Abstract
This study aimed to investigate the association between the Fibrosis−4 (FIB−4) index and functional outcomes and hemorrhagic complications in patients with large vessel occlusion acute ischemic stroke (LVO-AIS) treated with mechanical thrombectomy (MT). In this single-center retrospective cohort study, we consecutively enrolled patients with LVO-AIS who underwent MT between January 2018 and February 2024. The primary endpoint was poor functional outcome at 90 days (modified Rankin Scale score 3–6). Secondary endpoints included hemorrhagic transformation (HT) and symptomatic intracranial hemorrhage (sICH). Multivariable logistic regression models and restricted cubic spline analyses were used to evaluate the association between FIB−4 index and outcomes after adjusting for potential confounders. Among 421 patients, 254 (60.33%) had poor outcomes, 197 (46.79%) developed HT, and 76 (18.05%) experienced sICH. After adjustment for confounding factors, each unit increase in FIB−4 index was associated with a 38% higher risk of poor outcome (P = 0.013). This association showed significant nonlinearity (P-nonlinear = 0.010), with risk increasing exponentially beyond a FIB−4 threshold of 2.4. Advanced fibrosis (FIB−4 ≥ 2.67) was independently associated with poor outcomes (P = 0.024). FIB−4 index independently predicts poor functional outcomes in LVO-AIS patients. This readily available biomarker may help identify high-risk patients who could benefit from enhanced monitoring and individualized treatment strategies.
Similar content being viewed by others
Introduction
Despite advances in acute stroke care, large vessel occlusion acute ischemic stroke (LVO-AIS) remains a devastating condition with high mortality and disability rates, accounting for approximately 28–46% of all acute ischemic strokes1,2,3. While mechanical thrombectomy (MT) has revolutionized the treatment of LVO-AIS through rapid restoration of cerebral perfusion and salvage of the ischemic penumbra4, a substantial proportion of patients still experience poor outcomes, suggesting the existence of incompletely understood prognostic factors5.
Non-alcoholic fatty liver disease (NAFLD), the most prevalent chronic liver disease globally, shows marked geographic variation in prevalence, ranging from 13% in Africa to 42% in Southeast Asia6,7. The NAFLD spectrum encompasses a continuum from simple steatosis to non-alcoholic steatohepatitis, potentially progressing to liver fibrosis, cirrhosis, and hepatocellular carcinoma8. Recent evidence suggests that liver fibrosis, as the common end-pathway of various chronic liver diseases, may influence stroke outcomes through multiple mechanisms, including systemic inflammation, oxidative stress, endothelial dysfunction, and coagulation abnormalities9,10,11,12,13,14,15,16,17. This issue holds particular significance in China, where the prevalence of NAFLD, the primary cause of liver fibrosis, reaches 29.6%—significantly higher than the Asian average. By 2030, NAFLD is projected to affect more than 314 million people in China, making it the country with the largest NAFLD population globally18,19.
The Fibrosis−4 (FIB−4) index, a non-invasive assessment tool incorporating serum aminotransferase levels and platelet count, has emerged as a valuable predictor of outcomes in AIS patients. Growing evidence associates elevated FIB−4 indices with multiple adverse outcomes in AIS, including more severe neurological deficits at admission, higher rates of hemorrhagic transformation and in-hospital mortality, poor long-term functional outcomes, and increased risk of stroke recurrence20,21,22,23,24,25. Furthermore, the FIB−4 index has demonstrated efficacy in predicting the risk of symptomatic intracranial hemorrhage (sICH) and poor outcomes following intravenous thrombolysis26,27,28. However, LVO-AIS patients receiving MT face unique and complex pathophysiological challenges, characterized not only by more extensive initial ischemic injury and broader penumbral regions but also by susceptibility to various reperfusion-related complications. Consequently, the pattern of association between liver fibrosis and outcomes in this specific population may differ from that in conventional stroke patients. Nevertheless, a significant knowledge gap persists regarding the impact of liver fibrosis on short-term outcomes in Chinese LVO-AIS patients after MT.
Against this background, we aimed to investigate the association between liver fibrosis, as assessed by the FIB−4 index, and 90-day functional outcomes in Chinese LVO-AIS patients treated with MT. We hypothesized that elevated FIB−4 indices would be significantly associated with poor outcomes, potentially providing a reliable early risk stratification tool to optimize individualized treatment strategies.
Materials and methods
Study design and population
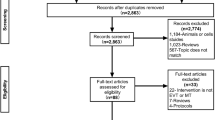
We conducted this single-center retrospective cohort study at a national comprehensive stroke center in China. A total of 421 consecutive patients with AIS who underwent MT between January 2018 and February 2024 were enrolled. Inclusion criteria were: age ≥ 18 years, diagnosis of acute ischemic stroke according to World Health Organization criteria, and large vessel occlusion confirmed by computed tomographic angiography or digital subtraction angiography (DSA), involving the internal carotid artery, M1/M2 segments of the middle cerebral artery, basilar artery, or P1 segment of the posterior cerebral artery. We excluded patients with intracranial hemorrhage on baseline imaging, pre-stroke modified Rankin Scale score > 2, history of severe liver disease (viral hepatitis, cirrhosis, hepatocellular carcinoma) or severe renal insufficiency, current use of hepatotoxic medications, incomplete baseline data, or loss to follow-up. To reflect real-world clinical practice, patients with chronic alcohol consumption were not excluded29. The patient selection process is detailed in Supplementary Fig. 1.
FIB−4 Index Distribution by Clinical Outcomes in LVO-AIS Patients Receiving Mechanical Thrombectomy. Box plots showing FIB−4 index distribution in patients stratified by (A) 90-day functional outcome, (B) hemorrhagic transformation (HT), and (C) symptomatic intracranial hemorrhage (sICH). Medians (horizontal lines), interquartile ranges (boxes), ranges (whiskers), and individual data points are shown. Red lines indicate linear trends. Patients with poor outcomes showed significantly higher FIB−4 indices compared with those with good outcomes (2.30 vs. 1.75, P < 0.001). Similarly, elevated FIB−4 indices were observed in patients with HT (2.29 vs. 1.77, P < 0.001) and sICH (2.97 vs. 1.88, P < 0.001). ***P < 0.001.
This study was approved by the Ethics Committee of Zhongshan Hospital of Xiamen University (approval number: xmzsyyky2022−196) and conducted in accordance with the Declaration of Helsinki. The Ethics Committee of Zhongshan Hospital of Xiamen University waived the requirement for informed consent due to the retrospective nature of the study and anonymized data handling.
Data collection
Baseline data were collected through electronic medical records, including demographic characteristics, cerebrovascular risk factors (smoking, alcohol consumption, hypertension, diabetes mellitus, previous stroke/transient ischemic attack [TIA], coronary heart disease, valvular heart disease, and atrial fibrillation), and vital signs at admission. Stroke severity was assessed using the National Institutes of Health Stroke Scale (NIHSS) and consciousness level was evaluated using the Glasgow Coma Scale (GCS) by trained neurologists. Stroke subtypes were classified according to the Trial of ORG 10,172 in Acute Stroke Treatment criteria as large-artery atherosclerosis, cardioembolism, or other causes (including other determined etiology and undetermined etiology).
MT-related parameters were recorded in detail, including onset-to-puncture time, onset-to-reperfusion time, puncture-to-reperfusion time, number of thrombectomy attempts, thrombectomy technique, use of intravenous thrombolysis, and reperfusion status. Post-procedure reperfusion was assessed using the modified Thrombolysis in Cerebral Infarction (mTICI) scale based on final DSA results, with successful reperfusion defined as mTICI grade 2b−330.
FIB−4 index assessment
Fasting venous blood samples were collected on the first morning after admission. Complete blood count parameters were measured using an automated hematology analyzer, and serum biochemical parameters, including liver enzymes, lipid profiles, and renal function indices, were assessed using an automated biochemical analyzer. The FIB−4 index was calculated using the following laboratory parameters:
Based on a meta-analysis of 37 studies (5,735 patients) for non-invasive diagnosis of advanced NAFLD fibrosis and thresholds recommended by Chinese guidelines for metabolic-associated fatty liver disease31,32, patients were stratified into three groups: minimal fibrosis (FIB-4 ≤ 1.3), significant fibrosis (1.3 < FIB-4 < 2.67), and advanced fibrosis (FIB-4 ≥ 2.67). These cutoff values have been extensively validated for non-invasive assessment of liver fibrosis, with FIB-4 < 1.3 effectively excluding advanced fibrosis and FIB-4 ≥ 2.67 indicating advanced fibrosis, and have been widely applied in multiple studies evaluating AIS outcomes24,26,28,29.
Clinical outcomes and follow-up assessment
The primary clinical endpoint was poor functional outcome at 90 days post-MT, defined as a modified Rankin Scale (mRS) score of 3–6. Secondary endpoints included hemorrhagic transformation (HT) and symptomatic intracranial hemorrhage (sICH). All patients underwent cranial CT scans at 24 and 72 h post-MT. According to the European Cooperative Acute Stroke Study-III criteria33, HT was classified into hemorrhagic infarction (HI−1: petechial hemorrhage along the margins of the infarct; HI−2: confluent hemorrhage within the infarcted area without mass effect) and parenchymal hemorrhage (PH−1: ≤30% of the infarcted area with mild mass effect; PH−2: >30% of the infarcted area with significant mass effect). sICH was defined as any intracranial hemorrhage associated with either a ≥ 4-point increase in total NIHSS score or a ≥ 2-point increase in any single NIHSS item from baseline, or requiring interventions such as endotracheal intubation, decompressive craniectomy, external ventricular drainage, or other significant medical interventions, with no other identifiable cause.
Follow-up assessments were conducted at 90 days post-stroke via telephone interviews by specially trained research coordinators. Functional status and all-cause mortality data were collected during follow-up. For deceased patients, preliminary information was obtained from family members and subsequently verified through death certificates from treating hospitals or community hospitals to ensure data accuracy and completeness. To maintain assessment consistency and reliability, all follow-up evaluations were performed by rigorously trained personnel. Assessment results were entered in real-time into the National Cerebrovascular Disease Big Data Platform (Stroke Center Construction Information Management System) for centralized data management and analysis.
Statistical analysis
Statistical analyses were performed using R software (Version 4.2.2). The Shapiro-Wilk test was used to assess the normality of continuous variables. Normally distributed continuous variables were presented as mean ± standard deviation and compared using independent samples t-tests, while non-normally distributed continuous variables were expressed as median (interquartile range [IQR]) and compared using Mann-Whitney U tests. Categorical variables were presented as frequencies and percentages, with between-group differences analyzed using Pearson’s chi-square test or Fisher’s exact test as appropriate. The predictive value of the FIB−4 index was evaluated using receiver operating characteristic (ROC) curves, with calculation of the area under the curve (AUC), optimal cutoff values, sensitivity, and specificity (Supplementary Table S1).
To examine the association between FIB−4 index and poor outcomes, we constructed three progressively adjusted multivariable logistic regression models. Model 1 was unadjusted; Model 2 was adjusted for demographic and clinical factors (age, hyperlipidemia, atrial fibrillation, baseline NIHSS score, and GCS score); and Model 3 was further adjusted for procedural parameters and laboratory measures (number of thrombectomy attempts, successful reperfusion status, white blood cell count, neutrophil count, lymphocyte count, platelet count, fasting glucose, creatinine, and uric acid levels). Model performance was assessed using Akaike Information Criterion (AIC), corrected AIC (AICc), Bayesian Information Criterion (BIC), Tjur’s R², root mean square error (RMSE), and percentage of correct predictions (PCP) (Supplementary Table S2). To investigate the association between FIB−4 index and 90-day mRS scores, we developed three similarly adjusted multivariable linear regression models, with covariate selection and adjustment strategies matching those of the logistic regression models. Multiple indicators were used to evaluate model performance, including R² (proportion of variance explained), RMSE, AIC, AICc, and BIC (Supplementary Table S3).
To explore potential nonlinear relationships, we performed restricted cubic spline regression analyses, with optimal knot placement determined by AIC. Three spline terms were generated to model nonlinear associations, and the statistical significance of each spline term was evaluated (Supplementary Table S4). Model goodness-of-fit was assessed using R-squared, adjusted R-squared, residual standard error, and F-tests (Supplementary Table S5).
Subgroup analyses were conducted based on sex, age (< 60 vs. ≥60 years), vascular risk factors, and TOAST classification, informed by previous evidence and biological plausibility. Sex stratification was based on documented differences in fibrosis progression between males and females, while TOAST classification stratification considered how different etiological mechanisms might influence the association between FIB−4 and outcomes. Effect modification was assessed by introducing interaction terms (FIB−4 × stratification variable) into the multivariable models. The statistical significance of interaction terms was evaluated using likelihood ratio tests, with P < 0.1 considered indicative of significant interaction. All statistical tests were two-sided, with P < 0.05 considered statistically significant.
Results
Demographic and clinical characteristics
Among 421 patients with LVO-AIS who underwent MT (Table 1), 283 (67.2%) were male, with a median age of 68 years (IQR, 57–76 years). At 90-day follow-up, 254 patients (60.3%) had poor functional outcomes (mRS 3–6). During hospitalization, HT occurred in 197 patients (46.8%), of whom 76 (18.1%) developed sICH.
Patients with poor outcomes were significantly older (median age 69 vs. 64 years, P < 0.001) and had a greater burden of vascular risk factors. While hypertension was the most prevalent comorbidity (68.7%), followed by atrial fibrillation (41.1%), diabetes mellitus (29.7%), and hyperlipidemia (23.5%), the poor outcome group exhibited a higher prevalence of atrial fibrillation (46.1% vs. 33.5%, P = 0.011) but a lower prevalence of hyperlipidemia (19.6% vs. 29.3%, P = 0.022).
Neurological assessment at admission revealed more severe functional deficits in the poor outcome group, as evidenced by higher baseline NIHSS scores (median 17 vs. 13, P < 0.001) and lower GCS scores (median 11 vs. 14, P < 0.001). Regarding treatment characteristics, 40.4% of patients received intravenous thrombolysis prior to MT. Successful reperfusion was achieved in 38.0% of patients, with a higher rate observed in the good outcome group (43.7% vs. 34.3%, P = 0.050). The poor outcome group required more thrombectomy attempts (median 2 vs. 1, P = 0.003).
Laboratory findings
Laboratory investigations (Table 2) revealed marked inflammatory responses and metabolic disturbances in the poor outcome group. These patients demonstrated elevated white blood cell counts (12.5 vs. 10.7 × 109/L, P < 0.001), increased neutrophil counts (10.7 vs. 8.6 × 109/L, P < 0.001), and decreased lymphocyte counts (0.93 vs. 1.22 × 109/L, P < 0.001). Regarding metabolic parameters, patients with poor outcomes exhibited higher fasting glucose levels (7.94 vs. 6.87 mmol/L, P < 0.001) and lower platelet counts (196 vs. 210 × 109/L, P = 0.013). Additionally, the poor outcome group showed elevated levels of creatinine (75 vs. 72 µmol/L, P = 0.008), uric acid (336 vs. 318 µmol/L, P = 0.037), and aspartate aminotransferase (26 vs. 24 U/L, P = 0.007).
Association of FIB−4 index with clinical outcomes
The FIB−4 index was significantly higher in patients with poor outcomes compared to those with good outcomes (2.30 vs. 1.75, P < 0.001; Table 2; Fig. 1). Quartile analysis revealed that patients with poor outcomes had a markedly higher proportion in Q4 (FIB−4 ≥ 3.01; 34.3% vs. 11.4%) and a significantly lower proportion in Q1 (FIB−4 < 1.35; 19.7% vs. 32.9%, P < 0.001). Based on threshold values recommended by meta-analyses and Chinese guidelines, patients were stratified into minimal fibrosis (FIB−4 ≤ 1.30; n = 89, 21.1%), significant fibrosis (1.30 < FIB−4 < 2.67; n = 191, 45.4%), and advanced fibrosis (FIB−4 ≥ 2.67; n = 141, 33.5%) groups. The poor outcome group demonstrated a higher proportion of advanced fibrosis (43.7% vs. 18.0%) and a lower proportion of minimal fibrosis (15.4% vs. 29.9%, P < 0.001).
The FIB−4 index also showed significant associations with hemorrhagic complications (Table 3; Fig. 2). Patients who developed HT had higher FIB−4 indices (2.29 vs. 1.77, P < 0.001), with a greater proportion in Q4 (32.0% vs. 19.2%) and a smaller proportion in Q1 (19.8% vs. 29.5%, P < 0.001). This pattern was more pronounced in patients with sICH, who exhibited substantially higher FIB−4 indices (2.97 vs. 1.88, P < 0.001). The proportion of advanced fibrosis was particularly high among patients with sICH (55.3% vs. 30.3% in significant fibrosis and 14.5% in minimal fibrosis groups, P < 0.001).
Predictive Performance of FIB−4 Index for Clinical Outcomes. Receiver operating characteristic curves comparing predictive performance of FIB−4 index analyzed as continuous variable (red), quartiles (blue), and clinical categories (green) for (A) 90-day poor outcome, (B) hemorrhagic transformation, and (C) symptomatic intracranial hemorrhage. Continuous FIB−4 showed modest discrimination for poor outcomes (AUC = 0.652, 95% CI: 0.600−0.704), with similar performance for HT (AUC = 0.597, 95% CI: 0.543–0.651) and sICH (AUC = 0.651, 95% CI: 0.575–0.727). Diagonal gray lines indicate random prediction (AUC = 0.5). AUC indicates area under the curve; CI, confidence interval.
Predictive value of FIB−4 index for clinical outcomes
ROC curve analysis (Fig. 2) demonstrated moderate predictive capability of the FIB−4 index whether analyzed as a continuous variable (AUC = 0.652), quartiles (AUC = 0.637), or clinical categories (AUC = 0.650). When analyzed as a continuous variable, the optimal cutoff value was 2.681, yielding a sensitivity of 83% and specificity of 43%. Regarding hemorrhagic complications, the FIB−4 index showed better predictive value for sICH (AUC = 0.651) than for HT (AUC = 0.597). For sICH, a cutoff value of 2.955 achieved 79% sensitivity and 50% specificity (Supplementary Table S1).
Associations of FIB−4 index with poor outcome
Multivariable logistic regression analysis revealed that the FIB−4 index independently predicted poor outcomes at 90 days (Table 4). In the fully adjusted model (Model 3), each unit increase in FIB−4 index was associated with a 38% higher risk of poor outcome (OR = 1.38, 95% CI: 1.11–1.77, P = 0.013). Quartile analysis showed that compared with Q1, patients in Q4 had significantly higher risk of poor outcomes, an association that persisted after comprehensive adjustment (Model 3: OR = 3.13, 95% CI: 1.06–9.30, P = 0.040). Similarly, when grouped by clinical thresholds, the advanced fibrosis group (FIB−4 ≥ 2.67) demonstrated higher risk of poor outcomes compared to the minimal fibrosis group (Model 3: OR = 3.29, 95% CI: 1.17–9.25, P = 0.024). Trend analysis revealed a significant dose-dependent relationship between increasing FIB−4 levels and poor outcomes (P for trend = 0.017).
Associations of FIB−4 index with 90-Day mRS scores
Linear regression analysis further confirmed the independent association between FIB−4 index and 90-day mRS scores (Table 5). In the fully adjusted model (Model 3), each unit increase in FIB−4 index was associated with a 0.25-point increase in mRS score (95% CI: 0.13–0.38, P < 0.001). Quartile analysis demonstrated that compared with Q1, patients in Q4 had significantly higher mRS scores (β=1.22, 95% CI: 0.52–1.92, P < 0.001). Similarly, the advanced fibrosis group (FIB−4 ≥ 2.67) showed a 1.21-point higher mRS score compared to the minimal fibrosis group (95% CI: 0.52–1.89, P < 0.001). This association exhibited a significant dose-dependent trend (P for trend < 0.001).
Nonlinear associations between FIB−4 index and poor outcome
Using the AIC principle, knots were automatically placed at the 5th, 27.5th, 50th, 72.5th, and 95th percentiles. Restricted cubic spline analysis revealed significant nonlinear associations between FIB−4 index and poor outcomes (Fig. 3). After comprehensive adjustment for confounders, the relationship between FIB−4 index and poor outcomes demonstrated nonlinear characteristics (P-overall = 0.001; P-nonlinear = 0.010). The risk increased exponentially when the FIB−4 index exceeded 2.4.
Nonlinear Relationship Between FIB−4 Index and Poor Outcomes. Restricted cubic spline analyses showing nonlinear associations between FIB−4 index and 90-day poor functional outcomes across three models: (A) unadjusted, (B) adjusted for clinical factors, and (C) fully adjusted for clinical and laboratory parameters. Red lines show odds ratios with 95% confidence intervals (pink shading). Blue histograms display FIB−4 index distribution. All models revealed significant nonlinearity (P < 0.01) with consistent break-points at FIB−4 = 2.4, above which risk increased exponentially. Dashed lines at odds ratio = 1 indicate reference level.
Subgroup analysis
Subgroup analyses revealed heterogeneity in the association between FIB−4 index and 90-day poor outcomes across different patient populations (Fig. 4). Significant effect modification was observed by sex (P for interaction = 0.012), with stronger associations in males (OR = 1.88, 95% CI: 1.36–2.59, P < 0.001) but non-significant associations in females (OR = 1.13, 95% CI: 0.82–1.55, P = 0.448). Similarly, significant interaction was found across TOAST classifications (P for interaction = 0.017), with the strongest association observed in cardioembolic stroke patients (OR = 2.22, 95% CI: 1.45–3.40, P < 0.001) and relatively weaker associations in large-artery atherosclerosis patients (OR = 1.14, 95% CI: 0.88–1.46, P = 0.317). No significant interactions were observed across other risk factor subgroups, including age, hypertension, diabetes, hyperlipidemia, coronary heart disease, atrial fibrillation, valvular heart disease, and history of stroke/TIA (all P for interaction > 0.05), suggesting the predictive value of FIB−4 index remained consistent across these subgroups.
Differential Associations of FIB−4 Index Across Patient Subgroups. Forest plot showing adjusted odds ratios for the association between FIB−4 index (per unit increase) and poor functional outcome across prespecified subgroups. Squares represent point estimates of odds ratios, with horizontal lines indicating 95% confidence intervals. Square sizes are proportional to subgroup sample sizes. Significant interactions were observed for sex (P for interaction = 0.012) and TOAST classification (P for interaction = 0.017), with stronger associations observed in males (OR = 1.88, 95% CI: 1.36–2.59) and patients with cardioembolic stroke (OR = 2.22, 95% CI: 1.45–3.40). The vertical dashed line represents an odds ratio of 1.
Discussion
In this retrospective cohort study of LVO-AIS patients undergoing MT, we identified several key findings regarding the prognostic value of the FIB−4 index. First, using threshold values validated by large-scale meta-analyses and recommended by Chinese clinical guidelines, approximately one-third (33.5%) of patients exhibited advanced liver fibrosis. Second, after comprehensive adjustment for potential confounders, the FIB−4 index showed significant associations with poor functional outcomes at 90 days, a relationship that remained consistent whether analyzed as a continuous variable, in quartiles, or by clinical thresholds. Notably, this association demonstrated marked nonlinearity, with risk increasing exponentially when the FIB−4 index exceeded 2.4. Furthermore, patients who developed HT or sICH exhibited significantly higher FIB−4 indices and a greater proportion of advanced fibrosis.
Our findings extend current understanding of the prognostic utility of the FIB−4 index in AIS. Previous studies have demonstrated that elevated FIB−4 indices correlate with multiple adverse outcomes, including more severe neurological deficits at admission, increased risk of hemorrhagic transformation, higher in-hospital mortality, poor functional outcomes, and increased stroke recurrence20,21,22,23,24,25. In patients receiving intravenous thrombolysis, the FIB−4 index has demonstrated particular prognostic value26,27,28. Chen et al.27 showed that, after adjusting for confounders, elevated FIB−4 levels were significantly associated with risks of both HT (adjusted OR = 1.340, 95% CI: 1.170–1.544) and sICH (adjusted OR = 1.358, 95% CI: 1.184–1.569). Similarly, Norata et al.28 found that compared to patients with minimal fibrosis (FIB−4 ≤ 1.3), those with advanced fibrosis (FIB−4 ≥ 2.67) demonstrated significantly higher rates of hemorrhagic complications and poor 90-day outcomes. In the context of MT, although research has been relatively limited, existing evidence highlights the significant predictive value of the FIB−4 index. Höfler et al.29 first revealed that elevated FIB−4 levels were significantly associated with poor functional outcomes (OR = 2.15, 95% CI: 1.21–3.83, P = 0.009) and mortality risk (OR = 2.16, 95% CI: 1.16–4.03, P = 0.01) at 3 months post-MT, although no association with hemorrhagic complications was found. Conversely, another cohort study identified elevated FIB−4 as an independent risk factor for post-MT sICH (OR = 1.306, 95% CI: 1.127–1.512, P = 0.001)34. Our study not only validates these associations in a different geographical and population context but also confirms the strong relationship between higher FIB−4 indices and both hemorrhagic complications and poor 90-day outcomes following MT, providing important complementary evidence to this field of research.
Multiple pathophysiological mechanisms may explain the association between liver fibrosis and poor outcomes in MT patients. Inflammatory response likely plays a central role in this process. Patients with liver fibrosis exhibit a state of chronic low-grade inflammation even before stroke onset. Du Plessis et al. demonstrated that the histological severity of NAFLD positively correlates with the expression of inflammation-regulatory genes and levels of pro-inflammatory mediators9,35. These patients typically show progressive elevation in levels of interleukin−8, tumor necrosis factor-α, and chemokine ligand 39. Wagner et al.10 further identified significantly elevated serum matrix metalloproteinase−9 (MMP−9) levels in these patients compared to controls. This finding is particularly significant given the established role of serum MMP−9 in blood-brain barrier disruption, vasogenic edema formation, and hemorrhagic transformation, as well as its crucial role in acute infarct expansion and disease progression in AIS patients36,37,38. During acute ischemic events, patients with liver fibrosis often demonstrate enhanced peripheral immune cell mobilization and tissue infiltration, potentially amplifying the inflammatory cascade and further compromising blood-brain barrier integrity11. Additionally, oxidative stress, serving as a common pathological foundation for both liver fibrosis and cardiovascular disease, directly damages blood-brain barrier structure through degradation of extracellular matrix components and disruption of tight junction proteins12,13. Moreover, advanced liver disease is accompanied by complex coagulation disorders that may simultaneously affect both thrombosis and bleeding risk16,17. The synergistic effects of these factors may exacerbate acute ischemic neuronal injury.
Liver fibrosis may also impair long-term neurological recovery through multiple mechanisms. Studies have revealed that hepatocytes in NAFLD patients release specific circulating extracellular vesicles that can activate vascular endothelial inflammatory responses, leading to cerebral microvascular barrier dysfunction14,39,40,41. This endothelial dysfunction, closely associated with insulin resistance and arterial stiffness, may delay post-stroke vascular remodeling and repair. Furthermore, hepatic dysfunction may exacerbate cerebral small vessel disease and white matter injury42, particularly in patients with high white matter lesion burden. The resulting disruption of white matter fiber network integrity and cerebral metabolic dysfunction can significantly impact neuroplasticity and functional reserve, ultimately hindering effective neurological recovery43,44.
Patients with LVO-AIS undergoing MT face unique and complex pathophysiological challenges, which may be particularly pronounced in those with liver fibrosis. LVO-AIS patients not only experience larger initial ischemic injuries and more extensive penumbra, but are also susceptible to a spectrum of reperfusion-related complications. Flow restoration can trigger severe reperfusion injury, amplification of secondary injury mechanisms (including increased risk of hemorrhagic transformation and cerebral edema), and more intense inflammatory cascade responses. As previously discussed, these pathophysiological cascades may be especially destructive in patients with liver fibrosis, as they already exhibit blood-brain barrier compromise due to chronic systemic inflammation and oxidative stress. The combination of pre-existing blood-brain barrier dysfunction and reperfusion-induced oxidative injury may create synergistic effects, significantly increasing susceptibility to post-MT hemorrhagic complications. Moreover, LVO-AIS patients inherently face elevated HT risk, which may be further amplified by liver fibrosis-associated coagulation disorders, as the latter involves complex hemodynamic disturbances affecting both coagulation and anticoagulation pathways. Additionally, secondary hepatic dysfunction and metabolic dysregulation associated with liver fibrosis may further compromise the physiological reserve in these critically ill patients.
Notably, our subgroup analyses revealed differential prognostic impacts of the FIB−4 index across patient populations, with the strongest associations observed in males and patients with cardioembolic stroke. These sex-specific differences may arise from multiple mechanisms. Androgens, particularly testosterone, play a crucial role in regulating liver fibrosis progression. Previous studies have demonstrated an inverse correlation between testosterone levels and fibrosis severity45. Conversely, another study found that females have a 37% higher risk of developing advanced fibrosis compared to males46. These hormonal influences may interact with stroke pathophysiology in a sex-specific manner. Furthermore, males typically exhibit more unfavorable lipid profiles, such as elevated low-density lipoprotein cholesterol and reduced high-density lipoprotein cholesterol levels, which may amplify the synergistic effects between liver fibrosis and atherosclerosis, thereby exacerbating stroke risk and outcomes47. The significant association observed in cardioembolic stroke patients may be mediated through liver fibrosis-induced cardiac remodeling and atrial fibrillation. Recent evidence suggests that liver fibrosis is associated with atrial structural remodeling and increased risk of atrial fibrillation, both established risk factors for cardioembolic stroke that can increase thrombus burden and stroke severity26.
Several important limitations should be acknowledged in our study. First, the retrospective observational design precludes establishment of a direct causal relationship between liver fibrosis and stroke outcomes. Although we adjusted for known confounders through multivariable regression analysis, we cannot completely rule out the potential influence of unmeasured or unknown confounding factors. Second, as a single-center cohort study, our findings may not fully represent the broader stroke population, potentially limiting the generalizability of our results. Patient characteristics, treatment protocols, and outcomes may vary across medical institutions, particularly in regions with different stroke care infrastructure or demographic characteristics. Third, methodological challenges exist in using day−1 post-admission FIB−4 index as a fibrosis marker. Acute stroke, as a severe systemic stress event, may significantly affect aminotransferase levels and platelet counts, thereby influencing FIB−4 calculations. Although the FIB−4 index is widely used for assessing liver fibrosis, its diagnostic performance in AIS patients has not been systematically validated. The lack of comparison with other validated non-invasive assessment methods (such as transient elastography or magnetic resonance elastography) limits our ability to confirm the accuracy of FIB−4 in this specific population.
These limitations provide direction for future research. Large-scale prospective multicenter validation studies are needed to confirm our findings and establish generalizability across different healthcare settings and patient populations. Such studies should incorporate multiple fibrosis assessment methods, including elastography techniques, to validate the utility of the FIB−4 index in stroke patients. Importantly, interventional trials are warranted to evaluate whether FIB−4-guided management strategies can effectively improve outcomes in high-risk populations.
Conclusion
Our study demonstrates that the FIB−4 index is independently associated with poor 90-day functional outcomes, with particularly strong associations observed in males and patients with cardioembolic stroke. This association exhibits marked nonlinearity, with risk increasing exponentially when the FIB−4 index exceeds 2.4. These findings suggest that the FIB−4 index may serve as a convenient biomarker for risk stratification in these patients, helping identify those who might benefit from enhanced monitoring and individualized treatment strategies. Although our results require further validation through prospective multicenter studies, they provide a foundation for developing personalized post-procedural treatment protocols for patients with concurrent liver fibrosis.
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author upon reasonable request.
References
Feigin, V. L. et al. World stroke organization: global stroke fact sheet 2025. Int. J. 20, 132–144 (2025).
Smith, W. S. et al. Significance of large vessel intracranial occlusion causing acute ischemic stroke and TIA. Stroke 40, 3834–3840 (2009).
Malhotra, K., Gornbein, J. & Saver, J. L. Ischemic strokes due to large-vessel occlusions contribute disproportionately to stroke-related dependence and death: a review. Front. Neurol. 8, 651 (2017).
Dhillon, P. S. et al. Perfusion imaging for endovascular thrombectomy in acute ischemic stroke is associated with improved functional outcomes in the early and late time windows. Stroke 53, 2770–2778 (2022).
Wang, J. et al. Characteristics of mortality after endovascular thrombectomy in patients with acute ischemic stroke. Clin. Interv Aging. 19, 2145–2155 (2024).
Younossi, Z. M. et al. Global epidemiology of nonalcoholic fatty liver disease-meta-analytic assessment of prevalence, incidence, and outcomes. Hepatology 64, 73–84 (2016).
Huang, D. Q., El-Serag, H. B. & Loomba, R. Global epidemiology of NAFLD-related HCC: trends, predictions, risk factors and prevention. Nat. Rev. Gastroenterol. Hepatol. 18, 223–238 (2021).
Ji, Y. X. et al. The deubiquitinating enzyme cylindromatosis mitigates nonalcoholic steatohepatitis. Nat. Med. 24, 213–223 (2018).
du Plessis, J. et al. Association of adipose tissue inflammation with histologic severity of nonalcoholic fatty liver disease. Gastroenterology 149, 635–648 (2015).
Wagner, J. et al. Fatty acid-binding protein-4 (FABP4) and matrix metalloproteinase-9 (MMP9) as predictive values for nonalcoholic steatohepatitis (NASH). Lipids Health Dis. 22, 1 (2023).
Farrell, G. C., van Rooyen, D., Gan, L. & Chitturi, S. NASH is an inflammatory disorder: pathogenic, prognostic and therapeutic implications. Gut Liver. 6, 149–171 (2012).
Polimeni, L. et al. Oxidative stress: new insights on the association of non-alcoholic fatty liver disease and atherosclerosis. World J. Hepatol. 7, 1325–1336 (2015).
Khatri, R., McKinney, A. M., Swenson, B. & Janardhan, V. Blood-brain barrier, reperfusion injury, and hemorrhagic transformation in acute ischemic stroke. Neurology 79, S52–S57 (2012).
Chen, X. et al. Hepatic steatosis aggravates atherosclerosis via small extracellular vesicle-mediated Inhibition of cellular cholesterol efflux. J. Hepatol. 79, 1491–1501 (2023).
Virović-Jukić, L. et al. Non-alcoholic fatty liver disease - a procoagulant condition? Croat. Med. J. 62, 25–33 (2021).
Tripodi, A. Liver disease and hemostatic (dys)function. Semin Thromb. Hemost. 41, 462–467 (2015).
Rios, R., Sangro, B., Herrero, I., Quiroga, J. & Prieto, J. The role of thrombopoietin in the thrombocytopenia of patients with liver cirrhosis. Am. J. Gastroenterol. 100, 1311–1316 (2005).
Riazi, K. et al. The prevalence and incidence of NAFLD worldwide: a systematic review and meta-analysis. Lancet Gastroenterol. Hepatol. 7, 851–861 (2022).
Estes, C. et al. Modeling Nafld disease burden in China, France, Germany, Italy, Japan, Spain, united Kingdom, and united States for the period 2016–2030. J. Hepatol. 69, 896–904 (2018).
Tziomalos, K. et al. Association between nonalcoholic fatty liver disease and acute ischemic stroke severity and outcome. World J. Hepatol. 5, 621–626 (2013).
Ztriva, E. et al. Hepatic fibrosis is a risk factor for greater severity and worse outcome of acute ischemic stroke. J. Clin. Med. 11, 5141 (2022).
Zhu, H. J. et al. Prognostic value of fibrosis-4 in acute ischemic stroke patients undergoing intravenous thrombolysis. Clin. Interv Aging. 19, 1663–1674 (2024).
Eto, F. et al. Liver fibrosis index is associated with functional outcome among acute ischemic stroke patients. J. Stroke Cerebrovasc. Dis. 33, 107537 (2024).
Baik, M. et al. Advanced liver fibrosis predicts unfavorable long-term prognosis in first-ever ischemic stroke or transient ischemic attack. Cerebrovasc. Dis. 49, 474–480 (2020).
Abdeldyem, S. M., Goda, T., Khodeir, S. A., Abou Saif, S. & Abd-Elsalam, S. Nonalcoholic fatty liver disease in patients with acute ischemic stroke is associated with more severe stroke and worse outcome. J. Clin. Lipidol. 11, 915–919 (2017).
Toh, E. M. S. et al. Risk of liver fibrosis is associated with more severe strokes, increased complications with thrombolysis, and mortality. J. Clin. Med. 12, 356 (2023).
Chen, J., Li, X., Hu, R. & Hu, C. The clinical value of fibrosis indices for predicting the hemorrhagic transformation in patients with acute ischemic stroke after intravenous thrombolysis. Front. Aging Neurosci. 16, 1492410 (2024).
Norata, D. et al. Liver fibrosis-4 score predicts outcome of patients with ischemic stroke undergoing intravenous thrombolysis. Front. Neurol. 14, 1103063 (2023).
Fandler-Höfler, S. et al. Non-invasive markers of liver fibrosis and outcome in large vessel occlusion stroke. Ther. Adv. Neurol. Disord. 14, 17562864211037239 (2021).
Zaidat, O. O. et al. Recommendations on angiographic revascularization grading standards for acute ischemic stroke: a consensus statement. Stroke 44, 2650–2663 (2013).
Mózes, F. E. et al. Diagnostic accuracy of non-invasive tests for advanced fibrosis in patients with NAFLD: an individual patient data meta-analysis. Gut 71, 1006–1019 (2022).
Chinese Society of Hepatology. Guidelines for the prevention and treatment of metabolic dysfunction-associated (non-alcoholic) fatty liver disease (Version 2024). Zhonghua Gan Zang Bing Za Zhi. 32, 418–434 (2024).
Hacke, W. et al. Intravenous thrombolysis with Recombinant tissue plasminogen activator for acute hemispheric stroke. JAMA 274, 1017–1025 (1995).
Xu, J. et al. Relationship between liver fibrosis and increased risk of symptomatic intracranial hemorrhage in ischemic stroke patients undergoing mechanical thrombectomy. Neuropsychiatr Dis. Treat. 20, 101–108 (2024).
du Plessis, J. et al. Pro-inflammatory cytokines but not endotoxin-related parameters associate with disease severity in patients with NAFLD. PLoS One. 11, e0166048 (2016).
Ling, C., Cao, S. & Kong, X. Changes of FSTL1 and MMP-9 levels in patients with acute cerebral infarction and its relationship with hemorrhagic transformation. J. Clin. Neurosci. 99, 164–168 (2022).
Ramos-Fernandez, M., Bellolio, M. F. & Stead, L. G. Matrix metalloproteinase-9 as a marker for acute ischemic stroke: a systematic review. J. Stroke Cerebrovasc. Dis. 20, 47–54 (2011).
Demir, R. et al. Relationship between plasma metalloproteinase-9 levels and volume and severity of infarct in patients with acute ischemic stroke. Acta Neurol. Belg. 112, 351–356 (2012).
Zuo, R. et al. Hepatic small extracellular vesicles promote microvascular endothelial hyperpermeability during NAFLD via novel-miRNA-7. J. Nanobiotechnol. 19, 396 (2021).
Zhao, X. et al. Communication between nonalcoholic fatty liver disease and atherosclerosis: focusing on exosomes. Eur. J. Pharm. Sci. 193, 106690 (2024).
Jiang, F. et al. Hepatocyte-derived extracellular vesicles promote endothelial inflammation and atherogenesis via microRNA-1. J. Hepatol. 72, 156–166 (2020).
Kim, Y. D. et al. Relationship between cerebral microbleeds and liver stiffness determined by transient elastography. PLoS One. 10, e0139227 (2015).
Lawrence, A. J. et al. Structural network efficiency is associated with cognitive impairment in small-vessel disease. Neurology 83, 304–311 (2014).
Etherton, M. R. et al. White matter integrity and early outcomes after acute ischemic stroke. Transl Stroke Res. 10, 630–638 (2019).
Sarkar, M. A. et al. Testosterone is associated with nonalcoholic steatohepatitis and fibrosis in premenopausal women with NAFLD. Clin. Gastroenterol. Hepatol. 19, 1267–1274 (2021).
Balakrishnan, M. et al. Women have a lower risk of nonalcoholic fatty liver disease but a higher risk of progression vs men: a systematic review and meta-analysis. Clin. Gastroenterol. Hepatol. 19, 61–71 (2021).
Kumar, S., Duan, Q., Wu, R., Harris, E. N. & Su, Q. Pathophysiological communication between hepatocytes and non-parenchymal cells in liver injury from NAFLD to liver fibrosis. Adv. Drug Deliv Rev. 176, 113869 (2021).
Funding
This study was supported by the Xiamen Medical and Health Guidance Project (No. 3502Z20224ZD1061), the Natural Science Foundation of Xiamen (3502Z20227270) and the Fujian Provincial Key Medical Discipline Construction Project (050172).
Author information
Authors and Affiliations
Contributions
W.G., X.W. and Z.Z. : Conceptualization, data analysis, validation, writing. L.C. and S.J.: data analysis, writing. X.C. and S.W.: writing and editing the manuscript. R.Z.:investigation, review and editing. All authors read and approved the fnal manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics declarations
This study were approved by the Ethics Committee of the Affiliated Zhongshan Hospital of Xiamen University (No. xmzsyyky2022-196).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Gao, W., She, J., Wu, X. et al. Association of liver fibrosis−4 index with functional outcomes in chinese patients with acute ischemic stroke undergoing mechanical thrombectomy. Sci Rep 15, 13086 (2025). https://doi.org/10.1038/s41598-025-98426-w
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-98426-w