Abstract
Neonatal mammalian hearts are capable of regenerating by inducing cardiomyocyte proliferation after injury. However, this regenerative capability in adult mammalian hearts almost disappears. Extracellular vesicles (EVs) have been shown to play vital cardioprotective roles in heart repair. Here, we report that EVs from regenerating neonatal heart tissues, after apical resection surgery (AR-Neo-EVs), exhibit stronger pro-proliferative, anti-apoptotic, and pro-angiogenesis activities than EVs from neonatal mouse cardiac tissues (Neo-EVs), effects which are absent in adult mouse heart-derived EVs (Adu-EVs). Proteomic analysis reveals the expression of Wdr75 protein, a regulator of p53, is higher in AR-Neo-EVs than in Neo-EVs. It is shown the regenerative potential of AR-Neo-EVs is abrogated when Wdr75 is knocked down. We further show that delivery of AR-Neo-EVs by sodium alginate hydrogel microspheres is an effective treatment in myocardial infraction. This work shows the potential of using EVs from regenerating tissue to trigger protective and regenerative mechanisms.
Similar content being viewed by others
Introduction
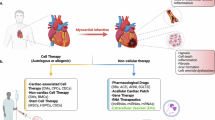
Myocardial infarction (MI) poses a serious threat to human health, with its occurrence and death rates rising annual1. In the event of MI, localized ischemia and hypoxia lead to necrosis, apoptosis, and other types of death of numerous functional cardiomyocytes, and the occlusion of blood vessels hinders the transport of nutrients needed to repair the damaged myocardium. The loss of beating cardiomyocytes are replaced by fibrous scar tissue, which in turn causes ventricular remodeling, decline in cardiac function, and eventual development of heart failure2. Lately, interventional, surgical, and pharmacologic therapies have been shown to improve cardiac function to a certain extent, but they fail to replenish the cardiomyocytes lost during infarction3. Therefore, it is of great significance to find the therapeutic strategies to that promote cardiac regeneration4.
Adult mammalian cardiomyocytes exist from the proliferation cycle and exhibit a limited ability to self-repair after myocardial injury, leading to irreversible loss of functional cardiomyocytes. On the contrary, neonatal mammalian hearts maintain their regenerative capacity within 7 days after birth, which may replenish the lost cardiomyocytes through division and proliferation upon injury stimulation. Sadek et al. conducted left ventricular apical resection (AR) in 1-day-old mice and found that myocardial regeneration and cardiac function restoration were achieved through autogenetic cardiomyocyte proliferation after resection. The regenerative capacity of neonatal mice heart gradually diminishes with development and maturation5,6,7,8. The discovery of regenerative ability of the neonatal hearts provides crucial insights into therapeutic strategies for the treatment of MI in adults. A series of studies reveal that the activation of cardiomyocyte proliferation is a complex physiological process mediated by multiple factors. However, how to take full advantage of the regenerative capacity of neonatal mice to regulate cardiac repair in adults has not been fully elucidated.
Extracellular vesicles (EVs), natural lipid bilayer vesicles, contain a variety of biologically active substances such as proteins, lipids, and nucleic acids, which are important carriers of intercellular communication9,10,11,12,13,14. EVs not only mimic the function of the source cells, but also have advantages that traditional cell therapies do not have, including low immunogenicity, no cytotoxicity, and the ability to penetrate biological barriers14,15,16. In recent years, cell-free therapeutic strategies based on EVs have shown remarkable potential in the treatment of cardiovascular diseases such as acute myocardial infarction, heart failure, and cardiomyopathy17,18,19,20. However, extensive research has focused on the EVs extracted from the supernatants of cells and various body fluids. Evidence is mounting that tissue-derived EVs can more accurately reflect the specific microenvironment of their originating tissues, which also have potential applications in the prevention and treatment of myocardial injury. Nevertheless, the current attention on tissue-derived EVs related to cardiac regeneration and repair remains insufficient.
In this work, we revealed that the EVs derived from neonatal mouse cardiac tissues (Neo-EVs) exhibited the pro-proliferative, anti-apoptotic, and pro-angiogenesis activities, which were absent in adult mouse heart-derived extracellular vesicles (Adu-EVs). Surprisingly, compared to Neo-EVs, the EVs from regenerating neonatal heart tissues by AR surgery (AR-Neo-EVs) showed stronger ability to promote cardiogenesis and angiogenesis in adult infarction hearts. Furthermore, the low retention rate of EVs in vivo is one of the main reasons for the limited therapeutic effect. In order to overcome the problem of low tissue retention by direct injection of EVs, we further prepared AR-Neo-EVs encapsulated with sodium alginate-based hydrogel microspheres (MS), and found that EVs delivered in the form of MS were more effective in the treatment of MI. These results suggest that this biomaterials-based approach can be effective in preparing high yields of bioactive EVs from cardiac tissues for the treatment of ischemic cardiac tissues, which is of potential clinical value in the future treatment of cardiac injury.
Results
Influences of Neo-EVs, AR-Neo-EVs, and Adu-EVs on cardiomyocyte cell cycle re-entry and apoptosis in vitro
First of all, to investigate the potential impact of neonatal cardiac tissue-derived EVs on cardiac regeneration, we sequentially collected EVs derived from Neo-EVs, AR-Neo-EVs, and Adu-EVs following the experimental procedure as depicted in Fig. 1a. Transmission electron microscope (TEM) and nanoparticle tracking analysis (NTA) showed a typical cup-shaped morphology of EVs with sizes of 100–150 nm in each group (Fig. 1b, c). In addition, Western blotting confirmed the presence of the EVs-typical biomarkers TSG101, CD63, and Flotillin 1 in cardiac tissue-derived EVs, indicating the successful extraction of EVs from cardiac tissues (Fig. 1d).
a Flow chart for the extracellular vesicles (EVs) purification procedure based on differential ultracentrifugation. Created in BioRender. gN, fW. (2025) https://BioRender.com/c15j088b Transmission electron microscope (TEM) of Neo-EVs, AR-Neo-EVs, and Adu-EVs. Scale bar = 100 nm. c Size distribution of Neo-EVs, AR-Neo-EVs, and Adu-EVs, as determined by nanoparticle tracking analysis (NTA). d The expression of typical EVs markers TSG101, CD63, and Flotillin 1 detected by Western blot. e PKH26-labeled EVs were co-cultured with cardiomyocytes for 6 h. Endocytosed EVs (PKH26, red) can be seen within the cytoplasm of cardiomyocytes (α-Actinin, green). Scale bar = 5 μm. f The effects of Neo-EVs, AR-Neo-EVs, and Adu-EVs on cardiomyocyte proliferation analyzed by the detection of Ki67, pH3, and EdU. Ki67, pH3, and EdU marked proliferating cells (red), α-Actinin labeled cardiomyocytes (green), and DAPI labeled nuclei (blue). Scale bar = 20 μm. White arrows point the positive cardiomyocytes. g–i Quantitative analysis of the Ki67, pH3, and EdU proliferation assay (n = 5 independent experiments). *p < 0.05, **p < 0.01, ***p < 0.001 vs. Ctl, ***p < 0.001 vs. Neo-EVs. j The effects of Neo-EVs, AR-Neo-EVs, and Adu-EVs on cardiomyocyte apoptosis analyzed by TUNEL staining. TUNEL marked apoptosis cells (red) and DAPI labeled nuclei (blue). Scale bar = 20 μm. k Quantitative analysis of the TUNEL assay (n = 5 independent experiments). ***p < 0.001 vs. Ctl, ***p < 0.001 vs. Hypoxia, *p < 0.05 vs. Hypoxia+Neo-EVs. One-way ANOVA followed by Tukey’s Multiple Comparisons test. Error bars represent the mean ± SEM of each group. Source data are provided as a Source Data file. Exact p values are provided in the Source Data file.
To further determine the biological effects of Neo-EVs, AR-Neo-EVs, and Adu-EVs on cardiomyocytes, we initially co-cultured PKH26-labeled EVs with neonatal mouse cardiomyocytes (NMCMs) for 6 h. Subsequently, an intense red fluorescence was observed in NMCMs, indicating that the cardiac tissue-derived EVs were effectively internalized by cardiomyocytes (Fig. 1e). Cardiomyocytes renewal by cell cycle re-entry has been confirmed as a key strategy for cardiac regeneration. Therefore, we then added different qualities of cardiac tissue-derived EVs of each group into NMCMs and evaluated the proliferation capacity of cardiomyocytes by Ki67 fluorescence staining and EdU incorporation assay, and thus determined the optimal bioactive concentration of EVs for the regulation of cardiomyocytes. The results showed that compared with the Ctl and Adu-EVs groups, Neo-EVs and AR-Neo-EVs increased the number of Ki67- and EdU-positve cardiomyocytes in a dose-dependent manner, with the most pronounced effect of the EVs at 90 μg, which was used in our follow-up studies (Supplementary Fig. 1). Intriguingly, it was a surprised discovery that compared with the Neo-EVs, AR-Neo-EVs exhibited the stronger ability to re-entering the cell cycle (Fig. 1f–i). Meanwhile, cell counts and cell cycle-related factors also indicated that treatment with the AR-Neo-EVs increased cardiomyocytes division (Supplementary Fig. 2). These suggest that AR-Neo-EVs as a better EVs for heart regeneration. In addition, to determine the effect of neonatal cardiac tissue-derived EVs on cardiomyocytes apoptosis after hypoxia, TUNEL staining was performed on NMCMs after EVs intervention. The results showed that the number of TUNEL-positive cells was significantly reduced in both the Neo-EVs and AR-Neo-EVs groups compared with the hypoxia group. Quantitative analysis further showed that the apoptosis index in the AR-Neo-EVs was lower than that in the Neo-EVs. In contrast, the Adu-EVs did not exhibit anti-apoptotic effects on cardiomyocytes in vitro (Fig. 1j, k). These results indicated that AR-Neo-EVs have higher biological activities in inducing cardiomyocyte cell cycle re-entry and anti-apoptosis.
Effects of Neo-EVs, AR-Neo-EVs, and Adu-EVs on angiogenesis in vitro
It is well known that angiogenesis is of great significance for ameliorating ventricular remodeling and cardiac functions after MI15. Therefore, we further explored the effects of EVs from different cardiac tissues on the angiogenesis capacity of human umbilical vein endothelial cells (HUVECs) in vitro. Representative images showed a strong red fluorescence signal in HUVECs after co-incubation with PKH26-EVs for 6 h, indicating that cardiac tissue-derived EVs were effectively internalized by HUVECs (Fig. 2a). Subsequently, HUVECs were inoculated in matrix gel-coated well plates to assess the effects of different EVs on vascular tube formation in vitro. As illustrated in Fig. 2b–e, compared with Neo-EVs, AR-Neo-EVs treated HUVECs were able to form the more tubular networks, whereas Adu-EVs did not show the ability to enhance angiogenesis. The results described above suggested that AR-Neo-EVs could also markedly promote the new blood vessels formation of HUVECs in vitro. Additionally, wound healing experiment showed that Neo-EVs and AR-Neo-EVs enhanced the migration of endothelial cells, and AR-Neo-EVs had the better migration-promoting activity than Neo-EVs (Fig. 2f, g). Consistently, we isolated adult mouse cardiac endothelial cells and further demonstrated the stimulating effect of EVs derived from different cardiac tissues on angiogenesis (Supplementary Fig. 3). These results showed that AR-Neo-EVs have higher angiogenic activity.
a PKH26-labeled EVs were co-cultured with HUVECs for 6 h. Endocytosed EVs (PKH26, red) can be seen within the cytoplasm of HUVECs (CD31, green). Scale bar = 5 μm. b Tube formation experiments of HUVECs treated with different EVs. Scale bar = 150 μm. c–e Quantitative analysis of tube formation experiments (n = 5 independent experiments). ***p < 0.001 vs. Ctl, ***p < 0.001 vs. Neo-EVs. f Scratch migration experiments of HUVECs treated with different EVs. Scale bar = 150 μm. g Quantitative analysis of scratch migration experiments (n = 5 independent experiments). ***p < 0.001 vs. Ctl, ***p < 0.001 vs. Neo-EVs. One-way ANOVA followed by Tukey’s Multiple Comparisons test (c–e). Two-way ANOVA followed by Tukey’s Multiple Comparisons test (g). Error bars represent the mean ± SEM of each group. Source data are provided as a Source Data file. Exact p values are provided in the Source Data file.
Effects of Neo-EVs, AR-Neo-EVs, and Adu-EVs in cardiac regeneration of mice with MI
Based on the above findings, we further explored the effects of EVs from different sources on cardiac biological functions of adult MI mice as depicted in Fig. 3a. We established a MI model by ligating left anterior descending (LAD) branch of the coronary artery, followed by intramyocardial injection of Neo-EVs, AR-Neo-EVs, Adu-EVs, and PBS into the infarct border region. Echocardiography measurement showed that the values of left ventricular ejection fraction (EF) and shortening fraction (FS) were significantly reduced in MI group, which were markedly elevated by Neo-EVs and AR-Neo-EVs treatment. Notably, AR-Neo-EVs had a more substantial effect on protecting cardiac functions of mice compared to Neo-EVs. However, cardiac functions were comparable between MI and Adu-EVs-treatment mice (Fig. 3b, c). Meanwhile, Masson’s trichrome and Sirius Red stainings revealed a notable reduced cardiac fibrosis area in the Neo-EVs and AR-Neo-EVs-treated mice compared with the Adu-EVs group (Fig. 3d, e and Supplementary Fig. 4a, b). Consistent with these results, quantitative real-time PCR (qRT-PCR) experiments also showed that Neo-EVs and AR-Neo-EVs significantly decreased the Collagen type I alpha 1 (Col1a1) and Collagen type III alpha 1 (Col3a1) mRNA levels (Supplementary Fig. 4c, d). All of above indicated that AR-Neo-EVs showed better potential to inhibit myocardial remodeling than Neo-EVs. Immunofluorescence of heart tissue showed that AR-Neo-EVs treatment could obviously increase the number of Ki67-, pH3-, and Aurora B-positive cardiomyocytes in the border region of MI mice hearts but not the remote region (Fig. 3f–i and Supplementary Fig. 4e–g). Subsequently, we isolated adult mice cardiomyocytes from each group based on Langendorff perfusion, and determined the number of mono-, bi-, and multi-nucleated cardiomyocytes. The results showed that the number of mono-nucleated adult cardiomyocytes in the Neo-EVs and AR-Neo-EVs groups was significantly increased compared with the group of MI and MI+Adu-EVs (Fig. 3j, k). Wheat germ agglutinin (WGA) staining revealed that cardiomyocytes exhibited a smaller cross-sectional area in MI + AR-Neo-EVs group (Supplementary Fig. 4h, i). Meanwhile, immunofluorescence results of the heart sections also showed that MI + AR-Neo-EVs treatment significantly increased the percentage of mono-nucleated cardiomyocytes and decreased the percentage of bi-nucleated cardiomyocytes (Supplementary Fig. 4j). Similar to the results obtained from NMCMs in vitro, we observed a significantly reduced number of apoptotic cardiomyocytes in the border region of MI mice treated with AR-Neo-EVs compared to the other groups (Fig. 3l, m and Supplementary Fig. 4k–m). All the above experiments demonstrate the EVs obtained from AR myocardial regeneration model enhanced cardiomyocyte cell cycle re-entry and reduced apoptosis of adult mice cardiomyocytes. To further confirm the stimulatory effect of EVs on angiogenesis in vivo, we assessed by flow cytometry analysis and immunofluorescence staining for CD31. The group of AR-Neo-EVs showed a better ability to stimulate the formation of new blood vessels (Fig. 3n, o and Supplementary Fig. 4n, o). In addition, Western blot experiments suggested that CD31 protein expression level was significantly increased in the MI+Neo-EVs and MI + AR-Neo-EVs groups, but no significant difference was observed between the Sham, MI, and MI+Adu-EVs groups (Supplementary Fig. 4p). These results indicated that AR-Neo-EVs could markedly improve cardiac functions post-MI in vivo.
a Schematic diagram. Created in BioRender. gN, fW. (2025) https://BioRender.com/j56n116 (b, c) Representative echocardiogram images and quantification of the ejection fraction (EF) and fractional shortening (FS) in the Sham, MI, MI+Neo-EVs, MI + AR-Neo-EVs, and MI+Adu-EVs groups on Day 28 after MI (n = 5 independent mice). ***p < 0.001 vs. Sham, **p < 0.01, ***p < 0.001 vs. MI, *p < 0.05 vs. MI+Neo-EVs. d, e Masson’s trichrome staining and infract area quantification of heart sections at Day 28 post-MI (n = 5, 3, 4, 4, 3 independent mice). Scale bar = 500 μm. **p < 0.01, ***p < 0.001 vs. MI, ***p < 0.001 vs. MI+Neo-EVs. f–i Representative immunofluorescence images and quantification of the Ki67, pH3, and Aurora B in the border region of adult mice at Day 7 after MI (n = 5 independent mice). Ki67, pH3, and Aurora B marked proliferating cells (red), α-Actinin labeled cardiomyocytes (green), and DAPI labeled nuclei (blue). Scale bar = 20 μm. White arrows point the positive cardiomyocytes. ***p < 0.001 vs. MI, ***p < 0.001 vs. MI+Neo-EVs. j, k Representative images and quantification of the number of mono-, bi-, and multi-nucleated cardiomyocytes in total cardiomyocytes (n = 4 independent mice). Scale bar = 50 μm. *p < 0.05, ***p < 0.001 vs. MI, *p < 0.05 vs. MI+Neo-EVs. l, m Representative flow cytometry images and quantification of Annexin V-FITC/PI staining was conducted to assess the apoptosis cells in EVs-treated mice hearts on Day 7 post-MI (n = 3 independent mice). ***p < 0.001 vs. Sham, *p < 0.05, ***p < 0.001 vs. MI, **p < 0.01 vs. MI+Neo-EVs. n, o Representative flow cytometry images and quantification of CD31-FITC-H staining was conducted to CD31+ cells in EVs-treated mice hearts on Day 7 post-MI (n = 3 independent mice). ***p < 0.001 vs. MI, ***p < 0.001 vs. MI+Neo-EVs. One-way ANOVA followed by Tukey’s Multiple Comparisons test (c, e, g, h, i, m, o). Two-way ANOVA followed by Sidak’s Multiple Comparisons test (k). Error bars represent the mean ± SEM of each group. Source data are provided as a Source Data file. Exact p values are provided in the Source Data file.
Preparation and characterization of injectable sodium alginate hydrogel microspheres (MS)
EVs-therapy has been proven to be a powerful alternative to cell therapy due to its small size, low immunogenicity, and good permeability16. Nevertheless, the short half-life and poor tissue retention of EVs are still the major challenges for EVs-therapy17,18,19. Thus, there is an urgent need to utilize the better regenerative capacity of AR-Neo-EVs while avoiding the problem of rapid clearance of EVs in vivo. Recently, MS have gained public attention due to their superior timeliness and stability20,21,22,23. In this study, we employed microfluidic technology to prepare EVs encapsulated sodium alginate hydrogel MS for sustained delivery of EVs in the infarct border region (Fig. 4a). Under the optical microscope, we clearly observed that the MS were evenly distributed in the solution with an average particle size of about 50 μm (Fig. 4b, c), and possessed smooth and intact surfaces revealed by the scanning electron microscope (SEM) (Fig. 4d). Further observation showed that PKH26-labeled EVs were uniformly dispersed within the MS (Fig. 4e). Additionally, to assess the ability of sodium alginate hydrogel MS to control the release of EVs, we placed the PKH26-EVs loaded with MS in PBS solution at 37 °C, after which a certain amount of supernatant was collected and the corresponding fluorescence intensity was measured at different time points. As shown in Fig. 4f, sodium alginate hydrogel MS could release EVs continuously for at least 14 days, which may effectively prolongs the exposure time of neonatal cardiac tissue-derived EVs for the treatment of MI.
a Schematic diagram of the sodium alginate hydrogel MS prepared by microfluidic technology. Created in BioRender. gN, fW. (2025) https://BioRender.com/w82q737b Optical photograph of sodium alginate hydrogel MS. Scale bar = 100 μm. c Particle size analysis of the MS. d Scanning electron microscope (SEM) image of sodium alginate hydrogel MS. Scale bar = 20 μm. e The fluorescence image of EVs encapsulated MS (PKH26, red). Scale bar = 50 μm. f The percentage of EVs cumulative release from MS (n = 3 independent experiments). Error bars represent the mean ± SEM of each group. Source data are provided as a Source Data file.
Delivery of AR-Neo-EVs via MS is more effective in promoting cardiac regeneration and repair
In view of our preliminary results, both Neo-EVs and AR-Neo-EVs could repair infarcted hearts in mice compared to Adu-EVs-treated group. It is worth noticing that AR-Neo-EVs have demonstrated even more significant potential for promoting myocardial regeneration and cardiac repair. Therefore, in the following studies, we mainly focused on exploring therapeutic effects of AR-Neo-EVs encapsulated in sodium alginate hydrogel MS on MI. Firstly, to ascertain the myocardial retention rate of EVs in mice, PKH26-labeled AR-Neo-EVs were encapsulated in sodium alginate hydrogel MS and subsequently injected into the infract border region of MI hearts. Then, the IVIS spectroscopy system was utilized to obtain near-infrared fluorescence images of the hearts at various time points post-injection. On the 1st day, EVs labeled with red fluorescent signals were evenly dispersed in the infarct area, and the amount of red fluorescence in the hearts of both AR-Neo-EVs and AR-Neo-EVs-MS groups decreased with time. On the 14th day, the fluorescence signal was very weak in the AR-Neo-EVs group, while still pronounced in AR-Neo-EVs-MS group, indicating that the engineered MS were capable of continuously and efficiently releasing EVs into the infarcted myocardium (Fig. 5a). To further evaluate therapeutic function of AR-Neo-EVs-MS, we measured cardiac functions of mice in each group by echocardiography 28 days after MS injection. As shown in Fig. 5b, c, AR-Neo-EVs-MS was prominent in improving the cardiac function of mice, as evidenced by higher EF% and FS% than those in the AR-Neo-EVs group. Next, cardiac tissues from each group were collected and stained with Masson’s trichrome and Sirius Red stainings for histologic analysis. The AR-Neo-EVs-MS group showed a markedly decrease the fibrosis area compared with MS and direct AR-Neo-EVs injection groups (Fig. 5d, e and Supplementary Fig. 5a, b). Meanwhile, qRT-PCR experiments also indicated that AR-Neo-EVs-MS was the most significant reduce the fibrosis levels of Col1a1 and Col3a1 (Supplementary Fig. 5c, d). Furthermore, immunofluorescence staining, flow cytometry, and Western blot experiments of heart sections revealed that compared with direct injection of AR-Neo-EVs, AR-Neo-EVs loaded with MS were more effective in promoting cardiomyocyte cell cycle re-entry, inhibiting apoptosis, and increasing angiogenesis (Fig. 5f–o and Supplementary Fig. 5e–p). The above findings suggest that the delivery of AR-Neo-EVs to infarcted myocardium via MS can prolong the residence time of EVs in the heart, thus more fully exerting the role of pro-cardiac regeneration and repair.
a Bioluminescent images of adult mice after injection of AR-Neo-EVs and AR-Neo-EVs-MS. b, c Representative echocardiogram images and quantification of the EF and FS in the Sham, MI, MI + AR-Neo-EVs, MI + MS, and MI + AR-Neo-EVs-MS groups on Day 28 after MI (n = 5 independent mice). ***p < 0.001 vs. Sham, ***p < 0.001 vs. MI, *p < 0.05, ***p < 0.001 vs. MI + AR-Neo-EVs. d, e Masson’s trichrome staining and infract area quantification of heart sections at Day 28 post-MI (n = 5, 4, 5, 3, 4 independent mice). Scale bar = 500 μm. ***p < 0.001 vs. MI, *p < 0.05 vs. MI + AR-Neo-EVs. f–i Representative immunofluorescence images and quantification of the Ki67, pH3, and Aurora B in the border region of adult mice at Day 7 after MI (n = 5 independent mice). Ki67, pH3, and Aurora B marked proliferating cells (red), α-Actinin labeled cardiomyocytes (green), and DAPI labeled nuclei (blue). Scale bar = 20 μm. White arrows point the positive cardiomyocytes. ***p < 0.001 vs. MI, ***p < 0.001 vs. MI + AR-Neo-EVs. j, k Representative images and quantification of the number of mono-, bi-, and multi-nucleated cardiomyocytes in total cardiomyocytes (n = 4 independent mice). Scale bar = 50 μm. ***p < 0.001 vs. MI, **p < 0.01, ***p < 0.001 vs. MI + AR-Neo-EVs. l, m Representative flow cytometry images and quantification of Annexin V-FITC/PI staining was conducted to assess the apoptosis cells in EVs-treated mice hearts on Day 7 post-MI (n = 3 independent mice). ***p < 0.001 vs. Sham, ***p < 0.001 vs. MI, *p < 0.05 vs. MI + AR-Neo-EVs. n, o Representative flow cytometry images and quantification of CD31-FITC-H staining was conducted to CD31+ cells in EVs-treated mice hearts on Day 7 post-MI (n = 3 independent mice). ***p < 0.001 vs. MI. One-way ANOVA followed by Tukey’s Multiple Comparisons test (c, e, g, h, i, m, o). Two-way ANOVA followed by Sidak’s Multiple Comparisons test (k). Error bars represent the mean ± SEM of each group. Source data are provided as a Source Data file. Exact p values are provided in the Source Data file.
The regulatory role of WD Repeat Domain 75 (Wdr75) protein in AR-Neo-EVs mediating cardioprotection
In light of the fact that the abundant proteins in EVs play a key role in mediating intracellular activity and intercellular communication24. To further explore the potential mechanism of neonatal cardiac tissue-derived EVs in repairing infarcted hearts, different proteins of Adu-EVs, Neo-EVs, and AR-Neo-EVs samples were determined using quantitative proteomics. Venn diagram result showed that there were 2291 proteins in Adu-EVs group, 2569 proteins in Neo-EVs group, and 2585 proteins in AR-Neo-EVs group (Fig. 6a). Next, in order to explore the protein differences among the Adu-EVs, Neo-EVs, and AR-Neo-EVs. We analyzed the specific proteins in EVs of different cardiac tissues by gene ontology (GO) analysis. The results showed that the Adu-EVs group mainly enriched in the immune response, the Neo-EVs group participated in the process of blood vessel development, mRNA processing, and RNA splicing, while the AR-Neo-EVs group played an important role in DNA damage and repair (Fig. 6b). Subsequently, we further analyzed the protein data and found that there were 1586 differentially expressed proteins (DEPs) between the Adu-EVs and Neo-EVs groups (p < 0.05, |log2 FC | > 1.3), of which 1263 were up-regulated and 323 were down-regulated, 1652 DEPs between Adu-EVs and AR-Neo-EVs groups, of which 1297 were up-regulated and 355 were down-regulated, 145 DEPs between Neo-EVs and AR-Neo-EVs groups, of which 83 were up-regulated and 62 were down-regulated. This indicates that the protein composition of Adu-EVs and Neo-EVs/AR-Neo-EVs is quite different, but Neo-EVs are similar to AR-Neo-EVs (Fig. 6c). Then we applied the fuzzy c-means algorithm to cluster the protein expression profiles of EVs in different heart tissues25. In general, we observed eight different pattern clusters representing different regulated proteins. Among them, protein cluster 5 showed a gradually increasing trend from Adu-EVs, Neo-EVs to AR-Neo-EVs, which was consistent with the law of myocardial regeneration in mice (Fig. 6d). Then we performed GO analysis on protein cluster 5. The results showed that the gradually up-regulated proteins tended to be involved in ribosome biogenesis, rRNA processing, and RNA binding (Fig. 6e). In addition, eight candidate proteins (p < 0.05, |log2 FC | > 1.3) were further screened by Heat map and Venn for protein cluster 5, including Wdr75, Pdlim7, A2m, Ilvbl, Ppp4c, Mpo, Ngp, and Ubap2l (Fig. 6f, g). According to previous experimental results, Adu-EVs had no significant effect on cell cycle re-entry, apoptosis, and angiogenesis in cardiomyocytes and endothelial cells. Therefore, we selected the proteins not expressed in Adu-EVs as our candidate proteins (Wdr75 and Pdlim7). Then, we induced knockdown in cardiomyocytes by transfecting Wdr75 and Pdlim7 siRNA. The immunofluorescence results showed that si-Wdr75 increased the number of Ki67- and EdU-positive cardiomyocytes, while si-Pdlim7 was not significantly increased (Fig. 6h). These suggest that Wdr75 may be our candidate target protein.
a Venn diagram showing the overlap of proteins of differentially expressed Adu-EVs, Neo-EVs, and AR-Neo-EVs. b Gene ontology (GO) analyses of proteins in Adu-EVs, Neo-EVs, and AR-Neo-EVs. c Volcano plot for a comparison of protein expression profiles between different tissue EVs. The x-axis indicates the differential expression profiles, plotting the log2(Fold Change). The y-axis indicates the statistical significance of differences. d Fuzzy c-means clustering analyses of the protein expression profiles of different cardiac tissue EVs. e GO analyses of proteins in cluster 5. f Heatmap of differentially expressed proteins enriched in cluster 5. g Venn diagram showing the overlap of proteins of differentially expressed in cluster 5. h Quantitative analysis of the Ki67 and EdU proliferation assay in cardiomyocytes (n = 6 independent experiments). ***p < 0.001 vs. si-NC. Two-tailed Student’s t-test was used to compare the differences between the two experimental groups. Error bars represent mean ± SEM. Source data are provided as a Source Data file. Exact p values are provided in the Source Data file.
The important role of Wdr75 protein in AR-Neo-EVs mediated cardiac repair in vitro
To validate the results of proteomics, the expression of Wdr75 protein in the EVs of cardiac tissues from each group was further analyzed using Western blotting. As shown in Fig. 7a, the expression of Wdr75 in AR-Neo-EVs was significantly higher than that in the Neo-EVs group, whereas almost no Wdr75 expression was detected in Adu-EVs, which was consistent with the proteomics results. Subsequently, to ascertain the potential involvement of Wdr75 in the biological function of cardiomyocytes and HUVECs mediated by AR-Neo-EVs, we performed AR surgery in P1 mice, and then shWdr75 adenovirus were delivered into AR mouse model via intramyocardial injection to silence the expression of Wdr75. 3 days after infection, immunoblotting confirmed that shWdr75 adenovirus successfully induced Wdr75 knockdown in cardiac tissues (Supplementary Fig. 6a). AR-Neo-EVs, AR-Neo+shWdr75-EVs, and AR-Neo+shNC-EVs were then co-cultured with NMCMs for 24 h, respectively. Immunofluorescence results indicated that the decrease in Wdr75 expression level eliminated the cardiomyocyte cell cycle entry-promoting effect of AR-Neo-EVs, as evidenced by the suppression of Ki67-, EdU-, and pH3-positive rate in AR-Neo+shWdr75-EVs group (Fig. 7b–e). It was previously reported that deletion of Wdr75 in human U2OS cells enhanced the stability of p53 protein and concomitantly induced the expression of CDK inhibitor p21, ultimately resulting in impaired proliferation26. However, there was no evidence whether Wdr75 could regulate proliferation through the p53-p21 signaling pathway in cardiomyocytes. To understand the underlying mechanisms by which Wdr75 in EVs regulates cardiomyocyte cell cycle re-entry, we examined the protein expression of p53 and p21 in NMCMs of each group. The results in Fig. 7f, g showed that AR-Neo-EVs markedly down-regulated the expression of p53 and p21 protein in cardiomyocytes, but this inhibition was reversed by knocking down Wdr75 in EVs.
a The expression of Wdr75 protein in EVs from different cardiac tissue sources was detected by Western blot. b The effects of AR-Neo-EVs, AR-Neo+shWdr75-EVs, and AR-Neo+shNC-EVs on cardiomyocyte proliferation analyzed by the detection of Ki67, EdU, and pH3. Ki67, EdU, and pH3 marked proliferating cells (red), α-Actinin labeled cardiomyocytes (green), and DAPI labeled nuclei (blue). Scale bar = 20 μm. White arrows point the positive cardiomyocytes. c–e Quantitative analysis of the Ki67, EdU, and pH3 proliferation assay (n = 5 independent experiments). ***p < 0.001 vs. Ctl, ***p < 0.001 vs. AR-Neo-EVs, ***p < 0.001 vs. AR-Neo+shWdr75-EVs. f, g The expression of p53 and p21 protein in cardiomyocytes treated with different EVs (n = 3, 5 independent experiments). *p < 0.05, **p < 0.01 vs. Ctl, **p < 0.01,***p < 0.001 vs. AR-Neo-EVs, *p < 0.05, **p < 0.01 vs. AR-Neo+shWdr75-EVs. h Tube formation experiments of HUVECs treated with different EVs. Scale bar = 150 μm. i–k Quantitative analysis of tube formation experiments (n = 3 independent experiments). **p < 0.01, ***p < 0.001 vs. Ctl, *p < 0.05, ***p < 0.001 vs. AR-Neo-EVs, **p < 0.01 vs. AR-Neo+shWdr75-EVs. l Scratch migration experiments of HUVECs treated with different EVs. Scale bar = 150 μm. m Quantitative analysis of scratch migration experiments (n = 4 independent experiments). *p < 0.05, ***p < 0.001 vs. Ctl, ***p < 0.001 vs. AR-Neo-EVs, *p<0.05,***p < 0.001 vs. AR-Neo+shWdr75-EVs. n The expression and quantitative analysis of p53 protein in HUVECs treated with different EVs by Western blot (n = 5 independent experiments). **p < 0.01 vs. Ctl, **p < 0.01 vs. AR-Neo-EVs, *p < 0.05 vs. AR-Neo+shWdr75-EVs. o The mRNA expression of vascular endothelial growth factor (VEGF) in HUVECs treated with different EVs by qRT-PCR (n = 4 independent experiments). ***p < 0.001 vs. Ctl, ***p < 0.001 vs. AR-Neo-EVs, ***p < 0.001 vs. AR-Neo+shWdr75-EVs. One-way ANOVA followed by Tukey’s Multiple Comparisons test (c, d, e, f, g, i, j, k, n, o). Two-way ANOVA followed by Tukey’s Multiple Comparisons test (m). Error bars represent the mean ± SEM of each group. Source data are provided as a Source Data file. Exact p values are provided in the Source Data file.
It is properly acknowledged that p53 deficiency in endothelial cells can also induce the formation of blood vessels by promoting the expression of vascular endothelial growth factor (VEGF)27,28. Based on this, we further verified the regulatory effect of Wdr75 on p53-mediated angiogenesis in HUVECs. It was found that inhibition of Wdr75 expression eliminated the role of AR-Neo-EVs in promoting migration and angiogenesis of HUVECs (Fig. 7h–m). Further Western blotting and qRT-PCR results showed a notable increase in p53 protein level and a decrease in VEGF mRNA expression in HUVECs treated with AR-Neo+shWdr75-EVs as compared to the AR-Neo-EVs group (Fig. 7n, o). In addition, to further explore the key role of Wdr75 in AR-Neo-EVs-mediated cardiac repair post-injury, we injected Wdr75-deficient AR-Neo-EVs encapsulated with sodium alginate hydrogel MS (AR-Neo+shWdr75-EVs-MS) into the hearts of MI mice. At 28 days after surgery, the results of echocardiography showed that the improvement of cardiac function in MI + AR-Neo+shWdr75-EVs-MS group was lower than that in MI + AR-Neo-EVs-MS group (Supplementary Fig. 7a–c). Then, heart tissues from each group were collected and stained with Masson’s trichrome for histological analysis. The infarct size was significantly increased in the MI + AR-Neo+shWdr75-EVs-MS group compared with the MI + AR-Neo-EVs-MS group (Supplementary Fig. 7d). In addition, immunofluorescence staining of cardiac sections showed that MS-loaded AR-Neo+shWdr75-EVs had a significantly lower role in promoting cardiomyocyte cell cycle re-entry, inhibiting apoptosis, and increasing angiogenesis compared with AR-Neo-EVs-MS group (Supplementary Fig. 7e–j). Collectively, these results suggest that AR-Neo-EVs participate in regulating cell cycle re-entry, apoptosis, and angiogenesis by delivering Wdr75 protein and mediating p53 expression in cardiomyocytes and endothelial cells, which is expected to be a potent resource for repairing adult damaged hearts.
Wdr75 positively regulates cardiomyocyte proliferation and angiogenesis
Next, we further determined whether Wdr75 exerts cardioprotective effects by regulating p53 expression. We effectively co-transfected Wdr75 and p53 plasmids in NMCMs, and found that simultaneous overexpression of p53 obviously blocked the effect of Wdr75 in promoting cardiomyocyte cell cycle re-entry (Fig. 8a–d, and Supplementary Fig. 6b). Consistently, overexpression of p53 in cardiomyocytes reversed the inhibitory effect of Wdr75 on p21 protein expression (Fig. 8e, f). In endothelial cells, angiogenesis and wound healing experiments showed that overexpression of p53 was able to reverse the pro-angiogenic effects of Wdr75 (Fig. 8g–m). Furthermore, we knocked down Wdr75 in cardiomyocytes and HUVECs, respectively (Supplementary Fig. 6c), which showed knockdown of Wdr75 markedly inhibited cell cycle re-entry and angiogenesis in vitro (Supplementary Fig. 8). These results suggest that Wdr75 exerts its diverse functions by affecting the levels of p53 protein in cardiomyocytes and endothelial cells.
a Cardiomyocytes were transfected with empty (NC), Wdr75 plasmid, and co-transfected with Wdr75 and p53 plasmids, and the proliferation of cardiomyocytes was evaluated by immunofluorescence staining with Ki67, EdU, and pH3. α-Actinin labeled cardiomyocytes (green) and DAPI labeled nuclei (blue). Scale bar = 20 μm. White arrows point the positive cardiomyocytes. b–d Quantitative analysis of the Ki67, EdU, and pH3 proliferation assay (n = 4 independent experiments). ***p < 0.001 vs. NC, **p < 0.01 vs. Wdr75-OE. e, f Western blot analysis of p53 and p21 expression after transfected with NC, Wdr75 plasmid, and co-transfected with Wdr75 and p53 plasmids in cardiomyocytes (n = 4 independent experiments). **p < 0.01, ***p < 0.001 vs. NC, **p < 0.01, ***p < 0.001 vs. Wdr75-OE. g Tube formation experiments of HUVECs after transfected with NC, Wdr75 plasmid, and co-transfected with Wdr75 and p53 plasmids. Scale bar = 150 μm. h–j Quantitative analysis of tube formation in HUVECs (n = 4 independent experiments). ***p < 0.001 vs. NC, ***p <0.001 vs. Wdr75-OE. k Scratch migration experiments of HUVECs after transfected with NC, Wdr75 plasmid, and co-transfected with Wdr75 and p53 plasmids. Scale bar = 150 μm. l Quantitative analysis of scratch migration experiments (n = 4 independent experiments). ***p < 0.001 vs. NC, ***p < 0.001 vs. Wdr75-OE. m Western blot analysis of p53 expression after transfected with NC, Wdr75 plasmid, and co-transfected with Wdr75 and p53 plasmids in HUVECs (n = 4 independent experiments). ***p < 0.001 vs. NC, ***p < 0.001 vs. Wdr75-OE. One-way ANOVA followed by Tukey’s Multiple Comparisons test (b, c, d, e, f, h, i, j, m). Two-way ANOVA followed by Tukey’s Multiple Comparisons test (l). Error bars represent mean ± SEM. Source data are provided as a Source Data file. Exact p values are provided in the Source Data file.
Discussion
Cardiovascular diseases, principally MI, are the leading causes of death and disability worldwide29. Exploring new therapeutic strategies to promote cardiac regeneration and microvascular system reconstruction is of great significance for cardiac repair after MI. In the present study, we uncovered that EVs derived from neonatal cardiac tissue, especially AR regenerative cardiac tissue, could exert pro-regenerative and cardioprotective effects against MI injury in adult mice. Mechanistically, we identified Wdr75 protein as a key regulator of cardiac regeneration in AR-Neo-EVs, which activated cardiomyocyte cell cycle re-entry, inhibited cardiomyocyte apoptosis, and promoted neovascularization by down-regulating p53 protein levels in cardiomyocytes and endothelial cells. The finding provides certain insights into therapeutic strategies for cardiac repair after MI, and confers regenerating neonatal cardiac tissue-derived EVs as a effective resource for the treatment of ischemic disease.
EVs enriched with signaling molecules of parental cells can migrate to recipient cells via paracrine or hormone-like mechanisms, mediating a variety of physiological and pathological processes, such as proliferation, apoptosis, and inflammation9,30. A recent study by Fafia´n-Labora et al. showed that EVs isolated from young human donor fibroblasts ameliorated senescence by increasing the antioxidant capacity of old fibroblasts and old mice, demonstrating the potential of EVs as regenerative therapy31. It has been widely accepted that tissues containing diverse cell types are important natural reservoirs of functional EVs, and their originating EVs more accurately reflect in vivo conditions. Although the newborn mammalian hearts have regenerative potential within 7 days after birth, whether the EVs from neonatal hearts and regenerative cardiac tissues possess pro-regenerative abilities remain unknown. Therefore, we hypothesized that EVs from neonatal mammalian myocardial might play a regulatory role in heart repair post-MI. In this study, we extracted EVs from cardiac tissues of neonatal mice and AR regeneration models, and found that Neo-EVs and AR-Neo-EVs can be effectively internalized by cardiomyocytes and endothelial cells, leading to a notable decrease in myocardial infarct size and enhanced cardiac function in adult mice, suggesting the EVs from cardiac tissues with regenerative potential may promote heart repair in adults. It also indicates that the EVs possibly mediates cardiac microenvironment communication during heart regeneration after AR surgery in neonates. Interestingly, Adu-EVs did not have any therapeutic effect on the repair of heart damage in our study, which led us to speculate that due to different EVs protein expression profiles produced in mice at different stages of development.
The mammalian heart is composed of diverse cell types, among which a variety of cells have been reported to be involved in regulating cardiovascular repair under different stimuli. For instance, endothelial cells secrete EVs can suppress senescence and stimulate an angiogenic program in target cells via miR-21432. In addition, EVs derived from Ang II-treated atrial myocytes can inhibit the polarization of M2-like macrophages by transferring miR-23a, thereby promoting myocardial fibrosis33. In order to further explore the major origins of cardiac regenerative EVs identified in our study, we isolated cardiomyocytes, fibroblasts, and endothelial cells, which accounted for the largest proportion of cardiac tissue, from neonatal and AR-neonatal hearts for in vitro cultivation. Subsequently, we extracted EVs from the culture medium of the three types of cells and added them to NMCMs. The results displayed that EVs obtained from the cardiomyocytes of Neo and AR-Neo hearts markedly promoted cardiomyocyte proliferation compared with fibroblasts and endothelial cells (Supplementary Fig. 9a, b). This suggest that neonatal cardiomyocytes may be the main donors of this reparative EVs. Notably, the pro-proliferative capacity of the neonatal heart tissue-derived EVs was the stronger than that of each individual cultured cells, indicating that this cardiac regenerative EVs may be the product of multiple cellular syntheses. Futhermore, in order to explore the reason for the significant increase of Wdr75 in EVs after AR stimulation, cardiomyocytes, endothelial cells, and fibroblasts of Sham and AR neonatal mice were isolated and cultured in vitro. qRT-PCR assay showed that compared with Sham group, the expression level of Wdr75 mRNA in cardiomyocytes of AR group was significantly increased, while the changes in endothelial cells and fibroblasts were not significant (Supplementary Fig. 9c), which indicated that the expression level of Wdr75 in cardiomyocytes was significantly higher than that in other cell types of the heart. Therefore, we speculate that AR mainly stimulates the production of Wdr75 in cardiomyocytes, resulting in an increase in Wdr75 in EVs. However, the underlying mechanism may need to be proved by more experiments in the future.
The presence of abundant proteins in EVs, including membrane proteins, cytoplasmic proteins, nuclear proteins, and extracellular matrix proteins, determines their crucial role in facilitating intercellular communication and signaling transduction24,34,35. To explain why AR-Neo-EVs has higher pro-myocardial repair activity, we analyzed the differential protein expression profiles of EVs in each group, and it was found that EVs from different sources had different protein expression profiles. Among them, the Neo-EVs is mainly RNA splicing, RNA processing, and ribosome biogenesis. In addition, AR-Neo-EVs is dominated by cell cycle, suggesting that cycle regulation is an important mechanism of its action (Supplementary Fig. 10). Wdr75 is a nucleolar protein, which has been reported to suppress p53 expression and regulated pre-rRNA processing within the 90S processome36. A recent study from Pavel et al. found that absence of Wdr75 activated the RPL5/RPL11-dependent p53 stabilization, which in turn induced the expression of p53’s transcriptional target, the CDK inhibitor p21, ultimately leading to impaired proliferation and senescence of U2OS cells26. It is well known that in addition to participating in the regulation of cell proliferation and apoptosis, p53 can also promote the ubiquitination and proteasome degradation of hypoxia inducing factor-1α (HIF-1α), resulting in the reduction of vascular endothelial expression factors, thereby inhibiting angiogenesis27. Therefore, we assumed that Wdr75, which has an inhibitory effect on p53, plays a key role in the therapeutic effects, and the higher activity of AR-Neo-EVs in cardiac repair may be mostly related to the elevated levels of Wdr75 protein in AR-Neo-EVs. To further confirm the effect of Wdr75 in AR-Neo-EVs, we silenced the expression of Wdr75 in myocardium and their EVs of AR-Neo mice by adenovirus, and found that AR-Neo-EVs-mediated cardiomyocyte proliferation, anti-apoptosis, and angiogenesis were markedly hindered. Moreover, the expression of p53 protein in cardiomyocytes and endothelial cells was also obviously up-regulated with the knockdown of Wdr75 in EVs. These data suggest that Wdr75 carried by AR-Neo-EVs can mediate the cardiac regeneration process by inhibiting the p53 axis of cardiomyocytes and endothelial cells.
In recent years, EVs have been recognized as a powerful, cell-free, and promising approach to ameliorate the outcome of cardiovascular disease32. Unfortunately, there are still major obstacles to the therapeutic application of EVs techniques. Particularly, the short half-life and low residency of EVs in the organism result in insufficient therapeutic doses to the injured area17,18,19. Administering EVs in a multi-dose intramuscular manner is highly invasive and time-consuming, which limits the therapeutic effect of EVs in the treatment of MI. Nonetheless, the development of natural biomaterials has provided new perspectives on the treatment of EVs37,38. Uyen et al. found that micrometer-sized alginate MS could not only controlled the drug release rate, but also discharged from the body through metabolic degradation after drug release39. On this basis, we further prepared a biocompatible sodium alginate hydrogel MS by microfluidic technology and loaded AR-Neo-EVs to construct a stable EVs delivery system. The results showed that sodium alginate hydrogel MS were able to prolong the residence time of AR-Neo-EVs in the infarcted myocardium. As expected, compared with direct intramyocardial injection, AR-Neo-EVs loaded with MS significantly reduced the infarct size and improved cardiac function in mice post-MI. In addition, CCK8, MTT, qRT-PCR, and IVIS fluorescence imaging assays showed that MS has a good biocompatibility, biosafety, and biodegradability (Supplementary Fig. 11). All of above confirms the efficacy of AR-Neo-EVs-MS in the treatment of ischemic myocardial injury and reflects the application value of EVs encapsulated with MS.
In summary, our study reveals AR-Neo-EVs are of cardiac regenerative activity, which inhibits the p53 signaling pathway by delivering the Wdr75 protein to the adult heart, thereby activating cardiomyocyte cell cycle re-entry, inhibiting cardiomyocyte apoptosis, and promoting neovascularization. In addition, this pro-regenerative EVs delivered to the infarct heart via sodium alginate hydrogel MS can effectively promote recovery of the heart after MI (Fig. 9). Our findings provide a experimental and theoretical basis for the application of engineered EVs in ischemic heart disease.
EVs was extracted from regenerating neonatal heart tissues by AR surgery, and then the extracted AR-Neo-EVs was mixed with sodium alginate solution to prepare sodium alginate hydrogel MS. The synthetic AR-Neo-EVs-MS was injected into the heart of adult mouse MI to mediate the sustained release of AR-Neo-EVs. Mechanically, after transferring highly expressed Wdr75 in AR-Neo-EVs to recipient cells, highly expressed Wdr75 can inhibit p53-p21 axis, promote cardiomyocyte cell cycle re-entry, reduce cardiomyocyte apoptosis, promote angiogenesis, and play a role in cardiac repair. This Figure was created by figdraw.com.
Methods
Animals
The neonatal mice (1–3 days old) and adult C57BL/6 mice (8–10 weeks old) were purchased from the Experimental Animal Center of The Second Affiliated Hospital of Harbin Medical University (Harbin, China) and were housed in an SPF-grade environment. All animal experiments were approved by the Ethic Committees of College of Pharmacy, Harbin Medical University (SYDW2024-117) and in accordance with the Guide for the Care and Use of Laboratory in Harbin Medical University. Mice were housed in ventilated cages under a temperature (20–24 °C) and humidity (40–60%) with a 12 h light/dark cycle and were fed with commercial formula feed satisfying the standard mice nutritional requirements and water ad libitum. The experimenters were blind to treatment grouping information during the experiment and quantification. No mice were excluded from the study unless died.
AR model
AR surgery was carried out on neonatal mice at postnatal day 1 (P1). In brief, P1 mice were anesthetized by cooling on an ice bed for 4 min. Lateral thoracotomy at the 4th intercostal space was performed by blunt dissection of the intercostal muscles following skin incision. After exposing the left ventricle, the apex of hearts was resected using the micro scissors. Following AR, adenoviruses Adeasy-Wdr75-shRNA (shWdr75) and shNC (HanBio, Shanghai, China) were injected into the myocardium (2 × 109 viral genomes (vg) per animal). Then, their thoracic wall incisions were sutured with 7-0 non absorbable silk suture, and the skin wounds were closed using skin adhesive. The mice in Sham group underwent the same procedure except for AR. The neonates were then placed under a heat lamp and warmed for several minutes until recovery. The hearts were collected 3 days after resection.
MI
Adult C57BL/6 mice were anesthetized with 2% avertin (0.1 ml 10 g−1) intraperitoneally (i.p.). After anesthesia, a left thoracotomy was performed to expose the heart and the coronary artery of LAD was ligated by a 7-0 prolene suture. Ischemia is manifested by localized pallor of the myocardium. In addition, the mice in the Sham group underwent the same procedure except for LAD ligation. 90 μg Neo-EVs, AR-Neo-EVs, and Adu-EVs were dissolved in 40 μL PBS and injected via 31 G needles into the border region of the infarcted hearts at three different locations after MI, respectively. According to our data (1 μg EVs ≈ 1.52*109 particles), the dose of EVs at the in vivo level was approximately 13.68*1010 particles/per mouse. 7 or 28 days after surgery, the adult mice were anesthetized by intraperitoneal injection of a mixture of xylazine (5 mg kg−1) and ketamine (100 mg kg−1) and then euthanized by cervical dislocation, and the hearts were extracted for detection of various indicators. The experimental groups were as follows: (1) Sham, MI (MI + PBS), MI+Neo-EVs, MI + AR-Neo-EVs, and MI+Adu-EVs. (2) Sham, MI (MI + PBS), MI + AR-Neo-EVs, MI + MS, and MI + AR-Neo-EVs-MS. We excluded mice that died of severe ischemia due to MI within 28 days as an exclusion criterion.
Isolation of cardiomyocytes and endothelial cells from adult mice
Adult mouse cardiomyocytes were freshly isolated via Langendorff perfusion with type II collagenase. Initially, the hearts of adult mice were excised and perfused with calcium-free Tyrode solution (mM) containing NaCl 123, KCl 5.4, HEPES 10, NaH2PO4 0.33, MgCl2 1.0, and glucose 10, with pH adjusted to 7.35–7.45 using NaOH, for approximately 5 min at 37 °C in a water bath. Subsequently, the hearts were perfused with Tyrode’s solution containing type II collagenase (1 mg/ml; 9001-12-1, Gibco, Grand Island, NY, USA) and bovine serum albumin (BSA, 0.02 mg/ml; 9048-46-8, Sigma-Aldrich, St. Louis, MO, USA) until the toughness of heart tissues was reduced. Finally, adult mouse cardiomyocytes were collected by centrifugation at 200 g/min and utilized for subsequent experiments.
Adult mouse endothelial cells purchased from Anwei-sci Cell Center (AW-PM142, Shanghai, China)
Cell culture and treatment
Cardiomyocytes were extracted from neonatal mice aged 1 day. Briefly, the heart tissues were completely digested with 0.25% trypsin EDTA solution (MA0232, Meilunbio, Dalian, China), and then purified using a selective adherent technique. Neonatal mouse cardiomyocytes (NMCMs) were plated at the density of 1.2×105 per cm2 on the 1% gelatin-coated plates and cultured in DMEM (12491015, Life Technologies, Carlsbad, MD, USA) with 10% fetal bovine serum (A5256701, Gibco, Grand Island, NY, USA) and 1% penicillin-streptomycin (SC118, Seven, Beijing, China) in a humidified incubator of 5% CO2 at 37 °C for 48 h. The overexpression plasmids of human Wdr75 gene (NM_032168) named pEGFP-N1-Wdr75 (Cat no. HG-HO032168) and Mouse Wdr75 gene (NM_028599) named pEGFP-N1-musWdr75 (Cat no. HG-MO028599) were obtained commercially from HonorGene (Changsha, China), which were transfected into NMCMs using Lipofectamine 2000 (11668019, Invitrogen, Carlsbad, CA, USA). Wdr75 siRNA, Pdlim7 siRNA, and NC siRNA were purchased from GenePharma Co., Ltd. (Shanghai, China), which were transfected using RNAiMAX reagent (13778150, Invitrogen, Carlsbad, CA, USA) according to the manufacturers’ instructions, and the target sequences are listed in Supplementary Table 1.
For the dose of EVs used in the cell experiments, cardiomyocytes or endothelial cells were cultured in complete DMEM medium containing 10% fetal bovine serum until cell fusion reached 80% (1*106 cells). Subsequently, 90 μg Neo-EVs, AR-Neo-EVs, and Adu-EVs were added to cultured cardiomyocytes or endothelial cells, respectively. We calculated by NTA technology that the number of particles in 1 μg EVs was about 1.52*109. Therefore, the dose of EVs at the in vitro level was approximately 1.37*105 particles/cell.
For calculations of cardiomyocytes counts, NMCMs were seeded in 12-well plates and treated with the Neo-EVs, AR-Neo-EVs, and Adu-EVs. Cardiomyocytes counts from 0 h to 24 h were quantified with an automatic cell counter (Counstar, Shanghai, China).
To induce hypoxia injury, NMCMs were cultured in DMEM high glucose medium prepared with 10% fetal bovine serum for 1–2 days. When the cells grow to 80%, the medium is replaced with sugar free and serum-free medium and placed in an hypoxia container (1% O2 + 5% CO2 + 94% N2 mixed gas) for 5 min to inflate. Return the hypoxic container to the 37 °C incubator for 24 h of treatment.
EVs isolation and characterization
The heart tissues from neonatal mice, AR model neonatal mice, and adult mice were divided into pieces in PBS, and ground the tissues to a flocculent state. Then, use gradient centrifugation to extract EVs (3000 g, 20 min; 10000 g, 1 h; 100000 g, 1 h, 10 min). The pelleted EVs were collected and resuspended in PBS. All steps were performed at 4 °C.
Protein concentration of EVs was measured by BCA protein assay kit (P0010, Beyotime, Shanghai, China). EVs markers such as Flotillin 1 (ab133497, Abcam, Cambridge, UK, 1:1000), CD63 (25682-1-AP, Proteintech, Wuhan, China, 1:500), TSG101 (28283-1-AP, Proteintech, Wuhan, China, 1:500) were detected by Western blot analysis. The morphology of EVs was characterized by TEM (HT7800, Hitachi, Japan). The size, particle concentration of EVs were analyzed by NTA (ZetaView, Particle Metrix, Germany).
EVs labeled with PKH26 (MINI26, Merck, Drmstadt, MA, Germany) were prepared for subsequent fluorescence imaging experiments. CMs and HUVECs (ATCC, USA) were incubated with PKH26-labeled EVs for 6 h for the internalization assay.
Immunofluorescence staining
Cells were fixed with 4% paraformaldehyde fixative solution (P1110, Solarbio, Beijing, China) for 15 min at 37 °C and then penetrated with 0.4% Triton X-100 (dissolved in 5 mg mL−1 BSA) for 1 h 30 min at room temperature. The cells were then blocked with goat serum (AR0009, Boster, Wuhan, China) for 30 min at 37 °C and incubated with antibodies to α-Actinin (GTX29465, Gene Tex, San Antonio, USA, 1:400), pH3 (#06–570, Millipore, Billerica, USA, 1:400), Ki67 (ab15580, Abcam, Cambridge, UK, 1:400), Aurora B (ab2254, Abcam, Cambridge, UK, 1:400), CD31 (ab28364, Abcam, Cambridge, UK, 1:400) overnight at 4 °C. The secondary antibodies Alexa Fluor 488 (ab150113, Abcam, Cambridge, UK, 1:400) and Alexa Fluor 594 (ab150080, Abcam, Cambridge, UK, 1:400) were incubated with cells for 1 h at room temperature in the dark. After mounting and nucleic staining with DAPI (C0065, Solarbio, Beijing, China, 1:30) for 15 min at room temperature, images were captured using Live cell Imaging System (FV300, Olympus, Japan) and analyzed with ImageJ software. Specifically, cells co-located by α-Actinin and DAPI were identified as cardiomyocytes, and the total number of cardiomyocytes was calculated using this criterion. Moreover, quantitative data were obtained by measuring co-localization of DAPI with EdU+, Ki67+, or pH3+ in the cardiomyocyte area.
EdU
To detect cell proliferation, cells were incubated with 5-ethyl-2 ‘-deoxyuridine (EdU) for 12 h and then fixed, penetrated, and blocked as described above. Cardiomyocytes were stained with α-Actinin. The dye solution was prepared with EdU Apollo567 in Vitro Kit (C10310-1, Ribobio, Guangzhou, China) according to the instructions, and the cells were incubated in the dark for 30 min at room temperature. The nucleus is labeled with DAPI.
Wheat germ agglutinin (WGA)
To measure cardiomyocytes cross-sectional area (CSA) and nucleation, cell borders were identified via staining at room temperature for 15 min with WGA (W849, Invitrogen, Carlsbad, CA, USA). Cardiomyocytes borders were manually traced. Then, cardiomyocytes surface area was quantified with Image J software.
Flow cytometry analysis
The endothelial cells in the hearts of adult mice were counted using Flow cytometry. Specifically, adult mouse cardiac endothelial cells were mixed with 4% paraformaldehyde and incubated for 30 min at room temperature in the presence of 0.5% Triton X-100. After incubation, cells were rinsed with PBS and then stained with anti-CD31-FITC monoclonal antibody (WM59, BioLegend, San Diego, CA, USA) for 30–60 min at room temperature and protected from light.
Apoptosis was quantitatively assessed using the Annexin V-FITC Apoptosis Detection Kit I (MA0220, Meilunbio, Dalian, China). The adult mouse cardiomyocytes were treated, harvested, and then incubated in Annexin V binding buffer with Annexin V and PI for 15 min and protected from light. All samples were analyzed on a NovoCyteTM II Flow Cytometer (Agilent, Beijing, China), and data were evaluated using the FlowJo software v. 10.8.1.
TUNEL assay
Cardiomyocytes and heart tissues embedded with paraffin and cut into thin sections (4 μm) were fixed and labeled by the In Situ Cell Death Detection Kit (12156792910, Roche, Basel, Switzerland) according to the manufacturer’s instructions to assess apoptosis. After TUNEL staining, the nucleus is labeled with DAPI. The TUNEL-positive cells were captured using Live cell Imaging System (FV300, Olympus, Japan) and analyzed with ImageJ software.
Angiogenesis assay
HUVECs were co-incubated with EVs for 24 h, then plated on growth factor-deprived Matrigel (BD Biosciences, Franklin Lakes, USA) to evaluate angiogenesis. 4 h later, tube formation was examined with a white light microscope (CKX41, Olympus, Japan) and analyzed with Image J software.
Wound healing assay
HUVECs were seeded in 6-well culture plates (Thermo Fisher Scientific, Waltham, MA, USA). After the cells reached more than 90% confluence, the monolayer of HUVECs was scraped with a 200 μL micropipette tip. Then, EVs were added to the well, and the cells were incubated for an additional 24 h. Cell images at 0 h, 12 h, and 24 h were taken using a white light microscope (CKX41, Olympus, Japan). The migration rate (%) of cells was calculated as follows: Migration rate (%) = (A0–An)/A0 × 100%. A0 represents the initial wound area, and An represents the final wound area.
Echocardiography
Cardiac function was evaluated by echocardiography using the Vevo 1100 Ultrasound machine (VisualSonics, Toronto, ON, Canada) 1 day before surgery and 28 days after MI. The mice were anesthetized and placed on the 37 °C platform. The left ventricular internal diameters at end-diastole (LVIDd) and at end-systole (LVIDs) were measured in two-dimensional long axis views, and left ventricular ejection fraction (EF) and fractional shortening (FS) were subsequently calculated to assess cardiac function.
Histology and immunofluorescence analysis
Mouse hearts were fixed with 4% paraformaldehyde solution, dehydrated, and embedded in paraffin. 4 µm thick sections were obtained for staining. Tissues were stained with the Masson kit (G1340, Solarbio, Beijing, China) and Sirius Red kit (G1472, Solarbio, Beijing, China) according to the manufacturer’s instructions. Scar size was measured using the Image Plus software. For immunofluorescence staining, heart tissues were embedded in OCT compound and sectioned at a thickness of 4 µm. Then tissue sections were fixed with acetone at 4 °C, penetrated with 0.5% Triton X-100 for 1 h at room temperature, blocked at room temperature with goat serum (AR0009, Boster, Wuhan, China) for 10 min, and incubated with primary antibody at 4 °C overnight. After washing with PBS, tissues were incubated with secondary antibodies Alexa Fluor 488 (ab150113, Abcam, Cambridge, UK, 1:400) and Alexa Fluor 594 (ab150080, Abcam, Cambridge, UK, 1:400) at room temperature for 1 h in the dark. Subsequently, tissues were stained with DAPI (C0065, Solarbio, Beijing, China, 1:30) at room temperature for 15 min. Images were captured using a Live cell Imaging System (FV300, Olympus, JAPAN) and analyzed with ImageJ software.
Preparation and characterization of MS-EVs
First, 5% sodium alginate solution (S817374, Macklin, Shanghai, China) was mixed with EVs (13.68*1010 particles/per mouse). Then, the water phase pipe and oil phase pipe are connected to the microfluidic pressure pump. The prepared mixed solution was dropped into mineral oil (S110245, Aladdin, Shanghai, China) through a microfluidic pressure pump and solidified with 20% calcium chloride (10301301, XiLong Scientific, Shenzhen, China). The size of MS was observed under light microscope (CKX41, Olympus, Japan), and the flow rates of aqueous and oil solutions were adjusted accordingly until the diameter of MS reached 50 μm. Finally, the mixture of oil and MS was centrifuged at 200 g for 5 min. Carefully suck the upper mineral oil and add an appropriate amount of PBS (VMS: VPBS = 2: 1) to suspend the MS. The morphology of MS was observed using a white light microscope (CKX41, Olympus, Japan) and SEM (SU-8010, Hitachi, Japan). In addition, soak EVs containing MS in PBS solution and place them in a 37 °C incubator. 100 μL of supernatant was collected and resupplemented with 100 μL of PBS every day until day 18, and the fluorescence intensity of PKH26 in the supernatant was measured by Infinite® 200 PRO Enzyme Labeling Instrument (TECAN, Switzerland) to quantitatively analyze the release of EVs.
Bioluminescence imaging
EVs were prestained with the liposomal dye PKH26 according to manufacturer’s instructions. Inntramyocardial injection of PKH26-labeled EVs were performed as indicated in the study. The hearts were excised and rinsed in PBS 24 h later. Bioluminescence imaging was performed using IVIS imaging system (Xenogen IVIS 50, USA).
Proteomics
EVs were isolated as described above, and heart tissue-derived EVs were collected for proteomic analysis. EVs were analyzed their expression patterns in different cardiac tissues by Enzekangtai (Beijing, China). Differentially expressed proteins were identified by a p < 0.05 and |log2 FC | > 1.3 as filters.
CCK-8
CCK-8 (C0041, Beyotime, Shanghai, China) method was used to detect the effect of MS on cell proliferation. Briefly, after co-culture of NMCMs with MS for 24 h, CCK-8 solution was added to the medium and then incubated in 5% CO2 at 37 °C for 2 h. The absorbance of supernatant was measured at 450 nm.
MTT
MTT (C0009S, Beyotime, Shanghai, China) method was used to detect the effect of MS on cell proliferation. Briefly, after co-culture of NMCMs with MS for 24 h, MTT solution was added to the medium and then incubated in 5% CO2 at 37 °C for 2 h. The absorbance of supernatant was measured at 490 nm.
RNA extraction and Real-time quantitative PCR (qRT-PCR)
Total RNAs were extracted from cells using TRIzol reagent (15596-026, Invitrogen, Carlsbad, CA, USA) according to the manufacturer’s guidelines and the concentration was determined with Nanodrop 8000 (Thermo, USA). SYBR Green PCR Master Mix (Applied Biosystems, Foster City, CA) was used to amplify and determine cDNA from High Capacity cDNA Reverse Transcription Kit (FSQ-101, Toyobo, Shanghai, China) according to the manufacturer’s instructions. The target sequences are listed in Supplementary Table 2.
Western Blot
Proteins were extracted from cells or tissues using lysis. Protein concentration was measured using the Enhanced BCA Protein Assay Kit (P0010, Beyotime, Shanghai, China). The samples were resolved by SDS-PAGE and the target antigens were detected using following antibodies Flotillin 1 (ab133497, Abcam, Cambridge, UK, 1:1000), CD63 (25682-1-AP, Proteintech, Wuhan, China, 1:500), TSG101 (28283-1-AP, Proteintech, Wuhan, China, 1:500), Wdr75 (PA5-70946, Thermo Fisher, Waltham, MA, USA, 1:1000), p53 (#9282, Cell Signaling Techonology, Danvers, MA, USA, 1:1000), p21 (10355-1-AP, Proteintech, Wuhan, China, 1:1000), and GAPDH (AB0037, Abways, Shanghai, China, 1:1000). The images were captured using Odyssey system (LI-COR Biosciences, Lincoln, USA).
Statistics analysis
All statistical analyses were conducted using Prism 8.2.1 (GraphPad Software, Boston, MA, USA). Graphed data are represented as mean ± SEM. Two-tailed Student’s t-test was used to compare the differences between two groups. One-way ANOVA and post hoc Tukey or Dunnet tests were used to compare differences among more than two groups. Data with more than one variable were evaluated by Two-way ANOVA, with Sidak post-tests. Significant differences were considered when p < 0.05.
Statistics and reproducibility
Each experiment was repeated 3 times or more independently with similar results.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
References
Yellon, D. M. & Hausenloy, D. J. Myocardial Reperfusion Injury. N. Engl. J. Med. 357, 1121–1135 (2007).
Wu, X., Reboll, M. R., Korf-Klingebiel, M. & Wollert, K. C. Angiogenesis after acute myocardial infarction. Cardiovasc. Res. 117, 1257–1273 (2021).
Heusch, G. Cardioprotection: chances and challenges of its translation to the clinic. Lancet 381, 166–175 (2013).
Shen, D., Cheng, K. & Marbán, E. Dose‐dependent functional benefit of human cardiosphere transplantation in mice with acute myocardial infarction. J. Cell. Mol. Med. 16, 2112–2116 (2012).
Fan, Q. et al. Depletion of Endothelial Prolyl Hydroxylase Domain Protein 2 and 3 Promotes Cardiomyocyte Proliferation and Prevents Ventricular Failure Induced by Myocardial Infarction. Circulation 140, 440–442 (2019).
Braga, L., Ali, H., Secco, I. & Giacca, M. Non-coding RNA therapeutics for cardiac regeneration. Cardiovasc. Res. 117, 674–693 (2021).
Singh, A. P. et al. Inhibition of GSK-3 to induce cardiomyocyte proliferation: a recipe for in situ cardiac regeneration. Cardiovasc. Res. 115, 20–30 (2019).
Li, J. et al. Regulatory T-cells regulate neonatal heart regeneration by potentiating cardiomyocyte proliferation in a paracrine manner. Theranostics 9, 4324–4341 (2019).
Théry, C., Zitvogel, L. & Amigorena, S. Exosomes: composition, biogenesis and function. Nat. Rev. Immunol. 2, 569–579 (2002).
Iero, M. et al. Tumour-released exosomes and their implications in cancer immunity. Cell Death Differ. 15, 80–88 (2007).
Ratajczak, J., Wysoczynski, M., Hayek, F., Janowska-Wieczorek, A. & Ratajczak, M. Z. Membrane-derived microvesicles: important and underappreciated mediators of cell-to-cell communication. Leukemia 20, 1487–1495 (2006).
Valadi, H. et al. Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat. Cell Biol. 9, 654–659 (2007).
Février, B. & Raposo, G. Exosomes: endosomal-derived vesicles shipping extracellular messages. Curr. Opin. Cell Biol. 16, 415–421 (2004).
Bheri, S., Kassouf, B. P., Park, H.-J., Hoffman, J. R. & Davis, M. E. Engineering Cardiac Small Extracellular Vesicle-Derived Vehicles with Thin-Film Hydration for Customized microRNA Loading. J. Cardiovasc. Develop. Dis. 8, https://doi.org/10.3390/jcdd8110135 (2021).
Zhang, Q. et al. Signaling pathways and targeted therapy for myocardial infarction. Sig. Transduc. Targeted Ther. 7, https://doi.org/10.1038/s41392-022-00925-z (2022).
Gallet, R. et al. Exosomes secreted by cardiosphere-derived cells reduce scarring, attenuate adverse remodelling, and improve function in acute and chronic porcine myocardial infarction. Eur. Heart J. https://doi.org/10.1093/eurheartj/ehw240 (2016).
MacArthur, J. W. et al. Sustained Release of Engineered Stromal Cell–Derived Factor 1-α From Injectable Hydrogels Effectively Recruits Endothelial Progenitor Cells and Preserves Ventricular Function After Myocardial Infarction. Circulation 128, https://doi.org/10.1161/circulationaha.112.000343 (2013).
Lai, C. P. et al. Dynamic Biodistribution of Extracellular Vesicles in Vivo Using a Multimodal Imaging Reporter. ACS Nano 8, 483–494 (2014).
Wiklander, O. P. B. et al. Extracellular vesicle in vivo biodistribution is determined by cell source, route of administration and targeting. J. Extracellular Vesicles 4, https://doi.org/10.3402/jev.v4.26316 (2015).
Li, X. et al. Fabrication of polymeric microspheres for biomedical applications. Mater. Horizons. https://doi.org/10.1039/d3mh01641b (2024).
Wan, J. et al. Injectable photocrosslinking spherical hydrogel-encapsulated targeting peptide-modified engineered exosomes for osteoarthritis therapy. J. Nanobiotechnol. 21, https://doi.org/10.1186/s12951-023-02050-7 (2023).
Wang, X. et al. Injectable Extracellular Matrix Microparticles Promote Heart Regeneration in Mice with Post‐ischemic Heart Injury. Adv. Healthcare Mater. 11, https://doi.org/10.1002/adhm.202102265 (2022).
Yu, B. et al. Extracellular vesicles engineering by silicates-activated endothelial progenitor cells for myocardial infarction treatment in male mice. Nat. Commun. 14, https://doi.org/10.1038/s41467-023-37832-y (2023).
Pathan, M. et al. Vesiclepedia 2019: a compendium of RNA, proteins, lipids and metabolites in extracellular vesicles. Nucleic Acids Res. 47, D516–D519 (2019).
Futschik, M. E. & Carlisle, B. Noise-Robust Soft Clustering of Gene Expression Time-Course Data. J. Bioinforma. Comput. Biol. 03, 965–988 (2011).
Moudry, P., Chroma, K., Bursac, S., Volarevic, S. & Bartek, J. RNA-interference screen for p53 regulators unveils a role of WDR75 in ribosome biogenesis. Cell Death Differ. 29, 687–696 (2021).
Sano, M. et al. p53-induced inhibition of Hif-1 causes cardiac dysfunction during pressure overload. Nature 446, 444–448 (2007).
Gogiraju, R. et al. Endothelial p53 Deletion Improves Angiogenesis and Prevents Cardiac Fibrosis and Heart Failure Induced by Pressure Overload in Mice. J. Am. Heart Assoc. 4, https://doi.org/10.1161/jaha.115.001770 (2015).
Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392, 1736-1788, https://doi.org/10.1016/s0140-6736(18)32203-7 (2018).
Seong, Y.-J. et al. Hyaluronic Acid-Based Hybrid Hydrogel Microspheres with Enhanced Structural Stability and High Injectability. ACS Omega 4, 13834–13844 (2019).
Fafián-Labora, J. A., Rodríguez-Navarro, J. A. & O’Loghlen, A. Small Extracellular Vesicles Have GST Activity and Ameliorate Senescence-Related Tissue Damage. Cell Metab. 32, 71–86.e75 (2020).
van Balkom, B. W. M. et al. Endothelial cells require miR-214 to secrete exosomes that suppress senescence and induce angiogenesis in human and mouse endothelial cells. Blood 121, 3997–4006 (2013).
Li, J., Zhang, Q. & Jiao, H. LncRNA NRON promotes M2 macrophage polarization and alleviates atrial fibrosis through suppressing exosomal miR-23a derived from atrial myocytes. J. Formos. Med. Assoc. 120, 1512–1519 (2021).
Wang, J. et al. Extracellular vesicles mediate the communication of adipose tissue with brain and promote cognitive impairment associated with insulin resistance. Cell Metab. 34, 1264–1279.e1268 (2022).
Caller, T. et al. Small Extracellular Vesicles From Infarcted and Failing Heart Accelerate Tumor Growth. Circulation. https://doi.org/10.1161/circulationaha.123.066911 (2024).
Tafforeau, L. et al. The Complexity of Human Ribosome Biogenesis Revealed by Systematic Nucleolar Screening of Pre-rRNA Processing Factors. Mol. Cell 51, 539–551 (2013).
Cheng, K. et al. Intramyocardial Injection of Platelet Gel Promotes Endogenous Repair and Augments Cardiac Function in Rats With Myocardial Infarction. J. Am. Coll. Cardiol. 59, 256–264 (2012).
Cheng, K. et al. Transplantation of platelet gel spiked with cardiosphere-derived cells boosts structural and functional benefits relative to gel transplantation alone in rats with myocardial infarction. Biomaterials 33, 2872–2879 (2012).
Uyen, N. T. T., Hamid, Z. A. A., Tram, N. X. T. & Ahmad, N. Fabrication of alginate microspheres for drug delivery: A review. Int. J. Biol. Macromolecules 153, 1035–1046 (2020).
Acknowledgements
This work was supported by the National Natural Science Foundation of China (92168119 and 92468301 to B.C., 82272387 to Y.L., 82300302 to YN.L., 82100300 and 82470266 to W.M., 82304480 to X.W.), the HMU Marshal Initiative Funding (HMUMIF-21018 to B.C.), Natural Science Foundation of Heilongjiang Province of China (ZL2024H017 to B.C. and HPL2024H083 to W.M.), the National Excellent Youth Science Fund Project of the National Natural Science Foundation of China (52322502 to T.L.), the National Natural Science Foundation of China (52175009 to T.L.).
Author information
Authors and Affiliations
Contributions
B.C. conceived the study concept. H.L., YQ.L., S.L., C.L., A.C., W.L., W.Z., X.G., Z.R., H.J. and Y.Y. performed the experimental studies. H.L., YN.L. and YQ.L. carried out the data analysis. B.C., H.L., YN.L., Y.L., D.Z. and N.W. wrote the manuscript. B.C., Y.L., W.M., YN.L. X.W., and T.L. provided the funding. All authors reviewed the manuscript. H.L., YN.L. and YQ.L. contributed equally to this work.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Communications thanks the anonymous reviewers for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Li, H., Liu, Y., Lin, Y. et al. Cardiac repair using regenerating neonatal heart tissue-derived extracellular vesicles. Nat Commun 16, 1292 (2025). https://doi.org/10.1038/s41467-025-56384-x
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41467-025-56384-x
This article is cited by
-
Tissue-derived extracellular vesicles: comparing Ts-EVs and Te-EVs in extraction, characteristics and research trends
Cancer Cell International (2026)
-
Platelet-bioengineered hiPSC-sEVs achieve targeted repair of fibrotic sinoatrial node in preclinical SND models
Nature Communications (2025)
-
The PIWI-interacting RNA CRAPIR alleviates myocardial ischemia‒reperfusion injury by reducing p53-mediated apoptosis via binding to SRSF1
Acta Pharmacologica Sinica (2025)
-
Biomedical applications of extracellular vesicles (EVs): even better with cryogels
Microchimica Acta (2025)
-
Extracellular Vesicles in Cardiovascular Diseases: Signaling, Biomarker, and Therapy
Journal of Cardiovascular Translational Research (2025)