Abstract
This article describes a Magnetic Resonance Imaging (MRI) -guided High-Intensity Focused Ultrasound (HIFU) robotic system for the treatment of uterine fibroids. The study presents the development and sensor-based accuracy assessment of the robotic system. The positioning accuracy was assessed in free space using a three-dimensional coordinate measuring machine (CMM) and verified in phantom study and ex vivo with porcine tissue. Average positioning accuracy with a standard deviation of 0.37 ± 0.17 mm was achieved with CMM, 0.9 ± 0.4 mm in the phantom study, and 0.9 ± 0.6 mm with porcine tissue. The MRI compatibility of the system was substantiated with signal-to-noise ratio (SNR) analysis. This robotic system has a positioning accuracy of millimeter level, with almost negligible interference to MRI. It has certain feasibility in the treatment of uterine fibroids. Further clinical trials are warranted to confirm therapeutic efficacy and clinical safety for uterine fibroid treatments.
Similar content being viewed by others
Introduction
With advances in medical technology and increasing patient awareness, there is a growing demand for minimally invasive treatments that enable faster postoperative recovery and reduced hospital stays. Leiomyomas, also termed uterine fibroids, are benign hormone-dependent tumors commonly found in women of reproductive age. These non-cancerous neoplasms often cause no symptoms and shrink after menopause due to declining hormone levels. However, uterine fibroids sometimes do cause problems such as heavy bleeding, pelvic pain, and infertility, for which treatment may become necessary1.
Common treatment methods include myomectomy, hormonal therapy, and uterine artery embolization (UAE). Laparoscopic myomectomy is a minimally invasive option for patients who want to keep their uterus but only works with fibroids of a certain size with risks including postoperative recurrence and cross-infection. Hormone therapy, which works by having hormone agonists to block estrogen and progesterone, can only temporarily relieve pain due to the risk of long-term side effects and only works for as long as it is used. UAE has been investigated as a minimally invasive alternative to surgical treatment of uterine fibroids. Although it can effectively reduce fibroid size, it may lead to vascular complications and a risk of recurrence2. Novel techniques such as radiofrequency ablation (RFA) and microwave ablation (MWA) have been explored for fibroid treatment, offering localized tissue destruction with minimal invasiveness. However, these thermal ablation methods may still cause complications such as tissue damage to surrounding structures3,4.
High-intensity focused ultrasound (HIFU) appears to be a safer non-invasive alternative, which is a thermo-ablative technique that treats tumors by converging ultrasound beams at a focal spot5. HIFU is widely recognized with both ultrasound-guided (US-HIFU) and MRI-guided (MRI-HIFU) systems commercially available6,7,8,9. While US-HIFU is limited by acoustic window constraints, poor soft tissue contrast, and the lack of real-time thermal monitoring. In contrast, MRI-HIFU provides superior anatomical visualization and quantitative temperature mapping, enabling precise targeting and real-time feedback during treatment. These features make MRI-HIFU particularly advantageous for treating fibroids located near sensitive structures or in patients requiring high safety and precision standards6,7,8,9. However, significant challenges arise from the electromagnetic compatibility due to the MRI environment. For the robotic system to operate safely, bidirectional MRI compatibility is required such that neither the magnetic field from MRI disrupts the robot’s performance nor the robot’s materials degrade the imaging quality of the MRI scanner10,11,12.
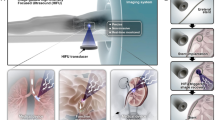
Architectural diagram of the MRI-guided HIFU robotic system for the treatment of uterine fibroids.
At present, the leading robotic MRI-guided HIFU systems approved for the clinical treatment of fibroids are either CE- and FDA-approved (ExAblate 2000, Insightec Ltd, Tirat Carmel, Israel) or CE-approved (Sonalleve MR-HIFU fibroid therapy system, Philips and Profound Medical Inc., Vantaa, Finland)13,14. The former system consists of four piezoelectric motors and one hydraulic drive, which achieves the goal of 5-DOF motion but increases the complexity of controlling due to the dual-drive system. The latter system adopts a circular treatment pattern intended to minimize the risks of over or under-treatment and incorporates real-time MRI thermometry data into the feedback loop. The use of high-density phased arrays has also been proven promising, which eliminates the need for mechanical movement to steer the ultrasound focus15. This allows for precise targeting and ablation of tissue volumes with reduced near-field heating and increased efficiency16. In terms of its mechanical design, the device employs a compact arrangement of five motors closely positioned. Though space efficient, the motors’ proximity to the scanning probe compromises the probe’s effectiveness and interferes with the MRI process, thereby introducing a notable limitation. Currently, the field of MRI-guided robotic systems still faces urgent clinical challenges, such as electromagnetic interference, limited robotic operation space, and large registration and positioning errors, all of which need to be addressed17.
In this work, we introduced an MRI compatible robotic system for uterine fibroids treatment. The main contributions included: (1) We proposed a novel mechanical design that separates the driver and transducer into distinct modules. By minimizing the driver’s interference with the HIFU probe, we ensured the MR imaging quality. Additionally, the independent movement across the five axes reduces the complexity of the robot kinematics. (2) The robot was developed with positioning accuracy validated through a Coordinate Measuring Machine (CMM) in free space. Its clinical applicability was demonstrated through phantom study and ex vivo, both in an MRI environment. (3) Electromagnetic compatibility was confirmed by analyzing the signal-to-noise ratio (SNR) of MRI acquired under varied scanning sequences, with comparisons made between the robot’s active and inactive state.
Methodology and design
System specifications
The architectural diagram of the robotic system is shown in Fig. 1. To reduce interference with MRI, all components were placed within the MRI console except for the amplifier box, main controlling box, and manipulator, which were positioned in the MRI scanning room. The components between the two rooms communicated exclusively via an optical fiber linkage. The MRI console and the robot workstation transmitted data via the local area network (LAN). The power supply was placed in the storage room.
The numerical difference between the robot’s current position and the target position was calculated in real time on the workstation and sent to the main controlling box to control the manipulator and probe. The power supply in the storage room provided all the components of the system with electricity. Additionally, a cooling circulation system actively lowered the temperature of the liquid in the working zone to ensure patient safety by preventing potential skin burns from elevated temperatures.
The robotic system was designed to provide diverse and precise acoustic pathways for the HIFU probe. To this end, three.
translational axes for anterior-posterior, lateral, and vertical movements, and two rotational axes for angulation of the probe were demanded. Based on a review of existing literature, the proposed design parameters as listed in Table 1 meet the exigencies for MRI-guided fibroid treatment16,17,18,19,20.
Architectural diagram of the manipulator in the robotic system.
Mechanical design
The robotic system is separated into three modules: the working zone, driving zone, and auxiliary zone, as marked with dashed line boxes in Fig. 2. The working zone was designed for HIFU probe mounting and independent maneuvering of the five DOFs. The driving zone encapsulates the motor units, and the auxiliary zone contains the system’s wiring.
Figure 2 highlights the driving mechanism consisting of three translational axes and two rotational axes. The forward-backward mechanism (FBM) enables the probe to advance or retreat (T1), left and right mechanism (LRM) enables left-to-right movement (T2), and the up-down mechanism (UDM) enables the probe to move vertically (T3). A probe roll rotation (PRR) mechanism (R1) enables the probe to roll and a probe pitch rotation (PPR) mechanism (R2) enables the probe to pitch, and each group of mechanisms is connected to the corresponding motor unit located in the driving zone so as to obtain motivation, and the probe connecting disk is equipped with HIFU probe, as illustrated in Fig. 3. Power transmissions are achieved via screw, nut, rods and bevel gears. The ultrasonic motors located in the driving zone power these mechanisms. The FBM mechanism (T1) connects the working and driving zones via pallet slide rails and dovetail guide rails. The driving zone pallet is connected to the working zone pallet by the connecting rod, and all components on the working zone, including the HIFU probe, follow the driving zone pallet to move in unison.
The PRR (R1) and PPR (R2) mechanisms of the probe transmit roll and pitch rotations through a sequential mechanical chain comprising a drive shaft, rotary sleeve, slider-crank mechanism, four-bar linkage, and probe-connecting disk. Limit switches establish the initial reference position, while rotary encoders provide closed-loop positioning feedback for precise motion control.
PPR and PRR mechanisms with transformation system.
Most mechanical parts of the manipulator were made with polyoxymethylene (POM) resin, non-magnetic copper, and 3D printed (Polylactic acid) PLA. Gears and certain guide rods were made with Hpb59-1 Lead Brass. Ultrasonic motors were from NUAA (NUAA Super Control Technology, Nanjing, China), and optical encoders were from US Digital (US Digital, California, US).
Forward and inverse kinematics
The kinematics model of the robot in Fig. 4 follows the Denavit-Hartenberg (D-H) convention with parameters listed in Table 2. In this configuration, the global frame is denoted {G}, and five frames starting from the robot’s base are {0}, {1}, {2}, {3} and {4}, with the focal point denoted {P}. Parameter d1 is the forward and backward translation distance, d2 is the left and right translation distance, θ3 is the roll rotation angle, θ4 is the angle for vertical movement, and θ5 is the pitch rotation angle. Parameters a3, a4, a5, d3 are fixed lengths intrinsic to the structural design, with a3 = 94 mm, a4 = 94 mm, a5 = 93 mm, and d3 = 110.5 mm from the CAD model. The transformation from {G} to {P}, denoted \(^{G} T_{P}\), requires the relative pose of {G} to {P}, which is directly determined based on workspace, and {P} to {0}, which be established through forward kinematics as shown in Eq. (1).
The latter part is a kinematic chain of the 5-DOF poses as
with \(^{0} T_{P}\), Which is now denoted as
the right-handed analytical solution can be calculated from.
Kinematic model of the robot.
the focal point using inverse kinematics in MATLAB as shown in Eq. (5).
when measurements are made, the standard deviation for a single marker distance error \({\sigma}_{epsilon}\) is calculated as
where \(\epsilon_{i}\) is the single trial error and \(\hat{\epsilon}\) is the mean error. N is the number of the measurements.
Registration overview. (a) Definition of MRI coordinate system. (b) Robot coordinate system on the probe. (c) The fiducial frame for registration. (d) Coronal and sagittal plane images during registration.
MRI registration
A fiducial frame was designed for the extrinsic registration between the robot and the MRI coordinate system shown in Fig. 5a and b. The markers, labeled T1 to T12, were 3D printed using photosensitive resin, a material that remains signal-silent during MRI scanning so that the markers can be visible on the image as a darker spot as illustrated in Fig. 5c. The MRI scanning sequence Pos-Cor-SE is used with 300 ms time of repetition (TR), 14 ms echo time (TE), slice thickness of 3 mm, and NEX = 1. (All MRI scans and sequences used in this study were performed on a GE Discovery MR750w 3.0T system. The sequence Pos-Cor-SE (Positioning Coronal Spin Echo), is a conventional spin echo sequence commonly used for geometric localization due to its high spatial fidelity and relatively low sensitivity to magnetic field inhomogeneities, making it suitable for robot-to-image registration tasks.)
To determine the transformation matrix between the MRI scanner and the robot, both of which were in the Cartesian coordinate, at least four non-coplanar points were needed. The registration process started with manually locating six points on the coronal plane, C1 to C6, and four non-coplanar points from the eight points labeled S1 to S8 on the sagittal plane as depicted in Fig. 5d. Two planes labeled \({\phi}_{1}\) and \({\phi}_{2}\) can be interpolated using points S1, S2, S5, S6 and S3, S4, S7, S8, respectively. Since the points on the two planes overlay, Fig. 5d only shows S1 to S4 on the top plane. Plane functions \({\phi}_{j}\) are derived as
Denoting the location of Ti, i = 1,2,···,12 in frame {M} and {R} as \(T_{i}^{{\left\{ {{\text{frame}}} \right\}}} = [x_{i} ,y_{i} ,z_{i} ,1]^{T}\), the transformation matrix between the robot and the MRI scanner can be calculated as
The fiducial registration error (FRE) is measured to be 0.23 ± 0.09 mm with the similar method detailed in21‚22.
HIFU setup
In this study, a 128-channel spherical phased array transducer was specifically designed for the treatment of uterine fibroids. The transducer operates at a frequency of 1.1 MHz, with a probe diameter of 120 mm and a spherical radius of 150 mm, as shown in Fig. 6a. The element arrangement(adjusted Fermat spiral arrangement) of the transducer is illustrated in Fig. 6b. The maximum acoustic power output of the transducer is 500 W, with the maximum sidelobe level not exceeding − 8 dB. The acoustic pressure gain distribution is presented in Fig. 6c and d. The generated focal region forms an ellipsoidal shape with a short axis of 5 ± 0.5 mm (W in the figure) and a long axis of 16 ± 0.7 mm (L in the figure), as depicted in Fig. 6a and e. The power amplifier used to drive the transducer was manufactured by Shende Noninvasive Era Medical Technology Co., Ltd. (Model: UIA-AMPC, Shende Noninvasive Era Medical Technology Co., Ltd., Nantong, China). It was placed inside the MRI suite during operation, and the electromagnetic interference generated was within an acceptable range.
HIFU setup: (a) Probe geometric dimensions. (b) Distribution of the 128 array elements. (c) X-axis sound pressure gain; (d) Z-axis sound pressure gain; (e) Probe focal size.
Experiments and results
System free space validation
The robot’s workspace is shown in Fig. 7a. Twenty-seven target points, labeled from A1 to I3, were carefully selected to span critical regions of the entire workspace. Point E2 was defined as the origin of the workspace for the convenience of measurement. To measure the hypothetical focal point of the HIFU probe, a measuring bracket was 3D printed with a red dot at the tip indicating the focal point, as shown in Fig. 7b and c.
Workspace of the robotic system and CMM experimental setup. (a) Workspace of the robotic system. (b) Measurement experimental setup in free space. (c) Measurement process demonstrated using CMM.
We used a 3-dimensional Coordinate Measuring Machine (CMM)(Tornado NCA153010, Qingdao, China) to validate the positioning accuracy of the robot. The CMM performance was tested before making measurements. The mean error 0.08 ± 0.03 mm was within the maximum permissible error of the machine.
The parameters were calculated and set in advance with Eq. (2) to (4). Each point, from A1 to I3, was measured and recorded using the CMM sequentially, as shown in Fig. 7a. This process was repeated five times, and the position error distribution was summarized in Fig. 8a and b. The mean accuracy was 0.37 ± 0.17 mm in free space.
Experimental results of the positioning accuracy with CMM. (a) Error distribution from A1 to D2. (b) Error distribution from E2 to I3.
Image-guided phantom study
To assess the robot’s positioning accuracy in an MRI setting, we conducted a phantom study using translucent acrylic sheets (ZUVAS, Shenzhen, China) as set up in Fig. 9. Acrylic sheets are capable of gauging the position of the focal point precisely, which makes measurement easier. An acrylic phantom was positioned on a stand within a water-filled testing bucket on top of the manipulator. The manipulator was put in the customized bed. The MRI’s fiducial frame was scanned to register the robotic system. The phantom was then scanned to identify target points as the sequence shown in Fig. 10a from S1 to S8. The probe, after focusing on these targets, left visible sintering markers on the sheets as shown in Fig. 10b and c. On the phantom, we set up a coordinate system and employed a vernier caliper to determine the position of the center of the circumscribed circle around the irregular shape. Five independent trials were conducted for each marker, and the result is summarized in Table 3. A mean accuracy of 0.9 ± 0.4 mm was achieved.
Acrylic phantom experimental setup. (The manipulator was put in the customized bed).
HIFU ablation results. (a) Phantom coordinate and targets. (b), (c) Measurement with vernier caliper.
Ex vivo porcine tissue study
To further verify the potential for clinical experiments of the robot system, we conducted an ex vivo experiment with porcine tissue shown in Fig. 11 To better handle the tissue after ablation, we designed a specialized container for holding the tissue and placed it on top of the robot. After registration, the robot focused the probe according to a 15 × 40 mm rectangular frame and performed ablation in the order from T1 to T6 in Fig. 12a. After the ablation, the porcine tissue was cut at the focal plane and two rulers were placed for measurements as Fig. 12b. When taking measurements, we took the center of the circle that encloses the focal point to be the measuring point and consistently used the center of T1 as the reference point. The experiment was repeated five times. A mean accuracy of 0.9 ± 0.6 mm was achieved, with positioning distribution summarized in Fig. 12c.
MRI ex vivo porcine tissue experimental setup with the robotic system.
Results of ex vivo porcine tissue. (a) Planned target on MRI (b) Tissue after ablation. (c) The error distribution.
of the target.
MRI compatibility study
Two MRI sequences were chosen to scan the same position of the robot under conditions where the robot was powered on and off. In the powered-on state, only the HIFU subsystem (transducer, amplifier, and water cooling) was active during MRI scanning, while the motors and encoders remained off. In the powered-off state, all electrical components were completely shut down. The SNR under each condition was then calculated. Sequence 1, a Coronal Single-Shot Fast Spin Echo (Cor-SSFSE) sequence (TR = 1356 ms, TE = 31.5 ms, slice thickness = 7 mm, NEX = 1), was for treatment planning. SSFSE is a rapid spin-echo sequence that enables high-speed anatomical imaging with good soft tissue contrast, often used for screening and planning in pelvic imaging. Sequence 2, a Positioning Sagittal Spin Echo (Pos-Sag-SE) sequence (TR = 300 ms, TE = 14 ms, slice thickness = 3 mm, NEX = 1), was used for robot-to-image registration. This conventional spin echo sequence provides high spatial accuracy and is often utilized for localization or alignment due to its geometric fidelity. A decrease of 7.34 and 6.21% in SNR ratio was measured with sequence 1 and sequence 2, respectively. The calculation method used is the same as in21‚22. Neither diagnostic quality of the acquired MRI deteriorated as shown in Fig. 13.
Results of MRI compatibility study. (a) Sequence 1 with robot off. (b) Sequence 1 with robot on. (c) Sequence 2 with robot off. (d) Sequence 2 with robot on.
Discussion
The paper presents a 5-DOF MRI compatible robotic system. Each axis can be controlled independently within a large workspace (100 × 90 × 50 mm in translation and 60° × 60° in rotation). A free space positioning accuracy of 0.37 ± 0.17 mm was measured with a 3-dimensional CMM, which is on par or better (< 0.5 mm) than comparable MRI-guided robots in the existing literature23,24,25,26.
Sub-millimeter precision is increasingly recognized as the benchmark for many clinical applications, including tumor treatment, neuromodulation, and thrombus ablation. The 5-DOF MRI-guided interventional radiology robot developed by Hungr et al. showed a positioning accuracy of within 5 mm for percutaneous needle interventions18 and the ultrasound Imaging-Guided system introduced by An et al. achieved an accuracy of 1.32 ± 0.58 mm27.
The phantom study indicated a positioning accuracy of 0.9 ± 0.4 mm in an MRI setting. The phantom used in the study was made with translucent acrylic plates so that the focal point was visible. Minimal deformation occurred during the process.
MRI ex vivo experiment measured an average error of 0.9 ± 0.6 mm. The positioning accuracy of the robot in this study was still at the millimeter level and comparable to the same type of robot5. However, in this study, our ultimate goal was to use HIFU to ablate tissues. Since the focusing area of HIFU also had an error margin, a 1 mm positioning accuracy is acceptable. Furthermore, we used the temperature information generated by HIFU during its operation as an auxiliary means to determine whether the positioning point had exceeded the target range. Despite the observed variation when juxtaposed with the CMM result, the achieved accuracy remained within the acceptable threshold of 1 mm. This level of precision is particularly relevant in the context of HIFU treatments, where ultrasound-induced phenomena such as reflections, refractions, and scattering inherently introduce focal point errors.
The chosen materials were either MR safe or MR conditional with an intent to minimize the robot’s electromagnetic interference with the MRI scanner. The modularized design that separates the probe from the actuators significantly decreased the impact of electrical disturbance on MRI. A 7.34 and 6.21% decrease in SNR was measured when the robot was on with two different MRI scanning sequences. This confirms that the robot’s electronics still introduced some unwanted signals to the MRI’s receiving coil. However, as seen in the results in Fig. 13, the variation neither affected the registration process nor the treatment plan. In summary, the decrease in the SNR is acceptable.
Despite the high positioning accuracy and minimal image interference demonstrated by the HIFU robotic system, several limitations remain. First, this design adopts a large variety of spur gears, bevel gears, and turbine worm screws. Though the position can be corrected by encoders and limit switches without affecting the positioning accuracy, friction-induced deviations could accumulate over time during robot movement. The complex mechanical structure would also imply a tedious installation process. Several factors could impact the positioning accuracy of the robot. (1) HIFU Probe error: Inaccuracies may arise from the imprecise installation of the piezoelectric transducer or during the phase-correction process; either could cause unwanted shifts of the focal point. (2) Registration error: Robot-MRI registration is a manual process susceptible to human error. (3) Fabrication and installation error: Deviations in the fabrication and assembly of robotic parts could accumulate and affect accuracy.
Conclusion
This paper introduces a 5-DOF MRI compatible HIFU robot for uterine fibroids treatment. The robot has a focal point positioning accuracy of millimeter level in MRI and negligible interference with MRI. It has certain feasibility in the treatment of uterine fibroids. Further clinical trials are warranted to confirm therapeutic efficacy and clinical safety for uterine fibroid treatments.
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Stewart, E. A. et al. Uterine fibroids. Nat. Rev. Dis. Prim.. 2 (1), 1–18 https://doi.org/10.1038/nrdp.2016.43 (2016).
Giuliani, E., As-Sanie, S. & Marsh, E. E. Epidemiology and management of uterine fibroids. Int. J. Gynecol. \& Obstet. 149 (1), 3–9. https://doi.org/10.1002/ijgo.13102 (2020).
Lee, B. B. & Yu, S. P. Radiofrequency ablation of uterine fibroids: A review. Curr. Obstet. Gynecol. Rep.. 5(4), 318–324. https://doi.org/10.1007/s13669-016-0183-x (2016)
Ierardi, A. M. Percutaneous high frequency microwave ablation of uterine fibroids: Systematic review. BioMed. Res. Int.. 2018 2360107. https://doi.org/10.1155/2018/2360107 (2018).
Gunderman, A., Montayre, R., Ranjan, A. & Chen, Y. Review of robot-assisted HIFU therapy. Sensors. 23(7), 3707. https://doi.org/10.3390/s23073707 (2023).
Verpalen, I. M. et al. Magnetic resonance-high intensity focused ultrasound (MR-HIFU) therapy of symptomatic uterine fibroids with unrestrictive treatment protocols: A systematic review and meta-analysis. Eur. J. Radiol. 120, 108700. https://doi.org/10.1016/j.ejrad.2019.108700 (2019).
Wood, B. J. et al. ``CT and ultrasound guided stereotactic high intensity focused ultrasound (HIFU). In: AIP Conference Proceedings, 829(1), 122–126, American Institute of Physics. https://doi.org/10.1063/1.2205450 (2006).
Bucknor, M. D. et al. MRI-guided high-intensity focused ultrasound ablation of bone: Evaluation of acute findings with MR and CT imaging in a swine model. J. Magn. Reson. Imaging. 40 (5), 1174–1180. https://doi.org/10.1002/jmri.24451 (2014).
Copelan, A., Hartman, J., Chehab, M. & Venkatesan, A. M. High-intensity focused ultrasound: Current status for image-guided therapy. In: Seminars in Interventional Radiology, Thieme Medical Publishers. 32(4) 398–415. https://doi.org/10.1055/s-0035-1564793 (2015).
Su, H. et al. State of the art and future opportunities in mri-guided robot-assisted surgery and interventions. Proc. IEEE. Inst. Electr. Electron. Eng. 110(7) 968–992. https://doi.org/10.1109/jproc.2022.3169146 (2022).
Li, K., Bai, J., Chen, Y. & Ji, X. Experimental evaluation of targeting accuracy of an ultrasound-guided phased-array high-intensity focused ultrasound system. Appl. Acoust. 141, pp. 19–25, (2018). https://doi.org/10.1016/j.apacoust.2018.06.011
Wu, H., Shen, G., Su, Z. & Chen, Y. A new FPGA-driven P-HIFU system with harmonic cancellation technique. In: AIP Conference Proceedings. 1816(1) https://doi.org/10.1063/1.4976595. AIP Publishing. (2017).
Tempany, C. M. et al. MR imaging-guided focused ultrasound surgery of uterine leiomyomas: A feasibility study. Radiology. 226(3) 897–905. https://doi.org/10.1148/radiol.2271020395 (2003).
Venkatesan, A. M. et al. Magnetic resonance imaging–guided volumetric ablation of symptomatic leiomyomata: Correlation of imaging with histology. J. Vasc. Interv. Radiol. 23 (6), 786–794. https://doi.org/10.1016/j.jvir.2012.02.015 (2012).
Aslani, P. et al. and K. Hynynen. A fully electronically steerable therapeutic ultrasound phased array with MR-guidance. IEEE Trans. Biomed. Eng. 71(2), 574–582. https://doi.org/10.1109/tbme.2023.3309540 (2024).
Chopra, R., Curiel, L., Staruch, R., Morrison, L. & Hynynen, K. An MRI-compatible system for focused ultrasound experiments in small animal models. Med. Phys. 36(5), 1867–1874. https://doi.org/10.1118/1.3115680 (2009)
Huang, S. et al. MRI-guided robot intervention—current state-of-the-art and new challenges. Med-X. 1(1), 4. (2023).
Hungr, N., Bricault, I., Cinquin, P. & Fouard, C. Design and validation of a CT- and MRI-guided robot for percutaneous needle procedures. IEEE Trans. Robot. 32 (4), 973–987. https://doi.org/10.1109/TRO.2016.2588884 (2016).
Dai, J. et al. July, A robotic platform to navigate mri-guided focused ultrasound system. IEEE Robot. Autom. Lett. 6(3) 5137–5144. https://doi.org/10.1109/LRA.2021.3068953(2021).
Nankani, A. et al. Body-mounted MR-HIFU robotic system: Mechanical design and accuracy evaluation. In: 57th Annual Conf. Inform. Sci. Syst. (CISS). 1–6. https://doi.org/10.1109/CISS56502.2023.10089665 (2023).
Liu, D., Shen, G., Tang, N., Lu, H. & Wei, B. Robotic system for magnetic resonance imaging-guided high‐intensity focus ultrasound application: Feasibility of breast fibroadenoma treatment. Int. J. Med. Rob. Comput. Assist. Surg. 19 (4), e2519https://doi.org/10.1002/rcs.2519 (Apr. 2023).
Liu, D. et al. A magnetic resonance conditional robot for lumbar spinal injection: Development and preliminary validation’’. Int. J. Med. Rob. Comput. Assist. Surg. 20 (1). https://doi.org/10.1002/rcs.2618 (2024). e2618.
Li, G. et al. A fully actuated body-mounted robotic assistant for MRI-guided low back pain injection. In: 2020 IEEE International Conference on Robotics and Automation (ICRA), pp. 5495–5501, (2020). https://doi.org/10.1109/ICRA40945.2020.9197534. IEEE.
Li, G. et al. Body-mounted robotic assistant for MRI-guided low back pain injection. Int. J. Comput. Assist. Radiol. Surg. 15 (2), 321–331. https://doi.org/10.1007/s11548-019-02080-3 (2020).
Li, G. et al. Fully actuated body-mounted robotic system for MRI-guided lower back pain injections: Initial phantom and cadaver studies.IEEE Robot. Autom. Lett. 5(4), 5245–5251, https://doi.org/10.1109/LRA.2020.3007459(2020)
Wu, D. et al. Remotely actuated needle driving device for MRI-guided percutaneous interventions. In: 2019 International Symposium on Medical Robotics (ISMR), pp. 1–7. https://doi.org/10.1109/ISMR.2019.8710176. (2019) IEEE.
An, C. Y., Syu, J. H., Tseng, C. S. & Chang, C. J. An ultrasound imaging-guided robotic HIFU ablation experimental system and accuracy evaluations. Appl. Bion. Biomech. 2017,(1) 5868695. https://doi.org/10.1155/2017/5868695 (2017)
Acknowledgements
This work was supported by the National Key Research and Development Program of the Ministry of Science and Technology of China (Grant No. 2022YFC2406900), the National Natural Science Foundation of China (Grants Nos. 81727806, 11774231), the Ningbo 2025 Key Research Program (Grant No. 2019B10065), the National Natural Science Foundation of China (Grants No. 82271969), the Project of Shanghai Education Commission (Grant No. 202101070002E00085), and the Grant from the Shanghai Hospital Development Center (Grant No. SHDC22022310-A).
Author information
Authors and Affiliations
Contributions
Conceptualization, Depeng Liu, methodology, Xiaorui Yin, software, Maoyun Zhao, validation, Xuhui Fan, formal analysis, Depeng Liu, investigation, Ming Li, resources, Han Wang, Guofeng Shen, data curation, Maoyun Zhao, writing—original draft preparation, Depeng Liu, writing—review and editing, Depeng Liu, Maoyun Zhao, visualization, Depeng Liu, supervision, Han Wang, Guofeng Shen, project administration, Depeng Liu, funding acquisition, Han Wang, Guofeng Shen. All authors have read and agreed to the version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Liu, D., Zhao, M., Fan, X. et al. MRI guided HIFU robotic system application in feasibility study for treating uterine fibroids. Sci Rep 15, 40829 (2025). https://doi.org/10.1038/s41598-025-24562-y
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-24562-y