).
Deboer, M. D. Animal models of anorexia and cachexia. Expert Opin. Drug Discov. 4, 1145–1155 (2009).
Bennani-Baiti, N. & Walsh, D. Animal models of the cancer anorexia–cachexia syndrome. Support Care Cancer 19, 1451–1463 (2011).
Euhus, D. M., Hudd, C., LaRegina, M. C. & Johnson, F. E. Tumor measurement in the nude mouse. J. Surg. Oncol. 31, 229–234 (1986).
Tomayko, M. M. & Reynolds, C. P. Determination of subcutaneous tumor size in athymic (nude) mice. Cancer Chemother. Pharmacol. 24, 148–154 (1989).
Ishida, K. et al. Current mouse models of oral squamous cell carcinoma: genetic and chemically induced models. Oral. Oncol. 73, 16–20 (2017).
Naik, K. et al. The histopathology of oral cancer pain in a mouse model and a human cohort. J. Dent. Res. 100, 194–200 (2021).
Pacharinsak, C. & Beitz, A. Animal models of cancer pain. Comp. Med. 58, 220–233 (2008).
Pineda-Farias, J. B., Saloman, J. L. & Scheff, N. N. Animal models of cancer-related pain: current perspectives in translation. Front. Pharmacol. 11, 610894 (2020).
Tetreault, M. P. Esophageal cancer: insights from mouse models. Cancer Growth Metastasis 8, 37–46 (2015).
Cardesa, A., Ovelar, M. Y. & Pera, M. in Digestive System (eds Carlyle Jones, T., Popp, J. A. & Mohr, U.) 318–322 (Springer Berlin, 1997).
Hu, H. et al. Real-time bioluminescence and tomographic imaging of gastric cancer in a novel orthotopic mouse model. Oncol. Rep. 27, 1937–1943 (2012).
Hayakawa, Y. et al. Mouse models of gastric cancer. Cancers 5, 92–130 (2013).
Bhargava, S., Hotz, B., Buhr, H. J. & Hotz, H. G. An orthotopic nude mouse model for preclinical research of gastric cardia cancer. Int. J. Colorectal Dis. 24, 31–39 (2009).
Liu, S. et al. Dynamic observation of the progression of chronic gastritis to gastric cancer in a disease–TCM pattern rat model. J. Trad. Chin. Med. Sci. 8, 124–134 (2021).
Herreros-Villanueva, M., Hijona, E., Cosme, A. & Bujanda, L. Mouse models of pancreatic cancer. World J. Gastroenterol. 18, 1286–1294 (2012).
Lwin, T. M. et al. Fluorescent humanized anti-CEA antibody specifically labels metastatic pancreatic cancer in a patient-derived orthotopic xenograft (PDOX) mouse model. Oncotarget 9, 37333–37342 (2018).
Becker, C. et al. In vivo imaging of colitis and colon cancer development in mice using high resolution chromoendoscopy. Gut 54, 950–954 (2005).
Hasty, P. et al. eRapa restores a normal life span in a FAP mouse model. Cancer Prev. Res. 7, 169–178 (2014).
Chartier, L. C., Hebart, M. L., Howarth, G. S., Whittaker, A. L. & Mashtoub, S. Affective state determination in a mouse model of colitis-associated colorectal cancer. PLoS ONE 15, e0228413 (2020).
Ikenoue, T. et al. A novel mouse model of intrahepatic cholangiocarcinoma induced by liver-specific Kras activation and Pten deletion. Sci. Rep. 6, 23899 (2016).
Vogt, A. et al. Alpha-fetoprotein- and CD40 ligand-expressing dendritic cells for immunotherapy of hepatocellular carcinoma. Cancers 13, 3375 (2021).
Chen, Z., Li, S., Han, L. & He, X. Optimized protocol for an inducible rat model of liver tumor with chronic hepatocellular injury, inflammation, fibrosis, and cirrhosis. STAR Protoc. 2, 100353 (2021).
Odashima, S. Comparative studies on the transplantability of liver cancers induced in rats fed with 3′-methyl-4-dimethylaminoazobenzene for 3–6 months. Gan 53, 325–348 (1962).
Pretto, F. et al. Sunitinib prevents cachexia and prolongs survival of mice bearing renal cancer by restraining STAT3 and MuRF-1 activation in muscle. Oncotarget 6, 3043–3054 (2015).
Roughan, J. V., Coulter, C. A., Flecknell, P. A., Thomas, H. D. & Sufka, K. J. The conditioned place preference test for assessing welfare consequences and potential refinements in a mouse bladder cancer model. PLoS ONE 9, e103362 (2014).
Naito, T., Higuchi, T., Shimada, Y. & Kakinuma, C. An improved mouse orthotopic bladder cancer model exhibiting progression and treatment response characteristics of human recurrent bladder cancer. Oncol. Lett. 19, 833–839 (2020).
Philyppov, I. B. et al. Alterations in detrusor contractility in rat model of bladder cancer. Sci. Rep. 10, 19651 (2020).
Xiao, Z. et al. Characterization of a novel transplantable orthotopic rat bladder transitional cell tumour model. Br. J. Cancer 81, 638––646 (1999).
Ding, J. et al. Current animal models of bladder cancer: awareness of translatability (review). Exp. Ther. Med. 8, 691–699 (2014).
Senapati, S. et al. Overexpression of macrophage inhibitory cytokine-1 induces metastasis of human prostate cancer cells through the FAK–RhoA signaling pathway. Oncogene 29, 1293–1302 (2010).
Pang, K. et al. Monitoring circulating prostate cancer cells by in vivo flow cytometry assesses androgen deprivation therapy on metastasis. Cytom. A 93, 517–524 (2018).
De Ciantis, P. D., Yashpal, K., Henry, J. & Singh, G. Characterization of a rat model of metastatic prostate cancer bone pain. J. Pain. Res. 3, 213–221 (2010).
Bosland, M. C., Schlicht, M. J., Horton, L. & McCormick, D. L. The MNU plus testosterone rat model of prostate carcinogenesis. Toxicol. Pathol. 50, 478–496 (2022).
Haldorsen, I. S. et al. Multimodal imaging of orthotopic mouse model of endometrial carcinoma. PLoS ONE 10, e0135220 (2015).
Baert, T. et al. The dark side of ID8-Luc2: pitfalls for luciferase tagged murine models for ovarian cancer. J. Immunother. Cancer 3, 57 (2015).
Rose, G. S. et al. Development and characterization of a clinically useful animal model of epithelial ovarian cancer in the Fischer 344 rat. Am. J. Obstet. Gynecol. 175, 593–599 (1996).
He, C. et al. A human papillomavirus-independent cervical cancer animal model reveals unconventional mechanisms of cervical carcinogenesis. Cell Rep. 26, 2636–2650 e2635 (2019).
Henkle, T. R. et al. Development of a novel mouse model of spontaneous high-risk hpve6/e7-expressing carcinoma in the cervicovaginal tract. Cancer Res. 81, 4560–4569 (2021).
Hamada, K., Ueda, N., Ito, M., Roth, J. A. & Follen, M. The nude rat as an orthotopic model for cervical cancer. Gynecol. Oncol. 99, S159–S165 (2005).
Koutcher, J. A. et al. MRI of mouse models for gliomas shows similarities to humans and can be used to identify mice for preclinical trials. Neoplasia 4, 480–485 (2002).
Bouckaert, C. et al. Development of a rat model for glioma-related epilepsy. Int. J. Mol. Sci. 21, 6999 (2020).
Nagarajan, P. P. et al. Lentiviral-induced spinal cord gliomas in rat model. Int. J. Mol. Sci. 22, 12943 (2021).
Shimoyama, M., Tanaka, K., Hasue, F. & Shimoyama, N. A mouse model of neuropathic cancer pain. Pain 99, 167–174 (2002).
Mao-Ying, Q.-L. et al. A rat model of bone cancer pain induced by intra-tibia inoculation of Walker 256 mammary gland carcinoma cells. Biochem. Biophys. Res. Commun. 345, 1292–1298 (2006).
Yang, H. et al. Proteomic analysis of spinal cord tissue in a rat model of cancer-induced bone pain. Front. Mol. Neurosci. 15, 1009615 (2022).
Gelbard, A. et al. An orthotopic murine model of sinonasal malignancy. Clin. Cancer Res. 14, 7348–7357 (2008).
Feron, V. J., Woutersen, R. A., van Garderen-Hoetmer, A. & Dreef-van der Meulen, H. C. Upper respiratory tract tumors in Cpb:WU (Wistar random) rats. Environ. Health Perspect. 85, 305–315 (1990).
Miller, A. L. & Roughan, J. V. Welfare assessment, end-point refinement and the effects of non-aversive handling in C57BL/6 mice with Lewis lung cancer. Animals https://doi.org/10.3390/ani12010023 (2021).
Mendoza, A. et al. A novel noninvasive method for evaluating experimental lung metastasis in mice. J. Am. Assoc. Lab. Anim. Sci. 52, 584–589 (2013).
Byhardt, R. W., Almagro, U. A., Fish, B. L. & Moulder, J. E. Development of a rat lung cancer model. Int. J. Radiat. Oncol. Biol. Phys. 10, 2125–2130 (1984).
Zhu, X. C. et al. Analgesic effects of lappaconitine in leukemia bone pain in a mouse model. PeerJ 3, e936 (2015).
Helseth, A., Siegal, G. P., Haug, E. & Bautch, V. L. Transgenic mice that develop pituitary tumors. a model for Cushing’s disease. Am. J. Pathol. 140, 1071–1080 (1992).
Chang-Wei, H., Li, Y. B., Han, X. Y., Yin, G. F. & Wang, X. R. To explore the change of motor cognitive function in pituitary tumor rats after operation. Comput. Assist. Surg. 28, 2198099 (2023).
Kim, W. G., Park, J. W., Willingham, M. C. & Cheng, S. Y. Diet-induced obesity increases tumor growth and promotes anaplastic change in thyroid cancer in a mouse model. Endocrinology 154, 2936–2947 (2013).
Snarskaya, E. S., Pylev, L. N., Akhunzyanov, A. A. & Kuznetсova, E. V. Experimental basosquamous carcinoma model in rats. BioNanoScience 7, 423–427 (2017).
Stribbling, S. M. & Ryan, A. J. The cell-line-derived subcutaneous tumor model in preclinical cancer research. Nat. Protoc. 17, 2108–2128 (2022).
Ehx, G. et al. Xenogeneic graft-versus-host disease in humanized NSG and NSG-HLA-A2/HHD mice. Front. Immunol. 9, 1943 (2018).
Lai, H. Y., Chou, T. Y., Tzeng, C. H. & Lee, O. K. Cytokine profiles in various graft-versus-host disease target organs following hematopoietic stem cell transplantation. Cell Transplant. 21, 2033–2045 (2012).
Ullman-Cullere, M. H. & Foltz, C. J. Body condition scoring: a rapid and accurate method for assessing health status in mice. Lab. Anim. Sci. 49, 319–323 (1999).
Hickman, D. L. & Swan, M. Use of a body condition score technique to assess health status in a rat model of polycystic kidney disease. J. Am. Assoc. Lab. Anim. Sci. 49, 155–159 (2010).
Burkholder, T., Foltz, C., Karlsson, E., Linton, C. G. & Smith, J. M. Health evaluation of experimental laboratory mice. Curr. Protoc. Mouse Biol. 2, 145–165 (2012).
Raja, S. N. et al. The revised International Association for the Study of Pain definition of pain: concepts, challenges, and compromises. Pain 161, 1976–1982 (2020).
Langford, D. J. et al. Coding of facial expressions of pain in the laboratory mouse. Nat. Methods 7, 447–449 (2010).
Sotocinal, S. G. et al. The Rat Grimace scale: a partially automated method for quantifying pain in the laboratory rat via facial expressions. Mol. Pain. 7, 55 (2011).
Jirkof, P. et al. Assessment of postsurgical distress and pain in laboratory mice by nest complexity scoring. Lab. Anim. 47, 153–161 (2013).
Jirkof, P. et al. Burrowing behavior as an indicator of post-laparotomy pain in mice. Front. Behav. Neurosci. 4, 165 (2010).
Turner, P. V., Pang, D. S. & Lofgren, J. L. A review of pain assessment methods in laboratory rodents. Comp. Med. 69, 451–467 (2019).
Deuis, J. R., Dvorakova, L. S. & Vetter, I. Methods used to evaluate pain behaviors in rodents. Front. Mol. Neurosci. 10, 284 (2017).
Wright-Williams, S. L., Courade, J. P., Richardson, C. A., Roughan, J. V. & Flecknell, P. A. Effects of vasectomy surgery and meloxicam treatment on faecal corticosterone levels and behaviour in two strains of laboratory mouse. Pain 130, 108–118 (2007).
Do, J. P. et al. Automated and continuous monitoring of animal welfare through digital alerting. Comp. Med. 70, 313–327 (2020).
Collins, D. E., Mulka, K. R., Hoenerhoff, M. J., Taichman, R. S. & Villano, J. S. Clinical assessment of urinary tract damage during sustained-release estrogen supplementation in mice. Comp. Med. 67, 11–21 (2017).
Pearse, G., Frith, J., Randall, K. J. & Klinowska, T. Urinary retention and cystitis associated with subcutaneous estradiol pellets in female nude mice. Toxicol. Pathol. 37, 227–234 (2009).
Guyenet, S. J. et al. A simple composite phenotype scoring system for evaluating mouse models of cerebellar ataxia. J. Vis. Exp. https://doi.org/10.3791/1787 (2010).
Gao, X. et al. in Brain Tumors Vol. 158 (ed. Seano, G.) 199–220 (Springer, 2021).
Kelp, A. et al. A novel transgenic rat model for spinocerebellar ataxia type 17 recapitulates neuropathological changes and supplies in vivo imaging biomarkers. J. Neurosci. 33, 9068–9081 (2013).
Bieler, L. et al. Motor deficits following dorsal corticospinal tract transection in rats: voluntary versus skilled locomotion readouts. Heliyon 4, e00540 (2018).
Brough, D. W., Murkin, J. T., Amos, H. E., Smith, A. I. & Turley, K. D. Comparing variability in measurement of subcutaneous tumors in mice using 3D thermal imaging and calipers. Comp. Med. 72, 364–375 (2022).
Jensen, M. M., Jorgensen, J. T., Binderup, T. & Kjaer, A. Tumor volume in subcutaneous mouse xenografts measured by microCT is more accurate and reproducible than determined by 18F-FDG–microPET or external caliper. BMC Med. Imaging 8, 16 (2008).
Czerninski, R., Amornphimoltham, P., Patel, V., Molinolo, A. A. & Gutkind, J. S. Targeting mammalian target of rapamycin by rapamycin prevents tumor progression in an oral-specific chemical carcinogenesis model. Cancer Prev. Res. 2, 27–36 (2009).
Tanaka, T., Kojima, T., Okumura, A., Yoshimi, N. & Mori, H. Alterations of the nucleolar organizer regions during 4-nitroquinoline 1-oxide-induced tongue carcinogenesis in rats. Carcinogenesis 12, 329–333 (1991).
Goetze, R. G. et al. Utilizing high resolution ultrasound to monitor tumor onset and growth in genetically engineered pancreatic cancer models. J. Vis. Exp. https://doi.org/10.3791/56979 (2018).
Glaser, G. et al. Conventional chemotherapy and oncogenic pathway targeting in ovarian carcinosarcoma using a patient-derived tumorgraft. PLoS ONE 10, e0126867 (2015).
Vitetta, E. S. et al. Tumor dormancy and cell signaling. V. Regrowth of the BCL1 tumor after dormancy is established. Blood 89, 4425–4436 (1997).
Bruckner, M. et al. Murine endoscopy for in vivo multimodal imaging of carcinogenesis and assessment of intestinal wound healing and inflammation. J. Vis. Exp. https://doi.org/10.3791/51875 (2014).
Kodani, T. et al. Flexible colonoscopy in mice to evaluate the severity of colitis and colorectal tumors using a validated endoscopic scoring system. J. Vis. Exp. 80, e50843 (2013).
Habibollahi, P. et al. Optical Imaging with a cathepsin B activated probe for the enhanced detection of esophageal adenocarcinoma by dual channel fluorescent upper GI endoscopy. Theranostics 2, 227–234 (2012).
Dassie, E. et al. Detection of fluorescent organic nanoparticles by confocal laser endomicroscopy in a rat model of Barrett’s esophageal adenocarcinoma. Int. J. Nanomed. 10, 6811–6823 (2015).
Wong, G. S. et al. Optical imaging of periostin enables early endoscopic detection and characterization of esophageal cancer in mice. Gastroenterology 144, 294–297 (2013).
El-Masry, O. S. et al. Oral intragastric DMBA administration induces acute lymphocytic leukemia and other tumors in male Wistar rats. J. Exp. Pharmacol. 14, 87–96 (2022).
Tannous, B. A. Gaussia luciferase reporter assay for monitoring biological processes in culture and in vivo. Nat. Protoc. 4, 582–591 (2009).
Delgado-SanMartin, J. et al. An innovative non-invasive technique for subcutaneous tumour measurements. PLoS ONE 14, e0216690 (2019).
Klerk, C. P. et al. Validity of bioluminescence measurements for noninvasive in vivo imaging of tumor load in small animals. Biotechniques 43, 7–13, 30 (2007).
Miller, I. S. et al. Durability of cell line xenograft resection models to interrogate tumor micro-environment targeting agents. Sci. Rep. 9, 9204 (2019).
Jarzabek, M. A. et al. Molecular imaging in the development of a novel treatment paradigm for glioblastoma (GBM): an integrated multidisciplinary commentary. Drug Discov. Today 18, 1052–1066 (2013).
Zeamari, S., Rumping, G., Floot, B., Lyons, S. & Stewart, F. A. In vivo bioluminescence imaging of locally disseminated colon carcinoma in rats. Br. J. Cancer 90, 1259–1264 (2004).
Netufo, O. et al. Refining glioblastoma surgery through the use of intra-operative fluorescence imaging agents. Pharmaceuticals 15, 550 (2022).
Christensen, J., Vonwil, D. & Shastri, V. P. Non-invasive in vivo imaging and quantification of tumor growth and metastasis in rats using cells expressing far-red fluorescence protein. PLoS ONE 10, e0132725 (2015).
Yang, N. et al. A novel GFP nude rat model to investigate tumor-stroma interactions. Cancer Cell Int. 14, 541 (2014).
Hoffman, R. M. Application of GFP imaging in cancer. Lab. Invest. 95, 432–452 (2015).
Marien, E., Hillen, A., Vanderhoydonc, F., Swinnen, J. V. & Vande Velde, G. Longitudinal microcomputed tomography-derived biomarkers for lung metastasis detection in a syngeneic mouse model: added value to bioluminescence imaging. Lab. Invest. 97, 24–33 (2017).
Nota, T. et al. Safety and feasibility of contrast-enhanced computed tomography with a nanoparticle contrast agent for evaluation of diethylnitrosamine-induced liver tumors in a rat model. Acad. Radiol. 30, 30–39 (2023).
Olson, J. D. et al. A gated-7T MRI technique for tracking lung tumor development and progression in mice after exposure to low doses of ionizing radiation. Radiat. Res. 178, 321–327 (2012).
Baier, J. et al. Influence of MRI examinations on animal welfare and study results. Invest. Radiol. 55, 507–514 (2020).
Song, H. T. et al. Rat model of metastatic breast cancer monitored by MRI at 3 tesla and bioluminescence imaging with histological correlation. J. Transl. Med. 7, 88 (2009).
Gui, Q. et al. A new rat model of bone cancer pain produced by rat breast cancer cells implantation of the shaft of femur at the third trochanter level. Cancer Biol. Ther. 14, 193–199 (2013).
Ayers, G. D. et al. Volume of preclinical xenograft tumors is more accurately assessed by ultrasound imaging than manual caliper measurements. J. Ultrasound Med. 29, 891–901 (2010).
Ghaddar, N. et al. Detection of lung tumor progression in mice by ultrasound imaging. J. Vis. Exp. https://doi.org/10.3791/60565 (2020).
Chen, J. Y. et al. Application of high-frequency ultrasound for the detection of surgical anatomy in the rodent abdomen. Vet. J. 191, 246–252 (2012).
O’Farrell, A. C. et al. Implementing systems modelling and molecular imaging to predict the efficacy of BCL-2 inhibition in colorectal cancer patient-derived xenograft models. Cancers 12, 2978 (2020).
Sun, R. et al. A radiomics approach to assess tumour-infiltrating CD8 cells and response to anti-PD-1 or anti-PD-L1 immunotherapy: an imaging biomarker, retrospective multicohort study. Lancet Oncol. 19, 1180–1191 (2018).
Aubry, K. et al. FDG-PET/CT of head and neck squamous cell carcinoma in a rat model. Mol. Imaging Biol. 11, 88–93 (2009).
Lofgren, J. et al. Analgesics promote welfare and sustain tumour growth in orthotopic 4T1 and B16 mouse cancer models. Lab. Anim. 52, 351–364 (2018).
Husmann, K. et al. Primary tumour growth in an orthotopic osteosarcoma mouse model is not influenced by analgesic treatment with buprenorphine and meloxicam. Lab. Anim. 49, 284–293 (2015).
Taylor, D. K. Influence of pain and analgesia on cancer research studies. Comp. Med. 69, 501–509 (2019).
Strohal, R. et al. Wound management with enzyme alginogels: expert consensus. Hautarzt 68, 36–42 (2017).
Chaudhary, A., Bag, S., Banerjee, P. & Chatterjee, J. Wound healing efficacy of Jamun honey in diabetic mice model through reepithelialization, collagen deposition and angiogenesis. J. Tradit. Complement. Med. 10, 529–543 (2020).
Mitchell, C. M., Salyards, G. W., Theriault, B. R., Langan, G. P. & Luchins, K. R. Evaluation of pain and distress and therapeutic interventions for rectal prolapse in mice to reduce early study removal. J. Am. Assoc. Lab. Anim. Sci. 60, 692–699 (2021).
Levin-Allerhand, J. A., Sokol, K. & Smith, J. D. Safe and effective method for chronic 17beta-estradiol administration to mice. Contemp. Top. Lab. Anim. Sci. 42, 33–35 (2003).
Fish, R., Danneman, P. J., Brown, M. & Karas, A. Anesthesia and Analgesia in Laboratory Animals (Academic Press, 2011).
Flecknell, P. Laboratory Animal Anaesthesia (Academic Press, 2015).
Foley, P. L., Kendall, L. V. & Turner, P. V. Clinical management of pain in rodents. Comp. Med. 69, 468–489 (2019).
Acknowledgements
K.C. and A.T.B. are funded by a European Union Horizon 2020 research and innovation program, ‘COLOSSUS’ (grant agreement no. 754923) and ‘GLIORESOLVE’ (grant agreement no. 101073386), Science Foundation Ireland (grants 18/RI/5759, 20/FFP-P/8884 and 20/FFP-P/8613), Irish Health Research Board (grants ILP-POR-2019-066 and ILP-POR-2022-007), Irish Higher Education Authority and North South Research Program ‘RADCOL’. Additional financial support was received from the Beaumont Hospital Foundation.
Author information
Authors and Affiliations
Contributions
Conceptualization: S.I.D.V. and E.R.H.; methodology: S.I.D.V., M.v.d.V., K.D., D.R., A.M.R., Y.D.R. and E.R.H.; writing–original draft preparation: S.I.D.V., M.v.d.V., A.O., K.D., K.C., D.R., A.M.R., Y.D.R., M.D., V.D.-M. and E.R.H.; writing–review and editing: S.I.D.V., A.T.B. and E.R.H. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Protocols thanks Neil Lipman, Patricia V. Turner and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information (download PDF )
Supplementary Note
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
De Vleeschauwer, S.I., van de Ven, M., Oudin, A. et al. OBSERVE: guidelines for the refinement of rodent cancer models. Nat Protoc 19, 2571–2596 (2024). https://doi.org/10.1038/s41596-024-00998-w
Received:
Accepted:
Published:
Version of record:
Issue date:
DOI: https://doi.org/10.1038/s41596-024-00998-w
This article is cited by
-
Harnessing PDX and PDX 2.0: the next-generation paradigm for precision oncology and translational breakthroughs
Molecular Cancer (2026)
-
haCCA: multi-module Integration of spot-based spatial transcriptomes and metabolomes
Communications Biology (2026)
-
Challenging the status quo to improve the translational potential of preclinical oncology studies
Nature Reviews Cancer (2025)
-
Spontaneous and experimental models of lymph node metastasis
Nature Protocols (2025)
-
Lymphatic collection and cell isolation from mouse models for multiomic profiling
Nature Protocols (2025)