Abstract
Brain aging is a major factor in cognitive decline and Alzheimer’s disease (AD) progression. Aging-induced microglial senescence critically drives inflammaging and brain aging processes. Nevertheless, the underlying reasons and mechanisms that promote microglial aging remain unclear. This study explores how 27-hydroxycholesterol (27-OHC), a key oxysterol, accelerates brain aging by promoting microglial senescence, iron overload, and neuroinflammation. Clinically, we observed a significant inverse correlation between plasma 27-OHC levels and Mini-Mental State Examination (MMSE) scores in AD patients, accompanied by reduced 24S-OHC concentrations. Experimental studies revealed that 27-OHC administration in mice induced hippocampal-dependent cognitive impairment and anxiety-like behaviors, concurrent with elevated expression of cellular senescence markers (P21, P16, SA-β-Gal) and M1 microglial polarization. In BV-2 cells, 27-OHC disrupted iron homeostasis (DMT1/ferritin/GPX4 dysregulation), elevating ROS and impairing mitochondrial function. Deferoxamine (DFX) mitigated microglial senescence and ferroptosis. These findings establish the 27-OHC-iron axis as a novel therapeutic target for combating cholesterol-driven neurodegeneration.
Similar content being viewed by others
Introduction
Brain aging is a high risk factor for neurodegenerative disorders. The aging process has numerous alterations in the brain, particular cognitive decline and low-grade inflammation being prominent characteristics1. These changes are evident in brain aging and the early stages of Alzheimer’s disease (AD)2.
The aging immune system plays a crucial role in brain aging. As age progresses, the immune functions of identify and eliminate senescent cells gradually declines, therefore, leading to the accumulation of senescent cells in the brain3. Microglia, the principal immune cells of the central nervous system, are integral to neurodegenerative processes and have garnered significant attention for their sentinel role in monitoring both internal and external perturbations, as well as their extended lifespans4,5. These intrinsic immune cells of the brain are essential throughout the human lifespan, contributing to processes from early brain development to the aging phase. Microglia fulfill various functions, such as phagocytosis for debris clearance, modulation of neuroinflammation, and synaptic pruning6. With advancing age, the accumulation of insults, including misfolded proteins, aggregates and pathogens induced by environmental factors, can lead to aberrant activation and impaired functioning of microglia. Aged microglia display a dystrophic morphology indicative of cellular senescence and adopt an activated (primed) phenotype that makes them highly responsive to environmental stimuli, resulting in the production of elevated levels of M1-like pro-inflammatory and neurotoxic mediators, which contribute to neuroinflammation7,8,9.
Evidence has shown that altering microglial iron import mechanisms contribute to blunting inflammation. Iron-accumulating microglia exhibit morphological dystrophy and alterations in iron homeostasis in the human brain, suggesting a potential molecular mechanism underlying the degeneration of microglia in neurodegenerative diseases10. Disruption in the iron transport and metabolism of microglial cells is marked by the activation of microglia and the secretion of proinflammatory cytokines. The accumulation of iron within microglia initiates a series of events culminating in microglial dysfunction and the accumulation of amyloid-beta (Aβ)11. It has been proposed that ‘M1’ microglia, which are characterized by high levels of inducible Nitric Oxide Synthase (iNOS), may be particularly susceptible to ferroptotic or iron-induce cell death12. Meanwhile, excessive iron can induce cellular senescence. Prolonged accumulation leads to microglia morphological changes, enhanced release of cytokines (TNF-α, IL-β, IFN-γ, ROS), and increased endoplasmic reticulum stress13. Despite the discovery of iron dyshomeostasis and neuroinflammation, the characteristic features of senescent microglia are implicated in aging brains and exacerbated in neurodegenerative diseases. However, the underlying reasons and mechanisms that promote microglial aging remain unclear.
Recent studies have suggested that high-fat diet is a potential environmental risk for microglia activation, the production of metabolites from the gut microbiome can impact brain homeostasis by influencing the reactivity and phenotype of microglia14,15. 27-Hydroxycholesterol (27-OHC) is the predominant oxysterol in peripheral blood. Animal studies demonstrate that 27-OHC crosses the blood-brain barrier (BBB) and accumulates in brain tissue, where it disrupts Aβ metabolism and impairs spatial learning and memory16. At submicromolar concentrations, 27-OHC induces senescence in human lung cells and acts as a potent senescence trigger in murine microglia and pheochromocytoma cells17. Postmortem analyses of AD brains reveal disease-progressive increases in specific oxysterols (25-OHC, 27-OHC), while 24S-hydroxycholesterol (24S-OHC) levels decline during late-stage AD. These findings underscore the pro-inflammatory and pro-senescence effects of oxysterols18,19, highlighting their potential contribution to brain aging and the pathogenesis of age-related neurodegenerative disorders by microglia activation.
We hypothesize that 27-OHC accelerates microglial senescence by promoting iron accumulation, thereby exacerbating neuroinflammation and cognitive decline. This study aims to: (1) Investigate the senescence-inducing effects of 27-OHC on microglia, with a focus on its role in iron dyshomeostasis. (2) Evaluate the therapeutic potential of iron chelators in mitigating microglial senescence and neuroinflammation. (3) Provide novel insights into the mechanisms linking oxysterol-driven iron overload to brain aging and cognitive impairment, offering new avenues for therapeutic intervention.
Results
Demographic and clinical characteristics
Demographic characteristics are shown in Table 1. There were 27 age-matched healthy elderly in the control group, 27 MCI group and 17 AD patients. There was no statistically significant difference between the three groups at age and gender (F (2,39) = 0.32, P = 0.054). Education level (F (2.21) = 3.96, P = 0.03) was lower in the AD group compared with the control group. In addition, the MMSE level (F (2.35) = 19.26, P < 0.001) was significantly lower in the MCI, AD compared with the control group.
Analysis of liver function, cholesterol, oxisterols and MMSE in AD and MCI
It has known cognitive function impairment linked to hyperlipidemia and nonalcoholic fatty liver disease, and. The damage to liver function significantly affects the learning memory and cognitive function of patients15. Herein, we detected the liver function by glutamic oxalacetic transaminase (AST) and glutamic pyruvic transaminase (ALT) in plasma from AD and MCI patients, which increased remarkably vs Control group (Fig.1A, B), and the ratio of AST to ALT was higher (Fig.1C). Consistently, increased levels of total cholesterol and 27-OHC were also confirmed in AD and MCI patients (Fig.1D–E). The equilibrium between 27-OHC and 24S-OHC in plasma is essential for cognitive function. Notably, the levels of 27-OHC were significantly elevated, whereas those of 24S-OHC were decreased (Fig.1E, F). The ratio of 27-OHC to 24S-OHC was higher in patients with AD and MCI (Fig.1G). It revealed a negative correlation between the ratios of AST/ALT, total cholesterol and 27-OHC with the MMSE scores in patients (Fig.1H, I, G). In contrast, the ratio of 24S-OHC demonstrated a positive correlation with MMSE scores (Fig.1K).
A, B Concentrations (U/L) of glutamic oxalacetic transaminase (AST) and glutamic pyruvic transaminase (ALT) in each group. C The ratio of AST to ALT in each group. D Concentrations (mmol/L) of cholesterol in each group. E, F The 27-OHC and 24S-OHC concentration (ng/ml) was obtained by established enzyme-linked immunosorbent assay (ELISA). G The ratio of 27-OHC to 24S-OHC in each group (*p <0.05, **p <0.01, ***p <0.001vs. Control). H Correlations between levels of ST/LT and MMSE score (r = −0.56, *p = 0.007). I Correlations between levels of Cholesterol and MMSE score (r = -0.61, p = 0.007). J Correlations between levels of 27-OH and MMSE score r = -049, p = 0.045). K Correlations between levels of 24S-OHC and MMSE score (for AD group: r = 0.57, p = 0.015).
Analysis of Aβ42/Aβ40 with total cholesterol and oxysterol levels
The Aβ42/Aβ40 ratio serves as a biomarker for AD. Further, we quantified Aβ40 and Aβ42 levels using ELISA and conducted correlation analyses with plasma total cholesterol and oxysterol levels. Compared to the control group, plasma Aβ40 levels were significantly elevated in the AD group (Fig. 2A), while no significant difference was observed in the MCI group. Aβ42 levels were reduced in both the MCI and AD (Fig. 2B). Additionally, the Aβ42/Aβ40 ratio was significantly decreased in the MCI and AD groups (Fig. 2C). The Aβ42/Aβ40 ratio was significantly negatively correlated with total cholesterol and 27-hydroxycholesterol (27-OHC) (Fig. 2D–E). Conversely, a positive association was found between 24S-OHC levels and the Aβ42/Aβ40 ratio (Fig. 2F).
A Aβ40 levels in each group. B Aβ42 levels in each group. C Ratio of Aβ42 to Aβ40 in each group. D Correlation in Aβ42/Aβ40 with cholesterol (r = −0.64, P = 0.005). E Correlation in Aβ42/Aβ40 with 27-OHC (r = −0.61, P = 0.006). F Correlation in Aβ42/Aβ40 with 24S-OHC (r = 0.70, P < 0.02).
27-OHC induces cognitive functions impairment
Based on patient-derived outcomes, alterations in liver function were observed, and the plasma concentration of 27-OHC in patients with MCI and AD was significantly elevated, ranging from 800 to 1000 ng/ml. This compound is capable of crossing the blood-brain barrier. We hypothesize that the oxysterol 27-OHC may contribute to brain aging. Drawing on previous studies, we employed the upper limit of this concentration range to calculate an equivalent dosage for mice, which was determined to be 5 mg/kg20. To assess the impact of 27-OHC on cognitive function in mice, we utilized the Morris Water Maze (MWM, Fig. 2A), Novel Object Recognition (NOR, Fig. 3B), and the three-chamber social interaction tests (Fig. 3G). In the MWM, mice administered with 27-OHC exhibited significantly fewer platform crossings and required more time to locate the platform post-training compared to the control group (Fig. 3C–E). Additionally, the cognitive index in the NOR test (Fig. 3F) and the preference index in the three-chamber social interaction test (Fig. 2H, I) were markedly lower in the 27-OHC group relative to the control group.
A Tracking plot of MWM. B Tracking plot of NOR. C Escape latency in test phase. D Escape latency in phase of training. E Number of across the platform. F Discrimination index. G Tracking plot of three chamber social test. H The preference index of phase 1. I The preference index of phase 2. Data are presented as the mean ± standard deviation (n = 8/group),* P < 0.05, **P < 0.01, and ***P < 0.001 (unpaired t test).
27-OHC induces anxiety-like behavior
The majority of patients with neurodegenerative diseases exhibit early symptoms of anxiety21. Consequently, the elevated plus-maze test (Fig. 4A) demonstrated that the frequency of entries into the open arm and the proportion of time spent in the open arm relative to the total time were significantly reduced in the 27-OHC mice compared to the control group (Fig. 4C). In the open field test (Fig. 4B), the duration spent in the central area of the open field was significantly decreased in the model mice (Fig. 4E), whereas the total distance traveled in the peripheral area was significantly increased (Fig. 4G), and the total number of rearing events in the open field was significantly reduced (Fig. 4H).
A Elevated plus maze trajectory plot. B Track plot of the open experiment. C Stay-open arm time ratio of EPM. D Time of the EPM. E Residence time ratio in the OFT center region. F Walking distance in the marginal area. G Total distance traveled. H Total grasp. Data are presented as the mean ± standard deviation (n = 8 / group). *P < 0.05, **P < 0.01, and ***P < 0.001 (unpaired t test).
27-OHC enhances the neurons senescence in hippocampus and prefrontal cortex
The observed cognitive functions decline suggests that 27-OHC may accelerate brain aging. To investigate this, we utilized senescence-associated detection methods, including senescence-associated β-galactosidase (SA-β-Gal) staining and the analysis of P16 and P21 protein expression. It demonstrated a significant increase in SA-β-Gal staining within the hippocampus and prefrontal cortex of mice treated with 27-OHC (Fig. 5A–E). Additionally, western blot analysis indicated substantially elevated levels of P21 and P16 protein expression in these brain regions (Fig. 5F–J). Moreover, there was a significant reduction in the number of Nissl bodies in the 27-OHC group (Fig. 5R–V).
A Representative images of the SA-β-Gal staining in the DG, CA1, CA3 region of the hippocampus and in the cortex, bar = 50 μm. B–E The quantification of SA-β-Gal + cells in hippocampus and cortex (n = 5). F Representative images western blot in the hippocampal tissues and prefrontal cortical tissues. G–J Quantitative analysis of protein levels in the hippocampus and prefrontal cortex. K Representative images of human homeostatic and dystrophic microglia cells. L Representative images of Iba1 of the Immunohistochemistry staining in CA1 region of the hippocampus and the cortex. M, N The proportion of dystrophic microglia in the hippocampus and prefrontal cortex. O Representative images of double immunofluorescence staining for P16/P21 (red) and Iba1 (green), bar = 20 μm. P, Q Statistical analysis of the co-staining of P16/Iba1 and P21/Iba1. R Representative Nissl staining of hippocampus and prefrontal cortex (bar = 20 µm). S–V The statistical analysis of Nissl bodies (n = 5). Data were expressed as mean ± SEM. *p < 0.05, **p < 0.01, ***p < 0.001.
The 27-OHC promotes the microglia senescence and dyshomeostasis of iron in hippocampus and prefrontal
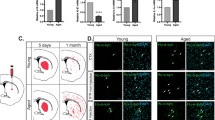
Immunosenescence manifests early in the aging process of the brain. Microglia, the innate immune cells, play a crucial role in brain aging and neurodegenerative diseases22. In this study, we evaluated the impact of 27-OHC on the senescence of microglia. Our findings indicated that microglia exhibited fragmentation and retraction (Fig. 5L-N), with a significantly higher number of dystrophic microglia observed in the hippocampus and prefrontal cortex of 27-OHC-treated mice compared to the control group. It was further observed that the levels of P16 and P21 were notably elevated in microglia following 27-OHC treatment (Fig.5O–Q). Dystrophic microglia serve as significant risk markers for brain aging. There is a well-established correlation between microglial senescence and abnormalities in iron metabolism. Iron overload is a specific marker of senescent microglia. We assessed the intrinsic iron metabolism within cellular systems by evaluating Ferritin and Ferritin light chain (FTL). The results showed that 27-OHC treatment significantly increased ferritin-labeled microglia in the hippocampal CA1 region of mice, while FTL-labeled microglia were markedly reduced (Fig. 6G–J). The fluorescence quantitative analysis of inducible nitric oxide synthase (iNOS, M1) in the hippocampus (Fig. 6A) and prefrontal cortex (Fig. 5B) of mice subjected to 27-OHC treatment was significantly elevated compared to the control group (Fig. 5C, E). In contrast, the fluorescence expression of Arginase 1 (Arg1, M2) in the 27-OHC-treated mice was markedly reduced (Fig.6D–F).
A, B Representative images of immunofluorescence staining of iNOS (M1, red) and Arg1 (M2, green) in the CA1 region of hippocampus and the prefrontal cortex, white box indicates an enlarged image of expression of iNOS or Arg1, bar = 50 μm. C–F The statistical analysis of intensity of fluorescence iNOS and Arg1 in hippocampus and prefrontal cortex. G, H Representative images of fluorescence co-localization of Iba1 and Ferritin and FTL, respectively in the hippocampus of mice. I The statistical analysis of the proportion of cells co-expressing Ferritin+Iba1+ of Iba1+ in hippocampus. J The statistical analysis of the proportion of cells co-expressing FTL+Iba1+ of Iba1+ in hippocampus. All data were expressed as mean ± SEM. *p < 0.05, ** p < 0.01, (n = 5).
27-OHC potentiates the BV2 senescence and inflammatory polarization
To investigate the impact of 27-OHC on microglia, we employed a murine microglial cell strain. BV2 cells were subjected to various concentrations of 27-OHC (0.5 μM, 1 μM, 5 μM, 10 μM, 15 μM, and 20 μM) over periods of 6, 12, 24, 48, and 72 hours. The analysis indicated no statistically significant differences in cell viability across all concentrations at the 6-hour mark (Fig. 7A). However, at 12 hours, a significant reduction in cell viability was detected at concentrations of 15 μM and 20 μM (Fig. 7B). A significant decrease was also observed at a concentration of 10 μM after 24 h (Fig. 7C) (**P < 0.01), and a concentration of 5 μM at both 48 and 72 hours (Fig. 7D–E). These findings suggest that the cytotoxic effects of 27-OHC on BV2 cells are both time- and dose-dependent. Based on clinical measurements, the average concentration of 27-OHC in the blood of patients with AD and MCI was found to be within the range of 800–1100 ng/ml (Fig. 1E), equivalent to a concentration of 0.32–0.44 μM. Consequently, BV2 cells were exposed to a 1 μM concentration of 27-OHC for varying durations of 6, 12, 24, 48, and 72 h. The result obtained from SA-β-Gal staining indicated a time-dependent increase in the percentage of senescent cells (Fig. 7G). Interestingly, we observed a time-dependent escalation in ROS levels, as indicated by DCFH-DA staining (Fig. 7F). Additionally, to verify the polarization status of BV2 cells, the fluorescence intensity of iNOS in cells treated with 27-OHC was significantly higher compared to the control group (Fig. 7K), while the Arg1 was lower than that of the control group (Fig. 7L).
A–E The cck8 test. The effects of different concentrations of 27-OHC on the viability of BV2 cells at 6 h, 12 h, 24 h, 48 h, and 72 h (n = 5). F–H Examine the aging of BV2 cells at 6 h, 12 h, 24 h, 48 h, and 72 h through SA-β-Gal staining and DCFH-DA fluorescent probe. J–L The immunofluorescence staining for the analysis of expression of iNOS (M1, red) and Arg1 (M2, green) in BV2 cells. Data were expressed as mean ± SEM. * p < 0.05, ** p < 0.01, *** p < 0.001, **** p < 0.0001, compare with control group, bar = 50 µm.
DFX rescues 27-OHC-Induced iron dyshomeostasis and M1/M2 imbalance in BV-2
Iron overload is a specific marker of microglial senescence23. The induction of microglial senescence by 27-OHC may be associated with iron dyshomeostasis. To investigate this hypothesis, we examined the interventive effects of Deferoxamine (DFX) on microglia treated with 27-OHC. The results indicated that the iron-treated group, the 27-OHC-treated group, and the combined 27-OHC and iron-treated group exhibited a significant reduction in microglial branching and an increase in surrounding cellular debris compared to the control group (Fig. 8A). Moreover, co-treatment with DFX ameliorated the dystrophic changes in microglia. Notably, it was observed that an increase in DMT1 and Ferritin protein levels and decrease in GPX4 levels in the iron-treated, 27-OHC-treated, and iron+27-OHC treatment groups, which were reversed upon co-treatment with DFX (Fig. 8B–E). Iron overload has the potential to induce mitochondrial dysfunction, thereby disrupting cellular energy metabolism and redox homeostasis, which may ultimately lead to an imbalance between the M1 and M2 microglial phenotypes24,25. We observed that treatment with 27-OHC, iron, or both concurrently promoted a microglial polarization toward the M1 phenotype, characterized by reduced Arg1 and elevated iNOS fluorescence intensity; this effect was reversed by DFX (Fig. 8F–H). We therefore assessed whether this phenotypic shift was associated with altered mitochondrial function. Measurement of mitochondrial membrane potential using the JC-1 probe revealed a significant decrease in the red-to-green fluorescence ratio in both the 27-OHC and iron-treated groups relative to the control (Fig. 8I–J), demonstrating mitochondrial depolarization.
A The morphological diagram of BV2 cells depicts cellular fragmentation, as indicated by the red arrows, bar = 20 μm. B–E Representative western blot images and statistical results of DMT1, Ferritin, GPX4 expressions of protein levels in the BV2 cells. F–H The immunofluorescence staining for the analysis of expression of iNOS (M1, red) and Arg1 (M2, green) in BV2 cells, bar = 20 μm. I The JC-1 fluorescent probe was used to visualize living cells under a fluorescence microscope, bar = 50 μm. J The ratio of red to green fluorescent cells for JC-1 in each group. Data were expressed as mean ± SEM (n = 5). *p < 0.05, **p < 0.01, ***p < 0.001, compare with control group; #p < 0.05, ##p < 0.01, ###p < 0.001 compare with iron group. Ns: No statistically significant difference. DFX: Deferoxamine.
DFX reversed the cognitive impairment and brain degeneration of 27-OHC mice
To evaluate the effect of DFX on cognitive function enhancement, we employed the WMW and NOR behavioral assays to assess the learning and memory capabilities of mice. The showed that, in comparison to the 27-OHC group, the 27-OHC + DFX group exhibited a significant reduction in latency time (Fig. 9A, B), increase in the number of platform crossings (Fig. 9C), and a significant enhancement in the recognition index (Fig. 9D). These outcomes were not statistically difference from those observed in the control group. HE staining revealed markedly improved in disordered and loose neuronal arrangement, as well as reduce in nuclear pyknosis in the group co-treated with DFX (Fig. 9E). Nissl staining results (Fig. 9F) demonstrated that, relative to the 27-OHC group, the number of Nissl bodies in the 27-OHC + DFX treatment group showed a significant increase, and no statistical difference to the Control group (Fig. 9G).
A Escape latency in test phase. B Escape latency in phase of training. C Number of across the platform. D Discrimination index. E Representative HE staining of hippocampus, Bar = 20 µm. F Representative Nissl staining of hippocampus, Bar = 20 µm. G The statistical analysis of Nissl bodies (n = 5). H–L The concentrations of 27-OHC and 24S-OHC in the brain, liver, and plasma were measured separately by ELISA. Data were expressed as mean ± SEM (n = 3). *p < 0.05, **p < 0.01, ***p < 0.001, compared with control group.
DFX reduced microglia ferroptosis in the brain, decreasing the level of 27-OHC in the body
The level change of 27-OHC in the body is to be evaluated in liver, plasma, and brain tissues using enzyme linked immunosorbent assay. The results showed a significant increase in the levels of 27-OHC in the liver, plasma, and brain tissue of mice following intraperitoneal injection of 27-OHC (Fig. 9H-J). However, 24S-OHC was significantly reduced in blood and brain (Fig. 9K, L). Unexpectedly, treatment with DFX markedly mitigated the augment of 27-OHC. DFX could cut down the body level of 27-OHC.
It has been implied a role of iron chelator as a therapeutic option for AD. Thus, we further detected the effect of DFX on microglia and brain. The level changes of GPX4, Ferritin in brain. It showed that the proportion of cells co-expressing GPX4+Iba1+ of Iba1+ in microglia of the hippocampus and prefrontal cortex of mice was decreased (Fig. 10A–D), while the proportion of cells co-expression of Ferritin with Iba1 increased in 27-OHC overloaded mice (Fig. 10B–F). However, DFX treatment reversed this process. It indicated that 27-OHC overload could induce microglia iron dysmetabolism in the brain.
A Fluorescence co-localization of Iba1 and GPX4 in the hippocampus and prefrontal cortex tissues of mice. B Fluorescence co-localization of Iba1 and Ferritin in the hippocampus and prefrontal cortex tissues of mice. C, D The statistical analysis of the proportion of cells co-expressing GPX4+Iba1+ of Iba1+ in hippocampus and prefrontal cortex. E, F The statistical analysis of the proportion of cells co-expressing Ferritin+Iba1+ of Iba1+ in hippocampus and prefrontal cortex. All data were expressed as mean ± SEM. *p < 0.05, **p < 0.01, n = 5, bar = 20 µm.
Discussion
Our findings indicate that 27-OHC contributes to the induction of microglial senescence. The underlying mechanism may involve iron overload, Microglial M1/M2 polarization imbalance, collectively contributing to brain aging and cognitive decline. DFX treatment was observed to attenuate these changes (Fig. 11).
The Graphical Abstract of this study. 27-OHC 27-Hydroxycholesterol, DMT1 Divalent Metal Transporter 1, FTL Ferritin light chain, GPX4 Glutathione peroxidase 4, DFX Deferoxamine.
Some studies suggest that peripheral hypercholesterolemia plays an role in accelarating aging processes and is related to AD or lower cognitive scores26. The oxysterol 27-hydroxycholesterol, a major cholesterol metabolite and main circulating oxysterol in the peripheral circulation of humans, possesses the ability to traverse the blood-brain barrier. Emerging evidence increasingly supports the hypothesis that oxidized cholesterol acts as a pivotal factor and potential missing link between peripheral hypercholesterolemia and AD, primarily through its role as a source of inflammatory mediators27.
Emerging research indicates a potential link between 27-OHC metabolic disorder and mild cognitive impairment (MCI) as well as multi-domain cognitive function in both human and animals subjects28. Additionally, elevated cholesterol levels have been observed in the cores of senile plaques in the human brain, showing a positive correlation with the severity of AD. Furthermore, individuals with AD demonstrate notably higher rates of liver dysfunction29. Single-cell transcription profiling has further revealed an age-related perturbation in cholesterol metabolism within the liver which serve as a central metabolic organ, 27-OHC, an endogenous oxysterol capable of crossing the BBB, induces oxidative stress and promotes systemic chronic inflammation30. Research has indicated a positive correlation between 27-OHC levels in the brain and blood cholesterol levels. Moreover, excessive 27-OHC has been found to expedite the aging process of human lung-resident macrophages and hinder brain glucose uptake, consequently impairing the brain renin-angiotensin system and affecting learning and memory function31. Some scholars propose that the elevation of 27-OHC resulting from dietary cholesterol intake also play a role in the mechanisms through which dietary cholesterol impacts learning and memory impairment32.
Despite the compelling evidence supporting the role of 27-OHC, the science reports heterogeneous associations between its circulating levels and AD pathology. This apparent inconsistency can be largely attributed to the stage-specific nature of 27-OHC’s impact. For instance, significant elevations are often detected in the prodromal or MCI stages, as observed in our cohort and supported by prior work33, whereas differences may attenuate in advanced dementia cohorts34. Furthermore, the strength of the association is influenced by population-specific factors such as the prevalence of comorbidities (e.g., liver dysfunction) and the use of cholesterol-lowering medications, which vary across studies and can confound the relationship35. Therefore, the heterogeneity does not refute the pathogenic role of 27-OHC but rather underscores that its effect is modulated by clinical context and disease phase.
In contrast, 24S-OHC, the dominant brain-derived oxysterol, facilitates cholesterol efflux and supports synaptic integrity and learning. Its circulating levels are considered a reflection of brain cholesterol metabolism36. Notably, the balance between these two oxysterols appears critical: we observed that higher total cholesterol and 27-OHC levels correlated with lower MMSE scores. An elevated 27-OHC/24S-OHC ratio in AD patients implies that disruption of this balance underlies cognitive impairment37. Furthermore, our study showed that patients with MCI and AD exhibited impaired liver function, as indicated by abnormal AST and ALT levels, suggesting that elevated total cholesterol and 27-OHC may be linked to the pathogenesis of both brain and liver disorders. Metabolism of peripheral endogenous cholesterol mainly takes place in the liver. These findings suggest a cross talk occurs between the brain and liver, in which peripheral cholesterol level regulated by liver metabolism, specifically oxysterols influence brain structure and function, to be mediator of the brain-liver axis.
The Aβ pathway is central to AD pathogenesis, with the Aβ42/Aβ40 ratio serving as a key indicator of amyloidosis. This ratio is typically elevated in the brain due to Aβ42 deposition but is consequently reduced in the CSF and plasma, reflecting its sequestration in plaques. This study is directly link this plasma Aβ biomarker to peripheral cholesterol metabolism38. We found the plasma Aβ42/Aβ40 ratio was significantly decreased in patients and exhibited an inverse correlation with total cholesterol and 27-OHC levels. Notably, a positive correlation was observed with 24S-OHC. These findings directly implicate systemic cholesterol homeostasis, and specifically the balance between 27-OHC and 24S-OHC, in Aβ-related pathology.
Cell senescence and cognitive deficits are the main pathologies of brain aging and AD. During aging, the senescent cells naturally accumulate at sites of age-related pathologies39. To detect the role of 27-OHC in brain aging, we evaluated the activity of senescence-associated β-galactosidase (SA-βgal), a widely utilized marker for distinguishing senescent cells from normal ones. Additionally, the p16 gene serves as a negative regulator of the cell cycle by inhibiting the cell cycle protein kinases CDK4 and CDK6, whereas the p21 gene functions to inhibit the cyclin-CDK complex. Both mechanisms contribute to inducing cell cycle arrest in the G1 phase40. Our data showed 27-OHC can make cells senescence and neurons death in the brain. Further, cognitive functions were assessed through water maze, novel object recognition, and three-chamber interaction tests, revealing a significant decline. This finding aligns with Wang et al.‘s study that elevated levels of 27-OHC from intestinal flora disturbance impaired learning and memory function in APP/PS1 mice41. We observed a notable rise in the presence of β-galactosidase staining positive cells, a recognized indicator of cellular senescence, in the hippocampal CA1, CA3, and DG regions of mice treated with 27-OHC. Administration of 27-OHC increased p16 and p21 protein levels in the mouse hippocampus and frontal cortex. Moreover, a marked increase in the expression of these senescence markers was specifically observed in microglia. Furthermore, a significant decrease in the quantity of neurons and Nissl bodies in the hippocampal CA1, CA3, and DG regions, as well as the prefrontal cortex, was observed. These results are consistent with the study conducted by Spanos et al.42, suggesting that exposure to 27-OHC can make cognitive functions decline, cell senescence and neurons loss, subsequently lead to brain aging.
Microglia respond to endogenous and exogenous signals in the body. It not only participates in the establishment and regulation of synapses and the neuronal network,but also contributes to neuroinflammation, serving key functions in the central nervous system (CNS)43. Oxysterols have an influence on the physiology of the immune system, from immune cell maturation and migration to innate and humoral immune responses. Studies have suggested that the senescence of immune cells occurs prior to others of tissue cells. In particular, microglia, the innate immune cells, are thought to act as ‘conductors’ of brain aging and key players in the neurodegenerative disease, but still lack specific evidence about the trigger of microglia senescence44. Thus, we explored the link between 27-OHC and microglia senescence. We found that the morphology of microglia in the hippocampus and prefrontal cortex, which are the brain regions related to spacial learning and memory function, exhibited their process fragmentation and retraction and demonstrated a augment number of retracted or dystrophic microglia in theses areas in the 27-OHC loaded mice A growing body of evidence suggests that the senescence of immune cells occurs prior to that of tissue cells in aging process. In this study, we firstly found 27-OHC can induce microglia senescence and accumualation.
Further, senescent microglia has a causal role in driving brain ageing. It has been reported that senescent microglia exhibit sustained metabolic activity and possess the ability to influence their surroundings via the release of senescence-associated secretory phenotype (SASP) molecules45. Age-related pathological changes manifest at the cellular and molecular levels years prior to clinical detection. Microglial dysfunction in aging serves as an early indicator in AD, potentially sensitizing microglia to inflammatory stimuli and worsening amyloid pathology46. Additionally, microglial activation and priming, as well as the presence of senescent microglia, are implicated in multiple sclerosis, leading to compromised clearance of myelin debris47.
27-OHC can increase microglia inflammatory polarization. Cellular senescence of microglia exhibit a primed phenotype characterized by heightened sensitivity to environmental stimuli and increased production of M1-like pro-inflammatory and neurotoxic mediators48. In the current study, the expression of iNOS (M1) in the hippocampus and prefrontal cortex of mice subjected to 27-OHC treatment was significantly elevated, while as Arg1 (M2) was markedly reduced in vivo and in vitrol. The percentage of 27-OHC induced senescent and dead BV-2 cells increased in dose and time dependently. It indicated that the primed microglia could be initiated by 27-OHC, implicating in the perpetuation of chronic neuroinflammation.
Iron overload serves as a specific biomarker for microglial senescence. Accumulating evidence has established a clear link between microglial senescence and dysregulated iron metabolism49. Iron, as an essential cofactor for the mitochondrial respiratory chain, iron plays a pivotal role in energy production. This suggests that iron metabolism dysregulation in senescent microglia may be interconnected with altered energy metabolism—iron participates in the Fenton reaction to generate oxygen free radicals, which induce lipid peroxidation (especially targeting phospholipids) and ultimately lead to neuronal death50. The increased expression of FTL constitutes an adaptive response to iron overload. It functions to sequester labile iron, thereby reducing the catalysis of lipid peroxidation and thus providing protection against ferroptosis51. Contrary to the typical adaptive increase in FTL during iron overload, we observed a significant FTL decrease following 27-OHC exposure. This interesting phenomenon, wherein 27-OHC induces a decrease in FTL against a backdrop of elevated pan-ferritin, suggests a fundamental disruption in iron homeostasis. A plausible explanation is that 27-OHC triggers ferritinophagy—the selective autophagic degradation of ferritin. This process compromises cellular iron storage, leading to a surge in labile iron that overwhelms antioxidant defenses and propagates oxidative damage. However, it is important to note that the direct evidence for ferritinophagy activation in our model, such as the measurement of NCOA4 protein levels or co-localization of ferritin with autophagosomal markers, is not yet available and remains a key objective for our future investigation52. DMT1 (Divalent Metal Transporter 1), a transmembrane protein primarily mediating Fe²⁺ uptake, plays a critical role in iron metabolism and ferroptosis. Its mechanism involves increased iron uptake, leading to intracellular free iron accumulation, lipid peroxidation, and ultimately ferroptosis. Studies demonstrate that DMT1 knockdown or its inhibitor effectively blocks ferroptosis and mitigates mitochondrial dysfunction53. Under elevated iron toxicity, reduced Glutathione peroxidase 4 (GPX4) protein expression results in the accumulation of cytotoxic lipid hydroperoxides, culminating in cell death54. GPX4 negatively regulates ferroptosis by converting toxic lipid hydroperoxides into harmless alcohols. In summary, these factors are pivotal in ferroptosis. The iron chelator DFX is a ferroptosis inhibitor, polarizes microglia to an M2-like phenotype, and improves behavioral and cognitive deficits in subarachnoid hemorrhage rats, reduces immunoreactivity for ferritin and HO-1 after intracerebral hemorrhage in aged rats55. Our results showed its potential role of 27-OHC in iron metabolism in microglial senescence. To mechanistically interrogate this association, we implemented DFX as an interventional strategy to bidirectionally assess 27-OHC’s regulatory effects on iron homeostasis.
In vitro, 27-OHC treatment induced a senescent-like morphology in BV2 microglia, characterized by reduced branching, enlarged soma, and increased cellular debris. This phenotypic shift was accompanied by significant intracellular iron overload, mirrored by the upregulation of the iron storage protein ferritin and the iron importer DMT1, alongside a downregulation of the ferroptosis inhibitor GPX4. Crucially, the iron chelator DFX concurrently reversed these morphological and molecular changes, demonstrating that 27-OHC promotes microglial senescence primarily by dysregulating iron homeostasis.
It has reported that iron overload can impairs mitochondrial function, the mitochondrial membrane’s central role in ROS generation, where resultant oxidative stress and free radical damage significantly promote microglial senescence56.These ROS attack polyunsaturated fatty acids in mitochondrial membranes, leading to early-stage mitochondrial membrane potential (ΔΨm) dissipation during ferroptosis57. Recently, the impact of peripheral factors on neurodegeneration during aging has gained significant research attention. Studies demonstrate that the cholesterol metabolite 27-OHC exerts neurotoxic effects on C6 cells by inducing oxidative damage through modulation of the Nrf2 signaling pathway58. 27-OHC dose-dependently promotes β-amyloid (Aβ) generation and exacerbates endoplasmic reticulum stress. Cholesterol has been shown to reduce ΔΨm, triggering ROS production, inflammatory responses, and cell death59. Therefore, using JC-1 fluorescence probe assays, we detected pronounced ΔΨm reduction in microglia treated with 27-OHC or 27-OHC+iron. These results demonstrated that 27-OHC exacerbates iron-driven mitochondrial dysfunction and oxidative stress in microglia, accelerating its senescent process.
Furtherly, we investigated the effects of the iron chelator DFX in 27-OHC-exposed mice and microglial cells. Interestingly, treatment with DFX could cause major improvements microglia aging in iron dyshomestasis, microglia inflammatory polarization, iron-driven mitochondrial dysfunction and brain degeneration, cognitive behavior declines in 27-OHC loaded aged mice, ameliorate microglial senescence and ferroptosis in the brain, even unexpectedly resulting in a reduction in the body level of 27-OHC (including in liver, plasma, and brain tissue). A plausible explanation for the 27-OHC-mediated decrease in body 24S-OHC is neuronal injury. Given that neurons are the primary cellular source of 24S-OHC, their impairment would be expected to directly reduce the synthesis and release of this oxysterol.
Methods
Participants’ recruitment and data collection
This study was approved by the Ethics Committee of Ningxia Medical University (Approval No. 2019-316), and informed consent was obtained from all participants prior to their enrollment, and all experiments were performed in accordance with the Declaration of Helsinki. The study cohort comprised 27 patients diagnosed with mild cognitive impairment (MCI), 17 patients with Alzheimer’s disease (AD), and 27 healthy control subjects matched for age (±5 years), sex, and educational background. Exclusion criteria encompassed individuals with conditions known to affect cognitive function, such as brain trauma and depression, as well as those with severe comorbidities, including malignant tumors and cardiac failure. Additionally, individuals undergoing treatment with specific medications, such as statins and immunotherapy drugs, were excluded. The clinical evaluation of AD patients was conducted by the attending physician at Ningxia Medical University, adhering to the AD Diagnostic Standards (NCDS-ADRDA) established by the American Society of Neurology, Language Impairment and Stroke, Alzheimer and Related Diseases in 2007. The Mini-Mental State Examination (MMSE) was used to assess cognitive function, and enzyme-linked immunosorbent assay (ELISA) and high-performance liquid chromatography-mass spectrometry (HPLC-MS) were utilized to analyze blood biomarkers.
Experimental animals
All animal experiments were conducted following the approval and guidelines set forth by the Animal Ethics Committee of Ningxia Medical University (Approval No. 2022-G224). Eight-week-old male C57BL/6 J mice, sourced from the Animal Laboratory Center of Ningxia Medical University, were housed in polycarbonate cages within a temperature-controlled chamber (ambient temperature maintained at 22 ± 2 °C, relative humidity between 40% and 70%, with a 12-h dark/light cycle).
Aging model and drug administration
Mice were randomly divided into two groups (n = 8/group).(a) control group, saline injection via intraperitoneal; (b) 27-OHC group, 5 mg/kg 27-OHC. The 27-OHC injections were performed once daily for 6 weeks20. Further, we added DFX group was treated with injected at 20 mg/kg60 began at the third week for four weeks (n = 8/group).
New object recognition (NOR)
NOR experiments assessed mice’s ability to recognize new objects, mimicking human learning and memory61. Mice first explored an empty box for 5 min, took a 10-min break, then explored the box with two identical objects for another 5 min. Exploration included approaching, sniffing within 2 cm, or touching. One object was then replaced with a new one, and mice explored for an additional 5 min. The time spent on new versus old objects was recorded, and a recognition index was calculated as the time spent on the new object divided by the total time spent on both objects.
Morris water maze (MWM)
Spatial learning and memory were assessed using the MWM task62, which consists of four quadrants and a hidden platform 1 cm below the water. Before training, animals acclimated to the pool for 60 s without the platform. Training lasted five days with four daily trials, recording the time taken to find the platform. Mice unable to find it within 60 seconds were placed on it for 20 s. On the sixth day, a probe trial tested memory by allowing mice to swim for 60 s without the platform, using video tracking to evaluate their recall of its location.
Open field test (OFT)
The OFT evaluated anxiety and movement in mice63. Before testing, mice acclimated to the environment for at least an hour. The test involved a 10-minute session in a 40 × 40 × 30 cm white arena, with a central zone covering 25% of the area. Mice roamed freely, and their movements during the last 5 min were tracked using Smart version 3.0 software. The arena was cleaned with 75% ethanol between sessions. Total distance traveled indicated locomotor activity, while rearing, defecation, and time spent in the center assessed anxiety levels.
Elevated Plus Maze (EPM)
Anxiety-related behavior was evaluated using an elevated plus maze, which leverages rodents’ natural fear of open spaces and heights64. The maze is a gray wooden cross with four 90 × 8 cm arms, elevated 70 cm above the ground. Two arms are open, and two are enclosed by 10 cm high walls. After a 30-min acclimation in the lab, mice were placed at the center, facing an open arm, and observed for five minutes. The time spent in open arms, frequency of open arm entries, and entry distribution across all arms were measured.
Three-chamber sociability
The Three-Chamber Sociability Test used a plexiglass apparatus divided into three chambers to evaluate mice’s social behavior65. The test included three 10-minute phases: the first assessed baseline activity, and the next two evaluated social interaction. Initially, mice explored the apparatus with two cylindrical enclosures. Then, confined to the central chamber, a companion mouse was introduced into one enclosure. In the final phase, another companion mouse was placed in the opposite enclosure. The social interactions of the mice were quantified by assessing their activity levels in relation to their proximity to companion mice. Data collection was facilitated by an automated video tracking system (Smart version 3.0; Panlab, S.L.U, Barcelona, Spain), which recorded the duration spent by the subject mice in each chamber, the frequency of their chamber entries, and the time allocated to sniffing each enclosure.
Sample collection
After the end of the behavioral test, euthanasia was performed by CO2 asphyxiation per protocol. The hippocampus, cortex, and serum were collected and stored at −80 °C, for subsequent experiments.
Nissl staining
Nissl staining was conducted to assess morphological changes in groups exposed to 27-OHC and those treated with DFX. Tissue sections (5 µm) were cut, dried, deparaffinized, and rehydrated. They were stained in 0.5% cresyl violet at 60 °C, washed, and differentiated with hydrochloric acid and ethanol until the background was clear and Nissl bodies were visible. The sections were then dehydrated, cleared, and sealed with neutral resin. Neuronal changes in hippocampal regions (CA1, CA3, DG) and the prefrontal cortex were examined under a microscope.
Immunohistochemistry (IHC) staining
IHC staining was conducted on 5 µm paraffin-embedded sections of brain tissues. Initially, the slides underwent dewaxing and rehydration. Following this, the slides were washed three times with phosphate-buffered saline (PBS), and antigen retrieval was achieved using sodium citrate in a microwave oven at 100 °C for 17 min. The slides were then blocked with 20% normal goat serum for 30 min. Brain tissue slides were incubated with a rabbit anti-mouse Iba-1 antibody at a dilution of 1:8000 (Abcam, catalog number 178847, USA), while intestinal tissue slides were incubated with a rabbit anti-mouse occludin antibody at a dilution of 1:200 (Abcam, catalog number 216327, USA) at 4 °C overnight in a humidified chamber. Post-incubation, the slides were washed with PBS and incubated with horseradish peroxidase (HRP)-conjugated goat anti-rabbit IgG secondary antibody at a dilution of 1:1000 (Abbkine, catalog number A21020, China) for 30 minutes at 37 °C. The slides were then treated with the substrate-chromogen 3,3′-diaminobenzidine for 4 min and subsequently counterstained with hematoxylin. Microscopic images were captured, focusing on positive areas within 40× optical fields of the prefrontal cortex, hippocampal dentate gyrus (DG), CA1, and CA3 regions. Quantitative analysis was performed using ImageJ software.
Immunofluorescence (IF) staining
IF staining was conducted at ambient temperature. In summary, mice were euthanized and subjected to transcardial perfusion with phosphate-buffered saline (PBS; 0.01 M, pH 7.40, 4°C), followed by perfusion with a 4% paraformaldehyde (PFA) solution (pH 7.40, 4°C). The cerebrums were dissected and subsequently immersed in the same PFA solution for fixation (24 h, 4 °C). The samples were then transferred to a 30% sucrose solution for dehydration (48 h, 4 °C). Subsequently, the brain tissues were embedded, frozen at −80 °C, and sectioned into coronal slices with a thickness of 20 µm, which were mounted on glass slides. Prior to staining, the slides were rinsed with PBS and treated with a solution containing 0.3% Triton X-100 and 3% bovine serum albumin (BSA; Sigma No. A7906) for 1 h. The slides were then incubated with primary antibodies overnight (24 h, 4 °C), followed by incubation with the appropriate secondary antibodies for 1 h at 24 °C. Afterwards, the slides were washed and sealed with a DAPI reagent (Thermo Fisher, MA, USA) and subsequently examined under a fluorescence microscope (Leica, Germany). Primary antibodies used were anti-Iba-1 (1:100; No. ab178847, Abcam, MA, USA), anti-Arg1 (1:100; No. DF6657, Affinity, MA, USA) and anti-NOS2 (1:100; No. sc-7271, SANTA CRUZ, MA, USA). Secondary antibodies used were anti-rabbit (1:100; No. ab-150077, Abcam, MA, USA) and anti-mouse (1:100; No. ab150117, Abcam, USA).
Western blot
Mouse hippocampus and cortical tissues were lysed using RIPA buffer on ice for 30 min, with periodic mixing. Protein concentrations were measured using a BCA Protein Assay Kit and denatured by boiling for 5 minutes. Proteins (40–60 µg per lane) were separated via 10% SDS-PAGE and transferred to 0.45 µm nitrocellulose membranes using wet transfer with 30% methanol for 40 min at 220 mA. Following the transfer process, the membrane was blocked using 0.1% BSA in TBST for one hour. Subsequently, it was incubated with rabbit monoclonal P16 and P21 antibodies (1:1000 dilution, catalog number ab272718, Abcam) in a blocking solution composed of PBS at 0.1 M with 5% w/v non-fat dry milk, overnight at 4 °C. The membrane was then subjected to three washes with PBS containing 0.05% Tween 20. It was further incubated for 1 h at room temperature in the blocking solution with either goat anti-mouse IgG 800RD (1:5000 dilution, catalog number 926–32210, BD Biosciences), goat anti-rabbit IgG 680RD (1:5000 dilution, catalog number 925–68071, BD Biosciences), HRP-conjugated anti-mouse (1:3000 dilution, catalog number 192345, Affinity), or HRP-conjugated anti-rabbit (1:3000 dilution, catalog number 56j9958, Affinity). Following additional washes, the membranes were visualized using Odyssey CLX software (catalog number 914100, Biosciences) or detected via enhanced chemiluminescence (catalog number 32106, Thermo Scientific, USA) and Azure c400 (Thermo Fisher, USA). Image analysis was conducted using ImageJ software.
β-Galactosidase (SA-β-Gal) staining
SA-βstaining is a staining assay for senescent cells or tissues based on the upregulation of SA-β-Gal activity levels during aging. The detection of SA-β-Gal activity was performed using the SA-β-Gal Staining Kit (Solarboio, G1580) according to the manufacturer’s instructions. Brain tissue was frozen and sectioned (15 μm), adding 400 μl of β-Gal fixative, fixed at room temperature for 15 min, and washed three times with PBS for 3 min each. An appropriate amount of proportional staining solution was added at 37 °C and left overnight in an incubator without CO2. Positive cells for the hippocampus and microglia were observed under the microscope (Olympus DP73, Olympus, Japan). The area percentage of SA-β-Gal positive cells was analyzed using the Image J software.
BV2 cells culture and treatment
BV-2 cells, derived from C57BL/6 J mice, constitute a microglial cell line that has been immortalized via the expression of the v-raf/v-myc oncogenes. These cells are provided by Guangzhou Secu Biotech Co, Ltd. The cells were cultured under conditions utilizing Dulbecco’s Modified Eagle Medium (DMEM) with high glucose, supplemented with 10% fetal bovine serum (FBS) and 1% penicillin-streptomycin. The cell culture was maintained at a stable temperature of 37 °C in an atmosphere containing 5% carbon dioxide. The cells were divided into 5 groups: Control, Iron (ferric citrate [27], 100 μM, Sigma, 3522-50-7), 27-OHC(27-OHC, 1 μM, LEMEITIAN MEDICINE, 20380-11-4), 27-OHC + Iron, 27-OHC + DFX (DFX [28], 50 μM, Sigma, 138-14-7) for 48 h. Cells and supernatants from different treatment conditions were collected for subsequent experiments.
Cell viability
The Cell Counting Kit-8 (CCK8, Invigentech, IV08-500) was employed to assess cell viability. BV2 cells were seeded into 96-well plates at a density of 1 × 104 cells per well, with six replicates established. Following a 24-h incubation period at 37 °C of varying concentrations of 6 h, 12 h, 24 h, 48 h, and 72 h, respectively. Subsequently, cells were stained with CCK8 for 2 h at 37 C. Absorbance was measured at 450 nm using a microplate reader, and cell viability was calculated using the formula: cell viability = [(As − Ab) / (Ac − Ab)] × 100%, where As represents the absorbance of the treatment group, Ac denotes the absorbance of the control group, and Ab indicates the absorbance of the blank group.
Statistical analysis
All statistical analyses and graphical representations were performed using GraphPad Prism (version 9.0) and IBM SPSS Statistics (version 23.0). Prior to analysis, all datasets were subjected to the Shapiro-Wilk test to assess normality of distribution. Homogeneity of variance was evaluated using Levene’s test. For normally distributed data with homogeneous variance, continuous variables were expressed as mean ± standard deviation (SD) to demonstrate both central tendency and dispersion. Comparative analyses were conducted using appropriate statistical tests: Student’s t-test for comparisons between two groups, and one-way analysis of variance (ANOVA) for multi-group comparisons. Results are presented as mean ± SD. Correlation analyses were performed using Pearson correlation coefficients (PCCs). The direction and strength of correlations were interpreted as follows: r > 0 indicated positive correlation; r < 0 indicated negative correlation; │r│ > 0.7 represented strong linear correlation; 0.5 < │r│ ≤ 0.7 indicated moderate correlation; 0.3 < │r│ ≤ 0.5 suggested weak correlation; and │r│ ≤ 0.3 denoted no linear relationship. A threshold of P ≤ 0.05 was set for statistical significance.
Data availability
The datasets used and/or analyzed during this study are available from the corresponding authors upon reasonable request.
References
Culig, L., Chu, X. & Bohr, V. A. Neurogenesis in aging and age-related neurodegenerative diseases. Ageing Res. Rev. 78, 101636 (2022).
Hou, Y. et al. Ageing as a risk factor for neurodegenerative disease. Nat. Rev. Neurol. 15, 565–581 (2019).
Ovadya, Y. et al. Impaired immune surveillance accelerates accumulation of senescent cells and aging. Nat. Commun. 9, 5435 (2018).
Colonna, M. & Butovsky, O. Microglia function in the central nervous system during health and neurodegeneration. Annu. Rev. Immunol. 35, 441–468 (2017).
Kabba, J. A. et al. Microglia: housekeeper of the central nervous system. Cell. Mol. Neurobiol. 38, 53–71 (2018).
Norris, G. T. et al. Neuronal integrity and complement control synaptic material clearance by microglia after CNS injury. J. Exp. Med. 215, 1789–1801 (2018).
Streit, W. J., Sammons, N. W., Kuhns, A. J. & Sparks, D. L. Dystrophic microglia in the aging human brain. Glia 45, 208–212 (2004).
Safaiyan, S. et al. Age-related myelin degradation burdens the clearance function of microglia during aging. Nat. Neurosci. 19, 995–998 (2016).
Hammond, T. R. et al. Single-cell RNA sequencing of microglia throughout the mouse lifespan and in the injured brain reveals complex cell-state changes. Immunity 50, 253–271 (2019).
Kenkhuis, B. et al. Iron loading is a prominent feature of activated microglia in alzheimer’s disease patients. Acta Neuropathol. Commun. 9, 27 (2021).
Mcintosh, A. et al. Iron accumulation in microglia triggers a cascade of events that leads to altered metabolism and compromised function in app/ps1 mice. Brain. Pathol. 29, 606–621 (2019).
Mccarthy, R. C. et al. Inflammation-induced iron transport and metabolism by brain microglia. J. Biol. Chem. 293, 7853–7863 (2018).
Castellani, R. J., Moreira, P. I., Perry, G. & Zhu, X. The role of iron as a mediator of oxidative stress in alzheimer disease. Biofactors 38, 133–138 (2012).
Ben-Azu, B. et al. Emerging epigenetic dynamics in gut-microglia brain axis: experimental and clinical implications for accelerated brain aging in schizophrenia. Front. Cell. Neurosci. 17, 1139357 (2023).
Vijaya, A. K. et al. Prebiotics mitigate the detrimental effects of high-fat diet on memory, anxiety and microglia functionality in ageing mice. Brain. Behav. Immun. 122, 167–184 (2024).
Wang, Z. et al. Apoe4 activates c/ebpbeta/delta-secretase with 27-hydroxycholesterol, driving the pathogenesis of alzheimer’s disease. Prog. Neurobiol. 202, 102032 (2021).
Hashimoto, Y. et al. 27-hydroxycholesterol accelerates cellular senescence in human lung resident cells. Am. J. Physiol. Lung Cell. Mol. Physiol. 310, L1028–L1041 (2016).
Dias, I. H. K., Shokr, H., Shephard, F. & Chakrabarti, L. Oxysterols and oxysterol sulfates in alzheimer’s disease brain and cerebrospinal fluid. J. Alzheimers Dis. 87, 1527–1536 (2022).
Gamba, P. et al. The controversial role of 24-s-hydroxycholesterol in alzheimer’s disease. Antioxidants 10 (2021).
Wang, T. et al. 27-hydroxycholesterol causes cognitive deficits by disturbing Th17/treg balance and the related immune responses in mild cognitive impairment patients and c57bl/6j mice. J. Neuroinflamm. 20, 305 (2023).
Andriolo, I. R. L. et al. Gastrointestinal issues in depression, anxiety, and neurodegenerative diseases: a systematic review on pathways and clinical targets implications. Cns Neurol. Disord. -Drug Targets 23, 1371–1391 (2024).
Santoro, A., Bientinesi, E. & Monti, D. Immunosenescence and inflammaging in the aging process: age-related diseases or longevity? Ageing Res. Rev. 71, 101422 (2021).
Fernandez-Mendivil, C. et al. Protective role of microglial ho-1 blockade in aging: implication of iron metabolism. Redox Biol. 38, 101789 (2021).
Ahola, S. & Langer, T. Ferroptosis in mitochondrial cardiomyopathy. Trends Cell Biol. 34, 150–160 (2024).
Kenkhuis, B. et al. Iron accumulation induces oxidative stress, while depressing inflammatory polarization in human ipsc-derived microglia. Stem Cell Rep 17, 1351–1365 (2022).
Wu, M. et al. Connecting the dots between hypercholesterolemia and alzheimer’s disease: a potential mechanism based on 27-hydroxycholesterol. Front. Neurosci. 16, 842814 (2022).
Wang, T. et al. Regulation of th17/treg balance by 27-hydroxycholesterol and 24s-hydroxycholesterol correlates with learning and memory ability in mice. Int. J. Mol. Sci. 23, 8–4370 (2022).
Riedel, B. C., Thompson, P. M. & Brinton, R. D. Age, apoe and sex: triad of risk of alzheimer’s disease. J. Steroid. Biochem. Mol. Biol. 160, 134–147 (2016).
Roca-Agujetas, V. et al. Cholesterol alters mitophagy by impairing optineurin recruitment and lysosomal clearance in alzheimer’s disease. Mol. Neurodegener. 16, 15 (2021).
Liu, Q., Liu, C., Hu, F., Deng, X. & Zhang, Y. Non-alcoholic fatty liver disease and longitudinal cognitive changes in middle-aged and elderly adults. Front. Med. 8, 738835 (2021).
Seo, S. W. et al. Nonalcoholic fatty liver disease is associated with cognitive function in adults. Neurology 86, 1136–1142 (2016).
Zhang, D. et al. 27-hydroxycholesterol contributes to disruptive effects on learning and memory by modulating cholesterol metabolism in the rat brain. Neuroscience 300, 163–173 (2015).
Wang, H. et al. Cholesterol, 24-hydroxycholesterol, and 27-hydroxycholesterol as surrogate biomarkers in cerebrospinal fluid in mild cognitive impairment and alzheimer’s disease: a meta-analysis. J. Alzheimers Dis. 51, 45–55 (2016).
Anstey, K. J., Ashby-Mitchell, K. & Peters, R. Updating the evidence on the association between serum cholesterol and risk of late-life dementia: review and meta-analysis. J. Alzheimers Dis. 56, 215–228 (2017).
Han, S., Park, Y. H., Jang, E. S., Nho, K. & Kim, S. Implications of liver enzymes in the pathogenesis of alzheimer’s disease. J. Alzheimers Dis. 88, 1371–1376 (2022).
Pikuleva, I. A. Targeting cytochrome p450 46a1 and brain cholesterol 24-hydroxylation to treat neurodegenerative diseases. Explor. Neuroprot. Ther. 1, 159–172 (2021).
Savulescu-Fiedler, I. et al. The cross-talk between the peripheral and brain cholesterol metabolisms. Curr. Issues Mol. Biol. 47, 2–115 (2025).
Chen, X. et al. Plasma abeta(42):abeta(40) ratio as a biomarker for cognitive impairment in haemodialysis patients: a multicentre study. Clin. Kidney J. 16, 2129–2140 (2023).
Dorigatti, A. O. et al. Brain cellular senescence in mouse models of alzheimer’s disease. Geroscience 44, 1157–1168 (2022).
Zinczuk, J. et al. P16, p21, and p53 proteins play an important role in development of pancreatic intraepithelial neoplastic. Ir. J. Med. Sci. 187, 629–637 (2018).
Wang, Y. et al. 27-hydroxycholesterol contributes to cognitive deficits in app/ps1 transgenic mice through microbiota dysbiosis and intestinal barrier dysfunction. J. Neuroinflamm. 17, 199 (2020).
Spanos, F. et al. Impaired astrocytic synaptic function by peripheral cholesterol metabolite 27-hydroxycholesterol. Front. Cell. Neurosci. 18, 1347535 (2024).
Masuda, T. et al. Novel hexb-based tools for studying microglia in the CNS. Nat. Immunol. 21, 802–815 (2020).
de Medina, P., Silvente-Poirot, S. & Poirot, M. Oxysterols are potential physiological regulators of ageing. Ageing Res. Rev. 77, 101615 (2022).
Loera-Valencia, R., Goikolea, J., Parrado-Fernandez, C., Merino-Serrais, P. & Maioli, S. Alterations in cholesterol metabolism as a risk factor for developing alzheimer’s disease: potential novel targets for treatment. J. Steroid. Biochem. Mol. Biol. 190, 104–114 (2019).
Knezevic, E., Nenic, K., Milanovic, V. & Knezevic, N. N. The role of cortisol in chronic stress neurodegenerative diseases, and psychological disorders. Cells 12, 23–2726 (2023).
Cignarella, F. et al. Trem2 activation on microglia promotes myelin debris clearance and remyelination in a model of multiple sclerosis. Acta Neuropathol. 140, 513–534 (2020).
Covarrubias, A. J. et al. Senescent cells promote tissue nad(+) decline during ageing via the activation of cd38(+) macrophages. Nat. Metab. 2, 1265–1283 (2020).
Singh, H., Gupta, R., Gupta, M. & Ahmad, A. Aging-induced alterations in microglial cells and their impact on neurodegenerative disorders. Mol. Biol. Rep. 52, 515 (2025).
Liddell, J. R. et al. Microglial ferroptotic stress causes non-cell autonomous neuronal death. Mol. Neurodegener. 19, 14 (2024).
Li, Y., Bai, B. & Zhang, Y. Expression of iron-regulators in the bone tissue of rats with and without iron overload. Biometals 31, 749–757 (2018).
Ajoolabady, A. et al. Ferritinophagy and ferroptosis in the management of metabolic diseases. Trends Endocrinol. Metab. 32, 444–462 (2021).
Peng, W. et al. Dmt1 knockout abolishes ferroptosis induced mitochondrial dysfunction in c. Elegans amyloid beta proteotoxicity. Free. Radic. Biol. Med. 224, 785–796 (2024).
Liu, Y., Wan, Y., Jiang, Y., Zhang, L. & Cheng, W. Gpx4: the hub of lipid oxidation, ferroptosis, disease and treatment. Biochim. Biophys. Acta-Rev. Cancer 1878, 188890 (2023).
Zhang, Y. & He, M. Deferoxamine enhances alternative activation of microglia and inhibits amyloid beta deposits in app/ps1 mice. Brain Res. 1677, 86–92 (2017).
Sousa, L., Oliveira, M. M., Pessoa, M. T. C. & Barbosa, L. A. Iron overload: effects on cellular biochemistry. Clin. Chim. Acta. 504, 180–189 (2020).
Schipper, H. M. Brain iron deposition and the free radical-mitochondrial theory of ageing. Ageing Res. Rev. 3, 265–301 (2004).
Ma, W. et al. The oxysterol 27-hydroxycholesterol increases oxidative stress and regulate nrf2 signaling pathway in astrocyte cells. Neurochem. Res. 40, 758–766 (2015).
Solsona-Vilarrasa, E. et al. Cholesterol enrichment in liver mitochondria impairs oxidative phosphorylation and disrupts the assembly of respiratory supercomplexes. Redox Biol 24, 101214 (2019).
Otto-Duessel, M., Brewer, C., Gonzalez, I., Nick, H. & Wood, J. C. Safety and efficacy of combined chelation therapy with deferasirox and deferoxamine in a gerbil model of iron overload. Acta Haematol 120, 123–128 (2008).
Zhang, B. et al. Long-term exposure to a hypomagnetic field attenuates adult hippocampal neurogenesis and cognition. Nat. Commun. 12, 1174 (2021).
Ma, T. et al. Suppression of eif2alpha kinases alleviates alzheimer’s disease-related plasticity and memory deficits. Nat. Neurosci. 16, 1299–1305 (2013).
Koronyo-Hamaoui, M. et al. Peripherally derived angiotensin converting enzyme-enhanced macrophages alleviate Alzheimer-related disease. Brain 143, 336–358 (2020).
Pandya, C. D. et al. Transglutaminase 2 overexpression induces depressive-like behavior and impaired trkb signaling in mice. Mol. Psychiatry 22, 745–753 (2017).
Fu, J. et al. Silica nanoparticle exposure during the neonatal period impairs hippocampal precursor proliferation and social behavior later in life. Int. J. Nanomed. 13, 3593–3608 (2018).
Acknowledgements
We deeply thanks for the Laboratory of Neural Injury and Repairing and Ningxia Key Laboratory of Cerebrocranial Disease of Ningxia Medical University and Qiqihar Medical University for their kind help on technical expertise. This work was supported by the Natural Science Foundation of Ningxia (No.2024AAC03254), Ningxia key research and development project (No.2020BEG03048), Item of scientific research fund for young doctor of Qiqihar Academy of Medical Sciences (No.QMSI2024B-06), The Qiqihar City Science and Technology Bureau project of China(LSFGG-2025123), and Basic scientific research business expenses of provincial undergraduate universities in Heilongjiang Province in 2024 (No.2024-KYYWF-0350).
Author information
Authors and Affiliations
Contributions
C.Y., W.W., and L.S. performed all the experiments and wrote the manuscript. Y.Z. and Z.C. completed the statistical analysis. R.M., T.W., and X.W. completed the collection and analysis of clinical data. J.T.and Y.Z. designed and guided the experiments, and critically revised the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Yu, C., Wang, W., Shi, L. et al. 27-Hydroxycholesterol triggers microglial senescence subsequent to iron over-loading contributes to brain aging, suppressed by Deferoxamine. npj Aging 12, 7 (2026). https://doi.org/10.1038/s41514-025-00303-3
Received:
Accepted:
Published:
Version of record:
DOI: https://doi.org/10.1038/s41514-025-00303-3