Abstract
LC2767, a mix of Lactiplantibacillus plantarum LC27 and Bifidobacterium longum LC67, alleviates high-fat diet- or alcohol-induced liver injury and steatosis in mice. In the present study, we examined the action mechanism of LC2767 on lipopolysaccharide (LPS)-, LPS/D-galactosamine (LGc)-, or LPS/thioacetamide (LTc)-induced liver damage and fibrosis in mice. Short-termly or long-termly intraperitoneal injection of LPS, LGc, or LTc caused liver damage and fibrosis in mice: they increased alanine transaminase (ALT), aspartate transaminase (AST), and γ-glutamyl transpeptidase (γ-GTP) in the blood and α-smooth muscle actin (SMA) and tumor necrosis factor (TNF)-α expression and NF-κB activation in the liver. Short-termly orally gavage of LPS also caused liver damage. However, oral administration of LC2767 significantly reduced LPS- or LGc-, or LTc-induced ALT, AST, and γ-GTP levels in the blood. LC2767 also suppressed LPS- or LGc-induced collagen-1, α-SMA, TNF-α, CYP7A1, tissue inhibitor of metalloproteinase (TIMP)-1, and matrix metalloproteinase (MMP)-14 expression, NF-κB activation, non-alcoholic fatty liver disease activity score, and fibrosis score in the liver, and TNF-α expression and NF-κB activation in the colon, while LPS- or LGc-suppressed farnesoid X receptor (FXR) expression was increased in the liver and colon. Furthermore, LC2767 alleviated LPS-induced gut dysbiosis: it increased Akkermansiaceae population and decreased LPS-producing Christensenellaceae, Porphyromonadaceae, and Rhodospirillaceae populations. These findings suggest that LC2767 can alleviate liver damage and fibrosis by regulating NF-κB activation, FXR expression, and gut microbiota.
Similar content being viewed by others
Introduction
Liver damage is caused by a number of factors, including viral infections, cancers, genetic predispositions, toxin exposure (e.g., alcohol), and excessive high-fat intake1,2. Moreover, these factors induce endotoxin-rich gut dysbiosis. In the United States, non-alcoholic fatty liver disease (NAFLD) is the most common liver disorder, affecting an estimated 20% to 30% of the adult population3,4,5. Of those with NAFLD, approximately 20% can progress to non-alcoholic steatohepatitis (NASH), a more severe form of the disease affecting around 5% of American adults6. NASH is strongly associated with an increased risk of developing advanced fibrosis and liver cirrhosis5,7.
Gut dysbiosis, particularly characterized by the overproduction of endotoxins such as lipopolysaccharide (LPS), has been identified as a key factor in the progression of liver damage and fibrosis3,8,9. LPS is overproduced in response to a high-fat diet and stresses10,11,12. Chronic exposure to LPS leads to inflammation in both the gut and liver13. Furthermore, gut dysbiosis contributes to the increased deconjugation of bile acids, which exacerbates conditions such as NAFLD and NASH14,15.
Live biotherapeutic products including probiotics have shown potential in alleviating liver damage caused by LPS or LPS/D-galactosamine (LGc) by inhibiting NF-κB activation and preserving the intestinal barrier16,17,18. Lactobacillus rhamnosus GG, for example, improves liver injury in rats by enhancing intestinal barrier integrity19. Lactiplantibacillus plantarum LC27, Bifidobacterium longum LC67, and their mix (LC2767) reduce LPS-, high fat diet-, or alcohol-induced liver injury and steatosis by modulating NF-κB and AMP-activated kinase (AMPK) signaling pathways9,20,21. Despite these findings, the precise mechanisms of LBPs that confer protection against liver damage and fibrosis remain unclear.
Therefore, the present study aimed to investigate the action mechanism of LC2767 in mice with liver damage and fibrosis induced by LPS, LGc, or LPS/thioacetamide (LTc).
Results
Effect of LC2767 on liver damage and colitis in mice intraperitoneally injected with LPS
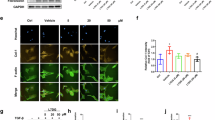
First, to investigate whether the mix of L. plantarum LC27 and B. longum LC67 could inhibit the secretion of alanine transaminase (ALT) and aspartate transaminase (AST) in LPS-stimulated HepG2 cells, we mixed LC27 and LC67 in ratios of 9:1, 3:1, 1:1, 1:3, and 1:9 and examined their effects in LPS-stimulated HepG2 cells (Supplement Fig. S1). They decreased AST, ALT, and lactate dehydrogenase (LDH) levels dose-dependently. Among the tested combinations, the 3:1 ratio of LC27 to LC67 (LC2767) showed the strongest effect in lowering LPS-induced AST, ALT, and LDH levels. LPS also induced NF-κB activation (p-p65/p65) and suppressed farnesoid X receptor (FXR) expression in Caco2 cells (Supplement Fig. S2 and Table S1). LC2767 strongly increased LPS-suppressed FXR expression, while LPS-induced NF-κB activation and TNF-α expression weakly decreased.
Therefore, we examined the effects of LC2767, Escherichia coli, and obeticholic acid on liver injury and colitis in mice intraperitoneally injected with LPS (Fig. 1A-E, Supplement Fig. S3A). LPS injection led to elevated levels of AST, ALT, γ-glutamyl transpeptidase (γ-GTP), total bile acid (TBA), total cholesterol (TCh), and interleukin (IL)-6 in the blood. However, oral administration of LC2767 significantly reduced LPS-induced AST, ALT, γ-GTP, TBA, TCh, and IL-6 levels. Of these, the efficacy of LC2767 at a dose of 1 × 109 CFU/mouse/day was comparable with that of obeticholic acid. Intraperitoneal injection of LPS also led to an increase in the toll-like receptor 4 (TLR4), tumor necrosis factor (TNF)-α, α-smooth muscle actin (SMA), collagen type 1 (collagen1), and cholesterol 7 α-hydroxylase (CYP7A1) expression in the liver to 204.8%, 199.2%, 276.2%, 171.7%, and 252.7% of LPS-untreated NC group, respectively (Fig. 1F-O, Supplement Fig. S3B–F and Table S2). LPS also increased NF-κB+F4/80+ and α-SMA+GFAP+ cell populations in the liver. However, LPS treatment decreased FXR expression to 40.1% of NC. Concurrently, there was a decrease in small heterodimer partner (SHP) expression and AMP-activated kinase (AMPK) phosphorylation. Oral administration of LC2767 most potently reduced LPS-induced TLR4 and TNF-α expression by 62.9% and 43.4%, respectively. LC2767 also suppressed LPS-induced NF-κB activation, and the NF-κB+F4/80+ cell population, followed by obeticholic acid. E. coli did not suppress their expressions. Both LC2767 and obeticholic acid significantly downregulated LPS-induced expression of α-SMA, collagen1, and CYP7A1, as well as the α-SMA+GFAP+ cell population. LC2767 increased LPS-suppressed FXR expression by 320.5%. LC2767 also increased expression of SHP and bile salt export pump (BSEP), along with enhancing AMPK activation.
Effects of LC2767 on liver damage in mice intraperitoneally injected with LPS. Effects on AST (A), ALT (B), γ-GTP (C), TCh (D), and TBA (E) levels in the blood. Effect on LPS-induced TLR4 (F), TNF-α (G), α-SMA (H), collagen1 (I), FXR (J), SHP (K), CYP7A1 (L), and BSEP (M) expression (assessed by qPCR), AMPK activation, NF-κB activation, and α-SMA expression (N, assessed by immunoblotting), α-SMA+GFAP+ and NF-κB+F4/80+ cell populations (O, assessed by immunofluorescence staining) in the liver. LC2767 at doses of 1 × 108 (LCL) and 1 × 109 CFU/mouse (LCH), E. coli at a dose of 1 × 109 CFU/mouse (Ec), obeticholic acid at a dose of 5 mg/kg (Oca), and saline (sLi) were orally administered once a day for 5 days to mice that were intraperitoneally injected with LPS for 5 days. NC group was treated with saline. Data are shown in mean ± SD (n = 8). #p < 0.05 vs. NC. *p < 0.05 vs. sLi (LPS).
Intraperitoneal exposure to LPS caused colon shortening and resulted in elevated levels of TLR4 and TNF-α in the colon to 241.0% and 183.6% of NC, respectively (Fig. 2, Supplement Fig. S3G–M and Table S3). LPS also increased NF-κB+CD11c+ cell population. FXR expression was suppressed to 37.9% of NC by LPS treatment. Oral administration of LC2767 partially recovered LPS-induced colon shortening. LC2767 also suppressed LPS-induced TLR4 and TNF-α expression in the colon by 60.8% and 48.6%, respectively, while increasing LPS-suppressed FXR expression by 217.0%. Additionally, LC2767 decreased LPS-induced NF-κB+CD11c+ cell population. The efficacy of LC2767 at a dose of 1 × 109 was the most potent.
Effects of LC2767 on LPS-induced colitis in mice. Effect on TLR4 (A, assessed by qPCR), TNF-α (B, assessed by ELISA), and FXR expression (C, assessed by qPCR), AMPK and NF-κB activation (D, assessed by immunoblotting) and NF-κB+CD11c+ cell population (E, assessed by immunofluorescence staining) in the colon. LC2767 at doses of 1 × 108 (LCL) and 1 × 109 CFU/mouse (LCH), E. coli at a dose of 1 × 109 CFU/mouse (Ec), obeticholic acid at a dose of 5 mg/kg (Oca), and saline (sLi) were orally administered once a day for 5 days to mice that were intraperitoneally injected with LPS for 5 days. NC group was treated with saline. Data are shown in mean ± SD (n = 8). #p < 0.05 vs. NC. *p < 0.05 vs. sLi.
Effect of LC2767 on liver damage and colitis in mice orally gavaged with LPS
We next explored the effect of LC2767 on liver damage and colitis in mice orally gavaged with LPS for 5 days (Fig. 3). Orally gavaged LPS led to an increase in AST, ALT, γ-GTP, TCh, and TBA levels in the blood (Fig. 3A–E). However, oral administration of LC2767 significantly reduced these LPS-induced AST, ALT, γ-GTP, TCh, and TBA levels in the blood.
Effect of LC2767 on liver damage-related biomarker levels in mice orally exposed to LPS. Effect on AST (A), ALT (B), γ-GTP (C), TCh (D), and TBA (E) in the blood. Effect on TLR4 (F), TNF-α (G), α-SMA (H), collagen1 (I), FXR (J), SHP (K), CYP7A1 (L), and BSEP (M), occludin (N), ZO-1 (O), and claudin-1 (P) expression (assessed by qPCR), AMPKa activation, NF-κB activation and α-SMA expression (Q, assessed by immunoblotting) and α-SMA+GFAP+ and NF-κB+F4/80+ cell populations (R) in the liver. LC2767 at a dose of 1 × 109 CFU/mouse (LCH) and saline (sLo) were orally administered once a day for 5 days to mice that were orally gavaged with LPS for 5 days. NC group was treated with saline. Data are shown in mean ± SD (n = 8). #p < 0.05 vs. NC. *p < 0.05 vs. sLo.
Oral exposure to LPS upregulated TLR4, TNF-α, α-SMA, and CYP7A1 expression to 184.4%, 146.4%, 143.1%, and 244.9% of NC, respectively, while FXR expression downregulated to 52.4% of NC. LPS also increased NF-κB activation, and NF-κB+F4/80+ and α-SMA+GFAP+ cell populations in the liver, while AMPK activation (phosphorylation) was reduced (Fig. 3F–R, Supplement Fig. S4A–E and Table S4). However, oral administration of LC2767 significantly suppressed the LPS-induced TLR4, TNF-α, α-SMA, collagen1, and CYP7A1 expression by 45.3%, 34.6%, 22.6%, and 27.6%, respectively. LC2767 also decreased LPS-induced NF-κB activation and α-SMA+GFAP+ and NF-κB+F4/80+ cell populations. Additionally, LC2767 increased LPS-suppressed FXR expression by 83.4%. Furthermore, LC2767 increased LPS-suppressed SHP, BSEP, ZO-1, claudin-1, and occludin expression.
Oral exposure to LPS caused colon shortening and colitis: it increased TLR4 and TNF-α expression in the colon to 129.8%% and 246.4% of NC, respectively, while FXR expression decreased to 50.2% of NC (Fig. 4, Supplement Fig. S4F–I and Table S5). LPS also increased NF-κB+CD11c+ cell population in the colon, while AMPK activation were reduced. Oral administration of LC2767 alleviated LPS-induced colon shortening. LC2767 also suppressed LPS-induced TLR4 and TNF-α expression in the colon by 21.4% and 43.9%, respectively, while increasing LPS-suppressed FXR expression by 55.4%. Additionally, LC2767 decreased LPS-induced NF-κB+CD11c+ cell population and increased LPS-suppressed colon length and AMPK activation.
Effects of LC2767 on colitis-related biomarker levels in mice orally exposed to LPS. Effects on TLR4 (A, assessed by qPCR), TNF-α (B, assessed by ELISA), and FXR expression (C, assessed by qPCR), AMPK and NF-κB activation (D, assessed by immunoblotting) and NF-κB+CD11c+ cell population (E, assessed by immunofluorescence staining) in the colon. LC2767 at a dose of 1 × 109 CFU/mouse (LCH) and saline (sLo) were orally administered once a day for 5 days to mice that were orally gavaged with LPS for 5 days. NC group was treated with saline. Data are shown in mean ± SD (n = 8). #p < 0.05 vs. NC. *p < 0.05 vs. sLo.
Effect of LC2767 on liver damage and colitis in mice long-termly, intraperitoneally injected with LPS
We examined the effects of LC2767 and obeticholic acid on liver damage and colitis in mice subjected to long-term LPS exposure. Long-termly intraperitoneal exposure to LPS resulted in elevated levels of AST, ALT, γ-GTP, TBA, TCh, TNF-α, and IL-6 in the blood (Fig. 5A–E, Supplement Fig. S5A). However, oral administration of LC2767 at doses of 1 × 108 and 1 × 109 CFU/mouse significantly reduced elevated levels of these biomarkers. Similarly, obeticholic acid at a dose of 5 mg/kg significantly decreased LPS-induced levels of AST, ALT, γ-GTP, TBA, and TCh, while TNF-α and IL-6 expression were weakly reduced compared to those of LC2767. Of these, LC2767 at a dose of 1 × 109 CFU/mouse showed the strongest inhibition.
Effect of LC2767 on liver injury and fibrosis-related biomarker levels in mice longtermly, intraperitoneally exposed to LPS. Effect on AST (A), ALT (B), γ-GTP (C), TCh (D) and TBA levels (E) in the blood. Effect on TLR4 (F), TNF-α (G), α-SMA (H), collagen1 (I), FXR (J), SHP (K), CYP7A1 (L), BSEP (M), TIMP-1 (N), MMP-9 (O), MMP-14 (P), MMP-10 (Q), occludin (R), ZO-1 (S), claudin-1 (T) expression (assessed by qPCR), NAS (U), fibrosis score (V), α-SMA expression and NF-κB and AMPK activation (W, assessed by immunoblotting), α-SMA+GFAP+, NF-κB+F4/80+, and FXR+ cell populations (assessed by immunofluorescence staining), Sirius red staining, and oil red staining (X) in the liver. LC2767 at doses of 1 × 108 (LCL) and 1 × 109 CFU/mouse (LCH), obeticholic acid 5 mg/kg/mouse (Oca), and saline (LP) were orally administered once a day for 2 weeks to mice that were intraperitoneally injected with LPS for 4 weeks. NC group was treated with saline. Data are shown in mean ± SD (n = 6). #p < 0.05 vs. NC. *p < 0.05 vs. LP.
Long-term exposure to LPS strongly increased TLR4, TNF-α, α-SMA, collagen1, and CYP7A1 expression in the liver to 151.6%, 149.6%, 147.8%, 142.6%, and 325.5% of NC, respectively (Fig. 5F–X, Supplement Fig. S5B–F and Table S6). LPS also increased tissue inhibitor of tissue inhibitor of metalloproteinase (TIMP)-1, matrix metalloproteinase (MMP)-9, and MMP-14 expression, NF-κB phosphorylation, NF-κB+F4/80+ and α-SMA+GFAP+ cell populations, α-SMA, collagen, and lipid accumulation, and NAFLD activity score (NAS) and fibrosis score in the liver. However, LPS exposure decreased FXR expression to 29.8% of NC. LPS also suppressed the expression of SHP, BSEP, MMP-10, ZO-1, claudin-1, and occludin was reduced, along with AMPK activation.
Oral administration of LC2767 significantly inhibited LPS-induced TLR4 and TNF-α expression by 56.6% and 37.6%, respectively. LC2767 also decreased LPS-induced NF-κB activation, and the NF-κB+F4/80+ cell population, whereas obeticholic acid weakly inhibited them compared to LC2767. LC2767 and obeticholic acid all effectively suppressed LPS-induced α-SMA (45.3% and 48.0%, respectively), collagen1 (48.9% and 35.9%, respectively), and CYP7A1 expression (53.7% and 62.2%, respectively), along with an increase in α-SMA+GFAP+ cell population and NAS and fibrosis score. LC2767 also decreased LPS-induced α-SMA, collagen, and lipid accumulation in the liver. LC2767 enhanced LPS-suppressed expression of FXR by 199.4%. LC2767 also increased LPS-suppressed SHP and BSEP expression, AMPK activation, and FXR+ cell population. Additionally, LC2767 and obeticholic acid reduced LPS-induced expression of MMP-9, MMP-14, and TIMP-1, while increasing LPS-suppressed MMP-10 expression. Furthermore, LC2767, but not obeticholic acid, restored LPS-suppressed expression of TIMP-1 and tight junction proteins ZO-1, occludin, and claudin-1. LC2767 at a dose of 1 × 109 CFU/mouse was the most effective.
Long-term exposure to LPS caused colon shortening and colitis: it induced TLR4 and TNF-α expression in the colon to 245.0% and 179.5% of NC, respectively, while FXR expression decreased to 17.1% of NC (Fig. 6, Supplement Fig. S5G–M and Table S7). LPS also increased NF-κB+CD11c+ cell population in the colon, while AMPK activation were reduced. Oral administration of LC2767 partially recovered colon shortening. LC2767 also suppressed LPS-induced TLR4 and TNF-α expression in the colon by 51.8%% and 50.0%, respectively, while increasing LPS-suppressed FXR expression by 322.7%. Additionally, LC2767 decreased LPS-induced NF-κB+CD11c+ cell population, while LPS-suppressed colon length and AMPK activation increased.
Effect of LC2767 on colitis-related biomarker levels in mice longtermly, intraperitoneally exposed to LPS. Effects on TLR4 (A, assessed by qPCR), TNF-α (B, assessed by ELISA), and FXR expression (C, assessed by qPCR), AMPK and NF-κB activation (D, assessed by immunoblotting) and NF-κB+CD11c+ cell population (E) in the colon. LC2767 at doses of 1 × 108 (LCL) and 1 × 109 CFU/mouse (LCH), obeticholic acid (5 mg/kg/mouse, Oca), and saline (LP) were orally administered once a day for 2 weeks to mice that were intraperitoneally injected with LPS for 4 weeks. NC group was treated with saline. Data are shown in mean ± SD (n = 6). #p < 0.05 vs. NC. *p < 0.05 vs. LP.
Effect of LC2767 on liver damage in mice long-termly, intraperitoneally exposed to LGc
We evaluated the effects of LC2767 and obeticholic acid on liver damage in mice subjected to long-term exposure to LGc (Fig. 7A–E). Long-term exposure to LGc elevated AST, ALT, γ-GTP, TBA, and TCh levels in the blood. However, oral administration of LC2767 at doses of 1 × 108, 3 × 108, and 1 × 109 CFU/mouse or obeticholic acid at a dose of 5 mg/kg significantly reduced LGc-induced expression of these biomarkers. Of these, LC2767 at 1 × 109 CFU/mouse showed the strongest inhibitory effect on LGc-induced increases in AST, ALT, γ-GTP, TBA, and TCh levels.
Effect of LC2767 on liver injury and fibrosis-related biomarker levels in mice longtermly, intraperitoneally exposed to LGc. Effect on AST (A), ALT (B), γ-GTP (C), TCh (D), and TBA (E) in the blood. Effect on TLR4 (F), TNF-α (G), α-SMA (H), collagen1 (I), FXR (J), SHP (K), CYP7A1 (L), BSEP (M), TIMP-1 (N), MMP-9 (O), MMP-14 (P), MMP-10 (Q), occludin (R), ZO-1 (S), claudin-1 (T) expression (assessed by qPCR), α-SMA expression, NAS (U), fibrosis score (V), and NF-κB and AMPK activation (W, assessed by immunoblotting), α-SMA+GFAP+, NF-κB+F4/80+, and FXR+ cell populations (X, assessed by immunofluorescence staining), Sirius red staining, and oil red staining in the liver of mice. LC2767 (LCL, 1 × 108 CFU/mouse; LCM, 3 × 108 CFU/mouse; LCH, 1 × 109 CFU/mouse), obeticholic acid 5 mg/kg/mouse (Oca), and saline (LG) were orally administered once a day for 2 weeks to mice that were intraperitoneally injected with LGc for 4 weeks. NC group was treated with saline. Data are shown in mean ± SD (n = 6). #p < 0.05 vs. NC. *p < 0.05 vs. LG.
Long-term exposure to LGc led to increased expression of TLR4, TNF-α, α-SMA, collagen1, and CYP7A1 in the liver by 192.0%, 277.5%, 178.8%, 253.6%, and 212.8% of NC, respectively (Fig. 7F–X, Supplement Fig. S6A–F and Table S8). LGc also induced the expression of MMP-9, MMP-14, and TIMP-1, along with the expansion of NF-κB phosphorylation, NF-κB+F4/80+ and α-SMA+GFAP+ cell populations, α-SMA, collagen, and lipid accumulation, NF-κB+F4/80+ and α-SMA+GFAP+ cell populations, and NAS and fibrosis score in the liver. However, LGc suppressed the expression of FXR to 40.0% of NC. LGc also decreased the expression of SHP, BSEP, MMP10, ZO-1, claudin-1, and occludin, AMPK activation (phosphorylation), and FXR+ cell population.
Oral administration of LC2767 significantly inhibited LGc-induced TLR4 and TNF-α expression by 45.8% and 41.9%, respectively. LC2767 also decreased LGc-induced NF-κB activation and NF-κB+F4/80+ cell population. However, obeticholic acid weakly suppressed TNF-α and TLR4 expression and NF-κB+F4/80+ cell population compared to LC2767. LC2767 and obeticholic acid markedly suppressed LGc-induced α-SMA (42.2% and 46.0%, respectively), collagen1 (42.3% and 42.5%, respectively), and CYP7A1 expression (43.9% and 49.3%, respectively). They also decreased LGc-induced α-SMA+GFAP+ cell population, NAS and fibrosis score, α-SMA, collagen, and lipid accumulation in the liver. LC2767 increased LGc-suppressed FXR expression by 128.0%. LC2767 also induced LGc-suppressed SHP, and BSEP expression, and enhanced AMPK activation. Additionally, LC2767 and obeticholic acid reduced LGc-induced MMP-9, MMP-14, and TIMP-1 expression, while restoring LGc-suppressed MMP-10 expression. LC2767 also increased LGc-suppressed tight junction proteins ZO-1, occludin, and claudin-1 expression, AMPK phosphorylation, and FXR+ cell population. Of these, LC2767 at a dose of 1 × 109 CFU/mouse showed the strongest inhibitory effect.
Exposure to LGc caused colon shortening and colitis: it induced TLR4 and TNF-α expression in the colon to 256.3% and 163.6% of NC, respectively, while FXR expression decreased to 27.5% of NC (Fig. 8, Supplement Fig. S6G–L and Table S9). LPS also increased NF-κB+CD11c+ cell population in the colon, while AMPK activation were reduced. Oral administration of LC2767 partially recovered LGc-induced colon shortening. LC2767 and obeticholic acid also suppressed LPS-induced TLR4 (69.6% and 32.3%, respectively) and TNF-α expression (33.2% and 23.2%, respectively) in the colon, while increasing LPS-suppressed FXR expression by 361.9% and 587.3%, respectively. Additionally, LC2767 decreased LPS-induced NF-κB+CD11c+ cell population, while LPS-suppressed colon length and AMPK activation increased. However, obeticholic acid weakly increased AMPK activation alone.
Effect of LC2767 on colitis-related biomarker levels in mice longtermly, intraperitoneally exposed to LGc. Effects on TLR4 (A), TNF-α (B), and FXR expression (C, assessed by ELISA), AMPK and NF-κB activation (D) and NF-κB+CD11c+ cell population (E) in the colon. LC2767 (LCL, 1 × 108 CFU/mouse; LCM, 3 × 108 CFU/mouse; LCH, 1 × 109 CFU/mouse), obeticholic acid (Oca, 5 mg/kg/mouse), and saline (LG) were orally administered once a day for 2 weeks to mice that were intraperitoneally injected with LGc for 4 weeks. NC group was treated with saline. Data are shown in mean ± SD (n = 6). #p < 0.05 vs. NC. *p < 0.05 vs. LG.
Effects of LC2767 on liver damage in mice long-termly, intraperitoneally injected with LTc
Next, we examined the impact of LC2767 and obeticholic acid on liver damage in mice subjected to long-term exposure to LTc (Fig. 9). Long-term exposure to LTc increased AST, ALT, γ-GTP, TBA, and TCh levels in the blood (Fig. 9A–E). However, oral administration of LC2767 at doses of 1 × 108 and 1 × 109 CFU/mouse markedly reduced LTc-induced AST, ALT, γ-GTP, TBA, and TCh levels.
Effect of LC2767 on liver injury and fibrosis-related biomarker levels in mice intraperitoneally exposed to LTc. Effect on AST (A), ALT (B), γ-GTP (C), TBA (D), and TCh (E) in the blood. Effect on TLR4 (F), TNF-α (G), α-SMA (H), collagen1 (I), FXR (J), SHP (K), CYP7A1 (L) and BSEP (M) expression (assessed by qPCR) in the liver. LC2767 (LCL, 1 × 108 CFU/mouse; LCH, 1 × 109 CFU/mouse), obeticholic acid (Oca, 5 mg/kg/mouse), and saline (LT) were orally administered once a day for 2 weeks to mice that were intraperitoneally injected with LTc from 8 weeks. NC group was treated with saline. Data are shown in mean ± SD (n = 6). #p < 0.05 vs. NC. *p < 0.05 vs. LT.
Long-term exposure to LTc elevated TLR4, TNF-α, α-SMA, collagen1, and CYP7A1 expression in the liver to 219.7%, 229.0%, 359.8%, 311.2%, and 512.0% of NC, respectively. However, LTc decreased FXR expression in the liver to 30.1% of NC. LTc also decreased SHP and BSEP expression decreased (Fig. 9F–M). Oral administration of LC2767 significantly inhibited LTc-induced TLR4 and TNF-α expression by 49.0% and 54.0%, respectively, whereas obeticholic acid weakly decreased TLR4 and TNF-α expression. LC2767 (LCH) and obeticholic acid significantly reduced LTc-induced expression of α-SMA (by 50.5% and 60.1%, respectively), collagen1 (by 58.4% and 32.1%, respectively), and CYP7A1 (by 57.6% and 73.7%, respectively). Furthermore, LC2767 restored LTc-suppressed FXR, SHP and BSEP expression and AMPK activation.
Effects of LC2767 on gut dysbiosis in mice long-termly exposed with LPS
Gut dysbiosis is closely associated with liver diseases22. Therefore, to understand whether the action mechanism of LC2767 for the amelioration of liver injury and fibrosis, we investigated the effect of LC2767 on the gut microbiota composition in mice long-termly (8-weeks) exposed with LPS (Fig. 10, Supplement Tables S10–S12). Furthermore, LPS exposure significantly shifted β-diversity (PCoA) in gut microbiota, while α-diversity was not affected. Exposure to LPS significantly increased the population of Proteobacteria including Christensenellaceae, Porphyromonacaceae, and Rhodospirillaceae, while the population of Clostridiaceae significantly decreased. The population of Verrucomicrobiota including Akkermansiaceae showed a weak but non-significant decrease, while the population of Helicobacteriaceae increased slightly without statistical significance. However, oral administration of LC2767 partially shifted LPS-induced β-diversity to those of NC. LC2767 significantly increased the population of Verrucomicrobiota including Akkermansiaceae, Erysipelotrichaceae, Sutterellaceae, and PAC001057_f, while Rhodospirillaceae population significantly decreased. Christensenellaceae and Helicobacteriaceae populations were weakly, but not significantly, reduced by treatment with LC2767. Rhodospirillaceae, Helicobacteriaceae, Deferribacteriaceae, and Christensenellaceae populations, which were positively correlated with TNF-α, α-SMA, and collagen1 expression levels in the liver and ALT, AST, and TNF-α levels in the blood. Akkermansiaceae population was positively correlated with FXR expression level in the liver and colon. Coryobacteriaceae population was negatively correlated with with TNF-α, α-SMA, and collagen1 expression levels in the liver and AST and TNF-α levels in the blood.
Effect of LC2767 on the gut microbiota composition in mice longtermly, intraperitoneally exposed to LPS. Effect on (A) α-diversity (Shannon index), (B) β-diversity (principal coordinate analysis plot based on Bray–Curtis analysis), phylum (C) and family levels (D) and network analysis—(E) gut microbiota and ALT/AST levels in the blood, (F) gut microbiota and blood/liver TNF-α levels, (G) gut microbiota and α-SMA/collagen1 expression levels, and (H) gut microbiota and liver/gut FXR expression levels. LC2767 at a dose of 1 × 109 CFU/mouse (LCH) and saline (LP) were orally administered once a day for 2 weeks to mice that were intraperitoneally injected with LPS for 4 weeks. NC group was treated with saline. Data are shown in mean ± SD (n = 6). #p < 0.05 vs. NC. *p < 0.05 vs. LP.
Discussion
Acute inflammation is a natural and advantageous response to injuries and infections, while chronic inflammation can lead to various inflammatory diseases, such as gut inflammation, hepatitis, and rheumatoid arthritis23,24. Gut inflammation can be activated by gut dysbiosis and gut microbiota byproducts such as LPS, peptidoglycan, and reactive oxygen species24. Excessive exposure to high-fat diet, ethanol, or stressors induces the overexpression of endotoxins including LPS in the gut microbiome, which causes gut inflammation through the induction of NF-κB activation and suppression of tight junction protein expression11,25,26.
Thus, LPS causes a leaky gut via gut inflammation, which accelerates the absorption of gut bacterial LPS into the blood25,27. D-galactosamine causes hepatocyte death (necrosis and apoptosis) through the inhibition of RNA synthesis1. Thioacetamide induces hepatoxicity through the upregulation of TNF-α expression28. LPS absorbed into the liver stimulates the expression of proinflammatory cytokines including TNF-α via the activation of TLR4-mediated NF-κB signaling, resulting in hepatitis and steatohepatitis. These results suggest that excessive exposure to LPS can cause liver injury and fibrosis through the gut inflammation and hepatoxic ingredients including D-glucosamine and thioacetamide can accelerate LPS-inducible liver injury. However, LC2767 alleviates ethanol-, 2,4,6-trinitrobenzenesulfonic acid-induced liver injury, or high-fat diet-induced steatohepatitis with obesity in mice by the regulation of NF-κB signaling9,20,21,29. These findings suggest that suppressing gut bacterial endotoxin production and TLR4-mediated NF-κB signaling may be important for the amelioration of liver injury and fibrosis.
In the present study, we found that shorttermly or longtermly intraperitoneal or oral exposure to LPS, LGc, or LTc increased ALT, AST, and γ-GTP levels in the blood and TLR4, TNF-α, and IL-6 expression and NF-κB activation in the liver, while decreasing the expression of tight junction proteins ZO-1 and occludin. Although they weakly, but not significantly, increased bodyweight (Supplement Fig. S7), total cholesterol levels significantly increased in the blood. Although they did not cause significant morphological changes in the liver, NF-κB- and α-SMA-positive cell populations and NAS and fibrosis scores increased. Thus, intraperitoneal or oral exposure to LPS caused systemic inflammation including gut inflammation and hepatitis. Exposure to LPS, LGc, or LTc increased α-SMA, and collagen1 expression in the liver. They increased TIMP-1, MMP-9, and MMP-14 expression in the liver, while MMP-10 expression decreased. They also increased ALT, AST, and γ-GTP levels in the blood and TNF-α and IL-6 expression and NF-κB activation in the liver. In particular, LGc or LTc more potently increased the expression of inflammation-related markers in the liver than LPS alone. Moreover, LPS exposure significantly shifted β-diversity (PCoA) in gut microbiota and increased the population of LPS-producing Proteobacteria including Christensenellaceae, Porphyromonacaceae, and Rhodospirillaceae. These results suggest that excessive exposure to LPS, LGc, or LTc may cause liver injury and fibrosis through the modulation of NF-κB-involved TIMP/MMP expression and overpopulation of LPS-producing gut microbiota.
However, LC2767 (at doses of 1 × 108 and 1 × 109 CFU/mouse) reduced blood ALT, AST, γ-GTP, TNF-α, and TCh levels in mice with LPS-, LGc-, or LTc-induced liver injury, while reduced bodyweight weakly, but not significantly, recovered. LC2767 also reduced LPS-, LGc-, or LTc-induced TNF-α and TLR4 expression, NF-κB activation, and NF-κB-positive cell population in the liver and TNF-α, myeloperoxidase, and TLR4 expression levels and shortening in the colon, while LPS-, LGc-, or LTc-suppressed ZO-1 and occludin expression in the liver increased. LC2767 inhibited LPS-induced cytotoxicity in vitro: it reduced ALT, AST, and LDH levels in LPS-stimulated HepG2 cells. LC2767 suppresses LPS-induced TNF-α expression and NF-κB activation in the macrophages.
LC2767 partially shifted LPS-induced β-diversity to those of NC: it significantly decreased Rhodospirillaceae population and increased Akkermansiaceae, Sutterellaceae, Erysipelotrichaceae, Sutterellaceae, PAC001057_f populations. Rhodospirillaceae, Helicobacteriaceae, Deferribacteriaceae, and Christensenellaceae populations, which were positively correlated with TNF-α, α-SMA, and collagen1 expression levels in the liver and ALT, AST, and TNF-α levels in the blood. Akkermansiaceae population was positively correlated with FXR expression level in the liver and colon. Coryobacteriaceae population was negatively correlated with TNF-α, α-SMA, and collagen1 expression levels in the liver and AST and TNF-α levels in the blood. Akkermansiaceae including Akkermansia muciniphila is negatively correlated with the obesity and diabetes30,31. LC2767 decreases blood and fecal LPS levels in mice with high diet- or 2,4,6-trinitrobenzenesulfonic acid-induced liver injury9,20. These results suggest that LC2767 may alleviate liver damage including hepatitis by suppressing TLR4-mediated NF-κB activation and gut dysbiosis.
Although some results were confusing, most of results showed that LC2767 suppressed LPS-, LGc-, or LT-induced α-SMA, collagen1, TIMP-1, MMP-9, and MMP-14 expression in the liver, while MMP-10 expression decreased. Furthermore, LC2767 decreased LPS- or LGc- induced α-SMA, collagen, and lipid accumulation, and NAS and fibrosis score in the liver. Moreover, in gene expression microarray analysis using the Affymetrix Mouse Gene 2.0 ST Array platform, LC2767 downregulated LPS-induced TLR4, TNF-α, NF-κB, collagenase-1, CYP7A1, TIMP-1, MMP-9, and MMP14 genes, while upregulating LPS-suppressed MMP-10 and SHP genes (Supplement Figure S8A). LC2767 also downregulated LGc-induced TLR4, TNF-α, NF-κB, collagenase-1, CYP7A1, TIMP-1, and MMP-9 genes, while upregulating MMP-10, MMP-14, BASEP, and SHP genes (Supplement Fig. S8B). TIMP1 is upregulated during hepatic fibrogenesis32. MMP-9, which promotes the apoptosis of hepatic stellate cells, is highly expressed in liver fibrosis33. MMP14 is highly expressed in liver fibrosis34,35. Collagen1 expression is increased and collagenase-1 (MMP1) degrades extracellular matrix in hepatic fibrosis36,37,38. α-SMA-positive myofibroblast-like cells increase their expression of fibrillar collagen and MMPs such as MMP-9 in fibrotic tissue36,39. However, MMP-10 promotes hepatic repair and regeneration after partial hepatectomy and bile duct ligation40. These results suggest that LC2767 may alleviate liver injury and fibrosis through the regulation of NF-κB-involved TIMP/MMPs expression.
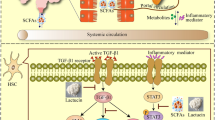
Exposure to LPS, LGc or LTc increased TC and TBA levels in the blood and CYP7A1 expression in the liver. However, they decreased FXR, SHP, and BSEP expression in the liver and FXR expression in the colon. However, LC2767 decreased LPS-, LGc-, or LTc-induced TC and TBA level in the blood and CYP7A1 expression in the liver and increased LPS-, LGc-, or LTc-suppressed FXR, SHP, and BSEP expression in the liver and FXR expression in the colon. FXR contributes directly and indirectly to the homeostasis of bile acid, hepatic triglyceride, and glucose. Activation of FXR results in the downregulation of CYP7A1: it suppresses the expression of profibrotic genes including α-SMA, collagen1, and TIMP-141,42. The overexpression of CYP7A1 activates the bile acid synthesis pathway43. Blic acids are transported from hepatocytes into the bile canaliculus through the BSEP, then enter the small intestine via the common bile duct, and are absorbed in the enterocytes of terminal ileum and colon through the apical sodium-dependent bile salt transporter44. Here, bile acids can activate the nuclear bile acid receptor, FXR, which results in the upregulation of fibroblast growth factor (FGF)19 and subsequent release of FGF19 into the portal circulation45. These results suggest that LC2767 may alleviate liver steatosis by suppressing the biotransformation of cholesterol to bile acid metabolites through the induction of FXR expression and the suppression of cholesterol biosynthesis.
LC2767 increased AMPK activation in the liver and colon. AMPK is a cellular energy sensor that can alleviate hepatic fibrosis46. LC2767 suppress the accumulation of fat accumulation in the liver of high-fat diet-fed mice9. These results suggest that LC2767 may alleviate liver steatosis and fibrosis through the suppression of gut microbiota-associated TLR4/NF-κB activation and the induction of AMPK activation.
In the present study, we could not perform MMP activity assay and in vivo histological assessments to confirm that the observed changes in gene expression translate into functional reductions in fibrosis. Therefore, to clarify these suggestions, further studies including these aspects are necessary to clarify the active components of LC2767 against liver injury and fibrosis.
In conclusion, LC2767 was found to suppress bacterial LPS biosynthesis in the intestinal fluid and blood while inhibiting the expression of TLR4 and TNF-α, and reducing the NF-κB-positive cell population in both the intestine and liver. In the liver, it also downregulated the expression of collagen1 and α-SMA. Additionally, LC2767 activated FXR and AMPK signaling pathways, which led to the attenuation of LPS- or LGc-induced liver inflammation (hepatitis), liver steatosis, and gut inflammation. Overall, LC2767 effectively alleviated liver damage, fibrosis, and intestinal barrier dysfunction by regulating TLR4-mediated NF-κB activation, FXR expression, AMPK activation, and gut microbiota.
Materials and methods
Preparation of LC2767
L. plantarum LC27 and B. longum LC67 strains were cultivated in a modified MRS and GAM medium, as previously reported21. Following cultivation, the cells were harvested by centrifugation at 5000 g for 20 min at 4 °C. The harvested cells were then resuspended in a 2% trehalose solution and subjected to freeze-drying. The resulting dried cells of LC27 and LC67 were then combined in ratios of 9:1, 3:1, 1:1, 1:3, and 1:9. For in vitro experiments, the combined cells were rehydrated in phosphate buffered saline (PBS). For in vivo studies, the freeze-dried cells were also suspended in sterilized saline.
Culture of HepG2 and Caco2 cells
HepG2 cells (Korean Cell Line Bank) and Caco2 cells (Korean Cell Line Bank) were cultured in DMEM (Sigma) supplemented with 1% antibiotic-antimycotic and 10% fetal bovine serum, and maintained at 37 °C. HepG2 cells were seeded at a density of 2 × 106 cells/mL and treated with or without LPS (100 ng/mL) in the absence or presence of LC2767, a (3:1) mix of LC27 and LC67, at concentrations of 1 × 102, 1 × 103, 1 × 104, and 1 × 106 colony-forming unit (CFU)/mL for 20 h. The levels of ALT, AST, and LDH were then measured using their respective assay kits. CacoG2 cells were seeded at a density of 1 × 106 cells/mL and treated with or without LPS (100 ng/mL) in the absence or presence of LC2767 at concentrations of 1 × 103 and 1 × 105 CFU/mL for 20 h. FXR expression level and NF-kB activation (p-p65/p65) were assayed using quantitative real-time polymerase chain reaction (qPCR) and immunoblotting, respectively.
Animals
Male C57BL/6 mice, aged 8 weeks and weighing between 19 and 21 g, were purchased from Koatech Inc. (Korea). The mice were housed in wire cages under controlled environmental conditions (temperature: 20–22 °C; humidity: 50 ± 10%) and provided with standard laboratory chow and water ad libitum. All animal experiments were approved by the Committee for the Care and Use of Laboratory Animals at Kyung Hee University (IACUC No: KHUASP(SE)-23087, KHUASP(SE)-23390) and were ethically conducted in accordance of the University Guideline for Laboratory Animals Care and Usage and ARRIVE guideline47.
Preparation of mice with liver injury or fibrosis and treatment with LC2767
First, we investigated liver injury-ameliorating effect of LC2767 in mice intraperitoneally injected with LPS. In brief, mice except normal control group (NC) received intraperitoneal injection of bacterial LPS (250 µg/kg/day, isolated from Escherichia coli, Sigma) for 5 days. Thereafter (24 h after the final LPS treatment), test agents (sLi, saline; LCL, 1 × 108 CFU/mouse/day of LC2767; LCH, 1 × 109 CFU/mouse/day of LC2767; Ec, 1 × 109 CFU/mouse/day of Escherichia coli; Oca, 5 mg/kg/day of obeticholic acid) was orally administered for 5 days. NC was treated with saline instead of LPS and test agents.
Second, we investigated liver injury-ameliorating effect of LC2767 in mice orally gavaged with LPS. In brief, mice except Nc received oral gavage of LPS (500 µg/kg/day) for 5 days. Thereafter, test agetns (sLo, saline; LCH, 1 × 109 CFU/mouse/day of LC2767) was orally administered for 5 days. NC was treated with saline instead of LPS and test agents.
Third, we examined the effect of LC2767 on subacute LPS-induced liver injury in mice. Mice except Nc received intraperitoneal injection of bacterial LPS (10 µg/kg/day) for 4 weeks (every other day). Thereafter, test agents (LP, saline; LCL, 1 × 108 CFU/mouse/day of LC2767; LCH, 1 × 109 CFU/mouse/day of LC2767; Oca, 5 mg/kg/day of obeticholic acid) was orally given every day for 2 weeks. NC was treated with saline instead of LPS and test agents.
Fourth, we tested the effect of LC2767 on subacute LGc-induced liver injury in mice. Mice except Nc received the intraperitoneal injection of LGc (LPS [10 µg/kg/day] and D-galactosamine [50 mg/kg/day, Sigma]) every other day for 4 weeks, as previously reported16. Thereafter, test agents (LG, saline; LCL, 1 × 108 CFU/mouse/day of LC2767; LCM, 3 × 108 CFU/mouse/day of LC2767; LCH, 1 × 109 CFU/mouse/day of LC2767; Oca, 5 mg/kg/day of obeticholic acid) was orally administered every day for 2 weeks, starting 24 h after the last LGc treatment. Mice were sacrificed 20 h after the final treatment. NC was treated with saline instead of LGc and test agents.
Fifth, we tested the effect of LC2767 on subacute LTc-induced liver injury in mice. Mice except Nc received the intraperitoneal injection of LTc (LPS [10 µg/kg/day] and thioacetamide [50 mg/kg/day, Sigma]) every other day for 4 weeks. Thereafter, test agents (LT, saline; LCL, 1 × 108 CFU/mouse/day of LC2767; LCH, 1 × 109 CFU/mouse/day of LC2767; Oca, 5 mg/kg/day of obeticholic acid) was orally administered every day for 2 weeks. NC was treated with saline instead of LPS/thioacetamide and test agents.
Mice were euthanized through CO2 exposure in a closed chamber 20 h after the final treatment with test agents, followed by cervical dislocation. The blood (collected from the carotid artery), liver, ileum, and colon were removed for the analyses of enzyme-linked immunosorbent assay (ELISA), immunoblotting, and histological exam. Sera were separated by centrifugation (4 °C, 10 min, 5000 g), as previously reported29 .
Determination of ALT, AST, LDH, γ-GTP, TBA, and TCh
The levels of ALT, AST, γ-GTP, TBA, TCh (Asan Pharm Co., Korea), and TBA (Elabscience, Texas) in serum and cell culture supernatant were measured using their respective assay kits.
ELISA and immunoblotting
Liver and colon tissues were homogenized on ice using radio-immunoprecipitation assay (RIPA) lysis buffer (Biosesang, Korea) that was supplemented with 1% phosphatase inhibitor cocktail and 1% protease inhibitor cocktail (Roche). The homogenates were then centrifuged (12,000 g, 15 min, 4 °C). In their supernatants, cytokine and biomarker expression levels were assayed.
For cytokine assays, the supernatants were transferred to a 96-well plate and analyzed using their ELISA kits (R&D Systems), as previously reported20.
For the immunoblotting analysis, the supernatants were applied to sodium dodecyl sulfate-polyacrylamide gel electrophoresis and transferred onto polyvinylidene fluoride membranes48. Proteins were detected using specific antibodies for p-NF-κB-p65 (S536, Cell Signaling), NF-κB-p65 (D14E12, Cell Signaling), α-smooth muscle actin (α-SMA, Invitrogen), F4/80 (Invitrogen), CD11c (Invitrogen), AMP-activated protein kinase a (AMPK, Santa Cruz), p-AMPK (Santa Cruz), and β-actin (Santa Cruz) and secondary antibodies conjugated with horseradish peroxidase (HRP). Conjugated proteins were visualized using an ECL detection kit.
qPCR analysis
mRNA (2 µg) was extracted from liver and colon tissues using the Qiagen RNeasy Mini Kit (Qiagen, Germany) and reverse-transcribed into cDNA using the PrimeScript cDNA Synthesis Kit (Takara, Japan)49. PCR amplification was carried out on the Rotor-Gene Q 5plex Platform (Qiagen) utilizing the TB Green Premix Ex Taq II (Takara). Primer sequences used for amplification are listed in Supplement Table S13.
Histopathological examination
Livers were collected, and the median lobe was fixed in 4% paraformaldehyde. Histological assessment and scoring (NAS, fibrosis score, oil red staining, and Sirius red staining) were evaluated according to the method of Kroh et al.50.
Immunofluorescence staining
Liver and colon tissues were harvested from mice, following transcardial perfusion with 4% paraformaldehyde on ice, sectioned at a thickness of 10 μm, incubated with primary antibodies (NF-κB, F4/80, α-SMA, glial fibrillary acidic protein [GFAP], CD11c, and/or FXR) for 12 h, and treated with secondary antibodies conjugated to Alexa Fluor 488 or Alexa Fluor 594 (Invitrogen) for 2 h48. Subsequently, the nuclei were counterstained with 4′,6-diamidino-2-phenylindole (DAPI). Stained sections were then visualized using a confocal microscope and intensities were determined using ImageJ, as previously described49.
Gut microbiota analysis
Bacterial genomic DNAs were extracted from the fresh stools of mice using a QIAamp DNA stool mini kit (Qiagen) and 16 S rRNA genes were sequenced51. Amplification of the genomic DNA was performed using barcoded primers, which targeted the V4 region of the bacterial 16 S rRNA gene. Sequencing for each amplicon was performed using Illumina iSeq 100 (San Diego, CA). Predictive functional genes were analyzed using the phylogenetic investigation of communities by reconstruction of unobserved states. Sequenced reads were deposited in the short read archive of NCBI under accession number PRJNA1230391.
Statistics
Data are expressed as mean ± SD using GraphPad Prism 10 software. The normal distribution of the data was assessed using the Shapiro–Wilk test. Statistical significance was analyzed using one-way ANOVA with Dunnett’s multiple comparisons test. The correlation between gut microbiota and biomarkers (network and heatmap analyses) were analyzed using Pearson correlation coefficient. The statistic data are indicated in Supplement Table S14.
Data availability
All data supporting our findings can be found in the main paper or supplementary files. Sequencing data are available via the NCBI’s short read archive PRJNA1230391. All data will be shared on request.
Abbreviations
- ALT:
-
Alanine transaminase
- AMPK:
-
AMP-activated protein kinase
- ASBT:
-
Apical sodium-dependent bile salt transporter
- AST:
-
Aspartate transaminase
- BSEP:
-
Bile salt export pump
- CFU:
-
Colony-forming unit
- Collagen1:
-
Collagen type 1
- CTP7A1:
-
Cholesterol 7 α-hydroxylase
- ELISA:
-
Enzyme-linked immunosorbent assay
- FXR:
-
Farnesoid X receptor
- GFAP:
-
Glial fibrillary acidic protein
- γ-GTP:
-
γ-Glutamyl transpeptidase
- IL:
-
Interleukin
- LC2767:
-
a (3:1) mix of LC27 and LC67
- LDH:
-
Lactate dehydrogenase
- LGc:
-
LPS and D-galactosamine
- LPS:
-
Lipopolysaccharide
- LTc:
-
LPS and thioacetamide
- MMP:
-
Matrix metalloproteinase
- NAFLD:
-
Non-alcoholic fatty liver disease
- NAS:
-
NAFLD activity score
- NC:
-
Normal control group
- RIPA:
-
Radio-immunoprecipitation assay
- SHP:
-
Small heterodimer partner
- SMA:
-
Smooth muscle actin
- TBA:
-
Total bile acid
- TCh:
-
Total cholesterol
- TIMP:
-
Tissue inhibitor of metalloproteinase
- TLR:
-
Toll-like receptor
- TNF:
-
Tumor necrosis factor
References
Farghali, H., Kgalalelo Kemelo, M., Wojnarová, L. & Kutinová Canová, N. In vitro and in vivo experimental hepatotoxic models in liver research: applications to the assessment of potential hepatoprotective drugs. Physiol. Res. 65, S417–s425. https://doi.org/10.33549/physiolres.933506 (2016).
Di Zeo-Sánchez, D. E. et al. Modeling drug-induced liver injury: current status and future prospects. Expert Opin. Drug Metab. Toxicol. 18, 555–573. https://doi.org/10.1080/17425255.2022.2122810 (2022).
Maurice, J. & Manousou, P. Non-alcoholic fatty liver disease. Clin. Med. (Lond). 18, 245–250. https://doi.org/10.7861/clinmedicine.18-3-245 (2018).
Muzurović, E., Mikhailidis, D. P. & Mantzoros, C. Non-alcoholic fatty liver disease, insulin resistance, metabolic syndrome and their association with vascular risk. Metabolism 119, 154770. https://doi.org/10.1016/j.metabol.2021.154770 (2021).
Powell, E. E., Wong, V. W. & Rinella, M. Non-alcoholic fatty liver disease. Lancet 397, 2212–2224. https://doi.org/10.1016/s0140-6736(20)32511-3 (2021).
Paternostro, R. & Trauner, M. Current treatment of non-alcoholic fatty liver disease. J. Intern. Med. 292, 190–204. https://doi.org/10.1111/joim.13531 (2022).
Czaja, A. J. Hepatic inflammation and progressive liver fibrosis in chronic liver disease. World J. Gastroenterol. 20, 2515–2532. https://doi.org/10.3748/wjg.v20.i10.2515 (2014).
An, L. et al. The role of gut-derived lipopolysaccharides and the intestinal barrier in fatty liver diseases. J. Gastrointest. Surg. 26, 671–683. https://doi.org/10.1007/s11605-021-05188-7 (2022).
Kim, I. Lactobacillus plantarum LC27 and bifidobacterium longum LC67 simultaneously alleviate high-fat diet-induced colitis, endotoxemia, liver steatosis, and obesity in mice. Nutr. Res. 67, 78–89. https://doi.org/10.1016/j.nutres.2019.03.008 (2019).
Kim, K. A., Gu, W., Lee, I. A., Joh, E. H. & Kim, D. H. High fat diet-induced gut microbiota exacerbates inflammation and obesity in mice via the TLR4 signaling pathway. PLoS One. 7, e47713. https://doi.org/10.1371/journal.pone.0047713 (2012).
Jang, H. M., Lee, K. E., Lee, H. J. & Kim, D. H. Immobilization stress-induced Escherichia coli causes anxiety by inducing NF-κB activation through gut microbiota disturbance. Sci. Rep. 8, 13897. https://doi.org/10.1038/s41598-018-31764-0 (2018).
Jang, S. E. et al. Gastrointestinal inflammation by gut microbiota disturbance induces memory impairment in mice. Mucosal Immunol. 11, 369–379. https://doi.org/10.1038/mi.2017.49 (2018).
Kessoku, T. et al. Endotoxins and non-alcoholic fatty liver disease. Front. Endocrinol. (Lausanne). 12, 770986. https://doi.org/10.3389/fendo.2021.770986 (2021).
Liu, L. et al. Gut dysbiosis and abnormal bile acid metabolism in colitis-associated cancer. Gastroenterol. Res. Pract. 2021 (6645970). https://doi.org/10.1155/2021/6645970 (2021).
Staley, C., Weingarden, A. R., Khoruts, A. & Sadowsky, M. J. Interaction of gut microbiota with bile acid metabolism and its influence on disease States. Appl. Microbiol. Biotechnol. 101, 47–64. https://doi.org/10.1007/s00253-016-8006-6 (2017).
Wang, Y. et al. Protective effects of probiotic Lactobacillus casei Zhang against endotoxin- and d-galactosamine-induced liver injury in rats via anti-oxidative and anti-inflammatory capacities. Int. Immunopharmacol. 15, 30–37. https://doi.org/10.1016/j.intimp.2012.10.026 (2013).
Wang, Y. et al. Probiotic Lactobacillus casei Zhang reduces pro-inflammatory cytokine production and hepatic inflammation in a rat model of acute liver failure. Eur. J. Nutr. 55, 821–831. https://doi.org/10.1007/s00394-015-0904-3 (2016).
Ewaschuk, J. et al. Probiotic bacteria prevent hepatic damage and maintain colonic barrier function in a mouse model of sepsis. Hepatology 46, 841–850. https://doi.org/10.1002/hep.21750 (2007).
Gao, J. et al. A novel postbiotic from Lactobacillus rhamnosus GG with a beneficial effect on intestinal barrier function. Front. Microbiol. 10, 477. https://doi.org/10.3389/fmicb.2019.00477 (2019).
Jang, S. E., Jeong, J. J., Kim, J. K., Han, M. J. & Kim, D. H. Simultaneous amelioratation of colitis and liver injury in mice by bifidobacterium longum LC67 and Lactobacillus plantarum LC27. Sci. Rep. 8, 7500. https://doi.org/10.1038/s41598-018-25775-0 (2018).
Kim, W. G., Kim, H. I., Kwon, E. K., Han, M. J. & Kim, D. H. Lactobacillus plantarum LC27 and bifidobacterium longum LC67 mitigate alcoholic steatosis in mice by inhibiting LPS-mediated NF-κB activation through restoration of the disturbed gut microbiota. Food Funct. 9, 4255–4265. https://doi.org/10.1039/c8fo00252e (2018).
Milosevic, I. et al. Gut-Liver Axis, gut Microbiota, and its modulation in the management of liver diseases: A review of the literature. Int. J. Mol. Sci. 20 https://doi.org/10.3390/ijms20020395 (2019).
Bistrian, B. Systemic response to inflammation. Nutr. Rev. 65, 170–172. https://doi.org/10.1301/nr.2007.dec.s170-s172 (2007).
Bawa, M. & Saraswat, V. A. Gut-liver axis: role of inflammasomes. J. Clin. Exp. Hepatol. 3, 141–149. https://doi.org/10.1016/j.jceh.2013.03.225 (2013).
Nighot, M. et al. Lipopolysaccharide-induced increase in intestinal epithelial tight permeability is mediated by toll-like receptor 4/Myeloid differentiation primary response 88 (MyD88) activation of myosin light chain kinase expression. Am. J. Pathol. 187, 2698–2710. https://doi.org/10.1016/j.ajpath.2017.08.005 (2017).
Jang, H. M. et al. Enterococcus faecium and pediococcus acidilactici deteriorate Enterobacteriaceae-induced depression and colitis in mice. Sci. Rep. 12, 9389. https://doi.org/10.1038/s41598-022-13629-9 (2022).
Guo, S., Al-Sadi, R., Said, H. M. & Ma, T. Y. Lipopolysaccharide causes an increase in intestinal tight junction permeability in vitro and in vivo by inducing enterocyte membrane expression and localization of TLR-4 and CD14. Am. J. Pathol. 182, 375–387. https://doi.org/10.1016/j.ajpath.2012.10.014 (2013).
Ezhilarasan, D. Molecular mechanisms in thioacetamide-induced acute and chronic liver injury models. Environ. Toxicol. Pharmacol. 99, 104093. https://doi.org/10.1016/j.etap.2023.104093 (2023).
Kwon, E. K., Kang, G. D., Kim, W. K., Han, M. J. & Kim, D. H. Lactobacillus plantarum LC27 and bifidobacterium longum LC67 simultaneously alleviate ethanol-induced gastritis and hepatic injury in mice. J. Funct. Foods. 38, 389–398. https://doi.org/10.1016/j.jff.2017.09.036 (2017).
Cani, P. D., Depommier, C., Derrien, M., Everard, A. & de Vos, W. M. Akkermansia muciniphila: paradigm for next-generation beneficial microorganisms. Nat. Rev. Gastroenterol. Hepatol. 19, 625–637. https://doi.org/10.1038/s41575-022-00631-9 (2022).
Yin, C. et al. Differences of gut microbiota composition in mice supplied with polysaccharides from γ-irradiated and non-irradiated schizophyllum commune. Food Res. Int. 151, 110855. https://doi.org/10.1016/j.foodres.2021.110855 (2022).
Thiele, N. D. et al. TIMP-1 is upregulated, but not essential in hepatic fibrogenesis and carcinogenesis in mice. Sci. Rep. 7, 714. https://doi.org/10.1038/s41598-017-00671-1 (2017).
Wang, Y. et al. The role of matrix metalloproteinase 9 in fibrosis diseases and its molecular mechanisms. Biomed. Pharmacother. 171, 116116. https://doi.org/10.1016/j.biopha.2023.116116 (2024).
Takahara, T. et al. Dual expression of matrix metalloproteinase-2 and membrane-type 1-matrix metalloproteinase in fibrotic human livers. Hepatology 26, 1521–1529. https://doi.org/10.1002/hep.510260620 (1997).
Zhou, X. et al. Expression of matrix metalloproteinase-2 and – 14 persists during early resolution of experimental liver fibrosis and might contribute to fibrolysis. Liver Int. 24, 492–501. https://doi.org/10.1111/j.1478-3231.2004.0946.x (2004).
Duarte, S., Baber, J., Fujii, T. & Coito, A. J. Matrix metalloproteinases in liver injury, repair and fibrosis. Matrix Biol. 44–46, 147–156. https://doi.org/10.1016/j.matbio.2015.01.004 (2015).
Luangmonkong, T., Parichatikanond, W. & Olinga, P. Targeting collagen homeostasis for the treatment of liver fibrosis: opportunities and challenges. Biochem. Pharmacol. 215, 115740. https://doi.org/10.1016/j.bcp.2023.115740 (2023).
Ala-Kokko, L., Pihlajaniemi, T., Myers, J. C., Kivirikko, K. I. & Savolainen, E. R. Gene expression of type I, III and IV collagens in hepatic fibrosis induced by Dimethylnitrosamine in the rat. Biochem. J. 244, 75–79. https://doi.org/10.1042/bj2440075 (1987).
Roeb, E. Matrix metalloproteinases and liver fibrosis (translational aspects). Matrix Biol. 68–69, 463–473. https://doi.org/10.1016/j.matbio.2017.12.012 (2018).
Garcia-Irigoyen, O. et al. Matrix metalloproteinase-10 expression is induced during hepatic injury and plays a fundamental role in liver tissue repair. Liver Int. 34, e257–270. https://doi.org/10.1111/liv.12337 (2014).
Fiorucci, S. et al. A farnesoid x receptor-small heterodimer partner regulatory cascade modulates tissue metalloproteinase inhibitor-1 and matrix metalloprotease expression in hepatic stellate cells and promotes resolution of liver fibrosis. J. Pharmacol. Exp. Ther. 314, 584–595. https://doi.org/10.1124/jpet.105.084905 (2005).
Li, J. et al. Roles of microRNA-29a in the antifibrotic effect of farnesoid X receptor in hepatic stellate cells. Mol. Pharmacol. 80, 191–200. https://doi.org/10.1124/mol.110.068247 (2011).
Chiang, J. Y. L. & Ferrell, J. M. Up to date on cholesterol 7 alpha-hydroxylase (CYP7A1) in bile acid synthesis. Liver Res. 4, 47–63. https://doi.org/10.1016/j.livres.2020.05.001 (2020).
Ren, T., Pang, L., Dai, W., Wu, S. & Kong, J. Regulatory mechanisms of the bile salt export pump (BSEP/ABCB11) and its role in related diseases. Clin. Res. Hepatol. Gastroenterol. 45, 101641. https://doi.org/10.1016/j.clinre.2021.101641 (2021).
Schumacher, J. D. & Guo, G. L. Pharmacologic modulation of bile Acid-FXR-FGF15/FGF19 pathway for the treatment of nonalcoholic steatohepatitis. Handb. Exp. Pharmacol. 256, 325–357. https://doi.org/10.1007/164_2019_228 (2019).
Liang, Z. et al. AMPK: a novel target for treating hepatic fibrosis. Oncotarget 8, 62780–62792. https://doi.org/10.18632/oncotarget.19376 (2017).
Percie du Sert. The ARRIVE guidelines 2.0: updated guidelines for reporting animal research. PLoS Biol. 18, e3000410. https://doi.org/10.1371/journal.pbio.3000410 (2020).
Lee, K. E. et al. The extracellular vesicle of gut microbial paenalcaligenes hominis is a risk factor for vagus nerve-mediated cognitive impairment. Microbiome 8, 107. https://doi.org/10.1186/s40168-020-00881-2 (2020).
Kim, J. K., Lee, K. E., Lee, S. A., Jang, H. M. & Kim, D. H. Interplay between human gut bacteria Escherichia coli and Lactobacillus mucosae in the occurrence of neuropsychiatric disorders in mice. Front. Immunol. 11, 273. https://doi.org/10.3389/fimmu.2020.00273 (2020).
Kroh, A. et al. Mouse models of nonalcoholic steatohepatitis: Head-to-Head comparison of dietary models and impact on inflammation and animal welfare. Gastroenterol. Res. Pract. 2020, 7347068. https://doi.org/10.1155/2020/7347068 (2020).
Ma, X. et al. Lipopolysaccharide-producing Veillonella infantium and Escherichia fergusonii cause vagus nerve-mediated cognitive impairment in mice. Brain Behav. Immun. 118, 136–148. https://doi.org/10.1016/j.bbi.2024.02.031 (2024).
Funding
This work was supported by the Commercialization Promotion Agency for R&D Outcomes (COMPA) grant funded by the Korea government (MSIT) (RS-2024-00486802) and the Ministry of Food and Drug Safety (22203MFDS539), and funded by the Korea Healthy Industry Development Institute.
Author information
Authors and Affiliations
Contributions
D.-Y.L., H.-M.J., S.-W.H., and D.-H.K. wrote the main manucritp text. D.-Y.L., H.-M.J., and S.H.K. prepared Figs. 1 and 2. D.-Y.L., H.-M.J., and J.-W.S. prepared Figs. 3, 4, 5, 6, 7 and 8. D.-Y.L. prepared Fig. 9. D.-Y.L. and Y.-J.S. prepared Fig. 10. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval and consent to participate
Animal experiments were approved by the Committee for the Care and Use of Laboratory Animals in the Kyung Hee University (IACUC No.: KHUASP(SE)-23087, KHUASP(SE)-23390) and conducted in accordance with the university’s guidelines for the care and use of laboratory animals.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Lee, DY., Jang, HM., Shin, JW. et al. LC2767 alleviates LPS-induced liver injury and fibrosis by regulating FXR expression, NF-κB activation, and gut microbiota. Sci Rep 16, 4466 (2026). https://doi.org/10.1038/s41598-025-34675-z
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-34675-z