Abstract
Oligoasthenozoospermia (OAS) is a common cause of male infertility, and Guilu Erxian Glue (GLEXG) is a traditional Chinese medicine known to improve male reproductive function. The role of GLEXG in OAS and its mechanism of action are not well understood. After the OAS model was established with Tripterygium wilfordii polyglycoside (GTW)-induced mice, the mice were orally administered GLEXG. The effects of GLEXG on testis and epididymis of GTW-induced mice were evaluated by HE, TEM, and Johnson scores. Meanwhile, the effects of GLEXG on semen quality of GTW-induced mice were explored by CTC staining and sperm viability assay, etc. Additionally, an H2O2-treated mouse spermatogonial (GC-2) cell model was established and incubated with GLEXG-containing serum. The mechanism of action of GLEXG was investigated by immunofluorescence, methylation-specific PCR (MSP), and western blot. The OAS mouse model was successfully constructed, and the testes, epididymis, and semen quality of mice were improved after GLEXG treatment. In vivo, GLEXG could promote the expression of TDRP, cAMP, and PKA, and the methylation levels of TDRP genes. Mechanistically, GLEXG could improve sperm viability in H2O2-treated GC-2 cells by promoting the methylation level of TDRP and TDRP genes, and also improve the rate of competent spermatozoa in H2O2-treated GC-2 cells by promoting cAMP/PKA. Our study demonstrates that GLEXG can improve sperm quality in GTW-induced mice and H2O2-treated GC-2 cells by promoting TDRP methylation and modulating the cAMP/PKA pathway. We elucidated the regulatory mechanisms of GLEXG in OAS, providing new potential targets for the treatment of OAS.
Similar content being viewed by others
Introduction
Infertility is prevalent among couples of childbearing age, which affects an individual’s physical health and generates significant psychological stress, hindering the establishment of a harmonious family atmosphere. Among the causes of infertility, male infertility accounts for approximately 50% and exhibits diverse and complex etiologies. Oligasthenospermia (OAS) prevails as the predominant cause, comprising 60–75% of male infertility cases1,2. Oligospermia and asthenospermia often coexist, as defined by the World Health Organization. Oligospermia is characterized by a sperm concentration < 15 × 106/mL, while asthenospermia is defined by reduced motility (< 32% progressive motility or < 40% total motility). OAS is diagnosed when both sperm density and forward progression fall below normal levels3,4. The treatment of OAS can be divided into non-pharmacological interventions such as surgical treatment, physical therapy, acupuncture or massage, and medication-based therapies primarily using Western medicine, including hormone therapy, antioxidant agents, and antimicrobial drugs5,6. Both of these treatment methods have certain limitations. The efficacy of non-pharmacological interventions like acupuncture is currently unclear, and they require patients to invest a significant amount of time and effort. Surgical treatment also involves a recovery period and carries certain surgical risks7,8. Additionally, the cost of non-pharmacological interventions may be higher. On the other hand, medication-based therapy has limited effectiveness and may reach a treatment bottleneck, with numerous adverse reactions such as gastrointestinal discomfort, cardiac arrhythmias, and neurological disorders, making them difficult for patients to tolerate9.
Based on the given background, males experiencing infertility are seeking other therapeutic approaches that offer greater efficacy, improved safety, and optimized time. Guilu Erxian Glue (GLEXG) is a traditional Chinese medicine formula employed in the management of male reproductive dysfunction. It is predominantly formulated using components such as turtle shells (Testudinis Carapacis et Plastri Colla), deer antlers (Cervi Cornus Colla), ginseng (Panax ginseng C.A. Mey), and goji berries (Lycium barbarum L)10,11. There is limited research on applying GLEXG of OAS, and its underlying mechanisms have not been extensively explored.
The etiology of OAS is complex and can be caused by various factors, including genetics, epigenetic mechanisms, as well as environmental and lifestyle factors12,13. DNA methylation is one form of epigenetic modification that can affect gene expression without altering the underlying genetic sequence, occurring at CpG islands in the pyrimidine bases14. Several studies have demonstrated a correlation between male fertility, abnormal semen abnormalities, and aberrant DNA methylation15,16,17,18,19. Additionally, the research in OAS has led to the identification of five genes (LRGUK, DZIP1, DNAAF5, SRPK1, and TDRP) that are significantly associated with sperm function and methylation15,16,17,18,19. Among these genes, TDRP, a testis development-related protein, is closely associated with sperm vitality, and the absence of TDRP significantly reduces sperm vitality20. TDRP has two transcript isoforms, TDRP1 and TDRP2, with the encoded proteins localized in the cytoplasm and the nucleus, influencing spermatogenesis at upstream or internal levels20,21. In comparison to the normal control group, asthenospermic sperm often exhibit downregulation of TDRP methylation19,22. Therefore, we hypothesized that increasing the methylation level of TDRP may improve sperm function in OAS mice.
The cAMP/PKA signaling pathway plays a significant role in the regulation of sperm vitality and is regarded as one of the key signaling pathways involved in this process23,24. Cyclic adenosine monophosphate (cAMP) functions as a secondary messenger in the process of sperm capacitation, playing a crucial role in signal transduction, it is derived from adenosine triphosphate (ATP)25,26. The activity of PKA, a serine/threonine kinase consisting of two regulatory (R) and two catalytic (C) subunits, is controlled by cAMP25,26. Research has shown that cAMP and PKA are involved in initiating sperm motion and activating metabolism during sperm passage through the epididymis27. Alkaline dilution may affect the activity of the sAC/cAMP/PKA pathway, thus altering sperm vitality in goats28. Therefore, we speculate that improving sperm function in OAS mice may be achieved through the cAMP/PKA signaling pathway.
Based on the above background, this study selected GLEXG as a therapeutic drug to investigate its efficacy in OAS mice and elucidate its potential mechanisms of action. The findings may offer support for the utilization of GLEXG in the treatment of OAS.
Results
GLEXG treatment effectively improved testicular damage of GTW-induced OAS mice
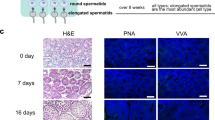
To examine the effects of GLEXG treatment on testicular tissue, an OAS mouse model was established. As shown in Fig. 1, the body weight, testis, and epididymis organ ratios of the Model group were notably lower than those in the Sham group, indicating the successful construction of the OAS mouse model. In comparison to the Model group, both the GLEXG and VE groups exhibited a significant increase in body weight, testis, and epididymal organ ratio. Furthermore, the upward trend in the GLEXG group was more significant than in the VE group (Fig. 1A). Testicular and epididymal tissue damage was assessed by HE staining. The seminiferous tubules in the Sham group had normal structure and orderly arrangement, with abundant germ cells and normal spermatogenic cell morphology. In contrast, the Model group showed disorganized arrangement, narrowed tubular lumen, epithelial degeneration, vacuoles, and reduced mature spermatozoa. There was a significant increase in abnormal sperm cells, nearly absent spermatogenic cells, disordered arrangement, and extensive infiltration of inflammatory cells, confirming the successful OAS model establishment. The GLEXG and VE group displayed a noticeably reduced severity and extent of damage compared to the Model group, along with a significant enlargement of the tubular lumen in the seminiferous tubules, a substantial increase in the number of sperm cells in the lumen, partial recovery seen in some seminiferous tubules, although not reaching the level of the Sham group. However, the therapeutic effect of GLEXG on convoluted seminiferous tubules and spermatogenic cells is superior to that of VE (Fig. 1B).
GLEXG treatment effectively improved testicular damage of GTW-induced OAS mice. A Body weight, testis, and epididymis organ ratio of mice (weight of the left and right testis or epididymis/body weight). B HE staining to detect damage to testicular and epididymal tissue (magnification: ×100, scale bar = 100 μm; magnification: ×400, scale bar = 25 μm). C Ultrastructural changes in testicular and epididymal tissues were observed using TEM. In the TEM images of testicular tissue, NU represents nuclei, red arrows represent mitochondria, yellow arrows represent spermatozoa, purple arrows represent Golgi apparatus, blue arrows represent endoplasmic reticulum, and green arrows represent structural damage to the cell membrane. In the TEM images of epididymal tissue, NU represents nuclei, yellow arrows represent normal mitochondria, red arrows represent damaged mitochondria, green arrows represent nucleoli, and purple represents chromatin. (magnification: ×5000, scale bar = 2 μm; magnification: ×20000, scale bar = 500 nm). D The Johnson score assesses the histological impact on testicular tissue. *P < 0.05 vs. Sham; #P < 0.05 vs. Model; n = 6. The data are presented as mean ± SD.
Figure 1C shows that the tubules in the Sham group exhibited intact structures with clear boundaries. The germ cells displayed normal morphology and orderly arrangement, with abundant mitochondria in the cytoplasm. In the Model group, the seminiferous epithelial cells exhibited disruption, vacuolization, and degeneration. Within the germ cells, an increase in organelle numbers was noted, with some cells lacking nuclei or exhibiting nuclear condensation. Furthermore, there was a notable reduction in the number of mitochondria, which was significantly lower when compared to the Sham group. After GLEXG treatment, the morphology of germ cells was relatively intact, and arranged in an orderly manner, with a significant increase in mitochondria and lysosomes, and some degenerated organelles and sperm could be observed. The VE group demonstrated a noticeable improvement in the disruption of seminiferous epithelial cells compared to the Model group, but did not recover to the level of the GLEXG group.
Additionally, the Johnson score was used to quantify the severity of testicular damage in each group. The results showed that the Model group had the most severe damage, with a Johnson score between 4 and 5, indicating the presence of only a small amount of spermatogonia. After treatment with GLEXG and VE, the extent of damage was reduced, with the Johnson score for the GLEXG group ranging from 7 to 8, suggesting the possible presence of few spermatozoa, while the Johnson score for the VE group was lower than that of the GLEXG group, ranging from 6 to 7, indicating the absence of spermatozoa and only a few spermatids (Fig. 1D). GLEXG therapy effectively improves the degree of testicular damage, and its treatment effect is superior to VE.
GLEXG treatment effectively improves the semen quality in GTW-induced OAS mice
Next, further analysis was performed on the changes in mouse semen quality after GLEXG treatment. Compared with the Sham group, the Model group showed significantly decreased sperm motility, mitochondrial membrane potential, and sperm capacitation rate. After treatment with GLEXG and VE, these indicators showed a significant increase, but the upward trend in the GLEXG group was more significant than that in the VE group, suggesting that GLEXG could improve the viability of spermatozoa in mice (Fig. 2A–C). Further results of the sperm Ca2+ and ATP concentration showed that the sperm Ca2+ and ATP concentration in the Model group was significantly lower compared to the Sham group. After GLEXG and VE treatments, both the Ca2+ and ATP concentrations significantly increased. The upward trend in the GLEXG group was more significant than that in the VE group (Fig. 2D–E). Based on these results, it could be concluded that GLEXG treatment effectively improves the semen quality of GTW-induced OAS mice in the epididymis.
GLEXG treatment effectively improves the semen quality in GTW-induced OAS mice. A Assessment of sperm motility. B Flow cytometry analysis of sperm mitochondrial membrane potential. C CTC staining for assessing sperm fertilization efficiency. F = Non-motile sperm; B = Motile sperm; AR = Acrosome-reacted sperm (magnification: ×400, scale bar = 25 μm). Sperm fertilization efficiency = (B + AR)/ (F + B + AR). D Flow cytometry measurement of sperm Ca2+ concentration. E Biochemical assay of intracellular ATP levels. *P < 0.05 vs. Sham; #P < 0.05 vs. Model; n = 6. The data are presented as mean ± SD.
Alterations in TDRP methylation and cAMP/PKA signaling pathway following GLEXG treatment
Next, we investigated the potential mechanism of GLEXG treatment in OAS mice and found that the expression of TDRP and the methylation levels of its gene were decreased in the testicular tissues of the Model group. After GLEXG and VE treatments, the expression of TDRP and the methylation levels of the TDRP gene increased, with the trend being more significant in the GLEXG group (Fig. 3A-C). Additionally, the expression of cAMP, p-PKA, and PKA in the testicular tissues of the Model group was significantly decreased. Following GLEXG and VE treatments, the expression levels of cAMP and PKA significantly increased, with the upward trend being more significant in the GLEXG group, indicating that GLEXG treatment can lead to changes in the cAMP/PKA pathway (Fig. 3D).
Alterations in TDRP methylation and cAMP/PKA signaling pathway following GLEXG treatment. A Immunofluorescence staining to assess TDRP expression in testicular tissue (magnification: ×400, scale bar = 25 μm). B qRT-PCR to measure the changes in TDRP levels in testicular tissue. C Methylation of TDRP gene in testicular tissue examined by MSP. D Detection of cAMP, p-PKA, and PKA levels. *P < 0.05 vs. Sham; #P < 0.05 vs. Model; n = 6. The data are presented as mean ± SD.
GLEXG enhances the vitality of H2O2-treated GC-2 cells by promoting the expression of TDRP
To further investigate the mechanism of action of GLEXG, TDRP knockdown plasmids were transfected into GC-2 cells. Reduced TDRP expression in GC-2 cells indicated successful transfection (Fig. 4A). In the H2O2-treated group, the expression of TDRP, cAMP, and PKA decreased, but their expression increased after GLEXG treatment. Compared to the H2O2-treated + GLEXG + si-NC group, the GLEXG + si-TDRP group showed reduced TDRP expression with no significant changes in cAMP and PKA expression (Fig. 4B, C). These suggested that GLEXG promotes the expression of TDRP and cAMP/PKA pathway-related factors in GC-2 cells, and knocking down TDRP does not affect the cAMP/PKA pathway. Further results showed that cell viability and migration were reduced in the si-TDRP group and the H2O2-treated group compared to the Control group, with a more significant decrease in the former. Cell viability and migration of H2O2-treated GC-2 cells increased after GLEXG treatment but decreased after knocking down TDRP, weakening the promoting effect of GLEXG (Fig. 4D, E). Subsequent results revealed that mitochondrial membrane potential and ATP levels were significantly decreased in the si-TDRP group and the H2O2-treated group compared to the Control group, with a more pronounced decrease in the former. After GLEXG treatment, the mitochondrial membrane potential and ATP levels of H2O2-treated GC-2 cells increased, whereas knocking down TDRP resulted in a decrease in mitochondrial membrane potential, weakening the promoting effect of GLEXG (Fig. 4F–H). It was speculated that GLEXG enhances the vitality of mouse spermatogonial cells H2O2-treated GC-2 by promoting TDRP expression.
GLEXG enhances the vitality of H2O2-treated GC-2 cells by promoting the expression of TDRP. A, B Detection of TDRP levels using qRT-PCR and WB. C Detection of cAMP and PKA expression. D Assessment of cell viability using the CCK-8 assay. E Measurement of cell migration using the Transwell assay (magnification: ×100, scale bar = 100 μm). F, G Flow cytometry analysis of mitochondrial membrane potential. H Biochemical measurement of intracellular ATP levels. *P < 0.05 vs. Control; #P < 0.05 vs. H2O2-treated; &P < 0.05 vs. H2O2-treated + GLEXG + si-NC; n = 3. The data are presented as mean ± SD.
GLEXG enhances the vitality of H2O2-treated GC-2 cells by promoting the methylation of TDRP
To further explore whether GLEXG exerts its effects by regulating the methylation of the TDRP gene. The results showed that in GC-2 cells, levels of TDRP, TDRP gene methylation, cAMP, and PKA decreased after H2O2 treatment, but increased with GLEXG treatment. Decitabine could decrease TDRP levels and gene methylation, weakening the effect of GLEXG. The cAMP and PKA expression remain unchanged after Decitabine treatment (Fig. 5A–C). These results indicated that GLEXG promotes the upregulation of TDRP and its gene methylation levels. Further results showed that compared to the H2O2-treated group, cell viability and the number of migrated cells increased in the GLEXG group. When Decitabine inhibited the methylation level of the TDRP gene, cell viability and the number of migrated cells decreased, weakening the promoting effect of GLEXG (Fig. 5D, E). In addition, the mitochondrial membrane potential and intracellular ATP levels significantly increased in H2O2-treated GC-2 cells after GLEXG treatment. Decitabine treatment weakened the promoting effect of GLEXG (Fig. 5F, G). In conclusion, GLEXG promotes TDRP methylation levels, thereby enhancing the vitality of H2O2-treated GC-2 cells.
GLEXG enhances the vitality of H2O2-treated GC-2 cells by promoting the methylation of TDRP. A qRT-PCR analysis of TDRP levels. B Detection of cAMP and PKA expression. C Methylation of TDRP gene in testicular tissue examined by MSP. D Assessment of cell viability using the CCK-8 assay. E Measurement of cell migration using the Transwell assay (magnification: ×100, scale bar = 100 μm). F Flow cytometry analysis of mitochondrial membrane potential. G Biochemical measurement of intracellular ATP levels. *P < 0.05 vs. Control; #P < 0.05 vs. H2O2-treated; &P < 0.05 vs. H2O2-treated + GLEXG; n = 3. The data are presented as mean ± SD.
GLEXG promotes cAMP/PKA expression in H2O2-treated GC-2 cells to improve sperm capacitation rates
Figure 3D showed elevated cAMP, p-PKA, and PKA expression in testicular tissues of OAS mice after GLEXG treatment. Therefore, we further explored here whether GLEXG treatment acts through cAMP/PKA. Figure 6A showed that H2O2-treated GC-2 cell viability was elevated after GLEXG treatment, whereas H2O2-treated GC-2 cell viability was reduced after treatment with the cAMP inhibitor SQ22536S, and the effect of GLEXG on cell viability was diminished. Next, the expression of cAMP, p-PKA, and PKA was examined. Compared to the Control group, the levels of p-PKA, PKA, and cAMP in the H2O2-treated group are significantly decreased. The levels of p-PKA, PKA, and cAMP in the GLEXG group are higher than those in the H2O2-treated group but decrease after treatment with the cAMP inhibitor SQ22536S, weakening the promoting effect of GLEXG, suggesting that GLEXG promotes the expression of cAMP, p-PKA, and PKA (Fig. 6B). The TDRP level decreased in the H2O2-treated group and increased in the GLEXG group. No significant change in the TDRP level is observed after SQ22536S treatment (Fig. 6C). Further results showed that after GLEXG treatment, the mitochondrial membrane potential and intracellular ATP levels increased, but the promoting effect weakened with SQ22536S (Fig. 6D, E). Additionally, after treatment with GLEXG, the intracellular Ca2+ concentration and sperm fertilization efficiency increased in H2O2-treated GC-2 cells. However, the efficacy of GLEXG decreased when SQ22536S was also used, leading to reduced intracellular Ca2+ concentration and energized sperm rate (Fig. 6F, G). Based on these results, it was speculated that GLEXG enhances sperm capacitation rates by promoting cAMP/PKA expression in H2O2-treated GC-2 cells.
GLEXG promotes cAMP/PKA expression in H2O2-treated GC-2 cells to improve sperm capacitation rates. A Assessment of cell viability using the CCK-8 assay. B Detection of cAMP, p-PKA, and PKA expression. C Detection of TDRP levels using qRT-PCR and WB. D Mitochondrial membrane potential was analyzed by flow cytometry. E Intracellular ATP levels detected by biochemical assay. F Intracellular Ca2+ concentration measured by flow cytometry. G CTC staining was used to assess the sperm capacitation state. #P < 0.05 vs. H2O2-treated; &P < 0.05 vs. H2O2-treated + GLEXG; n = 3. The data are presented as mean ± SD.
Discussion
According to the research, approximately 500,000 men worldwide have infertility, with OAS being the most common cause, manifested by decreased sperm concentration and motility29,30. Due to the diversity of OAS etiology and its complex pathogenesis, the effective treatment of OAS remains a hot topic in clinical research. Currently, the available treatments for OAS are limited. GLEXG, a traditional Chinese herbal, is used to enhance male reproductive function. It exerts regulatory effects on cellular metabolism, proliferation, and differentiation, while also participating in key processes such as spermatogenesis and maturation11. However, the mechanism of action of GLEXG in OAS is not well understood. This study aimed to investigate the therapeutic effect of GLEXG on OAS and two potential mechanisms of GLEXG treatment for OAS, TDRP methylation and the cAMP/PKA pathway.
Research reports that abnormalities in sperm are a direct manifestation of testicular spermatogenic dysfunction31. Long-term use of GTW leads to testicular atrophy, reduced sperm motility, and other effects32,33. Zhang et al. demonstrated that GTW can be utilized to induce an OAS model in rats1. Our previous experiments have corroborated the induction of OAS by GTW11. Besides, Research indicates a high degree of homology between mice and humans, making mice more advantageous than rats in studying gene function34. Mice and rats differ in size and physiological characteristics, but there is no significant difference in reproductive function, and mice are easier to handle and have lower costs. Therefore, in this study, GTW was selected to induce mice to investigate the effects of GLEXG on OAS. The OAS model was established 7 days before the initiation of the GLEXG intervention. Our results indicate that mice administered with GTW exhibited testicular and epididymal tissue damage, reduced sperm motility, and decreased sperm fertilization efficiency, demonstrating the successful establishment of the OAS model. Meanwhile, during the 21 to 28 days, only GLEXG was administered without GTW, yet significant weight differences were observed (p = 0.0005), indicating GLEXG’s therapeutic effect on OAS. Additionally, Zhou et al. reported that VE has therapeutic effects on male infertility35. Our results showed that GLEXG significantly ameliorated testicular and epididymal tissue damage in GTW-induced OAS mice, and the improvement was superior to VE treatment.
The semen quality is an important indicator of male reproductive capacity36. Spermatozoa are highly differentiated cells and their differentiation process is regulated only by germ cells37. During this process, differentiated germ cells migrate from the basement membrane to the seminiferous tubules, and errors in the migration process can lead to germ cell apoptosis and thus impede sperm development38. Ensuring the correct migration of germ cells plays a key role in aspects such as the correct localization of cells required for the sequential stages of sperm development. In addition, mitochondria are important in the development of spermatozoa to provide energy for sperm development and abnormal sperm development may be accompanied by mitochondrial defects39. Additionally, research reported that after inducing GC-2 cells with H2O2, levels of inhibin-α (a key protein related to sperm production), serum sex hormones, and biological markers responsible for sperm production and function all decreased40. Elizabeth et al. found that levels of HSPA2 (a robust indicator of fertilization potential) decreased after inducing cells with H2O2 41. Therefore, we used H2O2-treated GC-2 cells as an in vitro model and incubated them with GLEXG-containing serum, which also differed from the previous studies in terms of experimental design11. Jin et al. found that cell-secreted DEFB19 contributes to GC-2-spd cell migration, and knockdown of DEFB19 resulted in sterility in mice38. Our results showed a significant increase in the number of migrating H2O2-treated GC-2 cells and an increase in mitochondrial membrane potential after GLEXG treatment, suggesting that GLEXG contributes to sperm development.
Sperm undergoes a highly controlled process known as acrosome reaction (AR) before penetrating the oocyte42. The capacitated spermatozoa need to undergo AR to enter the oocyte and fertilize it42. During sperm capacitation, sperm require the involvement of capacitation factors such as Ca2+, which induces changes in sperm and enables them to acquire fertilization potential43. An increase in intracellular Ca2+ concentration can increase membrane fluidity and flagella strength, which plays a crucial role in sperm capacitation43. Meanwhile, the process of sperm capacitation requires a significant amount of ATP, and the maintenance of sperm vitality and membrane integrity in mammals mainly relies on ATP generated through non-oxidative glucose metabolism in the glycolysis process43,44,45. Therefore, Ca2+ concentration and ATP levels are important indicators for assessing mouse sperm viability. Our results showed that GLEXG increased intracellular Ca2+ concentration and ATP levels in H2O2-treated GC-2 cells, suggesting that significant increase in sperm viability.
Males with OAS display abnormal methylation patterns, with specific methylation sites or regions found to be closely associated with sperm motility16,19. TDRP is predominantly expressed in the testes, and its deficiency in mice has been linked to male infertility, characterized by decreased TDRP methylation in sperm from asthenozoospermic individuals19,20,46. This study demonstrated that GLEXG treatment significantly increased the methylation levels of TDRP and its genes in testicular tissues of GTW-induced OAS mice and H2O2-treated GC-2 cells and that silencing TDRP and inhibiting the methylation levels of the TDRP gene attenuated the therapeutic effects of GLEXG on sperm motility. Furthermore, inhibiting the 26 S proteasome can enhance the role of the AKAP3-mediated cAMP-PKA signaling pathway in sperm capacitation in boars. cAMP-activated protein kinase is the main activator of PKA47. Here, we found that GLEXG treatment promoted the expression of cAMP and PKA in GTW-induced OAS mice and H2O2-treated GC-2 cells and that the use of a cAMP inhibitor was able to attenuate the promotional effects of GLEXG on Ca2+ concentration and ATP levels, sperm viability, mitochondrial membrane potential, and spermatogenesis.
In summary, GLEXG treatment improved sperm quality in mice with GTW-induced OAS and sperm viability in H2O2-treated cells through the cAMP/PKA pathway and TDRP methylation, suggesting new targets for male infertility treatment and new theoretical support for GLEXG treatment of OAS. Besides, our study established a mouse model that is suitable for assessing the impact of GLEXG on reproductive function. However, there are some limitations in this study. The data obtained from the mouse model may not necessarily be directly applicable to humans, and further research is needed to validate our findings. In addition, given the cost of the experiment, we did not administer Decitabine and SQ22536S directly to OAS mice with and without GLEXG and analyze their effects in the testis, which will be further investigated in future experiments.
Methods
GLEXG preparation
The same batch of Cervi Cornus Colla [Cervus elaphus Linnaeus (Cervidae)] (9 g, batch No. 20221008), Testudinis Carapacis et Plastri Colla [Chinemys reevesii (Geoemydidae)] (4.5 g, batch No. 20220608), Lycium barbarum L. (Solanaceae) (3 g, batch No. A210616), and Panax ginseng C.A. Mey (Araliaceae) (3 g, batch No. 2104001) were procured from Hunan Dongjian Pharmaceutical CO., Ltd11. The authentication voucher specimens are deposited at the School of Integrated Chinese and Western Medicine, Hunan University of Chinese Medicine. GLEXG was further prepared and decocted following the guidelines of the “Chinese Pharmacopoeia” (2020)48. The ultimate GLEXG decoction was preserved at 4 ℃ within a refrigerator. Subsequently, a rotary evaporator was employed to prepare the concentration of 0.50 g/mL GLEXG for subsequent research.
Establishment of the OAS mouse model
Eight-week-old Male C57BL/6 mice were purchased from SJA. Laboratory Animal Co., Ltd, Hunan, China. All mice were housed in standard animal cages with a humidity of 60%, a temperature of 20 ℃, and a 12-hour light/dark cycle, with ad libitum access to food and water. This research received ethical approval from the Ethics Committee, and it adhered to the relevant guidelines for the ethical care and use of animals. The study is reported by ARRIVE guidelines. The previous method was used to establish the OAS model11. Following a one-week acclimation period, the OAS mouse model was induced by administering Tripterygium wilfordii polyglycoside (GTW) via intragastric administration at a daily dose of 58 mg/kg (220503, Yifan Pharmaceuticals, China) for four weeks. The assessment of the model involved analyzing histopathological characteristics of the testicular tissue, as well as evaluating sperm concentration and motility49,50.
Experimental design and sample preparation
24 mice were randomly divided into 4 groups (n = 6) for the study: (1) Sham group: normal mice receiving distilled water via oral gavage. (2) Model group: mice receiving distilled water by oral gavage. (3) GLEXG group: Model mice receiving oral gavage of GLEXG (1.44 g/kg/day)11. (4) VE group: Model mice receiving oral gavage of vitamin E (VE) (0.014 g/kg/day, No. H20073374, YiFan Pharmaceutical) serve as the positive control group. The mice were subjected to a 4-week treatment. The body weight of mice was monitored every 7 days. The mice were anesthetized with pentobarbital sodium (50 mg/kg) four weeks later, and the testes and epididymides were removed for weighing and subsequent sperm analysis The organ ratio of the testis and epididymides was calculated using the following formula: weight of left and right testis/epididymis divided by the body weight of the mouse.
Eight-week-old Male C57BL/6 mice were orally administered GLEXG for 7 days, and then mice were anesthetized with pentobarbital sodium (50 mg/kg) and then dissected, blood samples were collected from the abdominal aorta, allowed to stand for 2 h, stored in refrigerators, and subsequently centrifuged to induce blood clotting51. The obtained supernatant was heat-inactivated (56 ℃; 30 min) and filtered (0.2 μm millipore filter) to obtain GLEXG-containing serum52. After sample collection, the mice were euthanized with pentobarbital sodium (150 mg/kg).
Assessment of sperm vitality
The mouse sperm was collected following the previous research methodology53. After an appropriate amount of diluted semen was transferred to a counting chamber for quantification, the sperm were observed using an optical microscope (DSZ2000X, Cnmicro, China). The objective was set to 4× negative phase, ≥ 10 fields of view were selected for each mouse, and spermatozoa were analyzed using a CEROS computer-assisted sperm analysis (CASA, version 12.3, Hamilton Thorne Biosciences, USA) system at 37 ℃. CEROS used the default settings: 60 frames/s, a contrast of 30, cell size pixels, and intensities of 13 and 75, respectively. Then total of 90 frames were captured.
5-Cyano-2,3-ditolyl tetrazolium chloride (CTC) staining detection for sperm capacitation
To assess the mouse spermatozoa capacitation status, the epididymis was first cut caudally and then placed in capacitation medium containing 0.3% bovine serum protein BSA (99.3 mM NaCl, 2.7 mM KCl, 1.8 mM CaCl2·2H2O, 0.3 mM Na2H2PO4·2H2O, 0.5 mM MgCl2·2H2O, 25 mM NaHCO3, 5.6 mM glucose, 24.4 mM lactate, and 0.5 mM pyruvate) to collect mouse spermatozoa and incubate them to enable them. Reagent A (GMS14053, GENMED, USA) was added to the centrifuge tube containing sperm, followed by thorough mixing. The resulting mixture was then counted. Then, 10 µL of sperm was transferred to a new centrifuge tube, followed by the addition of an equal volume of Reagent B and thorough mixing. The mixture was allowed to incubate for 30 min in the dark. Subsequently, 1 µL of Reagent D was added to the centrifuge tube and thoroughly mixed, and 20 µL of the resulting mixture was carefully dropped onto a glass slide. Finally, the sample was covered with a cover slip and observed and counted using a fluorescence microscope.
Hematoxylin-eosin (HE) staining
To evaluate the condition of testicular and epididymal tissue lesions, the testicular and epididymal tissues were fixed, followed by embedding in paraffin, sectioning, dewaxing, and dehydration. The tissue samples were then stained with HE for further analysis. Finally, the dehydrated tissue sections were mounted with neutral gum and observed under a microscope (BA210T, Motic, Singapore) for further examination. Finally, the effect on testicular histology was evaluated by the Johnson score.
Transmission electron microscopy (TEM) assay
After fixing the testicular and epididymal tissues, the tissues were sequentially dehydrated, infiltrated, embedded, and sectioned. Subsequently, the testicular tissue sections underwent staining with Uranyl acetate (GZ02625, EMCN, China). The sections were subjected to examination using a transmission electron microscope (JEM1400, JEOL, Japan), and images were captured utilizing a digital camera (Morada G3, EMSIS GMBH).
Johnson score to assess the degree of testicular tissue damage
The testicular tissue of mice was scored (1–10) concerning the scoring criteria in the study of Maloos Naderi et al.54: 10, normal spermatogenesis with open lumen; 9, many spermatozoa with luminal occlusion; 8, only a few zooplankton; 7, no spermatozoa but many spermatozoa present; 6, no spermatozoa with only a few spermatogonial cells; 5, no spermatogonial/spermatocytes cells but a few spermatogonia; 4, only a few spermatogonia present; 3, spermatogonia with only germ cells present; 2 points, no germ cells, only supporting cells present; 1 point, no cells in tubular section.
Mitochondrial membrane potential assay
Referencing the assay kit manual for Mito-Tracker Red CMXRos (C1049B, Beyotime, China), the cell mitochondria were stained, and the mitochondrial membrane potential was detected using a flow cytometer (A00-1-1102, Beckman, USA).
Flow cytometry assay for Ca 2+ concentration in sperm
To detect the change in Ca2+ concentration in sperm, we strictly adhered to the guidelines of the ISAC. A Ca2+ dye solution (5 µM) was prepared by diluting the Ca2+ stock solution with Fluo-3 AM (S1056, Beyotime, China). The Ca2+ dye solution was added to the cells for staining and incubated at 37 ℃ in the dark for 30 min. After being washed with a serum-free cell culture medium, the cells were subjected to centrifugation to collect the cell pellet. Finally, the fluorescence intensity was measured using a flow cytometer. The excitation wavelength for Ca2+-FITC is 488 nm, and the emission wavelength is 530 nm.
Detection of ATP levels by biochemical analysis
After collecting proteins from sperm/GC-2 cells, the protein concentration of the collected samples was quantified using the BCA protein assay kit (AWB0104, Abiowell, China). The ATP and cAMP content were subsequently determined using the ATP Kit (A095-1-1, Abcam, UK). Finally, the absorbance at 636 nm and 450 nm was measured using a microplate reader (MB-530, Huison, China) to assess the ATP levels.
Detection of cAMP and PKA by Enzyme-linked immunosorbent assay (ELISA)
The OD values of cAMP and PKA were detected at 450 nm according to the instructions provided in the assay kit manuals for cAMP (ab285319, Abcam) and PKA (JL20309, Jonln, China).
Immunofluorescence (IF) detection of TDRP levels
After seeding GC-2 cells, they were subjected to a fixation process lasting 30 min. Then the cells were treated with 0.3% Triton X-100. Followed by blocking with 5% BSA, the cells were incubated with the primary antibody TDRP (1: 50, bs-15291R, Bioss) on the cell culture slides. After incubation, the cells were treated with the CoraLite488–conjugated Affinipure Goat Anti-Rabbit IgG(H + L) (SA00013-2, Proteintech, USA) for 90 min. Subsequently, the cells were stained with a DAPI working solution (AWI0331a, Abiowell) for 10–20 min. Once the slides were mounted using buffered glycerol, they were subjected to observation under a fluorescence microscope. Three fields of view were captured per sample, and fluorescence intensity was analyzed using ImageJ.
Real-time quantitative polymerase chain reaction (qRT-PCR)
To extract the total cellular RNA of TDRP and PKA in testicular tissue and GC-2 cells, the TRIzol method was used. The mRNA was subjected to reverse transcription, converting it into cDNA utilizing the mRNA reverse transcription kit (CW2569, Cowin Bio, China) with mRNA as the template. The resulting product was mixed with Ultra SYBR Mixture (CW2601, Cowin Bio), and specific primers were used for amplification using a fluorescence quantitative PCR instrument (SPL0960, Thermo, USA). The relative levels of the genes were calculated using the 2 −ΔΔCt method with β-actin as the reference gene. We followed the MIQE guidelines for the experiment, the primer sequences are shown in Table 1. Uncropped images for the bands are shown in Supplementary Info File.
Methylation levels detection of the TDRP gene by methylation-specific PCR (MSP)
Methylation levels of the TDRP gene were detected following the instructions of the BisulFlash™ DNA Modification Kit (P-1026-050, Epigentek, USA). The DNA was subjected to agarose gel electrophoresis using a horizontal gel electrophoresis system (DYCP-31DN, LIUYI Bio, China) and an electrophoresis apparatus (DYY-2 C, LIUYI Bio). Finally, the gel image was observed using a gel imaging system. Primer information is provided in Table 1. Uncropped images for the gels are shown in Supplementary Info File.
Western blot (WB)
After the protein was transferred onto the nitrocellulose filter membrane, the membrane was blocked with 5% BSA (9048-46-8,chinasaibao, China) for 90 min. The membranes were then cut into two pieces: one piece was incubated in the appropriately diluted primary antibody PKA (1: 1000, ab32514, Abcam), p-PKA (1: 1000, ab32390, Abcam), TDRP (1: 1000, PA5-52565, Thermo) or β-actin (1: 5000, 66009-1-Ig, Proteintech), while the other was incubated in a mixture of primary antibody and the corresponding blocking peptide (at twice the concentration of the primary antibody) for 2 h, followed by incubation with the corresponding primary antibody overnight. The membrane was left at room temperature for 30 min and washed with PBST. The membrane was then incubated with the diluted HRP goat anti-rabbit IgG (1: 6000, SA00001-2, Proteintech) and HRP goat anti-mouse IgG (1: 5000, SA00001-1, Proteintech) for 90 min. After washing with TBST, the membrane was visualized using a chemiluminescence imaging system (ChemiScope6100, Clinx Science, China) and exposed using enhanced chemiluminescence (ECL, AWB0650, Abiowell) for signal detection. β-actin was used as the internal reference.
Cell culture and grouping
The mouse spermatogonial cells GC-2 (AW-CNM391, Abiowell) were cultured in DMEM medium supplemented with 10% FBS and 1% antibiotics, and incubated in a CO2 incubator at 37 ℃ with 5% CO255. The passaged GC-2 cells were divided into the Control group, Model group, GLEXG group, GLEXG + si-NC group, GLEXG + Decitabine group, and GLEXG + SQ22536S group.
Control group: Cells undergoing normal culture conditions. H2O2-treated group: Cells incubated with H2O2 (50 µM) at 37 ℃ for 3 h to establish a cellular model41. GLEXG group: H2O2-treated cells were incubated in DMEM supplemented with 15% drug-containing serum and 1% antibiotics. GLEXG + si-NC group: H2O2-treated cells were transfected with si-NC and then incubated in DMEM supplemented with 15% drug-containing serum and 1% antibiotics. GLEXG + si-TDRP group: H2O2-treated cells were transfected with si-TDRP and then incubated in DMEM supplemented with 15% drug-containing serum and 1% antibiotics. GLEXG + Decitabine group: H2O2-treated cells were incubated in DMEM supplemented with 15% medicated serum and 1% antibiotics, and subsequently treated with a methylation inhibitor Decitabine (20 µM)56. GLEXG + SQ22536S group: H2O2-treated cells were incubated in DMEM supplemented with 15% drug-containing serum and 1% antibiotics, and subsequently treated with a cAMP inhibitor SQ22536S (25 µM)28.
Transfection of GC-2 cells
Transfection of the si-TDRP plasmid (HG-Si157695, HonorGene China) was carried out into the cells following the instructions provided in the plasmid assay kit manual and using Lipofectamine 2000 (11668019, Invitrogen, USA). After 6 h of transfection, replace it with a fresh DMEM complete culture medium.
Cell counting Kit-8 (CCK-8) assay for cell viability
Cell viability of GC-2 cells was assessed using the CCK-8 assay. After treatment with different drugs according to the groups, the cells were incubated for 0, 24, and 48 h before the assessment. The cells were treated according to the instructions provided in the CCK-8 assay kit (AWC0114b, Abiowell), and the OD value was measured at 450 nm.
Transwell assay for cell migration
500 µL of complete culture medium containing 10% fetal bovine serum was introduced into the lower chamber of the Transwell system (730119, NEST, China). In the upper chamber, GC-2 cell suspension reconstituted in serum-free medium (100 µL/well) was added, followed by a 48-hour incubation period. Afterward, the upper chamber was washed with PBS solution. Cells in the upper chamber were subjected to fixation. Subsequently, the surface of the upper chamber cells was gently wiped using a cotton ball. Subsequently, the cells were stained with 0.1% crystal violet. Finally, the stained upper chamber cells were rinsed with water and observed under an inverted microscope to assess cell migration.
Statistical analysis
Data analysis was performed using GraphPad Prism 9.0. The data are presented as mean ± standard deviation. The data were first evaluated to confirm adherence to normality and homogeneity of variances before any comparison. All normality and variance homogeneity assumptions were rigorously tested using Shapiro-Wilk and Brown-Forsythe tests, respectively. One-way analysis of variance (ANOVA) was used to analyze data across multiple groups under a single variable, exemplified in Figs. 1A and D, 2A–E and 3A–D, etc., followed by a Tukey post hoc test. Similarly, data across multiple groups at various time points were assessed using two-way ANOVA, as seen in Figs. 4D, 5D and 6A, complemented by a Bonferroni post hoc test. A P-value < 0.05 was considered statistically significant.
Data availability
The data used to support the findings of this study are included in the article.
References
Zhang, K. et al. Effects of Qilin pills on spermatogenesis, reproductive hormones, oxidative stress, and the TSSK2 gene in a rat model of oligoasthenospermia. BMC Complement. Med. Ther. 20, 42. https://doi.org/10.1186/s12906-019-2799-7 (2020).
Barratt, C. L. R. et al. The diagnosis of male infertility: an analysis of the evidence to support the development of global WHO guidance-challenges and future research opportunities. Hum. Reprod. Update. 23, 660–680. https://doi.org/10.1093/humupd/dmx021 (2017).
Vickram, A. S. et al. Cryo Lett. 36, 182–186 (2015).
Lu, J. C., Huang, Y. F. & Lü, N. Q. [WHO laboratory manual for the examination and processing of human semen: its applicability to andrology laboratories in china]. Zhonghua Nan Ke Xue. 16, 867–871 (2010).
Wang, Z. et al. Efficacy and safety of nonpharmacological strategies for the treatment of oligoasthenospermia: a systematic review and bayesian network meta-analysis. Eur. J. Med. Res. 28, 6. https://doi.org/10.1186/s40001-022-00968-6 (2023).
Dong, P. et al. Runjing Decoction alleviated cyclophosphamide-induced oligoasthenospermia rats by inhibiting cell apoptosis via RXFP1/AKT/FOXO1 pathway. Andrologia 53, e14216. https://doi.org/10.1111/and.14216 (2021).
Agarwal, A. & Said, T. M. Oxidative stress, DNA damage and apoptosis in male infertility: a clinical approach. BJU Int. 95, 503–507. https://doi.org/10.1111/j.1464-410X.2005.05328.x (2005).
Siterman, S., Eltes, F., Wolfson, V., Zabludovsky, N. & Bartoov, B. Effect of acupuncture on sperm parameters of males suffering from subfertility related to low sperm quality. Arch. Androl. 39, 155–161. https://doi.org/10.3109/01485019708987914 (1997).
Zhou, S. H., Deng, Y. F., Weng, Z. W., Weng, H. W. & Liu, Z. D. Traditional Chinese medicine as a remedy for male infertility: A review. World J. Mens Health. 37, 175–185. https://doi.org/10.5534/wjmh.180069 (2019).
Yang, Y. H. et al. GuiLu-ErXian glue extract promotes mesenchymal stem cells (MSC)-Induced chondrogenesis via exosomes release and delays aging in the MSC senescence process. J. Ethnopharmacol. 317, 116784. https://doi.org/10.1016/j.jep.2023.116784 (2023).
Ding, J. et al. Guilu-Erxian-Glue alleviates tripterygium wilfordii polyglycoside-induced oligoasthenospermia in rats by resisting ferroptosis via the Keap1/Nrf2/GPX4 signaling pathway. Pharm. Biol. 61, 213–227. https://doi.org/10.1080/13880209.2023.2165114 (2023).
Åsenius, F., Danson, A. F. & Marzi, S. J. DNA methylation in human sperm: a systematic review. Hum. Reprod. Update. 26, 841–873. https://doi.org/10.1093/humupd/dmaa025 (2020).
Mima, M., Greenwald, D. & Ohlander, S. Environmental toxins and male fertility. Curr. Urol. Rep. 19 https://doi.org/10.1007/s11934-018-0804-1 (2018).
Štiavnická, M. et al. Sperm DNA methylation patterns at discrete CpGs and genes involved in embryonic development are related to bull fertility. BMC Genom. 23, 379. https://doi.org/10.1186/s12864-022-08614-5 (2022).
Hammoud, S. S., Purwar, J., Pflueger, C., Cairns, B. R. & Carrell, D. T. Alterations in sperm DNA methylation patterns at imprinted loci in two classes of infertility. Fertil. Steril. 94, 1728–1733. https://doi.org/10.1016/j.fertnstert.2009.09.010 (2010).
Poplinski, A., Tüttelmann, F., Kanber, D., Horsthemke, B. & Gromoll, J. Idiopathic male infertility is strongly associated with aberrant methylation of MEST and IGF2/H19 ICR1. Int. J. Androl. 33, 642–649. https://doi.org/10.1111/j.1365-2605.2009.01000.x (2010).
Kumaresan, A., Das Gupta, M., Datta, T. K. & Morrell, J. M. Sperm DNA integrity and male fertility in farm animals: A review. Front. Vet. Sci. 7, 321. https://doi.org/10.3389/fvets.2020.00321 (2020).
Kitamura, A. et al. Epigenetic alterations in sperm associated with male infertility. Congenit Anom. (Kyoto). 55, 133–144. https://doi.org/10.1111/cga.12113 (2015).
Li, J. et al. Genome-wide methylation analyses of human sperm unravel novel differentially methylated regions in asthenozoospermia. Epigenomics 14, 951–964. https://doi.org/10.2217/epi-2022-0122 (2022).
Mao, S. et al. TDRP deficiency contributes to low sperm motility and is a potential risk factor for male infertility. Am. J. Transl Res. 8, 177–187 (2016).
Lee, M. et al. Opioid medication use and blood DNA methylation: epigenome-wide association meta-analysis. Epigenomics 14, 1479–1492. https://doi.org/10.2217/epi-2022-0353 (2022).
Liu, M., Zhang, W., Luo, W. & Nie, Q. Overexpression of TDRP1 gene in swine testis cell and its global transcriptome analysis. DNA Cell. Biol. 32, 511–516. https://doi.org/10.1089/dna.2013.2084 (2013).
Akbari, A. et al. ADCY10 frameshift variant leading to severe recessive asthenozoospermia and segregating with absorptive hypercalciuria. Hum. Reprod. 34, 1155–1164. https://doi.org/10.1093/humrep/dez048 (2019).
de Hurtado, A., Martin-Hidalgo, D., Gil, M. C., Garcia-Marin, L. J. & Bragado, M. J. The calcium/camkkalpha/beta and the cAMP/PKA pathways are essential upstream regulators of AMPK activity in Boar spermatozoa. Biol. Reprod. 90, 29. https://doi.org/10.1095/biolreprod.113.112797 (2014).
Zapata-Carmona, H. et al. The activation of the chymotrypsin-like activity of the proteasome is regulated by soluble adenyl cyclase/camp/protein kinase A pathway and required for human sperm capacitation. Mol. Hum. Reprod. 25, 587–600. https://doi.org/10.1093/molehr/gaz037 (2019).
Wennemuth, G., Carlson, A. E., Harper, A. J. & Babcock, D. F. Bicarbonate actions on flagellar and Ca2+ -channel responses: initial events in sperm activation. Development 130, 1317–1326. https://doi.org/10.1242/dev.00353 (2003).
Dey, S. et al. Cyclic AMP and glycogen synthase kinase 3 form a regulatory loop in spermatozoa. J. Cell. Physiol. 233, 7239–7252. https://doi.org/10.1002/jcp.26557 (2018).
He, Q. et al. Alkaline Dilution alters sperm motility in dairy goat by affecting sAC/cAMP/PKA pathway activity. Int. J. Mol. Sci. 24, 1771. https://doi.org/10.3390/ijms24021771 (2023).
Agarwal, A. et al. Male infertility. Lancet 397, 319–333. https://doi.org/10.1016/s0140-6736(20)32667-2 (2021).
Esteves, S. C. & Chan, P. A systematic review of recent clinical practice guidelines and best practice statements for the evaluation of the infertile male. Int. Urol. Nephrol. 47, 1441–1456. https://doi.org/10.1007/s11255-015-1059-0 (2015).
Baskaran, S., Finelli, R., Agarwal, A. & Henkel, R. Diagnostic value of routine semen analysis in clinical andrology. Andrologia 53, e13614. https://doi.org/10.1111/and.13614 (2021).
Jing, X. et al. Toxic effects of tripterygium wilfordii Hook F on the reproductive system of adolescent male rats. Biomed. Pharmacother. 95, 1338–1345. https://doi.org/10.1016/j.biopha.2017.09.038 (2017).
Qin, Z. et al. Integration of metabolomics and transcriptomics to reveal ferroptosis is involved in tripterygium wilfordii polyglycoside tablet-induced testicular injury. J. Ethnopharmacol. 304, 116055. https://doi.org/10.1016/j.jep.2022.116055 (2023).
Gurumurthy, C. B. & Lloyd, K. C. K. Generating mouse models for biomedical research: technological advances. Dis. Model. Mech. 12 https://doi.org/10.1242/dmm.029462 (2019).
Zhou, X., Shi, H., Zhu, S., Wang, H. & Sun, S. Effects of vitamin E and vitamin C on male infertility: a meta-analysis. Int. Urol. Nephrol. 54, 1793–1805. https://doi.org/10.1007/s11255-022-03237-x (2022).
Eisenberg, M. L. et al. Male infertility. Nat. Rev. Dis. Primers. 9, 49. https://doi.org/10.1038/s41572-023-00459-w (2023).
Teves, M. E. & Roldan, E. R. S. Sperm Bauplan and function and underlying processes of sperm formation and selection. Physiol. Rev. 102, 7–60. https://doi.org/10.1152/physrev.00009.2020 (2022).
Jin, J. et al. Defb19 regulates the migration of germ cell and is involved in male fertility. Cell. Biosci. 12, 188. https://doi.org/10.1186/s13578-022-00924-1 (2022).
Boguenet, M., Bouet, P. E., Spiers, A. & Reynier, P. May-Panloup, P. Mitochondria: their role in spermatozoa and in male infertility. Hum. Reprod. Update. 27, 697–719. https://doi.org/10.1093/humupd/dmab001 (2021).
Kopalli, S. R. et al. Pectinase-treated Panax ginseng ameliorates hydrogen peroxide-induced oxidative stress in GC-2 sperm cells and modulates testicular gene expression in aged rats. J. Ginseng Res. 40, 185–195. https://doi.org/10.1016/j.jgr.2015.08.005 (2016).
Bromfield, E. G., Aitken, R. J., McLaughlin, E. A. & Nixon, B. Proteolytic degradation of heat shock protein A2 occurs in response to oxidative stress in male germ cells of the mouse. Mol. Hum. Reprod. 23, 91–105. https://doi.org/10.1093/molehr/gaw074 (2017).
Breitbart, H. & Grinshtein, E. Mechanisms that protect mammalian sperm from the spontaneous acrosome reaction. Int. J. Mol. Sci. 24 https://doi.org/10.3390/ijms242317005 (2023).
du Plessis, S. S., Agarwal, A., Mohanty, G. & van der Linde, M. Oxidative phosphorylation versus glycolysis: what fuel do spermatozoa use? Asian J. Androl. 17, 230–235. https://doi.org/10.4103/1008-682x.135123 (2015).
Mukai, C. & Okuno, M. Glycolysis plays a major role for adenosine triphosphate supplementation in mouse sperm flagellar movement. Biol. Reprod. 71, 540–547. https://doi.org/10.1095/biolreprod.103.026054 (2004).
Leemans, B. et al. Update on mammalian sperm capacitation: how much does the horse differ from other species? Reproduction 157, R181–r197. https://doi.org/10.1530/rep-18-0541 (2019).
Wang, X. et al. Molecular cloning of a novel nuclear factor, TDRP1, in spermatogenic cells of testis and its relationship with spermatogenesis. Biochem. Biophys. Res. Commun. 394, 29–35. https://doi.org/10.1016/j.bbrc.2010.02.061 (2010).
Qu, X. et al. Inhibition of 26S proteasome enhances AKAP3-mediated cAMP-PKA signaling during Boar sperm capacitation. Anim. Reprod. Sci. 247, 107079. https://doi.org/10.1016/j.anireprosci.2022.107079 (2022).
Xu, X. et al. Development of the general chapters of the Chinese pharmacopoeia 2020 edition: A review. J. Pharm. Anal. 11, 398–404. https://doi.org/10.1016/j.jpha.2021.05.001 (2021).
Chen, W. Q. et al. Wuzi Yanzong Pill-Based on network Pharmacology and in vivo Evidence-Protects against spermatogenesis disorder via the regulation of the apoptosis pathway. Front. Pharmacol. 11, 592827. https://doi.org/10.3389/fphar.2020.592827 (2020).
Li, X. et al. Effects of Zuogui Wan on testis structure and expression of c-Kit and Oct4 in rats with impaired spermatogenesis. Pharm. Biol. 58, 44–50. https://doi.org/10.1080/13880209.2019.1693603 (2020).
Tao, T. et al. Shikonin combined with methotrexate regulate macrophage polarization to treat psoriasis. Bioengineered 13, 11146–11155. https://doi.org/10.1080/21655979.2022.2062090 (2022).
Wu, D. L. et al. Study on the mechanism of Wuzi-Yanzong-Wan-medicated serum interfering with the mitochondrial permeability transition pore in the GC-2 cell induced by atractyloside. Chin. J. Nat. Med. 20, 282–289. https://doi.org/10.1016/s1875-5364(22)60153-5 (2022).
Sheng, W. et al. Tortoise-shell glue ameliorates male infertility through the hypothalamic-pituitary-gonadal axis in obese rats. Anim. Cells Syst. 28, 110–122. https://doi.org/10.1080/19768354.2024.2329684 (2024).
Naderi, M., Ahangar, N., Badakhshan, F., Ghasemi, M. & Shaki, F. Zinc and selenium supplement mitigated valproic acid-induced testis toxicity by modulating the oxidative redox balance in male rats. Anat. Cell. Biol. 54, 387–394. https://doi.org/10.5115/acb.20.280 (2021).
Ma, J. et al. Mitochondria-related miR-574 reduces sperm ATP by targeting ND5 in aging males. Aging (Albany NY). 12, 8321–8338. https://doi.org/10.18632/aging.103141 (2020).
Lou, Y. F. et al. Combination of gefitinib and DNA methylation inhibitor decitabine exerts synergistic anti-cancer activity in colon cancer cells. PLoS One. 9, e97719. https://doi.org/10.1371/journal.pone.0097719 (2014).
Funding
This study was supported by the Key Project of Hunan Provincial Department of Education (No. 24A0765), Natural Science Foundation of Hunan Province (No. 2025JJ70415), National innovation and entrepreneurship training program for college students (No. S202310541041), Research Innovation Foundation of Hunan University of Chinese Medicine (Nos. 2023BKS070, 2024BKS091), and Doctoral Scientific Research Starting Foundation of Hunan University of Medicine (No. 202409).
Author information
Authors and Affiliations
Contributions
Conceptualization: YL; Methodology: CZ; Data curation, Formal analysis, and Visualization: CZ, YL, LL, JX and ZH; Supervision: WS; Project administration: QH; Writing-original draft: CZ and YL; Writing-review & editing: WS and QH. All authors agree to be accountable for the content of the work.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All operations involving animals were approved by the Ethics Committee of Hunan University of Chinese Medicine (LLBH-202304030007). The study is reported in accordance with ARRIVE guidelines.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhu, C., Li, Y., Liu, L. et al. Guilu erxian glue improves sperm quality in oligasthenospermia mice by promoting TDRP methylation and regulating the cAMP/PKA pathway. Sci Rep 15, 27498 (2025). https://doi.org/10.1038/s41598-025-09667-8
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41598-025-09667-8